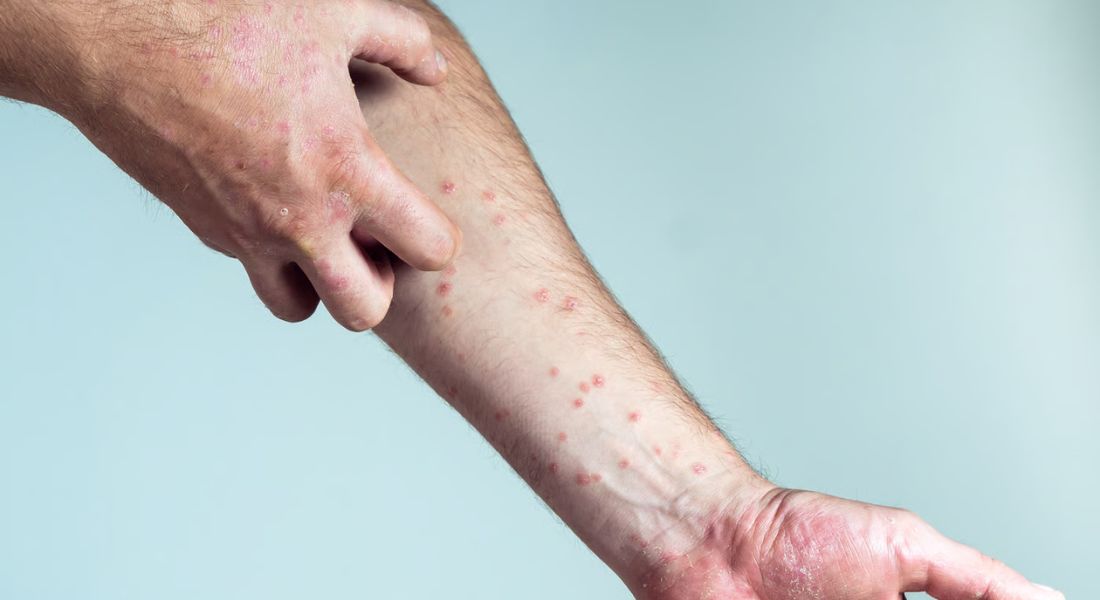
You may have been told that your skin condition is “genetic”, particularly if it appears repeatedly within your family. Perhaps psoriasis runs in your relatives, or eczema affected your parents before developing in you. This can make it seem as though your skin concerns were predetermined from birth. While genetics plays an important role, it does not always provide the complete explanation.
You may also notice something that feels confusing or even contradictory. Two people can share very similar genes yet experience completely different skin outcomes. Even identical twins, who have the same DNA sequence, do not always develop the same skin disease at the same time or with the same severity. This difference highlights the influence of factors beyond inherited genes.
This is where epigenetics enters the conversation and begins to offer clarity. Epigenetics does not change your DNA sequence itself, but it influences how certain genes are switched on or off. In other words, it affects how your genetic information is used rather than altering the code. This process helps explain why your skin may behave differently under varying circumstances.
Your environment, lifestyle, stress levels, diet, pollution exposure, and even sleep patterns can all shape how your genes are expressed. These influences interact with your biology in subtle but powerful ways. In this article, I will guide you through what epigenetics truly means and how it relates to conditions such as psoriasis, eczema, and acne. You will also gain insight into what this emerging field of research may mean for future treatment strategies.
What Is Epigenetics?
To understand epigenetics, you first need a basic understanding of genetics. Your DNA contains the instructions for building proteins that regulate essential functions, including skin barrier integrity and immune signalling. These proteins influence how your skin protects itself and responds to irritation or injury. In simple terms, your genes provide the blueprint for how your skin operates.
However, not all genes are active at all times. Some are strongly expressed and actively producing proteins, while others remain silent depending on your body’s needs. This selective activity allows your cells to respond to different internal and external conditions. The same genetic code can therefore produce different outcomes depending on which genes are switched on.
Epigenetics refers to chemical modifications that regulate gene activity without altering the underlying DNA sequence. You can think of your DNA as a script containing every possible line of dialogue. Epigenetics acts like stage direction, deciding which lines are spoken and which are skipped. In this way, your genes remain the same, but their expression can change according to circumstances.
The Main Epigenetic Mechanisms
Epigenetics explains how gene activity can change without altering the underlying DNA sequence. Rather than modifying the genetic code itself, epigenetic mechanisms influence how genes are switched on or off. Researchers primarily focus on three core systems that regulate this process. Together, these mechanisms allow the body to adapt gene expression dynamically in response to environmental signals.
1. DNA Methylation: DNA methylation involves the addition of methyl groups to specific regions of DNA. This process typically reduces gene expression by preventing transcription machinery from accessing the gene. It plays a key role in development, ageing, and disease regulation.
2. Histone Modification: DNA is wrapped around proteins known as histones, forming a compact structure. Chemical modifications to histones can either tighten or loosen this structure. When DNA is tightly packed, genes become less accessible and less active; when loosened, gene expression increases.
3. Non-Coding RNA Regulation: Non-coding RNA molecules do not produce proteins but instead regulate gene activity after transcription. These RNA fragments can enhance or suppress the translation of specific genes. They provide an additional layer of fine-tuning in gene control.
In conclusion, the three main epigenetic mechanisms DNA methylation, histone modification, and non-coding RNA regulation work together to control gene activity. They do not alter the DNA sequence itself but influence how genes are expressed. This flexible regulatory system allows the body to respond effectively to environmental changes and internal biological signals.
Why Epigenetics Matters in Dermatology
Your skin is the largest organ in your body and acts as your first line of defence. It is constantly exposed to environmental stressors that other organs rarely encounter directly. Ultraviolet radiation, air pollution, allergens, microbes, temperature fluctuations, and mechanical irritation all interact with your skin on a daily basis. Because of this continuous exposure, your skin must adapt more frequently than many internal systems.
Unlike organs protected inside your body, your skin faces the external world at all times. It must respond quickly to injury, infection, dryness, and environmental change. Epigenetic regulation allows this flexibility by adjusting which genes are active in response to different conditions. This adaptability helps maintain barrier strength, control inflammation, and support repair.
However, when environmental stress becomes chronic or intense, the adaptive system may become dysregulated. Persistent stressors can trigger maladaptive epigenetic changes that disrupt normal gene expression. These shifts may contribute to ongoing inflammation, weakened barrier function, and altered immune responses. This is why epigenetics has become such an important and compelling focus within modern dermatological research.
Psoriasis and Epigenetic Alterations
If you live with psoriasis, you will already know how unpredictable the condition can feel. You may experience flare-ups during periods of stress or when you are unwell. Some people notice seasonal variation, with symptoms worsening in colder months. Although psoriasis has a recognised genetic component, genes alone do not fully explain when or why the disease begins.
Research has identified altered DNA methylation patterns in psoriatic skin compared with unaffected areas. These epigenetic differences can influence how certain inflammatory genes behave. In many cases, genes involved in immune signalling become overexpressed, contributing to persistent inflammation. Epigenetic changes also appear to affect immune cell activation and the rapid proliferation of keratinocytes, which leads to thickened plaques.
Environmental triggers such as infections, smoking, and psychological stress may modify these epigenetic marks over time. This means that your surroundings and lifestyle can influence how strongly certain genes are expressed. Such changes may partly explain why two individuals with similar genetic risk develop psoriasis differently. Epigenetics therefore helps bridge the gap between inherited susceptibility and real-world disease expression.
Eczema (Atopic Dermatitis) and the Skin Barrier
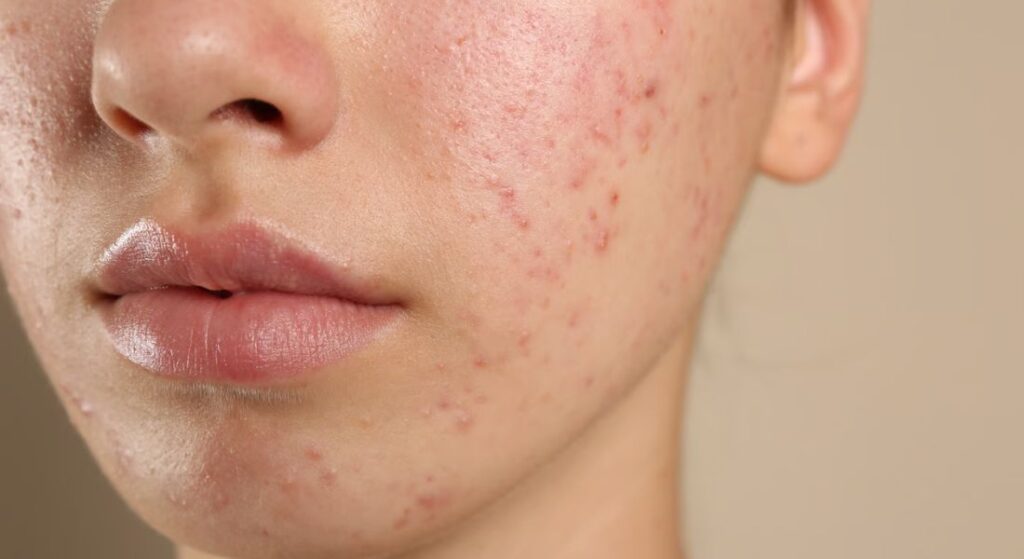
Eczema, also known as atopic dermatitis, is another condition in which epigenetics appears to play an important role. You may already know that mutations in the filaggrin gene are strongly associated with this condition. Filaggrin is essential for maintaining your skin barrier and preventing excessive water loss. When this barrier is weakened, your skin becomes more vulnerable to irritation and inflammation.
However, not everyone who carries a filaggrin mutation develops severe eczema. This suggests that genetic variation alone does not determine the outcome. Epigenetic mechanisms may influence how strongly the filaggrin gene is expressed in your skin. In other words, the gene may be present, but its level of activity can vary depending on regulatory signals.
Environmental exposures such as allergens, irritants, and pollution may alter DNA methylation patterns in genes linked to barrier function. These epigenetic shifts can worsen inflammation, dryness, and sensitivity over time. Early childhood exposure appears particularly significant, as infancy is a critical period for immune system development. Growing evidence suggests that epigenetic programming during this stage may shape your long-term immune responses and influence the severity of eczema later in life.
Acne and Hormonal Influence
Acne is often dismissed as a straightforward hormonal problem, particularly during adolescence. However, if you experience acne, you will know that it is far more complex than fluctuating hormones alone. Sebaceous gland activity, inflammation, microbial colonisation, and immune signalling all interact within your skin. These overlapping processes make acne a multifactorial condition rather than a single-cause disorder.
Epigenetic regulation may influence how your skin responds to hormonal signals, including the expression of androgen receptors. This can affect how strongly your sebaceous glands react to circulating hormones. Epigenetic mechanisms may also alter inflammatory pathways within sebocytes, shaping how your skin responds to blocked pores and bacteria. In this way, gene activity, rather than gene sequence alone, may contribute to acne severity.
Dietary factors, including high glycaemic load diets, are currently being studied for their potential epigenetic effects on acne-prone skin. Emerging research suggests that what you eat may influence gene expression linked to oil production and inflammation. Although this field is still developing, it highlights the possible connection between lifestyle and skin biology. This growing evidence supports the idea that environmental influences can shape gene activity in acne over time.
Pollution and Urban Skin Ageing
If you live in a city, your skin is exposed daily to particulate matter, exhaust fumes, and airborne toxins. Unlike occasional sun exposure, pollution is a constant environmental stressor that interacts with the skin at a molecular level. Increasing research suggests that urban living does not simply irritate the skin temporarily it may influence gene expression through epigenetic pathways. Over time, these subtle molecular shifts can translate into visible skin changes.
1. Oxidative Stress from Air Pollution: Air pollution generates reactive oxygen species, leading to oxidative stress within skin cells. This damages cellular components, including lipids, proteins, and DNA. Persistent oxidative stress accelerates the ageing process and weakens the skin barrier.
2. Altered DNA Methylation Patterns: Environmental pollutants have been linked to changes in DNA methylation within skin cells. These epigenetic alterations can modify how certain genes are expressed without changing the DNA sequence itself. Disrupted gene regulation may contribute to long-term structural and functional changes in the skin.
3. Pigmentation and Premature Ageing: Over time, pollution-related oxidative stress and epigenetic shifts may contribute to uneven pigmentation and fine lines. Increased melanin production and collagen breakdown are commonly observed effects. This can lead to earlier and more pronounced visible ageing in urban populations.
4. Inflammatory Skin Conditions: Airborne toxins can activate inflammatory pathways in susceptible individuals. Chronic low-grade inflammation may worsen conditions such as eczema or acne. Urban environments may therefore influence not only cosmetic ageing but also inflammatory skin health.
In conclusion, urban pollution affects the skin at both a surface and molecular level. Through oxidative stress and potential epigenetic changes such as altered DNA methylation, city living may accelerate pigmentation changes and premature ageing. These environmental influences could partly explain differences in skin health between urban and rural populations. Understanding this connection highlights the importance of protective skincare and environmental awareness.
Ultraviolet Radiation and Epigenetic Damage
Ultraviolet radiation does far more than cause temporary redness or sunburn. When your skin is exposed to excessive sunlight, direct DNA damage can occur within skin cells. This damage may disrupt normal cellular repair mechanisms and increase long-term risk. However, the effects of ultraviolet exposure extend beyond structural DNA injury.
UV radiation can also trigger epigenetic alterations that influence how certain genes are expressed. Chronic exposure may modify methylation patterns in genes responsible for tumour suppression and cell cycle control. When these protective genes are disrupted, your skin may become more vulnerable to abnormal cell growth. This has clear implications for the development of skin cancer over time.
Importantly, some epigenetic changes may persist even after sun exposure has ended. This means that the biological impact of UV radiation can continue long after visible tanning or burning has faded. Such lasting effects reinforce the importance of consistent and reliable sun protection. Regular use of broad-spectrum sunscreen and protective measures remains essential for long-term skin health.
Stress, Cortisol, and Gene Expression
You may notice that your skin condition worsens during periods of emotional or physical stress. Flare-ups can seem to appear without an obvious external trigger. Stress hormones, particularly cortisol, play a significant role in regulating immune signalling within your body. When these hormones remain elevated for prolonged periods, they can disrupt normal inflammatory balance in your skin.
Chronic stress may also induce epigenetic changes in genes linked to inflammation and immune response. These chemical modifications can alter how strongly certain inflammatory pathways are activated. Over time, this may increase your susceptibility to flare-ups in conditions such as psoriasis and eczema. In this way, stress does not simply affect how you feel; it can influence gene expression at a biological level.
The connection between your mind and skin is therefore not an abstract idea or psychological theory. It is increasingly measurable through molecular and epigenetic research. Scientists can now observe how stress-related signals affect cellular behaviour and gene regulation. This growing evidence highlights the importance of managing stress as part of a comprehensive approach to skin health.
The Microbiome and Epigenetic Crosstalk
Your skin is home to billions of microorganisms, including bacteria, fungi, and viruses. These microbes form a complex ecosystem known as the skin microbiome. They do not simply exist on the surface; they actively interact with your immune system. In many cases, this relationship helps maintain balance and protect against harmful pathogens.
Emerging research suggests that the composition of your microbiome may influence epigenetic regulation within skin cells. Certain microbial metabolites appear capable of affecting histone modification and altering patterns of gene expression. This means that microscopic organisms on your skin could indirectly shape how your genes behave. Such interactions highlight the close biological relationship between your environment and your genetic activity.
If the microbiome becomes disrupted, whether through antibiotics, harsh skincare, or environmental stress, there may be downstream epigenetic consequences. Changes in microbial balance could potentially influence inflammation and barrier function. Although this area of research is still in its early stages, it is scientifically compelling. It offers a new perspective on how microbial health and gene regulation may be interconnected in your skin.
Can Epigenetic Changes Be Reversed?
One of the most encouraging aspects of epigenetics is that many of its changes are potentially reversible. Unlike permanent DNA mutations, epigenetic marks can shift in response to internal and external influences. This means that altered gene expression patterns may not be fixed for life. For you, this opens the possibility that future treatments could actively modify harmful gene activity.
This reversibility creates opportunities for more targeted therapeutic strategies. Certain medications are already known to influence epigenetic pathways in other areas of medicine. For example, in oncology, drugs that target histone deacetylases are used clinically to regulate abnormal gene expression. These treatments demonstrate that epigenetic mechanisms can be modified in a controlled medical setting.
In dermatology, researchers are exploring whether similar approaches could help modulate inflammatory skin diseases. The aim would be to reduce inappropriate immune activation by adjusting gene regulation rather than suppressing the immune system broadly. However, achieving precision is complex, as epigenetic pathways are interconnected and influence many genes at once. Specificity and long-term safety therefore remain significant challenges before such therapies can become routine in skin care.
Implications for Personalised Dermatology

Personalised dermatology is increasingly guided by insights from epigenetics, recognising that genetic risk alone doesn’t dictate how a skin condition will present or progress. Each patient may have unique triggers and environmental exposures that influence disease expression. This approach emphasises tailoring care to the individual, rather than relying solely on standard treatment protocols. Considering lifestyle, stress, and broader health factors is essential for truly effective skin management.
1. Epigenetics and Personalised Care: Epigenetic research shows that two patients with identical genetic risks can experience very different outcomes. This means treatment plans must account for individual variability, rather than assuming a one-size-fits-all approach.
2. Environmental and Lifestyle Influences: Factors such as diet, pollution exposure, sleep patterns, and stress levels can all affect how skin conditions manifest. Understanding these influences allows dermatologists to target interventions more precisely.
3. Comprehensive Assessment: Consulting a specialist enables a holistic evaluation, incorporating medical history, lifestyle, and environmental context. This ensures that care plans address both visible symptoms and underlying contributing factors.
4. Tailored Management Strategies: Personalised dermatology encourages ongoing monitoring and adjustment of treatments. Regular follow-ups help refine strategies as patient circumstances and environmental exposures change.
Personalised dermatology represents a shift from reactive treatment to proactive, patient-focused care. By integrating genetics, epigenetics, and lifestyle factors, dermatologists can develop strategies that are far more precise and effective. Collaborating with experienced consultants ensures that your care plan reflects your unique profile, optimising outcomes and overall skin health.
Lifestyle Interventions and Epigenetic Influence
Although research is still emerging, certain lifestyle measures may help support healthier gene expression in your skin. Consistent sun protection, for example, can reduce UV-induced epigenetic changes that might otherwise disrupt tumour-suppressing genes. By shielding your skin from harmful radiation, you help maintain more stable gene regulation over time.
Balanced nutrition may also influence inflammatory pathways in the skin. Diets rich in antioxidants, healthy fats, and essential nutrients can provide the building blocks your cells need for repair and resilience. Adequate sleep further supports hormonal balance, which in turn affects gene expression related to inflammation and skin barrier function.
Stress management is another key factor, as chronic stress can drive cortisol-related changes in inflammatory gene activity. Techniques such as mindfulness, exercise, or relaxation routines may help mitigate these effects. While these interventions are not cures for genetic or epigenetic conditions, they align closely with emerging insights into how lifestyle can shape the way your genes are expressed.
Limitations of Current Research
It is important to remain realistic when considering epigenetics in dermatology. Much of the current evidence comes from laboratory experiments or small cohort studies, which may not fully reflect real-world outcomes. While these studies provide valuable insights, they cannot yet establish definitive cause-and-effect relationships between environmental exposures and specific gene changes.
Mapping every external factor to a precise epigenetic modification is not currently possible. The interactions between genes, lifestyle, and environment are highly complex. Even two people with similar genetics may respond very differently to the same exposures, highlighting the limits of our current understanding.
Individual variability adds another layer of complexity. Your epigenetic profile is shaped by decades of interactions between your genes and your environment, from early childhood through adulthood. This makes personalised predictions challenging and underscores the need for cautious interpretation of emerging research findings.
The Future of Epigenetic Therapies

In the coming years, we may see diagnostic tools that can measure epigenetic markers in your skin or blood. These tools could help predict disease severity, flare-up risk, or how you might respond to specific treatments. By providing a more personalised picture, they could guide more targeted and effective management strategies for conditions like psoriasis, eczema, and acne.
Researchers are also exploring targeted therapies designed to normalise specific methylation patterns or other epigenetic modifications. The aim would be to adjust gene expression directly, rather than only treating symptoms. Some studies are investigating combination approaches that integrate biologic medications with epigenetic modulators, potentially enhancing treatment precision and outcomes.
Although this is an exciting prospect, it remains a rapidly evolving research frontier. Many therapies are still in early experimental stages, and long-term safety and effectiveness have yet to be fully established. For now, understanding the potential of epigenetics offers insight into why your skin behaves the way it does and how future treatments may become more personalised and targeted.
What This Means for You
If you live with a chronic skin condition, understanding epigenetics can offer a powerful explanation for why symptoms vary so much between individuals. It highlights that your genes are not your destiny. The way your skin behaves is influenced by your environment, daily habits, and lifetime exposures, which all interact with your genetic makeup in complex ways.
At the same time, epigenetics reminds you to be cautious about simplistic solutions. No single supplement, cream, or product can “reset” your epigenome overnight or guarantee long-term change. True modification of gene expression is a gradual and highly regulated process.
The most reliable way to manage your skin remains informed, evidence-based dermatological care. Working with a qualified dermatologist ensures that you receive treatments supported by scientific research, while lifestyle adjustments can complement professional care to support your skin’s health over time.
FAQs:
1. What is epigenetics and how does it affect skin health?
Epigenetics refers to chemical modifications that regulate gene activity without changing the DNA sequence itself. These changes influence how genes are expressed, affecting processes such as skin barrier function, inflammation, and repair. Environmental factors and lifestyle can modulate these epigenetic mechanisms, impacting skin health over time.
2. How do epigenetic changes contribute to psoriasis?
In psoriasis, DNA methylation and other epigenetic modifications can alter inflammatory gene expression, immune cell activation, and keratinocyte proliferation. Environmental triggers such as stress, infections, and smoking can further influence these epigenetic marks, explaining variations in disease onset and severity among individuals with similar genetic risk.
3. Can epigenetics explain differences in eczema severity?
Yes. Although mutations in the filaggrin gene affect skin barrier integrity, epigenetic regulation determines how strongly this gene is expressed. Environmental exposures like allergens, pollutants, or irritants can modify DNA methylation patterns, influencing inflammation, dryness, and susceptibility to eczema flare-ups.
4. What role does epigenetics play in acne?
Epigenetic mechanisms can affect how skin responds to hormones and regulate sebaceous gland activity. They may also influence inflammatory pathways in sebocytes, impacting pore blockage and bacterial responses. Diet, lifestyle, and environmental exposures may further modulate gene expression relevant to acne severity.
5. How does pollution impact epigenetic regulation in the skin?
Air pollution generates oxidative stress and can alter DNA methylation patterns in skin cells. These epigenetic changes may disrupt gene expression related to barrier function, pigmentation, inflammation, and collagen production, contributing to premature ageing and exacerbating conditions like eczema and acne.
6. Can ultraviolet (UV) exposure cause epigenetic changes?
Yes. UV radiation can trigger epigenetic modifications that affect gene expression in tumour suppression, cell cycle regulation, and DNA repair. Some of these changes may persist after sun exposure ends, highlighting the importance of consistent sun protection to maintain long-term skin health.
7. How does stress influence gene expression in skin disease?
Chronic stress elevates cortisol levels, which can induce epigenetic changes in genes regulating inflammation and immune response. These modifications may increase susceptibility to flare-ups in conditions like psoriasis and eczema, showing a measurable link between mental health and skin biology.
8. Is the skin microbiome linked to epigenetic changes?
Emerging research suggests that microbial metabolites from the skin microbiome can affect histone modifications and gene expression. Disruptions in microbial balance through antibiotics, harsh skincare, or environmental stress may indirectly influence inflammation, barrier function, and skin disease progression.
9. Are epigenetic changes in the skin reversible?
Many epigenetic modifications are potentially reversible. Unlike permanent DNA mutations, chemical marks on genes can shift in response to lifestyle, environment, or therapeutic interventions. This opens the possibility for targeted treatments that modify harmful gene activity rather than altering DNA itself.
10. How can epigenetics inform personalised dermatology?
Epigenetic insights allow dermatologists to tailor treatments based on individual gene-environment interactions. By considering factors such as diet, pollution exposure, stress, and lifestyle, personalised care can optimise outcomes for conditions like psoriasis, eczema, and acne. This approach goes beyond genetics alone, recognising that gene expression is influenced by real-world circumstances.
Final Thoughts: Understanding Epigenetics for Better Skin Health
Epigenetics reveals that your genes are not your destiny. While inherited DNA provides a blueprint, environmental factors, lifestyle choices, stress, and the skin microbiome all interact to influence how those genes are expressed. This dynamic regulation helps explain why two people with similar genetic backgrounds can experience very different outcomes in conditions like psoriasis, eczema, and acne. By understanding these influences, you gain a clearer perspective on why your skin behaves the way it does and how targeted interventions both lifestyle and medical can make a meaningful difference.
For personalised guidance, it is essential to consult an experienced Dermatologist in London, who can assess your unique genetic and environmental profile and recommend appropriate care. If you’d like to book a consultation with one of our dermatologists, you can contact us at the London Dermatology Centre.
References:
1. Olejnik‑Wojciechowska, J., Boboryko, D., Bratborska, A.W., Rusińska, K., Ostrowski, P. and Baranowska, M. (2024) The Role of Epigenetic Factors in the Pathogenesis of Psoriasis, International Journal of Molecular Sciences https://www.mdpi.com/1422-0067/25/7/3831
2. Mervis, J.S. and McGee, J.S. (2020) DNA Methylation and Inflammatory Skin Diseases, Archives of Dermatological Research https://pubmed.ncbi.nlm.nih.gov/31696298/
3. Dopytalska, K., Ciechanowicz, P., Wiszniewski, K., Szymańska, E. and Walecka, I.(2021) The Role of Epigenetic Factors in Psoriasis, International Journal of Molecular Sciences, https://pmc.ncbi.nlm.nih.gov/articles/PMC8431057/
4. Barnes, B.M. and Shyne, A. (2024) Epigenetics and Ultraviolet Radiation: Implications for Skin Ageing and Carcinogenesis, Skin Health and Disease, https://academic.oup.com/skinhd/article/4/6/ski2.410/7950893
5. Zeng, C., et al. (2015) Epigenetics in psoriasis: methylation, histone modification and non‑coding RNAs, inEpigenetics and Dermatological Disease https://www.sciencedirect.com/science/chapter/edited-volume/abs/pii/B9780128009574000114