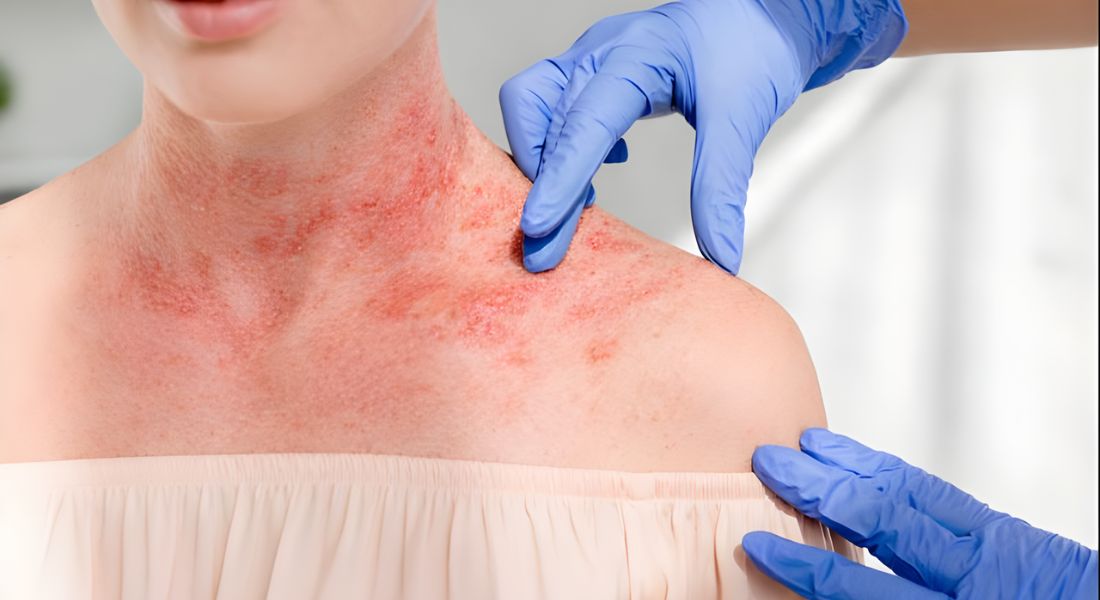
When you live with eczema, it can feel like a condition that only shows up on the surface of your skin. Redness, dryness, flaking, and relentless itching are what you notice first. These visible signs often make you think it’s purely a skin problem.
Eczema, or atopic dermatitis, is more than irritated skin. It is a chronic inflammatory condition driven by your immune system, rather than just external triggers. At the centre of this process is Th2-dominant inflammation, which shapes how your skin reacts and how your body responds.
By understanding Th2 inflammation, you can see why treatments work differently at different times. Cytokines such as IL-4, IL-13, and IL-31 play a key role in driving symptoms and persistent irritation. This is why some therapies target your immune system directly, instead of focusing only on moisturisers or barrier creams.
Why Eczema Is Not “Just Sensitive Skin”
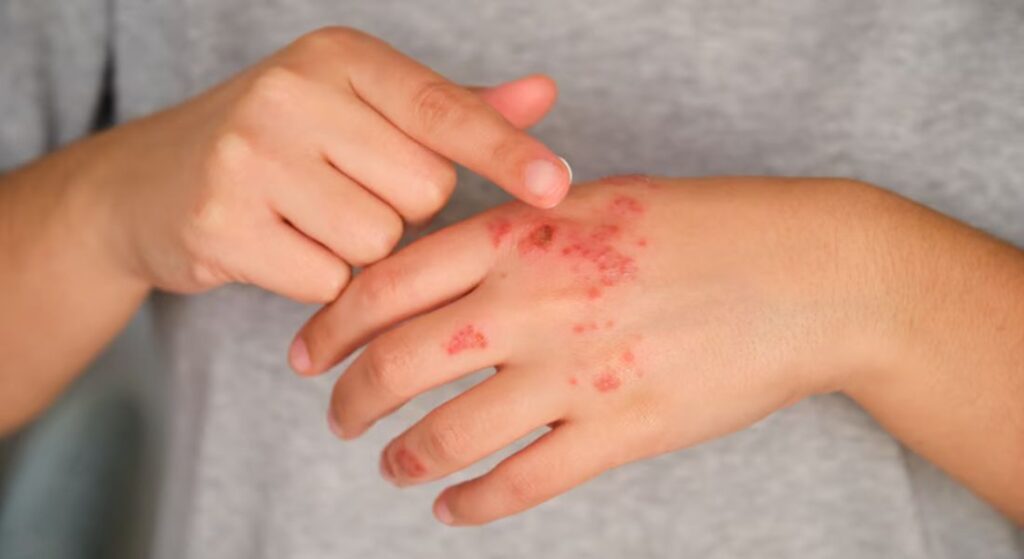
You might have heard that eczema is caused by weak or sensitive skin alone. While your skin barrier is indeed affected, that’s only part of the picture. The real issue lies in how your immune system behaves beneath the surface.
In healthy skin, your immune responses are carefully controlled. They activate when a threat appears and calm down once it’s gone. In eczema, however, your immune system stays switched on, even when there’s no infection or injury.
This constant immune activity drives inflammation from the inside out. That’s why your eczema can flare without any obvious trigger. The redness, itching, and irritation you see are just the visible result of a deeper internal process.
A Quick Primer on the Immune System (Without the Jargon)
To understand Th2 inflammation, it helps to know a little about how your immune system is organised. Your body uses specialised white blood cells called T helper (Th) cells to coordinate its responses. Each type of Th cell releases chemical messengers, known as cytokines, to guide your immune reactions.
Every Th pathway has a specific role. Some fight bacteria, others target viruses, and some manage parasites or allergens. Problems occur when one pathway becomes dominant at the wrong time.
In eczema, your immune system leans heavily towards the Th2 pathway. This imbalance influences everything that happens next, from inflammation to itching and redness. Understanding this helps you see why treatments that target Th2 activity can be so effective.
What Does “Th2-Dominant” Actually Mean?
The term Th2-dominant describes a specific imbalance in how your immune system responds. It refers to increased activity of T helper type 2 (Th2) cells, which normally play a useful and tightly controlled role in immune defence. In conditions like eczema, this balance is disrupted, leading to ongoing inflammation rather than protection.
- Th2 Cells and Their Normal Function: Th2 cells help protect the body against parasites and support antibody production. Antibodies are essential for identifying and neutralising threats. Th2 responses also contribute to allergic reactions, but under normal circumstances, these reactions are mild and well regulated.
- Th2 Overactivity in Eczema: In eczema, Th2 cells become overactive and dominate immune signalling. They release high levels of cytokines, which are chemical messengers that drive inflammation. This process causes itching and weakens the skin barrier, even when there is no infection or visible injury.
- Chronic Inflammation and Long-Term Effects: Persistent Th2 activity keeps the immune system switched on in the skin. This leads to repeated flare-ups and prevents proper barrier repair. Over time, the skin remains stuck in a cycle of inflammation, making eczema a chronic condition rather than a short-term rash.
Being Th2-dominant means the immune system is biased towards excessive Th2 responses. In eczema, this imbalance drives ongoing inflammation, damages the skin barrier, and explains why symptoms tend to persist without long-term management.
The Key Cytokines Driving Eczema
Cytokines are small signalling proteins that act like text messages between your immune cells. They help your body coordinate responses and react to potential threats. In eczema, a few cytokines become overactive and play a central role in driving your symptoms.
The most well-studied cytokines are IL-4, IL-13, and IL-31. IL-4 and IL-13 contribute to inflammation and weaken your skin barrier, making it harder for your skin to retain moisture. IL-31 is closely linked to itching, which is often the most bothersome symptom.
Together, these cytokines create the backbone of Th2-driven eczema. They explain why flare-ups can appear suddenly, even without an obvious trigger. Understanding their role helps you see why modern therapies focus on blocking these specific signals rather than just treating the surface.
IL-4: The Master Switch
IL-4 is often called the “master regulator” of Th2 inflammation. It encourages your immune cells to commit to the Th2 pathway, shifting the entire immune response in that direction. Once IL-4 signalling is active, your body’s immune system is essentially set on a Th2-driven course.
In eczema, IL-4 drives inflammation in your skin. It reduces the production of proteins that are essential for a strong skin barrier, making your skin more permeable and prone to irritation. This weakening of the barrier also makes flare-ups more likely and more severe.
IL-4 also suppresses parts of your immune system that would normally keep inflammation in check. That imbalance allows Th2 activity to continue unchecked. In simple terms, IL-4 keeps the inflammatory loop running, which is why eczema often persists over time.
IL-13: The Barrier Disruptor
IL-13 works closely with IL-4, and they even share some receptor components. While their functions overlap, IL-13 has a particularly strong impact on your skin barrier. It directly affects the proteins that keep your skin healthy and resilient.
This cytokine interferes with the production of filaggrin and other structural proteins. Filaggrin is essential for maintaining hydration and integrity in the outer layers of your skin. When filaggrin levels are low, water escapes and irritants can enter more easily, making your skin more vulnerable.
Over time, IL-13 also encourages thickening of your skin. This leads to lichenification, where chronic scratching makes the skin leathery. The more active IL-13 is, the harder it becomes for your skin to heal and stay calm.
IL-31: The Itch Cytokine
IL-31 is a key driver of the intense itching commonly experienced in eczema. Unlike cytokines that mainly promote visible inflammation, IL-31 acts directly on itch-sensing nerve fibres in the skin. This explains why itching can be severe even when redness or swelling appears limited.
- IL-31 and Itch Sensation: IL-31 directly activates nerve fibres responsible for sensing itch. Its action is partly independent of classic inflammatory signs like redness or swelling. This helps explain why eczema itch can feel relentless even during mild-appearing flares.
- Elevated IL-31 Levels in Eczema: People with moderate to severe eczema often have increased IL-31 levels. Higher levels are associated with stronger and more persistent itching. Itch can continue even when other inflammatory features seem controlled.
- The Itch–Scratch Cycle: Scratching damages the skin barrier, increasing vulnerability to irritation and infection. Barrier disruption triggers further immune activation and cytokine release. This creates a self-perpetuating cycle that prolongs flare-ups and worsens symptoms.
IL-31 plays a central role in driving persistent itch in eczema. By directly stimulating nerves and fuelling the itch–scratch cycle, it highlights why effective itch control is essential alongside reducing visible inflammation.
How Th2 Inflammation Alters the Skin Barrier
Your skin barrier is more than just a physical wall it’s an active interface between your body and the environment. It keeps moisture in and harmful substances out, helping your skin stay healthy. In eczema, Th2 cytokines interfere with this barrier at multiple levels.
IL-4 and IL-13 reduce the production of lipids in your outer skin layers. These lipids normally seal moisture inside your skin, keeping it soft and hydrated. When lipid levels drop, dryness becomes persistent and more severe, making your skin feel tight and irritated.
At the same time, Th2 activity suppresses antimicrobial peptides. These peptides normally protect your skin from bacteria like Staphylococcus aureus. When they are reduced, your skin becomes more prone to infections, which in turn worsen inflammation and trigger flare-ups.
Why Eczema Is Linked to Allergies and Asthma
Th2 dominance doesn’t just affect your skin it reflects a broader immune tendency towards allergic conditions. This is why eczema often occurs alongside hay fever, food allergies, or asthma. The same underlying immune pattern drives these reactions across different parts of your body.
This progression is sometimes called the atopic march. It describes how allergic conditions can appear over time in the same person. Th2 inflammation is the common thread linking them all.
Understanding this helps you see that eczema isn’t just an isolated skin issue. It’s part of a wider systemic immune pattern. Recognising this connection has changed how modern treatments approach eczema and related conditions.
Acute vs Chronic Eczema: A Shifting Immune Landscape
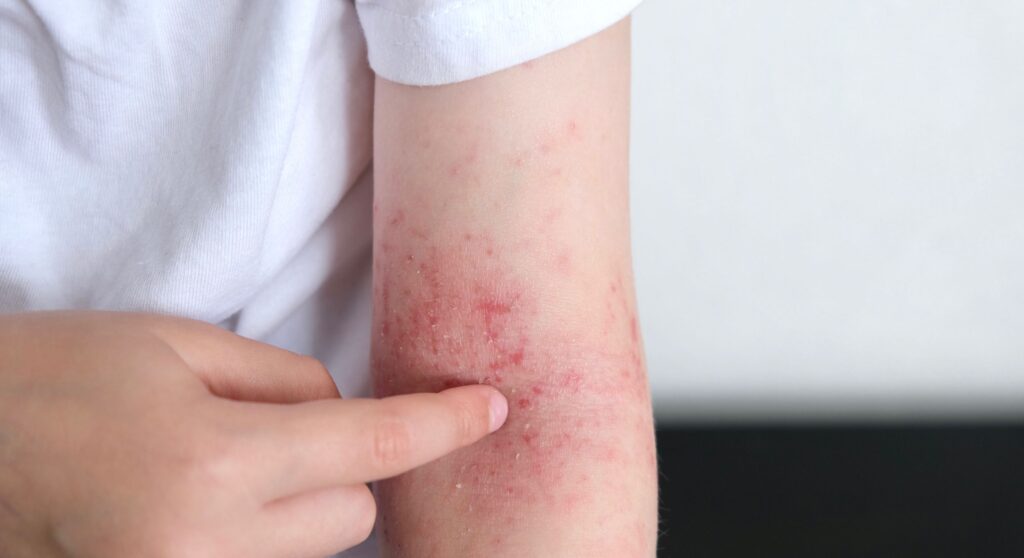
Eczema is not static when it comes to your immune system. Early or acute flare-ups are largely driven by Th2 activity. As the condition becomes chronic, other immune pathways, such as Th1 and Th17, begin to contribute.
Despite these changes, Th2 activity usually remains dominant. This layered immune response explains why chronic eczema can look and feel different from initial flare-ups. It also helps you understand why some treatments that worked early may become less effective over time.
Targeting only surface inflammation often isn’t enough. Systemic therapies are designed to address these deeper shifts in your immune system. By doing so, they aim to bring longer-lasting relief and control of your eczema.
Why Topical Treatments Sometimes Fall Short
Topical steroids and emollients are important tools for managing eczema. They reduce inflammation and help restore hydration to your skin. However, they don’t address the underlying immune signalling that drives the condition.
When Th2 cytokines remain active, inflammation often returns. You may notice flare-ups reappear as soon as treatment stops. This can feel frustrating, but it’s not a reflection of anything you’ve done wrong.
The limitations of surface-level treatments highlight the need for deeper interventions. Persistent immune activation often requires therapies that target the immune system itself. This approach aims to provide longer-lasting relief and better control of your eczema.
The Science Behind Targeted Systemic Therapies
Modern eczema treatments are designed with Th2 biology at their core. Rather than broadly suppressing your immune system, they target specific cytokines or receptors. This precision helps control your symptoms while reducing side effects.
Biologic therapies provide the clearest example. They use monoclonal antibodies to block IL-4 and IL-13 signalling, directly interrupting the Th2 cascade. By tackling inflammation at its source, they can bring longer-lasting relief.
This represents a shift from simply managing symptoms to addressing the underlying mechanism. It is one of the most significant advances in eczema care in decades. All of this progress is grounded in our understanding of Th2 inflammation.
IL-4 and IL-13 Blockade: Why It Works
Blocking IL-4 and IL-13 affects several processes that drive your eczema. Your skin barrier begins to recover as structural protein production improves, and fewer inflammatory cells are recruited to the skin. These changes help reduce redness, irritation, and ongoing inflammation.
Many people notice that their itch decreases within just a few weeks. Over time, skin texture and hydration improve, and flare-ups tend to become less frequent. This makes day-to-day management of eczema much easier.
These results confirm what immunology predicts. By interrupting Th2 signalling, the underlying drivers of eczema activity are dampened. In effect, the science translates directly into real, clinical benefits for your skin.
Treatment Resistance Explained by Immune Biology
Not everyone responds to treatment in the same way, and this variability is rooted in immune differences. Some people have stronger contributions from non-Th2 pathways, which can make standard therapies less effective.
Long-standing skin changes may also take time to reverse, even when inflammation decreases. In addition, nerve sensitisation can persist, meaning itch may continue after visible improvement. These factors help explain why some symptoms linger despite treatment.
Understanding treatment resistance helps you set realistic expectations. It also guides adjustments to your care plan. By respecting the underlying biology, personalised treatment becomes possible, improving long-term outcomes.
Why Scratching Makes Everything Worse
Scratching can feel like temporary relief, but in eczema it actively worsens the condition. Each scratch causes microscopic damage to the skin, triggering immune signals that increase inflammation and intensify itching. This creates a vicious cycle that makes flare-ups harder to control over time.
- Mechanical Damage from Scratching: Scratching physically injures skin cells, even when the damage isn’t visible. These injured cells release danger signals that alert the immune system. The body responds as if the skin is under threat, even when no infection is present.
- Amplification of Th2 Immune Activity: Danger signals attract more immune cells to the affected area. Th2 cells release additional cytokines, including itch-promoting molecules. This escalation increases redness, inflammation, and the intensity of itch with each scratch.
- Strengthening of the Itch–Scratch Cycle: Increased inflammation further sensitises itch-sensing nerves. This makes the urge to scratch stronger and more frequent. Each episode of scratching reinforces the cycle, prolonging flare-ups.
- Breaking the Itch–Scratch Cycle: Simply trying not to scratch is rarely enough to stop the process. Effective management focuses on reducing the biological drivers of itch, such as IL-31 and nerve signalling. Treatments that calm itch at its source help protect the skin barrier and reduce ongoing inflammation.
Scratching fuels immune overactivity in eczema, turning mild irritation into persistent flare-ups. Addressing the underlying biological causes of itch, rather than relying on willpower alone, is essential for breaking this cycle and managing symptoms effectively.
The Psychological Burden of Th2-Driven Eczema
Chronic inflammation in eczema doesn’t stay limited to your skin. Persistent itch, discomfort, and disrupted sleep can take a real toll on your mental health. Many people experience anxiety, low mood, or heightened stress as a result of living with eczema.
Th2 cytokines may also interact with your nervous system, amplifying stress responses. This creates a feedback loop where stress can further dysregulate your immune system, potentially worsening flare-ups. Understanding this connection helps explain why eczema often feels overwhelming beyond the physical symptoms.
Addressing eczema effectively means looking at the condition holistically. Treatments that target the immune system can improve both your skin and overall quality of life. By managing Th2-driven inflammation, you are supporting not just your skin, but your mental wellbeing too.
Why Early Intervention Matters
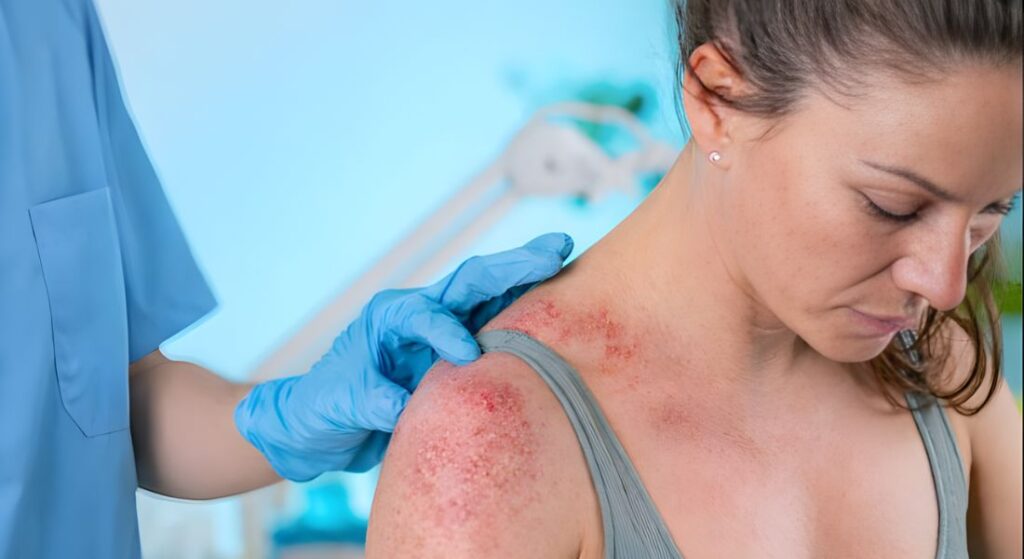
The longer Th2 inflammation continues, the harder it becomes to reverse the effects. Chronic changes in your skin’s structure and increased nerve sensitivity can develop over time, making flare-ups more severe and persistent. Controlling inflammation early can help prevent this progression and protect your skin long-term.
Early intervention doesn’t mean aggressive treatment for everyone. It means timely escalation of care when appropriate, guided by a clear understanding of the underlying immune drivers. Knowing what is happening in your skin helps make treatment decisions more precise and effective.
If eczema is affecting your daily life, it deserves proper assessment by a healthcare professional. This may include considering advanced therapies designed to target Th2 inflammation directly. Using biology as the guide ensures your care is targeted, rather than relying on trial-and-error approaches.
Personalised Eczema Care in Clinical Practice
Eczema doesn’t look the same in every person, and the immune processes driving it can differ widely. Your immune profile may influence how your skin responds to various treatments. As a result, care is moving towards a more stratified, personalised approach.
Biomarkers are increasingly being used to identify which immune pathways are most active in your eczema. This information can help predict which therapies are likely to work best for you. While Th2 dominance is the most common pattern, other pathways may contribute to your condition as well.
In specialist settings, this knowledge already shapes treatment plans. For example, if you are exploring eczema care in London, immune-targeted therapies are becoming central to personalised treatment strategies. The ultimate goal is to achieve long-term control rather than relying on repeated short-term fixes.
The Future of Th2 Research in Eczema
Research continues to refine our understanding of Th2 inflammation and its role in eczema. Scientists are studying new cytokines and receptors, and combination treatment approaches may further improve outcomes. These advances aim to target the underlying immune mechanisms more precisely.
There is also growing interest in how your skin microbiome interacts with immune signalling. The bacteria on your skin can influence Th2 activity and the health of your skin barrier. Modulating this relationship may offer new therapeutic strategies in the future.
What is clear is that eczema science has moved far beyond simple surface explanations. Immune precision is shaping the future of treatment, focusing on the biology that drives your condition. As these insights continue to grow, patients like you stand to benefit enormously from more effective and personalised care.
FAQs:
1. What is Th2-dominant inflammation in eczema?
Th2-dominant inflammation occurs when a type of immune cell called T helper 2 (Th2) becomes overactive. These cells release cytokines like IL-4, IL-13, and IL-31, which drive inflammation, itch, and skin barrier damage, making eczema chronic and persistent.
2. Why isn’t eczema just sensitive skin?
Eczema is more than a skin barrier issue. While dryness and irritation are visible, the core problem is an overactive immune system that keeps your skin inflamed even without external triggers.
3. Can Th2 inflammation affect mental health?
Yes. Chronic itch and discomfort can cause anxiety, stress, and sleep disruption. Th2 cytokines may also interact with the nervous system, amplifying stress responses and creating a feedback loop that worsens eczema.
4. What are cytokines and why are they important in eczema?
Cytokines are signalling proteins that help immune cells communicate. In eczema, IL-4, IL-13, and IL-31 are overproduced, driving inflammation, skin barrier disruption, and persistent itching.
5. How does Th2 inflammation weaken the skin barrier?
IL-4 and IL-13 reduce essential skin proteins and lipids, making the skin dry, leaky, and prone to irritation. This also decreases antimicrobial peptides, increasing susceptibility to infections.
6. Can Th2 inflammation explain eczema’s link to allergies and asthma?
Yes. Th2 dominance is associated with other allergic conditions like hay fever, food allergies, and asthma. This interconnected pattern is called the “atopic march.”
7. Why do eczema flare-ups happen without triggers?
Because the Th2 immune pathway is overactive, your skin remains inflamed internally, even when no external irritants or infections are present.
8. Why do topical treatments sometimes fail?
Creams and steroids mainly address surface inflammation and hydration. They don’t target the underlying Th2-driven immune overactivity, so flare-ups can recur when treatment stops.
9. What are targeted systemic therapies for eczema?
These treatments, including biologics, block specific cytokines like IL-4 and IL-13. By addressing the immune overactivation directly, they reduce inflammation, improve the skin barrier, and provide longer-lasting relief.
10. How does IL-31 contribute to eczema itch?
IL-31 stimulates nerve fibres in the skin that detect itch. It creates a cycle where scratching damages the skin barrier, triggers more immune activation, and worsens inflammation and itching.
Final Thoughts: Taking Control of Eczema: Understanding and Managing Th2 Inflammation
Eczema is far more than a surface skin condition. Understanding the science behind Th2-dominant inflammation reveals why flare-ups occur, why itch can be relentless, and why topical treatments alone sometimes fall short. By recognising the key roles of cytokines like IL-4, IL-13, and IL-31, we can appreciate how targeted therapies work at the root of the problem, not just on the surface. Early intervention and personalised care are essential in managing eczema effectively, preventing long-term skin changes, and reducing the psychological burden of chronic itching and discomfort.
If you’re looking for Eczema treatment in London, you can reach out to us at the London Dermatology Centre to book a consultation with one of our specialists. With modern therapies grounded in immune science, long-lasting relief and improved skin health are possible.
References:
- Wollenberg, A., Flohr, C., Simon, D., et al., 2025. Immunopathogenesis of Atopic Dermatitis: Focus on Interleukins as Disease Drivers. International Journal of Molecular Sciences, https://www.mdpi.com/1422-0067/24/1/781
- Nakagawa, H., Furue, M., 2024. Multiple Roles for Cytokines in Atopic Dermatitis: IL-4, IL-13, IL-31, and Alarmins. International Journal of Molecular Sciences, 23(5), https://www.mdpi.com/1422-0067/23/5/2684
- Bieber, T., 2011. Atopic Dermatitis. New England Journal of Medicine, https://pubmed.ncbi.nlm.nih.gov/21994899/
- Czarnowicki, T., He, H., Krueger, J.G. and Guttman-Yassky, E., 2021. Novel Pathogenesis of Atopic Dermatitis: Advances in Understanding Immune Dysregulation. https://pubmed.ncbi.nlm.nih.gov/34388479/
- Howell, M.D., Kim, B.E., Gao, P., et al., 2018. From Pathways to Patients in Atopic Dermatitis: Advanced Systemic Therapies. Experimental Dermatology, https://www.sciencedirect.com/science/article/pii/S1578219020300238