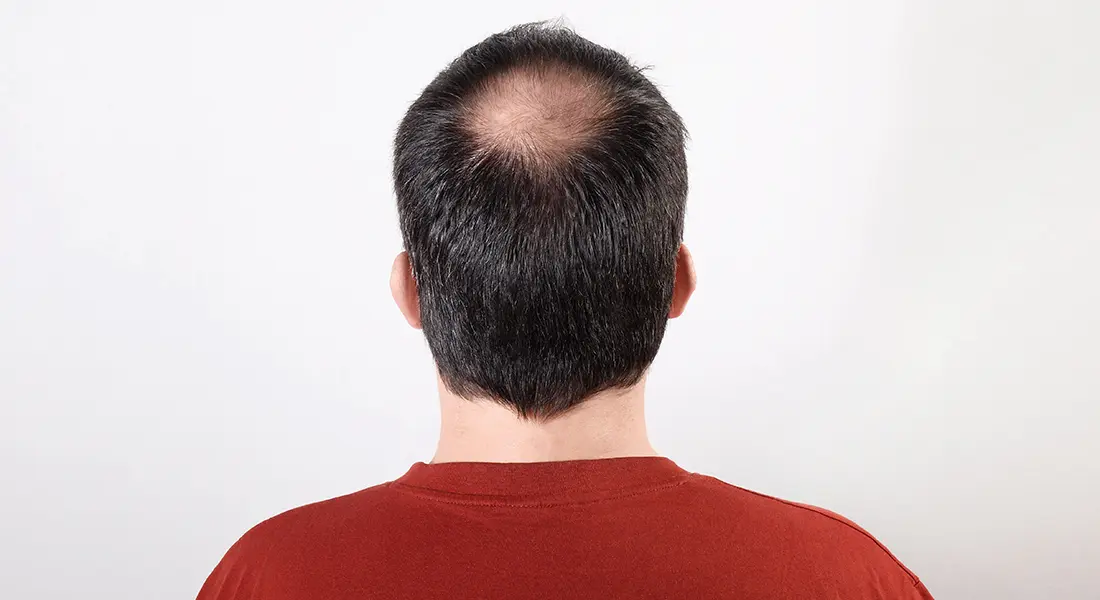
One of the first questions most people ask after being diagnosed with alopecia is simple but deeply personal: will my hair grow back? It’s a completely natural concern, and the answer is rarely a simple yes or no.
Hair loss behaves differently depending on the type of alopecia, how long it has been present, and what is happening beneath the skin. Dermatologists assess prognosis by looking at patterns, inflammation, follicle health, and response to early treatment.
In this guide, I’ll explain how dermatologists predict hair regrowth and long-term stability in different forms of alopecia, what signs suggest recovery is possible, and when expectations need to be adjusted.
Why Alopecia Prognosis Varies So Widely
Alopecia encompasses a range of disorders, each impacting hair follicles differently. Not all hair loss is the same, and the underlying mechanism determines how likely hair is to regrow. Understanding the specific type of alopecia is crucial for predicting outcomes and guiding treatment.
- Multiple underlying conditions – Alopecia includes temporary shedding, inflammatory forms, and permanent follicle damage.
- Disruption of hair growth cycles – Some types cause short-term hair loss that often regrows naturally.
- Inflammatory damage – Certain forms trigger follicle inflammation, which can slow or alter regrowth.
- Permanent follicle destruction – Rare types lead to irreversible hair loss, making early detection vital.
- Prognosis depends on type, not extent – The amount of hair lost does not always predict recovery; understanding the cause is key.
- Guides treatment strategy – Accurate diagnosis ensures interventions target the specific mechanism of hair loss.
Recognizing the diversity of alopecia helps set realistic expectations and informs a personalized approach to management, improving both outcomes and patient confidence.
How Dermatologists Approach Prognosis
Predicting hair regrowth involves a structured approach. Dermatologists use clinical examination, patient history, and sometimes additional tests to form a realistic outlook.
They evaluate hair loss patterns, scalp condition, hair shaft characteristics, and the presence of viable follicles. The duration and progression of hair loss also influence predictions.
Accurate, early diagnosis greatly enhances the ability to forecast treatment outcomes and set realistic expectations for patients.
The Importance of Duration in Hair Loss Prognosis

The length of time hair loss has been occurring plays a critical role in predicting regrowth potential. Early intervention often leads to better outcomes, while prolonged hair loss can reduce the likelihood of full recovery.
1. Short-Term Hair Loss Responds Better – When hair loss is recent and follicles remain healthy, treatments are more likely to stimulate regrowth effectively. Rapid action can preserve follicle function and density.
2. Long-Standing Hair Loss Presents Challenges – Hair that has been thinning for months or years may show follicle miniaturisation or even permanent destruction. This makes regrowth slower, less complete, or sometimes unlikely without advanced interventions.
3. Early Assessment Improves Prognosis – Prompt evaluation by a dermatologist allows for timely treatment and a tailored plan. Understanding the duration of hair loss helps guide realistic expectations and the most effective approach.
Early attention is key: the sooner hair loss is assessed and addressed, the higher the chances of meaningful regrowth.
Understanding Hair Follicle Viability
Successful hair regrowth hinges on the health and functionality of hair follicles. Not all follicles respond the same way, and their condition determines whether treatments will be effective. Assessing follicle viability helps dermatologists predict outcomes and tailor therapy.
- Alive and functional follicles – Healthy follicles can respond to treatment and regrow hair.
- Dormant or miniaturised follicles – These may still produce hair with appropriate medical or procedural intervention.
- Destroyed follicles – If follicles are replaced by scar tissue, regrowth is unlikely, limiting treatment options.
- Signs of viability – Dermatologists examine follicular openings, hair calibre variation, and scalp condition.
- Guides treatment planning – Identifying viable follicles helps select the most effective approach for hair restoration.
- Predicts realistic outcomes – Understanding follicle health sets expectations for potential regrowth and success rates.
Evaluating follicle viability is a critical step in managing alopecia. It ensures treatment is targeted, realistic, and tailored to each patient’s unique scalp condition.
Inflammation: A Key Prognostic Factor
Inflammation is a major factor in alopecia. Active inflammation can hinder hair growth and gradually damage follicles. Early detection and management of inflammation increase the chances of follicle recovery. Persistent, uncontrolled inflammation raises the risk of permanent hair loss. Promptly addressing inflammation is therefore critical for improving long-term hair regrowth outcomes.
Alopecia Areata: Prognosis and Regrowth Potential
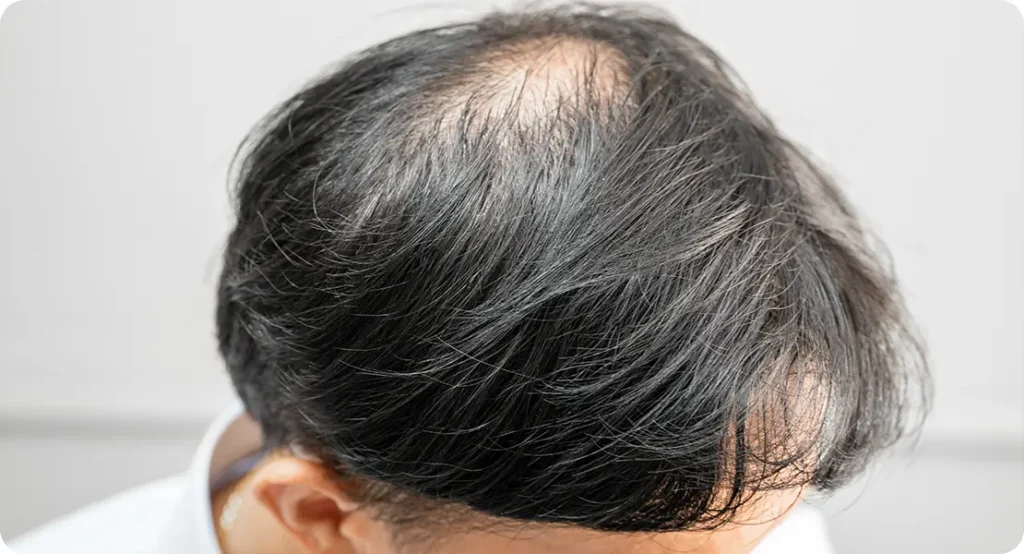
Alopecia areata is an autoimmune condition in which the body’s immune system mistakenly attacks hair follicles. Despite this, the follicles often remain structurally intact, which means there is a strong potential for regrowth in many cases.
1. Follicle Integrity Supports Regrowth – Because the hair follicles are usually preserved, even significant hair loss can often be reversed with appropriate treatment, particularly when caught early.
2. Factors Influencing Prognosis – The likelihood and speed of regrowth depend on several factors, including the extent of hair loss, how long it has been present, involvement of nails, and how well the patient responds to initial therapy.
3. Early and Tailored Treatment Matters – Prompt diagnosis and targeted management improve outcomes. Mild or early cases generally have the best prognosis, highlighting the importance of consulting a dermatologist as soon as hair loss is noticed.
Understanding these factors helps patients set realistic expectations and pursue treatment strategies that maximise the chances of regrowth.
Patchy Alopecia Areata vs Extensive Disease
Small, patchy areas of alopecia areata generally have a more favourable outlook. These limited patches often respond well to treatment.
Short-duration patches may even regrow spontaneously without intervention. Early treatment can further improve outcomes.
Extensive scalp involvement carries a higher risk of relapse or chronic progression. Managing expectations is crucial in these cases. Dermatologists assess both the pattern and progression of hair loss to provide realistic prognoses and guide treatment decisions.
Androgenetic Alopecia: Long-Term Stability vs Regrowth
Androgenetic alopecia progresses gradually through follicle miniaturisation rather than sudden shedding. Understanding this slow pattern is key to managing expectations.
Regrowth is achievable in early stages when follicles are still active and producing fine hairs. Early intervention improves the chances of visible improvement.
Once follicles are severely miniaturised, regrowth is limited. Treatment therefore focuses equally on stabilising existing hair and encouraging new growth where possible.
Why Early Treatment Matters in Pattern Hair Loss
In androgenetic alopecia (pattern hair loss), starting treatment early can make a significant difference in long-term outcomes. Early intervention helps preserve vulnerable follicles before irreversible changes occur, improving the chances of maintaining natural hair density.
- Preserves follicles – Initiating treatment promptly protects follicles from progressive miniaturisation.
- Prevents irreversible loss – Delaying therapy allows follicles to shrink beyond the point where regrowth is possible.
- Assessment guides timing – Dermatologists evaluate hair density, diameter variation, and family history to determine when to start treatment.
- Focus on maintenance – Retaining existing hair is often the primary goal and considered a successful result.
- Improves treatment efficacy – Early intervention enhances the effectiveness of medical or procedural therapies.
- Supports long-term outcomes – Consistent early management slows progression and maximizes hair preservation.
Timely treatment empowers patients to maintain hair health and slows the natural course of pattern hair loss. It emphasizes prevention as much as restoration.
Telogen Effluvium: One of the Best Prognoses
Telogen effluvium is a common form of hair shedding caused by temporary disruptions such as stress, illness, hormonal shifts, or nutritional deficiencies. Unlike scarring forms of alopecia, follicles remain healthy, making recovery highly likely once the underlying cause is addressed.
- Triggered by temporary factors – Stress, illness, hormonal changes, or nutrient deficiencies can push hair into the resting phase.
- Follicles remain intact – No permanent damage occurs, preserving the potential for regrowth.
- Widespread shedding – Hair loss is often noticeable across the scalp rather than in specific patches.
- Regrowth expected – Once the trigger is resolved, most patients experience full hair recovery.
- Timeline varies – Hair may take several months to return to its pre-shedding density.
- Supportive care helps – Nutritional optimization, stress management, and gentle hair care can support faster recovery.
Telogen effluvium generally carries an excellent prognosis. Early identification and addressing the root cause allow hair to regrow naturally, making it one of the more treatable forms of hair loss.
How Long Regrowth Takes in Telogen Effluvium
Telogen effluvium is a temporary hair shedding condition that often follows stress, illness, or hormonal changes. While regrowth is generally expected, it occurs gradually and requires patience.
1. Continued Shedding Before Improvement – Even after the triggering factor resolves, shedding may persist for several months. This is a normal part of the hair cycle resetting itself.
2. Timeline for Visible Regrowth – New hair typically becomes noticeable around three to six months after the underlying cause is addressed. Full recovery and return to previous hair density can take up to a year.
3. Managing Expectations and Anxiety – Understanding that regrowth is gradual helps patients remain calm and reduces anxiety during the recovery period. Patience and consistent care are key to optimal results.
Recognising the natural timeline of telogen effluvium allows patients to approach recovery with realistic expectations and confidence in eventual improvement.
Scarring Alopecia: Why Prognosis Is More Guarded
Scarring alopecia is a group of hair loss conditions in which inflammation permanently damages hair follicles, replacing them with scar tissue. Unlike non-scarring forms, regrowth in affected areas is not possible, making early detection and intervention critical.
- Permanent follicle destruction – Inflammation destroys follicles, preventing any future hair regrowth in those areas.
- Early diagnosis is crucial – Prompt recognition allows treatment to halt progression before more follicles are lost.
- Focus on prevention – The primary treatment goal is stopping further hair loss rather than restoring what is already gone.
- Variable progression – The speed and pattern of scarring differ among individuals and conditions.
- Monitoring is essential – Regular follow-up helps ensure inflammation is controlled and new areas are protected.
- Limited restorative options – Treatments may include anti-inflammatory medications or procedural interventions, but regrowth in scarred areas is rare.
Because hair restoration is unlikely once scarring occurs, managing scarring alopecia centers on early intervention and disease control. This approach helps preserve remaining hair and minimize long-term cosmetic impact.
Early vs Late Scarring Alopecia Outcomes
In early scarring alopecia, inflammation may have started but some follicles remain intact. Prompt intervention at this stage can preserve these follicles and maintain hair density. Early treatment often leads to meaningful regrowth and slows further progression.
In contrast, late-stage scarring alopecia typically presents with a smooth, shiny scalp and loss of follicular openings. By this point, follicles are permanently destroyed, making regrowth extremely unlikely.
Recognising the condition early is critical. Timely diagnosis and management dramatically improve long-term outcomes and help patients maintain as much natural hair as possible.
Pattern and Distribution as Prognostic Clues
The way hair loss is distributed provides key insights into likely outcomes. Diffuse shedding across the scalp often points to reversible causes, whereas focal patches or loss along the hairline may suggest an inflammatory or scarring process.
Symmetry, involvement of scalp edges, and accompanying symptoms such as pain, itching, or burning are also important indicators. These details help dermatologists distinguish between temporary shedding and conditions that may lead to permanent loss.
By carefully evaluating these patterns, specialists can guide investigations, tailor treatment strategies, and set realistic expectations for hair regrowth and long-term stability.
The Role of Trichoscopy in Prognosis
Trichoscopy is a detailed, magnified examination of the scalp that lets dermatologists evaluate follicle health closely. It highlights subtle features such as miniaturised hairs, inflammation, scarring, and changes in the hair shaft.
This information is crucial for refining prognosis and designing a personalised treatment plan. By revealing early signs that may not be visible to the naked eye, trichoscopy helps predict which areas are likely to respond to therapy.
It is particularly valuable when the diagnosis is uncertain, guiding further investigation and ensuring that interventions are targeted and effective.
Blood Tests and Prognosis
Blood tests are an important part of assessing hair loss, as they can reveal underlying factors that contribute to shedding. Identifying and addressing these issues helps guide a more effective treatment plan.
1. Identifying Contributing Factors – Tests can detect conditions such as iron deficiency, thyroid disorders, or autoimmune diseases, all of which can influence hair health and regrowth potential.
2. Correcting Abnormalities Improves Outcomes – Addressing deficiencies or hormonal imbalances can significantly enhance the likelihood of hair regrowth in certain types of alopecia.
3. Targeting the Root Cause – By understanding the underlying contributors, treatment can be personalised rather than symptomatic, ensuring a more efficient and effective approach to restoring hair.
Blood tests provide valuable insight, allowing clinicians to tailor interventions and maximise the chances of successful hair regrowth.
Response to Early Treatment as a Prognostic Indicator
The initial months of hair loss treatment offer important clues about likely outcomes. How hair responds early on helps dermatologists predict long-term results and tailor therapy effectively. Monitoring early changes can guide adjustments to maximize success.
- Early improvement signals responsive follicles – Reduced shedding or initial regrowth suggests hair follicles can still respond to treatment.
- Lack of response indicates caution – Minimal or no change may point to more advanced or resistant hair loss.
- Guides treatment adjustments – Dermatologists can modify medications, procedures, or intensity based on early response.
- Supports realistic expectations – Early trends help set patient expectations for recovery and timeline.
- Helps prioritize interventions – Patients showing limited early response may benefit from alternative or combination approaches.
- Predictive value for prognosis – Early outcomes often correlate with long-term treatment success and hair retention.
Monitoring the response in the first few months allows dermatologists to personalize treatment plans. It ensures interventions are effective and provides patients with a clearer understanding of what to expect over time.
Psychological Impact and Managing Expectations
Hair loss impacts more than just physical appearance; the uncertainty about regrowth can be emotionally challenging. Many patients experience anxiety, reduced confidence, and frustration. Understanding prognosis helps set realistic expectations, giving patients a clearer sense of likely outcomes. Honest, transparent conversations with a dermatologist are essential in this process. Providing support and education not only eases emotional distress but also encourages better adherence to treatment plans, improving long-term results.
Why Prognosis Is Reassessed Over Time
Alopecia prognosis is not static. Hair loss patterns and treatment responses can change over weeks or months, so early predictions may need updating.
Dermatologists schedule periodic reassessments to monitor progress and adjust management plans accordingly. This ensures treatment remains appropriate as the condition evolves.
Some aspects of hair loss that are unclear at the start may become more predictable over time, helping refine expectations. Regular review allows for timely intervention if new signs appear, making ongoing monitoring a key strength of quality dermatological care.
When Hair Transplantation Is Considered
Hair transplantation is typically reserved for cases where hair follicles have been permanently lost and the underlying condition is stable. Surgery is not a first-line treatment but may be an option once medical therapy has halted disease progression. Careful evaluation ensures realistic expectations and optimal outcomes.
- Permanent follicle loss – Transplantation is only considered when natural regrowth is no longer possible.
- Disease stability required – Hair loss must be controlled before surgery to prevent future graft loss.
- Medical management first – Treatments are initiated to halt progression before considering surgical intervention.
- Accurate prognosis is essential – Understanding potential for regrowth guides whether transplantation is appropriate.
- Personalized planning – Surgeons evaluate scalp density, donor area availability, and patient goals.
- Optimizes long-term results – Timing and planning increase the likelihood of a successful and lasting outcome.
Hair transplantation is a targeted solution for stable, permanent hair loss. Combining medical management with careful surgical planning ensures the best cosmetic and functional results.
The Importance of Specialist Care
Accurately predicting hair regrowth demands specialist knowledge and experience. Incorrect assessment can either give false hope or undue concern. A qualified dermatologist offering alopecia treatment in London carefully evaluates all prognostic factors before providing guidance. Thorough initial assessment plays a crucial role in determining long-term outcomes and optimising treatment strategies.
FAQs:
1. Will my hair grow back after being diagnosed with alopecia?
The likelihood of regrowth depends on the type of alopecia you have, how long it has been present, and the health of your hair follicles. Some forms, like telogen effluvium or early alopecia areata, often show good recovery with appropriate treatment, while scarring alopecia can result in permanent hair loss if not addressed early.
2. How does the duration of hair loss affect recovery?
Hair loss that has occurred recently usually responds better to treatment, as the follicles are more likely to remain healthy and functional. On the other hand, hair that has been thinning for months or years may be more difficult to restore, and achieving full regrowth may require more intensive interventions or may not be entirely possible.
3. Can inflammation really stop hair from growing back?
Yes, active inflammation around hair follicles can interfere with the growth cycle and gradually damage the follicles. Controlling inflammation early is important because persistent inflammation increases the risk of permanent hair loss and can limit the success of any treatments.
4. What role does the type of alopecia play in prognosis?
Different types of alopecia affect the follicles in different ways. For example, alopecia areata often leaves follicles structurally intact, allowing for potential regrowth, whereas androgenetic alopecia gradually miniaturises follicles, making regrowth more challenging as the condition progresses. Accurate diagnosis is essential to guide treatment and set realistic expectations.
5. How do dermatologists evaluate whether my follicles are healthy?
Specialists examine your scalp for visible signs of viable follicles, hair shaft variations, and the overall scalp condition. They may also use tools like trichoscopy or recommend blood tests to assess underlying factors, providing a clearer picture of how your follicles might respond to treatment.
6. Is early treatment really that important?
Yes, starting treatment as soon as hair loss is noticed can preserve existing follicles, prevent irreversible damage, and increase the chances of visible regrowth. Even in conditions like androgenetic alopecia, early intervention can slow progression and improve long-term outcomes.
7. How long does it take for hair to regrow after a condition like telogen effluvium?
Regrowth in telogen effluvium typically occurs gradually. While new hair often becomes noticeable within three to six months, full restoration of hair density can take up to a year. Patience and consistent care during this period are key to optimal recovery.
8. Can scarring alopecia be reversed?
Unfortunately, once follicles are replaced by scar tissue, regrowth in those areas is generally not possible. The focus in scarring alopecia is on early diagnosis and controlling inflammation to prevent further hair loss rather than restoring lost hair.
9. When should I consider hair transplantation?
Hair transplantation is usually considered only when hair follicles have been permanently lost and the underlying condition is stable. Medical therapy is prioritised first to halt progression, and surgery is planned carefully to ensure realistic outcomes and long-term success.
10. Why is specialist care important for hair loss?
Accurately predicting hair regrowth requires experience and knowledge of various types of alopecia. A qualified dermatologist can assess all relevant factors, tailor treatment to your specific condition, and provide realistic guidance, reducing anxiety and helping maximise the chances of successful outcomes.
Final Thought: Understanding Alopecia Prognosis and Next Steps
Predicting hair regrowth is complex, but understanding the key factors alopecia type, duration, follicle health, inflammation, and early treatment response helps set realistic expectations. While some forms, like telogen effluvium or patchy alopecia areata, often respond well to timely intervention, others, such as scarring alopecia, require early detection to preserve remaining hair. Regular monitoring, tailored treatment plans, and specialist guidance are essential for achieving the best possible outcomes.
If you’re thinking about alopecia treatment in London, you can contact us at London Dermatology Centre. At London Dermatology Centre, our experienced dermatologists assess each case comprehensively, using advanced diagnostic tools and personalised strategies to maximise hair regrowth potential.
References:
1. Rawlings, A. V., et al. (2021) Hormonal effects on hair follicles and their cycling: implications for menopause and female pattern hair loss, International Journal of Molecular Sciences, 21(15), p.5342. https://www.mdpi.com/1422-0067/21/15/5342
2. Kanti, V., et al. (2023) Female Pattern Hair Loss: An Overview with Focus on Genetics, Genes, 14(7), p.1326. https://www.mdpi.com/2073-4425/14/7/1326
3. Gupta, A. K., Economopoulos, V., Mann, A., Wang, T. & Mirmirani, P. (2025) Menopause and hair loss in women: Exploring the hormonal transition, Maturitas, 198, p.108378. https://www.sciencedirect.com/science/article/pii/S0378512225001860
4. Sinclair, R. & others (2017) Hormonal therapy in female pattern hair loss, International Journal of Women’s Dermatology, 3(1), pp.53–57. https://www.sciencedirect.com/science/article/pii/S2352647517300011 5. Gupta, A. K., Economopoulos, V., Mann, A., Wang, T. & Mirmirani, P. (2025) Menopause and hair loss in women: Exploring the hormonal transition. https://pubmed.ncbi.nlm.nih.gov/40318238/