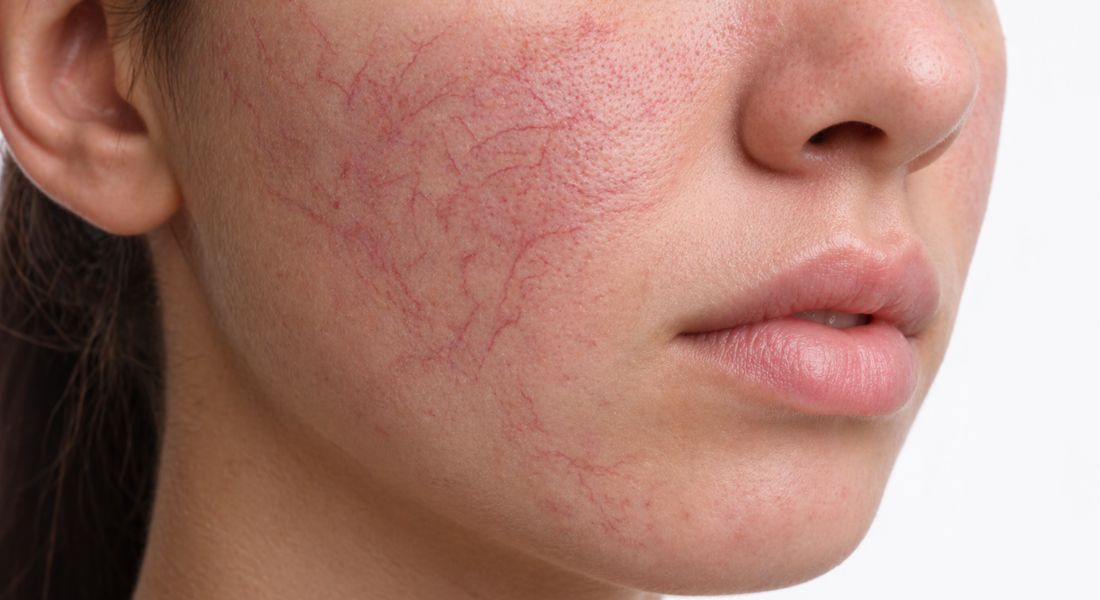
If you have treated broken capillaries and then noticed them returning, you are not alone. Many people feel frustrated when redness or visible vessels reappear after what seemed like a successful treatment. Understanding why this happens is important, as it helps set realistic expectations and supports better long-term skin care decisions.
Broken capillaries, also known as telangiectasia, are small dilated blood vessels that sit close to the surface of the skin. Treatments such as laser or light therapy are highly effective at removing these visible vessels. However, they only target the existing capillaries they do not prevent new ones from forming over time. This is why recurrence can occur, even after good initial results.
In this article, we will explain the main reasons broken capillaries can come back after treatment, including lifestyle factors, skin sensitivity, and underlying conditions. We will also explore practical steps you can take to reduce recurrence and maintain clearer skin. The aim is to give you a clear, realistic understanding so you can approach treatment with confidence rather than disappointment.
What Are Broken Capillaries and Why Do They Form?
Broken capillaries are tiny blood vessels that become enlarged and visible just beneath the surface of the skin. Often referred to as telangiectasia, they commonly appear on the nose, cheeks, and chin where the skin is thinner and more exposed. Although they are medically harmless, they can affect the overall appearance of the skin and are a frequent cosmetic concern.
These vessels form when the capillary walls weaken or lose their elasticity. Factors such as genetics, repeated flushing, sun exposure, and environmental stress can all contribute to this process. Over time, the vessels lose their ability to contract properly, so they remain dilated and visible rather than returning to their normal size.
It is important to understand that treating visible capillaries does not change your skin’s underlying tendency to develop new ones. Even after successful removal, new vessels can form if the same triggers continue to affect your skin. This is why broken capillaries are often considered an ongoing condition rather than a one-time issue, requiring both treatment and long-term management.
How Laser and Light Treatments Remove Capillaries

Modern treatments for broken capillaries including vascular lasers and intense pulsed light (IPL) are designed to precisely target and remove visible vessels without damaging the surrounding skin. These technologies use controlled energy to treat the problem at its source. The process is both effective and widely used for improving skin clarity.
- They target haemoglobin within the vessel: Treatments such as laser treatment for broken capillaries and IPL direct light energy into the skin, where it is absorbed by haemoglobin (the pigment in blood). This allows the treatment to focus specifically on the blood vessel. The surrounding tissue remains largely unaffected. Precision is a key advantage.
- Heat causes the vessel to collapse: Once the energy is absorbed, it generates heat within the vessel. This heat damages the vessel wall, causing it to collapse and seal shut. The body then recognises it as no longer functional. This is a controlled and targeted process.
- The body naturally clears the treated vessel: After the vessel collapses, your body gradually breaks it down and reabsorbs it over time. This leads to a visible reduction in redness or lines on the skin. Results often improve progressively over several weeks. The treated capillary does not reopen.
- Treatment removes existing vessels, not future ones: While treated capillaries are permanently removed, new ones can still form due to factors such as sun exposure, genetics, or skin sensitivity. These treatments do not address the underlying causes. This is why maintenance and prevention are important. Understanding this helps set realistic expectations.
Laser and light-based treatments are highly effective for removing visible capillaries, but long-term results depend on combining treatment with good skin care and lifestyle habits.
Why Treated Capillaries Usually Do Not Return
When you have a visible capillary properly treated, it is effectively destroyed and then cleared away by your body. Treatments such as laser therapy work by targeting the blood inside the vessel, which causes it to collapse. Over time, your body naturally reabsorbs the treated vessel, so it is no longer visible. Once this process is complete, that specific capillary cannot simply reopen or come back.
What you might think of as a recurrence is often the development of new capillaries in the same or nearby area. These new vessels can look very similar to the ones you had treated, especially if they appear in familiar places on your skin. Because of this, it can seem as though the original capillaries have returned. In reality, the initial treatment has worked, but your skin is responding to ongoing underlying triggers.
Understanding this difference can help you manage your expectations after treatment. While the procedure removes the visible vessels that are present at the time, it does not stop new ones from forming in the future. Factors such as sun exposure, skin sensitivity, and lifestyle habits can all influence whether new capillaries appear. Taking steps to manage these triggers can help you maintain your results for longer.
The Role of Genetics in Recurrence
Genetics play a significant role in whether broken capillaries recur after treatment. If you naturally have more fragile or reactive blood vessels, your skin is more likely to develop new visible vessels over time. This underlying tendency often associated with telangiectasia cannot be changed by treatment alone.
Some individuals are simply more predisposed to facial redness and vascular visibility. This can be influenced by inherited factors such as thinner skin, more delicate vessel walls, or a higher tendency to flush. These characteristics remain even after successful treatment, continuing to affect how your skin responds to triggers like heat, sun exposure, or irritation.
Because your genetic makeup does not change, recurrence is often part of the long-term pattern rather than a failure of treatment. While procedures can effectively remove existing vessels, they do not alter your baseline vascular behaviour. This is why ongoing care and occasional maintenance treatments are often recommended to help manage new capillaries as they develop.
Sun Exposure and Its Impact on Blood Vessels
Sun exposure plays a major role in the development of broken capillaries. Ultraviolet (UV) radiation doesn’t just affect the surface of your skin it also weakens the tiny blood vessels underneath. Over time, this damage makes vessels more likely to dilate and become permanently visible. Understanding this link is essential for protecting your skin long term.
- UV damage weakens vessel walls: Repeated sun exposure breaks down collagen and reduces the skin’s ability to support underlying blood vessels. As these vessels lose strength and elasticity, they are more likely to expand. This makes them more visible on the surface. The damage builds gradually over time.
- New capillaries can form after treatment: Even if you’ve had successful laser treatment for broken capillaries, ongoing sun exposure can trigger new vessels to appear. Treated capillaries won’t return, but new ones can develop in nearby areas. This is particularly common on sun-exposed areas like the nose and cheeks. Without protection, recurrence is more likely.
- Daily exposure adds up over time: You don’t need intense sunbathing to cause damage. Everyday activities such as walking outside or sitting near a window can contribute to cumulative UV exposure. Over months and years, this repeated exposure increases your risk. Consistency in protection matters more than occasional effort.
- Sun protection is essential for prevention: Using a broad-spectrum sunscreen daily helps protect both your skin and the blood vessels beneath it. Additional measures like wearing a hat or seeking shade can further reduce exposure. These habits lower the risk of new capillaries forming. Prevention is a key part of maintaining results.
Protecting your skin from the sun is one of the most effective ways to reduce the risk of broken capillaries and support long-term skin health.
Skin Sensitivity and Chronic Redness
If you have sensitive skin, you may find that it reacts more easily to both internal and external triggers. This can include things like temperature changes, certain skincare products, or even stress. When your skin flushes or becomes irritated frequently, it places repeated strain on the tiny blood vessels near the surface. Over time, this can cause them to dilate and become more visible, leading to what you may recognise as telangiectasia.
You may also notice that conditions such as rosacea are closely linked to recurring capillaries. If you have rosacea, ongoing inflammation can lead to persistent redness and make your blood vessels more unstable. Even if you have had visible capillaries treated, new ones can still form if this underlying inflammation is not properly controlled. This is why managing the root cause is just as important as treating the visible signs.
Looking after your skin sensitivity plays a key role in reducing the chance of recurrence. You can support your skin by using gentle, barrier-friendly products and avoiding known triggers such as heat, spicy foods, or harsh ingredients. It may also help to seek professional advice if your symptoms are ongoing or difficult to manage. By keeping inflammation under control, you not only improve your skin’s comfort but also help protect your blood vessels over time.
Temperature Changes and Environmental Triggers
If you are often exposed to extreme temperatures, this can have a noticeable effect on your skin over time. Moving quickly between hot and cold environments causes your blood vessels to expand and contract repeatedly. This constant change puts stress on the vessel walls and can gradually weaken them. As a result, they may stay enlarged and become visible, which is known as telangiectasia.
You might not always realise how common these triggers are in your daily routine. Things like hot showers, saunas, steam rooms, or even cold, windy weather can all play a part. While each exposure may seem harmless on its own, the repeated effect can increase your skin’s sensitivity. Over time, this can lead to the formation of new visible capillaries, even if you have had previous ones treated.
Making small changes to your routine can help protect your skin in the long run. You can switch to lukewarm water, limit prolonged heat exposure, and cover your face in colder conditions. These simple steps can reduce the repeated stress placed on your blood vessels. With consistent care, you can help maintain healthier, more resilient skin.
Lifestyle Factors That Influence Recurrence
Certain lifestyle habits can increase the likelihood of broken capillaries returning over time. If you regularly drink alcohol, you may notice more frequent flushing, as it causes your blood vessels to widen temporarily. When this happens often, it places repeated stress on the vessel walls. Over time, this can contribute to the development of new visible capillaries, also known as telangiectasia.
Smoking is another factor that can have a strong impact on your skin and vascular health. It weakens the walls of your blood vessels and reduces your skin’s ability to repair itself properly. This makes your capillaries more fragile and more likely to remain visible once they are damaged. In addition, smoking can speed up the overall ageing process, which further increases your skin’s vulnerability.
Your daily habits, including diet, hydration, and skincare, also play an important role. You can support your skin by eating a balanced diet, drinking enough water, and following a gentle, consistent skincare routine. These steps help strengthen your skin barrier and maintain healthier blood vessels. Over time, making these changes can reduce the risk of recurrence and improve your skin’s resilience.
Hormonal Influences on Blood Vessels
Hormonal changes can have a noticeable effect on how your blood vessels behave, including those close to the surface of the skin. Fluctuations during life stages such as pregnancy or menopause, or with certain treatments, can increase vascular sensitivity. This can contribute to the development of broken capillaries, even if you’ve previously had successful treatment. Understanding this link helps explain why changes can sometimes reappear.
- Hormones affect how vessels dilate and respond: Hormonal shifts can influence the way blood vessels expand and contract. Increased sensitivity may cause them to dilate more easily in response to heat, stress, or environmental triggers. Over time, repeated dilation can make vessels more visible. This is part of a natural physiological response.
- Certain life stages increase susceptibility: Periods such as pregnancy or menopause often involve significant hormonal changes. These can increase circulation or alter vascular stability, making capillaries more noticeable. Even hormonal medications can have a similar effect. These changes vary from person to person.
- New capillaries can form despite treatment: Treatments like laser treatment for broken capillaries remove existing vessels effectively. However, they do not prevent new ones from developing if hormonal influences persist. This can lead to recurrence in different areas. It’s a reflection of ongoing internal factors rather than treatment failure.
- Understanding these factors helps set realistic expectations: Not all influences on your skin are within your direct control. Recognising the role of hormones can help you plan treatment timing and manage expectations. It also reinforces the importance of combining treatment with preventive care. A balanced approach leads to better long-term results.
Hormonal changes are a natural part of life, but being aware of their impact can help you better manage and maintain your skin over time.
Ageing and Skin Thinning

As you get older, your skin naturally becomes thinner and less supportive. You may notice that it feels more delicate or looks less firm than it used to. This happens because your body produces less collagen and elastin over time, which are essential for maintaining strength and structure. As this support reduces, small blood vessels can become more visible through the skin, often appearing as telangiectasia.
Ageing also affects the blood vessels themselves, not just the skin around them. Over time, the vessel walls can lose their elasticity and become more prone to staying enlarged. This means that once they expand, they may not return to their original size as easily as before. As a result, you may be more likely to develop new visible capillaries.
Even if you have had successful treatment, the ageing process continues. This means you might notice new capillaries appearing gradually over time, even though previous ones have been removed. You can help manage these changes with good skincare, sun protection, and, if needed, occasional maintenance treatments. Taking a consistent approach can support your skin’s appearance in the long term.
Why Some Areas Are More Prone to Recurrence
You may notice that certain areas of your face are more likely to develop broken capillaries than others. The nose and cheeks, in particular, tend to have thinner skin and a richer blood supply, which makes the underlying vessels more visible. These areas are also more exposed to environmental factors such as sun, wind, and temperature changes. Over time, this combination can place extra stress on your blood vessels and increase the chances of developing telangiectasia.
It is quite common for new capillaries to appear repeatedly in these same regions. When this happens, you might feel as though the previous treatment has not worked or that the same vessels have come back. In most cases, the original capillaries have been successfully treated and removed. However, these areas remain more vulnerable, so new vessels can form in a similar pattern.
Because of this, you may find that certain parts of your face need occasional maintenance treatments. Understanding this pattern can help you set realistic expectations and feel more confident about your results. With consistent skin protection and the right approach to follow-up care, you can better manage recurrence. Over time, this helps you maintain clearer and more even-looking skin.
The Importance of Proper Treatment Technique
The success of treatment for broken capillaries depends greatly on how precisely it is carried out. When you have treatment for telangiectasia, the aim is to deliver enough energy to fully collapse the vessel without affecting the surrounding skin. If the technique is not accurate, the vessel may only be partially treated. This can reduce how effective the procedure is and affect how long your results last.
Choosing an experienced practitioner is therefore very important for your outcome. A skilled clinician will assess your skin type, the size of the vessel, and its location before deciding on the best approach. This ensures that the most suitable technology and settings are used for your specific needs. With the right expertise, you are more likely to achieve safe and consistent results.
If the treatment is incomplete, you may notice that the capillaries remain visible or seem to return quite quickly. This is often due to the vessel not being fully closed rather than a problem with the treatment itself. You can improve your chances of longer-lasting results by choosing a practitioner who focuses on precision and detail. This careful approach helps deliver more reliable and effective outcomes over time.
How Many Sessions Are Typically Needed?
When treating broken capillaries, it’s important to understand that results are usually achieved gradually rather than in a single session. While some vessels may respond quickly, others require additional treatments to fully fade. A staged approach allows for safer, more precise results and better overall skin clarity.
- Multiple sessions are usually needed: Most people require a series of treatments with laser treatment for broken capillaries or similar light-based methods. Not all capillaries respond at the same rate, and some may only partially fade after the first session. Additional treatments help target any remaining vessels. This builds towards a more complete result.
- Gradual improvement leads to better outcomes: Treating capillaries in stages allows your skin to respond naturally. After each session, the body gradually clears the treated vessels. This process takes time and varies from person to person. A step-by-step approach improves both safety and effectiveness.
- Spacing between sessions is important: Treatments are usually spaced a few weeks apart to allow the skin to heal and settle. This also makes it easier to identify which vessels still need treatment. Proper spacing reduces the risk of irritation and enhances precision. Timing is an important part of the plan.
- Realistic expectations are key: Expecting complete clearance in a single session can lead to disappointment. Understanding that multiple treatments are part of the process helps set realistic goals. Your practitioner will guide you on the number of sessions needed based on your skin and the extent of the condition. Clear expectations support better satisfaction.
Achieving the best results with capillary treatment is a gradual process, with multiple sessions working together to deliver long-term improvement.
The Role of Maintenance Treatments
Maintenance treatments play an important role in helping you keep your results consistent over time. They focus on treating any new vessels early, before they become more noticeable on your skin. This can help you maintain a clearer and more even-looking complexion. It is especially useful if you are prone to conditions like telangiectasia, where new capillaries can gradually develop.
It is important to understand that needing maintenance does not mean your original treatment has failed. Instead, it reflects the natural and ongoing changes that happen in your skin over time. Factors such as your genetics, environment, and lifestyle continue to influence how your blood vessels behave. Even after successful treatment, these underlying influences are still present.
How often you need maintenance treatments will depend on your individual skin and risk factors. You may only need occasional touch-ups, or you might benefit from more regular reviews. A personalised plan can help ensure that treatment is timed appropriately for you. This approach supports longer-lasting results while helping to maintain your overall skin health.
Skincare Strategies to Reduce Recurrence
A gentle and consistent skincare routine can make a real difference in reducing the recurrence of telangiectasia. If you use harsh exfoliants, strong acids, or overly aggressive treatments, you may unintentionally irritate your skin. This can place extra stress on delicate capillaries and make them more prone to becoming visible. Choosing calming, barrier-supporting products helps protect your skin and keeps it more resilient over time.
You may find it helpful to focus on ingredients that soothe redness and support your skin barrier. Options such as niacinamide, ceramides, and anti-inflammatory ingredients can help strengthen your skin and reduce sensitivity. Rather than using too many products, you are often better off sticking to a simple and consistent routine. This approach helps your skin stay balanced and less reactive.
It is also important to pay attention to your personal triggers. You might notice that things like heat, spicy foods, alcohol, or certain skincare ingredients cause your skin to flush. Identifying and avoiding these triggers can reduce repeated stress on your blood vessels. By combining the right skincare with good lifestyle habits, you can support longer-lasting results and healthier-looking skin.
When Recurrence May Indicate an Underlying Condition
If you keep noticing visible vessels returning, it may not just be a simple cosmetic concern. In some cases, frequent or widespread recurrence can suggest an underlying skin condition that needs proper assessment. Paying attention to patterns such as ongoing redness, flushing, or repeated capillary formation can help you understand when something more is going on. When you address the underlying cause not just the visible vessels you are more likely to achieve longer-lasting results.
- Persistent symptoms may point to a skin condition: If you regularly experience flushing, redness, or new visible vessels, it could be linked to a condition such as rosacea. This condition affects how your blood vessels behave and can make your skin more sensitive. Without proper management, it may lead to repeated formation of visible capillaries.
- Treating vessels alone may not be enough: You may find that treatments like laser therapy remove visible vessels effectively. However, these treatments focus on what you can see rather than what is causing the issue. If the underlying triggers are not controlled, new vessels can continue to appear over time.
- Medical treatment may be needed: If your symptoms are linked to an underlying condition, you may benefit from a broader treatment plan. This could include prescription medication, targeted skincare, and lifestyle adjustments. These approaches help reduce inflammation and stabilise your skin, making recurrence less likely.
- Recognising patterns helps guide treatment: If you notice that the vessels return quickly, spread across larger areas, or persist despite treatment, it is a good idea to seek further evaluation. Understanding the root cause allows your practitioner to create a more tailored and effective plan for you.
Overall, recognising when recurrence may be linked to an underlying condition helps you move beyond surface-level treatment. By addressing both the appearance and the cause, you can achieve more stable, long-term improvements in your skin.
Setting Realistic Expectations Before Treatment

Setting realistic expectations before your treatment is an important part of having a positive experience. Treatments for telangiectasia are very effective at removing the visible vessels you currently have. However, they do not prevent new ones from forming in the future. Factors such as your genetics, skin sensitivity, and environmental exposure will continue to influence your skin over time.
If you expect complete and permanent clearance, you may feel disappointed if new capillaries appear later on. On the other hand, if you understand that some level of maintenance is normal, you are more likely to feel satisfied with your results. It helps to think of treatment as part of an ongoing skin management plan rather than a one-off solution. This mindset can make a big difference in how you view your results.
Having open and clear communication with your practitioner is key to getting the most out of your treatment. You can discuss what results are realistic, how many sessions you might need, and whether maintenance treatments are likely. This helps you plan ahead and feel more prepared for the process. When you know what to expect, you are more likely to feel confident in your decisions and happy with your long-term results.
FAQs:
1. What are the most common eye conditions after 60?
The most common eye conditions after 60 include cataracts, glaucoma, age-related macular degeneration (AMD), and diabetic retinopathy. These conditions affect different parts of the eye and can lead to gradual or sudden vision loss. Regular eye exams help detect them early.
2. Is vision loss after 60 inevitable?
No, vision loss is not always inevitable. While some changes are part of normal ageing, many serious conditions can be treated or managed effectively. Early detection and proper care play a key role in preserving vision.
3. How do cataracts affect vision?
Cataracts cause the natural lens of the eye to become cloudy. This leads to blurred, dim, or hazy vision and increased sensitivity to light. The condition can be treated successfully with surgery.
4. Why is glaucoma called the “silent” eye condition?
Glaucoma is often called “silent” because it develops without noticeable symptoms in the early stages. It usually affects peripheral vision first. By the time symptoms appear, some vision loss may already be permanent.
5. What are the early signs of macular degeneration?
Early signs include blurred central vision, difficulty reading, and straight lines appearing wavy. These symptoms can develop gradually or suddenly depending on the type. Prompt assessment is important for management.
6. Can diabetes lead to vision loss after 60?
Yes, diabetes can cause diabetic retinopathy, which damages the blood vessels in the retina. This can lead to blurred vision, floaters, or even severe vision loss. Managing blood sugar levels and regular eye screening are essential.
7. Are floaters in vision normal with age?
Floaters are common as you age and are usually harmless. However, a sudden increase in floaters or flashes of light may indicate a more serious condition. In such cases, immediate eye examination is necessary.
8. Why does night vision get worse with age?
Night vision declines due to changes in the lens and retina, as well as conditions like cataracts. Increased glare and reduced contrast sensitivity make it harder to see in low light. Assessment can help identify treatable causes.
9. How often should someone over 60 have an eye test?
Most people over 60 should have an eye test every one to two years. Those with existing conditions may need more frequent check-ups. Regular monitoring helps detect problems early.
10. When should I seek urgent medical help for vision problems?
You should seek urgent care if you experience sudden vision loss, flashes of light, a shadow or curtain over your vision, or severe eye pain. These symptoms may indicate serious conditions requiring immediate treatment.
Final Thoughts: Managing Broken Capillaries Long-Term
Broken capillaries can be effectively treated, but understanding that they may recur is essential for setting realistic expectations. Treatments such as laser therapy successfully remove existing visible vessels, yet they do not prevent new ones from forming. Factors such as genetics, sun exposure, skin sensitivity, and ageing continue to influence your skin over time. This is why a long-term approach that combines treatment with preventive care is the most effective way to maintain clearer skin.
Focusing on consistent skincare, sun protection, and managing triggers like heat, alcohol, and irritation can significantly reduce recurrence. Regular follow-up treatments may also be needed to maintain results, especially in areas prone to vascular changes. If you’re considering dermatologist in London, you can get in touch with us at London Dermatology Centre.
References:
- Lin, Y., Wang, J., Chen, X., Li, H., Zhang, Q. & Liu, Y. (2023) ‘Association between inflammatory biomarkers and risk of cardiovascular disease: a systematic review and meta-analysis’, Frontiers in Cardiovascular Medicine, 10, p.1187654. https://pubmed.ncbi.nlm.nih.gov/37654935/
- Yin, H.-Y., Li, C.-Y., Chen, H.-C., Lin, Y.-C., Wu, C.-L. & Huang, J.-L. (2021) ‘Successful management of chronic blepharo-rosacea associated demodex by lid scrub with terpinen-4-ol’, Clinical and Experimental Optometry, 104(6), pp. 694-699. https://pmc.ncbi.nlm.nih.gov/articles/PMC8326346/
- Beg, K., Padmapriya, B., Noorul Shajar, S., Ahmad, M.M. and Faiyyaz, A.G. (2024)
‘The bibliometric analysis of previous twenty-five years’ literature: A microfinance review’, Heliyon, 10(3), e24979. https://www.sciencedirect.com/science/article/pii/S2352512623003181 - Chen, Y.-C., Foster, J., Wang, M.-L., Rohmah, I., Tseng, Y.-H. & Chiu, H.-Y. (2021) ‘Global prevalence and risk factors of emergence delirium in paediatric patients undergoing general anaesthesia: a systematic review and meta-analysis’, Journal of Paediatric Nursing, 77, pp. 74-80. https://pubmed.ncbi.nlm.nih.gov/34824181/
- Campolmi, P., Cannarozzo, G., Dragoni, F., Conti, R. & Moretti, S. (2016) ‘Efficacy of rhodamine light in the treatment of superficial vascular lesions of the face’, Medicina Princ Pract, 25(5), pp. 477-482. https://pmc.ncbi.nlm.nih.gov/articles/PMC5588436/