Over the past decade, biologic therapies have fundamentally changed dermatology. If you live with chronic inflammatory skin disease, you may already be familiar with treatments targeting specific immune pathways. Conditions such as psoriasis, atopic dermatitis, and hidradenitis suppurativa have seen dramatic improvements with targeted biologics.
However, progress has not stopped. Even as current biologics deliver excellent results, researchers are already developing next-generation therapies that aim to be more precise, faster acting, and potentially safer. The field continues to evolve rapidly.
In this article, we explore emerging biologics, novel pathway inhibitors, and early clinical trial developments shaping the next phase of dermatologic care. Understanding what lies ahead helps you appreciate how personalised and targeted treatment is becoming. The future of dermatology is increasingly immune-specific and data-driven.
How Biologics Transformed Dermatology
Biologics work by targeting specific parts of your immune system rather than suppressing it as a whole. Instead of dampening everything down, they block individual cytokines or receptors that drive inflammation. This targeted approach makes treatment far more precise. For many patients, that precision has led to significantly better outcomes.
Before biologics became widely available, you would often be prescribed systemic immunosuppressants. While these treatments could control the disease, they tended to affect the entire immune system and carried broader side-effect risks. The arrival of targeted therapies shifted that balance. You could achieve control with greater specificity and, in many cases, improved safety profiles.
If you live with moderate-to-severe psoriasis, for example, biologics have likely changed what you can expect from treatment. Many patients now achieve near-clear skin, something that was far less common in the past. As results improved, so did overall quality of life. In many ways, biologics have reshaped how you think about long-term disease management.
The Current Landscape of Approved Biologics
Today, biologics mainly target key immune pathways like TNF-alpha, IL-17, IL-12/23, and IL-23. These molecules are central to the inflammation that drives skin conditions such as psoriasis. By blocking them, you can reduce immune-driven skin inflammation and see real improvement in your symptoms.
If you have atopic dermatitis, treatments often focus on the IL-4 and IL-13 pathways. In psoriasis, IL-23 inhibitors have shown impressive results. These targeted therapies have really transformed what modern care can do for you.
Even with these advances, not everyone responds fully. You might notice only partial improvement, or the effect may fade over time. Next-generation therapies are designed to address these gaps and give you better long-term outcomes.
Why New Biologics Are Still Needed
You might wonder if we already have effective biologic treatments, why keep developing new ones? The reality is that even the best therapies do not work perfectly for everyone. Some people do not respond as expected, others lose response over time, and some struggle with side effects or inconvenient dosing schedules. As our understanding of the immune system deepens, it becomes clear that more precise and flexible treatment options are still needed.
1. You may not achieve a complete response: Even with advanced biologics, you might only see partial improvement. In some cases, symptoms persist despite treatment. This happens because different immune pathways can drive disease in different individuals. New biologics target alternative mechanisms, giving you additional options if one approach does not work fully.
2. You could lose response over time: Sometimes a biologic works well initially, but its effect gradually declines. Your immune system may adapt, or the disease may shift pathways. When this happens, having access to newer agents with different targets becomes essential for maintaining long-term control.
3. Side effects may limit long-term use: While biologics are more targeted than traditional systemic therapies, you may still experience infections, injection-site reactions, or other adverse effects. Safer, more selective treatments aim to reduce these risks and improve your overall treatment experience.
4. Convenience matters in real life: If you need frequent injections or clinic visits, treatment can feel burdensome. More convenient dosing schedules, longer-acting formulations, and alternative delivery systems are being developed to better fit into your daily routine.
5. Some conditions still lack strong targeted options: Diseases such as Alopecia areata and Vitiligo have only recently begun to see biologic-level innovation. If you are living with these conditions, expanded precision therapies may offer new hope where limited options previously existed.
6. Your immune system is highly complex: Blocking one pathway may not fully control disease activity in every person. Your immune response operates through multiple overlapping systems. Researchers are now exploring deeper pathway mapping and combination strategies to create treatments that are more personalised and effective for you.
In the end, new biologics are not about replacing what already works they are about expanding your options. Greater precision, improved safety, and more flexible dosing give you a better chance of achieving consistent and lasting disease control.
Targeting IL-36 and Rare Inflammatory Conditions
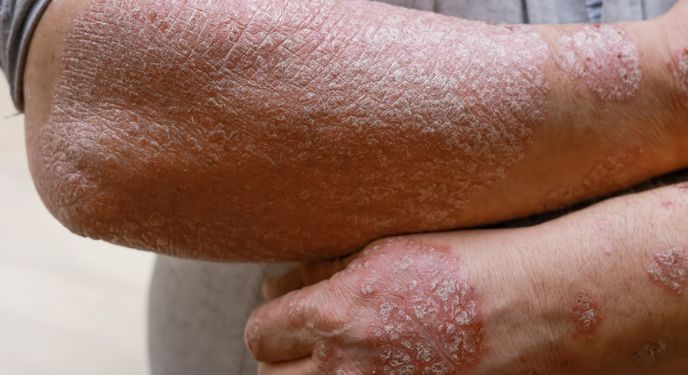
Targeting the IL-36 pathway is becoming a key focus in inflammatory dermatology. IL-36 plays a central role in rare but severe conditions, such as generalised pustular psoriasis. By blocking this pathway, researchers aim to interrupt the specific inflammatory signals driving the disease. Early clinical trials have shown encouraging results, especially in reducing acute flare symptoms.
Next-generation IL-36 inhibitors are designed to act quickly during severe flares. Early data suggest they may provide faster control compared with older systemic therapies. This represents a shift towards more crisis-focused biologic treatment. Rather than broadly suppressing your immune system, these therapies target the immediate inflammatory trigger.
For patients living with rare inflammatory subtypes, this precision is especially valuable. You get treatment that directly targets the main driver of inflammation, without unnecessary wider immune suppression. As research advances, therapies are becoming increasingly specific and personalised, reflecting a broader move towards refined, individualised care.
Dual-Pathway Inhibitors
Researchers are now exploring biologics that target more than one pathway at the same time. These dual inhibitors can block two cytokines with a single therapy, aiming to give you better results without increasing side effects. By addressing overlapping inflammatory pathways, they may help reduce partial responses that some patients experience with single-target treatments.
These therapies might also lower the risk of your body losing response over time. Early-phase trials are ongoing to understand their safety and effectiveness. Dual-pathway inhibitors represent a natural step forward in precision medicine.
Instead of simply increasing dosage, these treatments work smarter by modulating the immune system in a more tailored way. This approach could improve how long the therapy remains effective and provide more durable control of inflammation for you.
Biologics for Hidradenitis Suppurativa
Hidradenitis suppurativa (HS) can be particularly challenging to manage, especially if you are living with recurring pain and inflammation. While current biologics have improved outcomes for many patients, response rates can still vary. That means you may not always achieve the level of control you hope for with first-line options. As a result, researchers are continuing to explore additional inflammatory targets involved in HS.
Newer treatments are investigating pathways such as IL-17 and IL-1, both of which play a role in driving inflammation. Early studies suggest that inhibiting these pathways may improve lesion control in certain patients. This growing body of research helps doctors better understand why you might respond well to one therapy but not another. Broader immune mapping is now guiding more informed treatment decisions.
HS research highlights an important lesson: one pathway does not suit every inflammatory disorder. If you have HS, your condition may involve a slightly different immune signature compared with other diseases. Next-generation biologics aim to close this gap by offering more disease-specific targeting. Over time, this approach could mean more personalised and effective care for you.
Advances in Atopic Dermatitis Treatment
Atopic dermatitis treatment has expanded rapidly in recent years, giving you more options than ever before. While IL-4 and IL-13 inhibitors marked a major breakthrough, newer biologics are now targeting IL-31 and other itch-related pathways. This shift reflects a growing focus on the symptoms that affect you most day to day. Reducing itch directly has become a central therapeutic goal.
Chronic pruritus can seriously disrupt your sleep, concentration, and overall wellbeing. By targeting itch-specific cytokines, these newer therapies aim to improve both comfort and quality of life. Early clinical trials have shown encouraging results, particularly in reducing persistent itching. For many patients, that relief can make a meaningful difference in daily functioning.
Precision therapy in atopic dermatitis continues to evolve. The goal is not only to reduce visible eczema severity but also to improve your overall daily experience. Personalised pathway selection is becoming increasingly important in guiding treatment decisions. As research advances, your care is likely to become more tailored and symptom-focused.
JAK Inhibitors and Small Molecule Alternatives
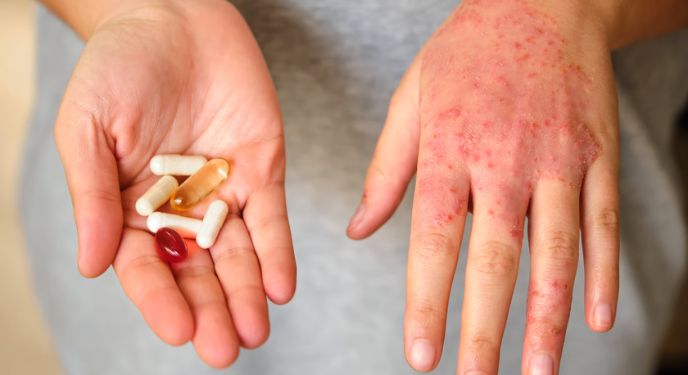
Although they are not traditional biologics, JAK inhibitors represent an important form of targeted immune therapy. If you prefer an oral option over injections, these small-molecule agents may offer greater convenience. They work by blocking intracellular signalling pathways that drive inflammation. In doing so, they expand your treatment options beyond injectable biologics.
Selective JAK inhibition aims to reduce systemic risk while maintaining strong efficacy, and refinement of pathway specificity is still ongoing. As researchers deepen their understanding, you may see combination strategies emerge, where biologics and small molecules complement one another. The goal is to balance safety with meaningful disease control. Integrated immune modulation is becoming an increasingly important concept in modern inflammatory care.
Personalised Dermatology Through Biomarkers
The future of dermatology is moving towards treatment plans that are tailored specifically to you. Instead of selecting a biologic based mainly on general guidelines or past experience, doctors may soon rely more heavily on measurable biological signals known as biomarkers.
1. Biomarkers may guide biologic selection: In the future, your treatment could be chosen based on specific biomarkers detected in your blood or tissue samples. These markers might reveal which inflammatory pathways are driving your disease. By identifying the dominant mechanism, clinicians can match you with a biologic that directly targets that pathway.
2. Genetic profiling could enhance precision: Genetic analysis may help determine how your immune system behaves and how you are likely to respond to certain therapies. This deeper understanding allows for more strategic drug selection. Rather than applying a broad approach, treatment becomes biologically informed and personalised to you.
3. Reducing trial-and-error prescribing: At present, treatment selection often involves a process of trial and response. You may try one biologic, assess improvement, and switch if the results are insufficient. Biomarker-guided therapy has the potential to reduce this uncertainty by predicting response before treatment begins.
4. Minimising unnecessary exposure: When therapy is more accurately matched, you are less likely to be exposed to ineffective medications. This reduces the risk of avoidable side effects and limits delays in achieving disease control. Precision benefits both safety and speed of response.
5. Improving efficiency and outcomes: Personalised medicine aims to increase both effectiveness and healthcare efficiency. By selecting the right therapy earlier, you may achieve faster improvement and better long-term stability. This approach also reduces healthcare resource burden.
In conclusion, biomarker-driven dermatology represents the next frontier in precision medicine. By using biological data to guide treatment decisions, care becomes more targeted and predictable. As research advances, you can expect dermatology to continue shifting towards smarter, more individualised therapy selection that prioritises both efficacy and safety.
Long-Acting Biologics
Next-generation biologics are being designed with longer dosing intervals, which could make a real difference to your treatment routine. With extended half-lives, you may only need an injection every few months rather than every few weeks. That added spacing can make therapy feel far less intrusive. For many patients, this kind of flexibility improves adherence and overall confidence in long-term management.
When you reduce how often you need injections, your quality of life often improves as well. Fewer clinic visits or self-injections can ease both physical and mental burden. It may also reduce pressure on healthcare systems, making care more efficient. Convenience might seem minor, but for you, it can play a meaningful role in treatment success.
Long-acting biologics are designed to maintain more stable immune modulation over time. With fewer peaks and troughs in drug levels, you may experience fewer flare-ups. This steady control can help you feel more consistent in how your condition is managed. As dosing innovation continues to evolve, your treatment experience is likely to become even more streamlined and patient-friendly.
Safety Optimisation in New Therapies
Improving safety is a major focus in the development of new therapies. By selectively targeting specific inflammatory pathways, these treatments reduce the risk of infections and other complications. Narrower pathway inhibition limits off-target effects, helping you get effective relief without unnecessary immune suppression.
Clinical trials play a key role in tracking long-term safety, with data collection continuing beyond initial approval. Post-marketing surveillance adds real-world insight into how these therapies perform over time. Transparent reporting helps build your confidence and trust in the treatment.
Next-generation biologics aim to combine strong efficacy with minimal systemic risk. Precision is central to this approach, ensuring therapies remain both effective and safer. This careful targeting represents the future of inflammatory disease management.
Biologics in Alopecia Areata
If you are following developments in hair disorders, you may have noticed how quickly research into Alopecia areata has progressed in recent years. What was once considered a difficult and unpredictable condition is now being studied with far greater biological clarity. Researchers better understand how immune cells target hair follicles and disrupt their normal growth cycle.
1. Deeper understanding of immune mechanisms: Scientists now recognise that alopecia areata involves immune-mediated disruption of hair follicle immune privilege. In simple terms, your immune system mistakenly identifies hair follicles as targets. Understanding the cytokines and signalling pathways involved allows for more precise therapeutic intervention.
2. Targeted inhibitors entering advanced trials: Several pathway-specific inhibitors are progressing through late-stage clinical trials. These therapies aim to block key inflammatory signals responsible for follicle attack. Rather than broadly suppressing immunity, they focus on the specific drivers of hair loss.
3. Encouraging early regrowth results: Early clinical data has shown meaningful hair regrowth in selected patients. While responses vary, some individuals experience substantial improvement in scalp coverage. For a condition historically associated with limited options, this progress represents genuine hope.
4. Restoring immune privilege: One central goal of new therapies is to restore the protective immune environment around the hair follicle. By calming the inappropriate immune response, follicles may return to normal growth cycles. This targeted modulation is more strategic than older systemic treatments.
5. Expanding biologic innovation beyond psoriasis and eczema: Immune-modulating therapies were once primarily associated with conditions such as Psoriasis and Eczema. Now, biologic innovation is extending into hair disorders and other dermatological fields. This shift reflects a broader understanding of immune-driven skin and follicular disease.
In conclusion, biologic development in alopecia areata signals an important expansion in dermatology. As immune pathways become clearer, targeted therapies are offering new possibilities where options were previously limited. For you, this means a future where hair disorders are treated with the same precision.
Vitiligo and Immune Targeting
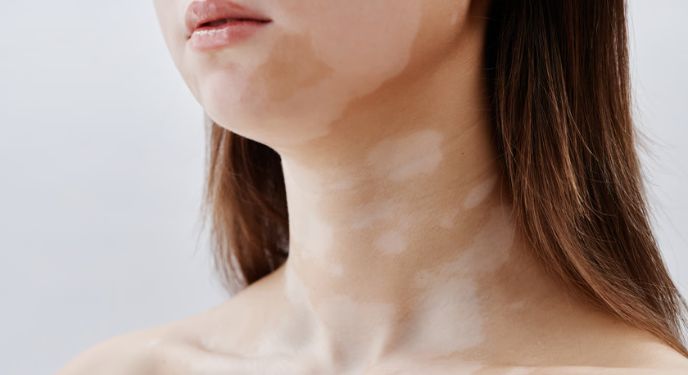
Vitiligo develops when your immune system mistakenly targets and destroys melanocytes, the cells responsible for skin pigment. Researchers are now exploring targeted therapies that interrupt the specific immune pathways involved in this process. Rather than using broad immunosuppression, these newer approaches focus on the signals driving pigment loss. Early-stage studies have shown encouraging signs of repigmentation in some patients.
By selectively calming the immune response, targeted treatments may help stabilise the progression of vitiligo. In some cases, combining biologic-style therapies with light treatment appears to enhance results. This multimodal approach means you are not relying on a single strategy alone. Instead, treatments are being layered to improve both control and pigment recovery.
Vitiligo research reflects a broader shift in how autoimmune skin diseases are understood and managed. As scientists refine pathway-specific targeting, your treatment options are becoming more precise. The goal is not only to halt disease activity but to support visible improvement. Innovation in this area is advancing steadily, offering cautious but genuine optimism.
Early Clinical Trial Data
In early Phase I and II trials, researchers focus on safety and early signs of effectiveness, helping you understand whether a new therapy shows real potential. Many emerging biologics have already demonstrated promising lesion reduction at this stage. However, it is the larger Phase III trials that confirm how durable and safe those results are over time. This step-by-step process ensures that when a treatment reaches you, it has been carefully evaluated.
Trial endpoints are also evolving to reflect what truly matters in daily life. In addition to clinical measures, quality-of-life scores and patient-reported outcomes now carry much greater weight. That means your experience, comfort, and overall wellbeing are part of how success is defined. With an active research pipeline and new agents continually entering development, progress continues to reflect a deeper understanding of immunology and more patient-centred care.
Cost and Accessibility Considerations
Biologics are complex medicines to manufacture, and that complexity often drives up cost. In many healthcare systems, you may find that access is limited by funding or reimbursement policies. Even when a treatment is highly effective, affordability can become a real barrier. Over time, biosimilars may help improve accessibility by offering more cost-effective alternatives.
As patents expire, competition typically increases, which can bring prices down. That shift may gradually expand access so more patients like you can benefit from advanced therapies. Wider availability supports more equitable care across different regions and healthcare settings. Still, changes in pricing and policy do not happen overnight.
Innovation must balance strong clinical efficacy with long-term affordability. If treatments are not economically sustainable, access may remain uneven. Healthcare economics plays a significant role in determining what is realistically available to you. Ultimately, progress in medicine must consider both scientific advancement and practical accessibility.
Combination Therapy Strategies
Future dermatologic care may increasingly involve combination regimens tailored to your specific condition. Rather than relying on a single therapy, you may use a biologic alongside a topical treatment or a small-molecule agent. This layered approach aims to optimise disease control from multiple angles. When treatment is personalised in this way, you may achieve more consistent and effective results.
That said, combination strategies must be studied carefully before becoming routine. If you are using more than one immune-modulating therapy, safety and cumulative immune effects need thorough evaluation. Clinical trials assess how these treatments interact and whether risks increase. Evidence, rather than enthusiasm alone, will ultimately guide best practice.
The overall goal is durable remission with as little treatment burden as possible for you. Intelligent combination therapy may help maintain control while reducing flare frequency. Ideally, this means fewer disruptions to your daily life. Research in this area continues to evolve, shaping a more precise and balanced future for care.
The Role of Artificial Intelligence
Artificial intelligence is starting to make a real impact in dermatology research, and its influence continues to grow. AI-driven analysis helps researchers identify potential therapeutic targets that might otherwise be missed. By examining large datasets, patterns within immune pathways become clearer and more measurable. This deeper understanding strengthens discovery and opens new avenues for treatment development.
Machine learning is also improving how clinical trials are designed and run. Predictive modelling can help select the right patients for the right studies, increasing efficiency and relevance. This ensures that trials are more targeted and informative.
With AI increasingly integrated into research and care, dermatology is becoming more data-informed. Digital tools are enhancing both scientific discovery and precision medicine. For you, this means treatments are likely to become smarter, more personalised, and better tailored to individual needs.
FAQS:
1. What are next-generation biologics in dermatology?
Next-generation biologics are newer targeted therapies designed to improve on existing treatments. They focus on very specific immune pathways that drive your condition, aiming to be more precise, faster acting, and potentially safer. The idea is to tailor treatment more closely to how your immune system behaves.
2. Why are new biologics needed if current ones already work?
Current biologics work very well for many people, but you might not achieve full clearance or you could lose response over time. Some patients also experience side effects or find dosing inconvenient. New therapies give you more options and improve the chances of long-term control.
3. How are emerging biologics more precise?
Newer biologics target narrower and more clearly defined inflammatory signals. Instead of broadly dampening parts of your immune response, they focus on the specific cytokines driving your disease. This precision may help reduce unnecessary immune suppression.
4. What are dual-pathway inhibitors?
Dual-pathway inhibitors block two inflammatory pathways at the same time. If your condition is driven by overlapping immune signals, this approach may improve effectiveness without increasing overall drug exposure. It is a smarter way of targeting inflammation.
5. How could new biologics help in hidradenitis suppurativa?
Research is exploring additional pathways such as IL-17 and IL-1 that may be central in hidradenitis suppurativa. If your immune profile differs from others, these targeted options could offer better control and fewer flares over time.
6. Are there new treatments for itch in atopic dermatitis?
Yes, newer biologics are targeting itch-specific pathways like IL-31. If persistent itching affects your sleep or daily comfort, these therapies aim to address that symptom directly rather than only improving visible eczema.
7. Where do JAK inhibitors fit in?
JAK inhibitors are targeted oral treatments that block inflammatory signals inside your cells. If you prefer tablets to injections, they may feel more convenient. Ongoing research aims to improve their safety and selectivity.
8. How might biomarkers change treatment selection?
Biomarkers could help identify which immune pathway is most active in your condition. This means your doctor may one day choose a biologic based on measurable data rather than trial and error, making treatment more personalised.
9. What are long-acting biologics?
Long-acting biologics are designed to require fewer injections, sometimes only every few months. If frequent dosing feels burdensome, this could make treatment easier to manage while maintaining steady disease control.
10. Will cost affect access to these new treatments?
Biologics are expensive to develop and manufacture, which can limit access depending on funding systems. Over time, biosimilars may improve affordability, but economic factors will continue to influence what is available to you.
Final Thoughts: The Future of Targeted Skin Treatment Is Becoming Personal
The next generation of biologics is not just about stronger medication it is about smarter treatment that works with your immune system rather than simply suppressing it. As research moves towards biomarker-guided prescribing, dual-pathway inhibitors, longer-acting formulations and highly selective targeting, you are likely to see care that feels far more tailored to your individual condition. That means fewer delays in finding the right therapy, better long-term stability, and treatment plans designed around your daily life rather than the other way around.
If you are considering a consultation with a dermatologist in London, you can get in touch with us at the London Dermatology Centre. Personalised specialist guidance ensures your treatment plan reflects the latest advances while remaining carefully tailored to your specific needs.
References:
1. Ordaz-Rodriguez, J., et al. (2024) ‘Inflammatory memory in chronic skin disease’, Journal of Investigative Dermatology. https://pubmed.ncbi.nlm.nih.gov/38708420/
2. Elewski, B.E. (2011) ‘Eczema (Atopic Dermatitis)’, The New England Journal of Medicine. https://pubmed.ncbi.nlm.nih.gov/21913202/
3. Gonzalez, A. and Ruiz, I. (2024) ‘Inflammation and psoriasis: a comprehensive review’, International Journal of Molecular Sciences, 24(22), 16095. https://www.mdpi.com/1422-0067/24/22/16095
4. Smith, C. and Lee, Y. (2024) ‘Current landscape of chronic inflammatory dermatoses’, International Journal of Molecular Sciences, 46(9), 611. https://www.mdpi.com/1467-3045/46/9/611
5. Silverberg, J.I. and Gelfand, J.M. (2024) ‘Atopic dermatitis: chronic relapsing–remitting patterns. https://www.sciencedirect.com/science/article/abs/pii/S0140673624025194
