Scar treatment has traditionally relied on single-modality approaches. You may have been offered a laser, microneedling, steroid injections, or topical therapy depending on the scar type. While many of these treatments are effective, they often address only one component of the scar.
Modern dermatology is moving towards combination therapy. Instead of treating texture, pigmentation, and inflammation separately, future protocols aim to target multiple pathways at once. This shift reflects a deeper understanding of how scars form and remodel over time.
In this article, we explore how lasers, microneedling, and biologic pathway modulation may work together in evolving scar management strategies. You will understand why combining energy-based devices with targeted biologic modulation may improve long-term results. Scar treatment is becoming more intelligent, layered, and personalised.
Understanding How Scars Form
Scars form as part of your body’s natural wound-healing response. When your skin is injured, collagen production increases to repair the damaged area and restore strength. However, this repair process does not always recreate the smooth structure of normal skin. Instead, your body prioritises speed and stability over perfect regeneration.
During healing, collagen fibres are often laid down in a more disorganised pattern. This is why you may notice scars that are raised, thickened, or sometimes slightly sunken. The final appearance depends on the balance between how much collagen your body produces and how effectively it breaks it down. If that balance shifts, the scar can become more noticeable.
Inflammation plays a central role in how your scar ultimately develops. If inflammatory signals are prolonged or exaggerated, scarring can become more severe. That is why modern treatments increasingly focus on regulating these pathways rather than simply treating the surface. By understanding how your body heals, therapies can become more targeted and effective.
Why Single-Modality Treatment Has Limitations
Traditional scar treatments often focus on a single mechanism of action. For instance, you might have laser therapy to improve surface texture, or steroid injections to calm inflammation. While these approaches can help, scars rarely stem from just one underlying issue. If only one factor is treated, you may notice improvement, but not complete correction.
A raised scar can involve excess collagen, increased blood vessel formation, and ongoing inflammation all at once. A depressed acne scar, on the other hand, may reflect collagen loss and structural tethering beneath the skin. If you address only one component, the overall result may remain partial. That is why an integrated, combination approach often offers greater potential, targeting multiple dimensions of scarring simultaneously.
The Role of Energy-Based Devices
Energy-based devices such as fractional lasers and radiofrequency systems help remodel scar tissue by stimulating your skin’s natural repair processes. They create controlled micro-injuries, which encourage collagen to reorganise in a more structured way. As your skin heals, texture can gradually become smoother and more even. You are essentially prompting your skin to rebuild itself more effectively.
With fractional laser treatment, tiny columns of skin are targeted while the surrounding tissue is left untouched. This selective approach allows you to heal more quickly and supports ongoing collagen renewal beneath the surface. Improvements tend to develop progressively rather than instantly. Over time, you may notice a steady refinement in texture and tone.
That said, lasers mainly address the structural side of scarring. They do not directly calm the inflammatory pathways that may be driving abnormal scar formation. If inflammation remains active, structural treatment alone may not fully resolve the issue. This is where biologic modulation becomes relevant, as it can help regulate the underlying immune signals influencing how your skin heals.
Microneedling and Collagen Induction
If you are exploring treatments for acne scars or skin texture concerns, microneedling is likely already on your radar. This technique works by creating controlled micro-injuries in the skin, triggering your body’s natural repair response. Rather than damaging the skin randomly, it stimulates a regulated wound-healing cascade that encourages collagen remodelling.
1. Stimulating collagen through controlled micro-punctures: During microneedling, fine needles create tiny, precise channels in your skin. These micro-punctures activate fibroblasts and stimulate collagen and elastin production. As new collagen forms, the skin gradually becomes firmer and more even in appearance, particularly in areas with atrophic or depressed scars.
2. Activating the wound-healing cascade in a controlled way: Your body naturally responds to injury by initiating inflammation, proliferation, and tissue remodelling phases. Microneedling harnesses this process in a measured and therapeutic manner. Because the injury is controlled and superficial, recovery is generally quicker than with more aggressive resurfacing procedures.
3. Enhancing topical delivery: The micro-channels created during treatment temporarily increase skin permeability. This allows topical agents such as growth factors, platelet-rich plasma (PRP), or biologic modulators to penetrate more effectively. When you combine microneedling with these agents, you may see enhanced regenerative outcomes.
4. Effective as a standalone therapy: If your scarring is mild, microneedling alone may produce noticeable improvement over multiple sessions. Gradual collagen induction can smooth texture and refine pores without significant downtime.
5. Amplified results through combination therapy: For deeper scars or more complex concerns, pairing microneedling with targeted treatments can amplify results. Integration with regenerative biologics or energy-based devices is becoming increasingly central in modern dermatology. This layered approach allows you to address structural damage from multiple angles.
In summary, microneedling works by activating your body’s own repair mechanisms to rebuild collagen and improve skin quality. While effective on its own for mild concerns, it often delivers stronger outcomes when thoughtfully combined with complementary therapies.
Biologic Pathway Modulation Explained
Biologic pathway modulation means targeting the specific molecular signals involved in how your scar forms. Certain cytokines, such as TGF-beta, play a major role in driving fibrosis and excess collagen production. If these signals become overactive, your body may lay down too much collagen, leading to thick or raised scars. By carefully controlling these pathways, treatment aims to reduce abnormal collagen deposition without disrupting normal healing.
Emerging therapies are designed to regulate these signals with precision rather than broadly suppressing the entire healing process. Instead of shutting healing down, they fine-tune its intensity so your tissue repair stays balanced. Looking ahead, you may see approaches that combine physical remodelling, such as laser therapy, with molecular regulation. By addressing both structure and signalling, outcomes could become more predictable and effective, with precision at the centre of care.
Targeting Fibrosis More Precisely
Excess fibrosis is what leads to hypertrophic scars and keloids, where your skin produces too much collagen during healing. At present, you might be offered treatments such as steroid injections or silicone therapy to help flatten and soften the scar. While these options can improve appearance, they do not directly target the deeper molecular drivers behind abnormal collagen production. As a result, recurrence or incomplete improvement can still occur.
New research is now exploring antifibrotic agents designed to inhibit excessive collagen formation at its source. By targeting specific growth factors involved in fibrosis, these therapies aim to prevent scar thickening before it becomes pronounced. Early clinical studies have shown encouraging signals, particularly in reducing scar volume and firmness. This more precise biological targeting could change how you approach high-risk scarring.
There is also growing interest in combining antifibrotic modulation with laser resurfacing. In this approach, structural remodelling improves texture while pathway suppression addresses the biological cause. By treating both the visible scar and the signalling driving it, you may achieve more durable results. This layered strategy reflects the direction of innovation in modern scar management.
Combining Lasers With Biologic Agents
Future treatment protocols may involve performing fractional laser therapy followed by topical or injectable biologic agents. When you undergo laser treatment, tiny microchannels are created in your skin. These channels can improve the penetration of applied therapies. As a result, the biologic agent may work more effectively at the target site.
Laser-induced remodelling stimulates collagen turnover and encourages your skin to rebuild itself. However, without guidance, new collagen can still form in an uneven pattern. By adding biologic modulation, you help ensure that collagen develops in a more balanced and controlled way. This combination supports healthier tissue architecture overall.
When structural stimulation and molecular regulation work together, outcomes may become more predictable. You are not just resurfacing the skin but also influencing how it heals at a cellular level. This dual approach addresses both appearance and underlying signalling. It represents a more strategic form of intervention.
Research is still ongoing to refine timing, dosage, and sequencing. Determining when to introduce the biologic agent in relation to laser treatment may significantly influence results. Careful protocol design aims to maximise synergy between the two methods. With precise planning, you may achieve smoother texture and more durable improvement over the long term.
Improving Pigmentation in Scars
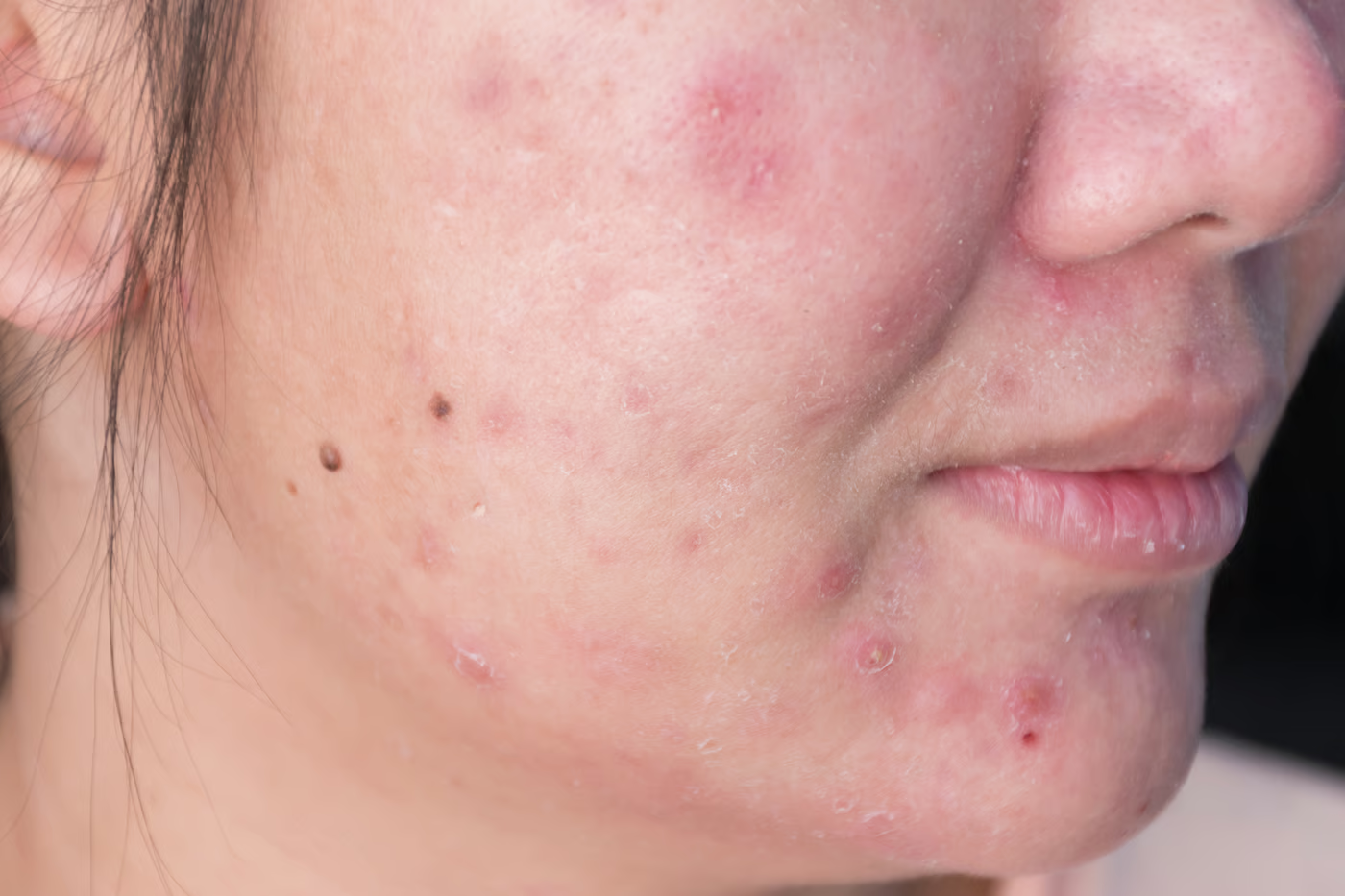
Scars often involve changes in pigmentation as well as texture. Even if you improve the surface smoothness, post-inflammatory hyperpigmentation or hypopigmentation can still persist. That means your skin tone may remain uneven despite structural progress. Combination therapy aims to address both colour and texture together, rather than treating them separately.
Energy-based devices can help reduce excess pigmentation by specifically targeting melanin within the skin. At the same time, anti-inflammatory modulation works to reduce the triggers that cause recurring pigment changes. By calming the inflammatory pathways, you lower the risk of further discolouration. This dual strategy helps you move closer to a more uniform skin tone.
Looking ahead, pigmentation treatment may become even more personalised. Biomarkers could guide how intense or frequent your therapy should be. Instead of a one-size-fits-all approach, protocols may be tailored to your skin’s specific response patterns. This integrated strategy aims to improve overall aesthetic outcomes in a more precise and predictable way.
Managing Acne Scars With Combination Therapy
If you are dealing with acne scars, you already know they are rarely simple. Scars can involve volume loss (atrophy), fibrous bands pulling the skin downward (tethering), and changes in pigmentation. Because these elements develop through different biological processes, relying on a single treatment often delivers limited improvement.
1. Addressing multiple scar components at once: Acne scars do not form from just one mechanism. You may have depressed areas from collagen loss, tight bands anchoring scars downward, and uneven pigmentation layered on top. Treating only the surface will not correct deeper structural issues.
2. Subcision to release tethered tissue: Subcision works by mechanically breaking the fibrous bands beneath your scar that pull the skin inward. Once released, the skin can lift naturally. This step is particularly useful for rolling scars and improves the foundation before additional treatments.
3. Laser resurfacing to stimulate collagen: Laser therapies create controlled thermal injury in the skin, triggering collagen remodelling. Over time, this can smooth texture and improve atrophic depressions. When used after subcision, lasers help reinforce structural improvement by encouraging new collagen formation.
4. Biologic modulation to regulate inflammation: Biologic agents or regenerative treatments can help control inflammation and optimise healing. By influencing your skin’s repair response, these therapies may enhance collagen quality and reduce the risk of excessive post-treatment pigmentation or scarring.
5. Layered therapy mirrors how scars form: Scars develop through a cascade of inflammation, tissue breakdown, and uneven repair. A layered treatment strategy mirrors this complexity by addressing each contributing factor. Rather than targeting one surface feature, you are supporting structural, cellular, and pigment correction together.
In the end, combination therapy acknowledges that your scars are multi-dimensional. By integrating subcision, laser resurfacing, and biologic support, you create a more comprehensive correction strategy. When treatment addresses both depth and surface, results tend to be more meaningful.
Radiofrequency and Controlled Thermal Injury
Radiofrequency devices work by delivering controlled heat to your dermis, stimulating collagen contraction and remodelling. This process can gradually improve firmness and skin texture, giving your scars a smoother, more supported appearance. When combined with microneedling, the energy reaches deeper layers, further enhancing collagen reorganisation and structural support over time.
Adding biologic modulation to this approach can refine how your skin heals. Instead of forming excessive fibrosis, collagen develops in a more balanced and organised pattern. By addressing both structural and molecular aspects of healing, this combined strategy represents the future of scar management, creating more predictable and durable results for you.
Timing and Sequencing in Combination Protocols
The order in which treatments are delivered can make a big difference in how well they work for you. For example, laser therapy may be performed first to create microchannels, allowing a biologic agent to penetrate more effectively. In other cases, biologic modulation might be used beforehand to prepare the tissue and calm inflammation before energy-based treatment. Getting the sequence right helps maximise effectiveness.
Understanding your skin’s healing timeline is crucial when planning combination therapy. If treatments are applied too quickly or too frequently, you could trigger excess inflammation, which may worsen scarring. Controlled spacing between sessions gives your tissue time to respond and remodel properly. This careful pacing can make results more reliable and consistent.
Future research is focused on standardising the timing and sequencing of these protocols. Evidence-based guidance will help ensure that you receive therapy at the optimal moment for both safety and effectiveness. As protocols are refined, combination approaches are likely to become more predictable, precise, and tailored to your individual healing response.
Personalised Scar Mapping
Advanced imaging techniques are making personalised scar mapping increasingly possible for you. Tools like optical coherence tomography and high-resolution photography can assess the depth, density, and overall structure of your scars. By visualising these details, clinicians can plan treatment with much greater precision, tailoring approaches to your skin’s specific needs.
Different areas of a single scar may respond better to different treatments. For example, one zone might benefit from laser resurfacing, while another may require a targeted injection or topical therapy. By individualising treatment in this way, you can get more efficient and effective results, addressing each component of the scar appropriately.
Personalised scar mapping fits perfectly with the principles of precision medicine. Not all scars behave the same way, and a one-size-fits-all approach often falls short. By customizing therapy to your scar’s unique characteristics, the chances of achieving smoother, more uniform skin are significantly improved.
Reducing Recurrence in Keloid Scars
If you’ve ever struggled with Keloid scars, you’ll know how frustrating they can be. Unlike typical scars, keloids have a high tendency to come back even after treatment. Standard approaches like steroid injections, cryotherapy, or laser therapy can help, but recurrence remains a major challenge.
1. High recurrence makes keloids tricky to manage: Even after apparently successful treatment, keloids can regrow. The underlying fibrotic pathways driving excess collagen production remain active, which means you may need repeated interventions if the cause isn’t addressed directly.
2. Emerging biologics target fibrotic pathways: New biologic therapies are being developed to interfere with the molecular signals that promote keloid formation. By modulating key fibrotic pathways, these agents aim to reduce the chance of relapse. For you, this could mean more durable results and fewer repeat treatments.
3. Combination with energy-based therapies: Pairing biologics with lasers or other energy-based treatments can stabilise the results of scar correction. While lasers remodel tissue and reduce bulk, biologics act at the cellular level to prevent overproduction of collagen. This dual approach targets both existing scars and the processes that cause recurrence.
4. Early intervention improves outcomes: Acting quickly when a keloid begins to form can prevent it from growing larger. Prompt modulation of inflammatory signalling and fibrotic activity can limit expansion and make treatment more effective. The sooner you address abnormal scar formation, the better your long-term control.
5. Prevention is as important as correction: Managing keloids isn’t just about reducing existing scars it’s about stopping them from returning. By combining proactive care, targeted biologics, and conventional therapies, you have a higher chance of maintaining smooth, stable skin over time.
In conclusion, reducing keloid recurrence requires a multi-layered strategy. Emerging biologics, when combined with energy-based treatments and early intervention, offer hope for more lasting results. For you, this means fewer setbacks, less frustration, and improved long-term confidence in your skin.
Long-Term Collagen Quality
The quality of collagen in your skin plays a major role in how your scar looks over time. When collagen fibres are disorganised, scars can appear raised, lumpy, or uneven. Future therapies aim not just to increase collagen but to influence how those fibres align, creating a smoother and more natural appearance. By focusing on fibre structure, treatment can improve both texture and long-term outcomes.
Energy-based devices help stimulate new collagen formation, while biologic modulation can guide how it arranges itself within the tissue. When collagen remodelling is balanced, your scar develops with better structural harmony, enhancing durability. By combining these approaches, integrated therapy addresses both the formation and organisation of collagen, giving you more consistent and lasting improvement.
Safety Considerations in Combination Treatment
Combining multiple treatment modalities for scars requires careful planning to keep you safe. If therapies are applied too aggressively or too close together, there’s a higher risk of excessive inflammation or changes in pigmentation. Regular monitoring throughout your treatment ensures that your skin responds well and that progress remains safe and controlled.
Experienced clinicians tailor both the intensity and timing of each intervention to suit your specific scar. Not every area or type of scar needs aggressive combination therapy, so individual assessment is essential. By adjusting treatment based on your response, they can optimise results while minimising risks.
Looking ahead, future protocols are likely to place even more emphasis on safety data. Evidence-based guidelines will help ensure that innovations are applied responsibly. With precision planning, combination therapy can deliver effective results while reducing the likelihood of complications for you.
Artificial Intelligence in Scar Treatment Planning
Artificial intelligence is starting to play a role in scar treatment planning, helping you and your clinician understand complex scar patterns more precisely. Machine learning can analyse how different scars respond to various therapies and predict which combination is likely to work best. This data-driven approach adds a new level of precision to your treatment planning.
By examining large datasets, AI may identify optimal protocols for different scar types. It can also help refine dosing intervals, energy settings, and treatment intensity, tailoring each session to your skin’s specific needs. Technology doesn’t replace clinician expertise but enhances it, giving your care a smarter, more informed foundation.
Digital integration represents the next step in personalised dermatology. Scar management is likely to become increasingly customised, with AI guiding decisions that previously relied solely on experience. Innovation continues to evolve, offering you more precise, effective, and predictable outcomes.
Patient Expectations and Realistic Outcomes
Even with advanced combination therapies, it’s important for you to understand that complete scar removal is rarely achievable. The goal is improvement rather than perfection, and having clear expectations can help you feel more satisfied with the results. Recognising what is realistic ensures you approach treatment with confidence and patience.
Combination therapy can still make a significant difference in texture, tone, and overall appearance. Changes happen gradually over months as collagen remodels and your skin heals. While progress may be incremental, the aesthetic benefits can be meaningful. Staying patient and consistent with treatment is key to achieving the best possible outcome for you.
FAQs:
1. What makes combination scar therapy different from traditional treatments?
Combination therapy addresses multiple factors at once, like texture, pigmentation, and inflammation. Instead of focusing on just one aspect, you get a more comprehensive approach that can lead to better and longer-lasting results.
2. How do scars form and why can they be uneven?
Scars form when your body rapidly repairs skin, producing collagen in a disorganised way. Inflammation and collagen imbalance can make scars raised, thick, or sunken, which is why targeted treatment is necessary to improve both structure and appearance.
3. What role do lasers play in scar management?
Lasers create controlled micro-injuries that stimulate your skin to remodel collagen in a more organised way. They improve texture and tone gradually but don’t directly calm the inflammation driving abnormal scarring.
4. How does microneedling improve scars?
Microneedling creates tiny channels in your skin to trigger collagen and elastin production. It also helps topical treatments penetrate better, making it effective alone for mild scars and even more so when combined with other therapies.
5. What is biologic pathway modulation?
Biologic modulation targets the molecular signals that drive abnormal collagen production. By fine-tuning these pathways, treatment can reduce excessive scarring without disrupting normal healing, improving both safety and results.
6. Can combination therapy help with acne scars?
Yes, acne scars often involve volume loss, tethering, and pigmentation. Combining subcision, laser resurfacing, and biologic modulation addresses all these layers, giving you smoother, more uniform skin than a single treatment could.
7. How are keloid scars treated with emerging therapies?
New biologics target the fibrotic pathways that cause keloids to recur. When combined with energy-based devices like lasers, this dual approach helps prevent regrowth and offers more durable, long-term improvement.
8. How does collagen quality affect long-term outcomes?
The organisation of collagen fibres determines how your scar looks over time. Treatments that stimulate balanced collagen remodelling can make scars smoother and more natural, rather than just adding bulk without structure.
9. Is safety a concern with multiple therapies?
Yes, combining treatments needs careful planning. Too aggressive or poorly timed sessions can increase inflammation or pigment changes. Clinicians monitor progress and adjust intensity to keep you safe while optimising results.
10. How might AI influence future scar treatment?
AI can analyse scar patterns and predict which combination therapies will work best for you. By refining treatment timing, energy settings, and protocols, it helps make care more personalised, precise, and potentially more effective.
Final Thoughts: Advancing Scar Care Through Combination Therapy
Understanding that scars are multi-dimensional is key to achieving meaningful improvement. Modern approaches that combine lasers, microneedling, and biologic modulation target both the visible structure and the underlying molecular signals driving abnormal healing. While no treatment can completely erase scars, carefully designed combination therapy can improve texture, tone, and long-term collagen quality, providing more predictable and durable results. If you’d like to book a consultation with one of our dermatologists in London, you can contact us at the London Dermatology Centre.
References:
1. Lin, X. & Lai, Y. (2024) ‘Scarring skin: mechanisms and therapies’, International Journal of Molecular Sciences, 25(3), 1458. https://www.mdpi.com/1422-0067/25/3/1458
2. Clementi, A. (2025) ‘Combined laser strategies for scar treatment’, MDPI Bioengineering, 12(12), 1368. https://www.mdpi.com/2306-5354/12/12/1368
3. Deflorin, C., Hohenauer, E., Stoop, R., et al. (2020) ‘Physical management of scar tissue: a systematic review and metaanalysis’, Journal of Alternative and Complementary Medicine, 26(10), pp.854–865. https://pubmed.ncbi.nlm.nih.gov/32589450/
4. Juhasz, M. & Cohen, J.L. (2020) ‘Microneedling for the treatment of scars: an update for clinicians’, Clinical, Cosmetic. https://pubmed.ncbi.nlm.nih.gov/33376377/
5. Fernandes, M.G., da Silva, L.P., Cerqueira, M.T., et al. (2022) ‘Mechanomodulatory biomaterials prospects in scar prevention and treatment’, Acta Biomaterialia, 150, pp.22–33. https://www.sciencedirect.com/science/article/pii/S1742706122004445