If you live with eczema, you have probably been told at some point that it is “genetic”. While that explanation is common, it often feels unsatisfying. You may wonder what genetics actually means for your skin, why your symptoms behave the way they do, and whether this knowledge changes how your condition should be managed.
One of the most significant genetic discoveries in eczema research involves the filaggrin gene. You may have heard it described as a key risk factor, but its role is often simplified. Filaggrin is not just another gene linked to eczema; it plays a central role in maintaining the skin barrier that protects you from irritants, allergens, and moisture loss.
When filaggrin does not function properly, your skin barrier becomes more fragile. This helps explain why your skin may feel dry, reactive, or prone to inflammation even before visible eczema appears. However, having a filaggrin mutation does not automatically mean you will develop eczema, which is why genetics alone never tells the full story.
What Is Filaggrin and Why Does It Matter?

Filaggrin is a structural protein that plays a vital role in keeping your skin barrier strong and functional. Your skin depends on filaggrin to maintain hydration, provide mechanical strength, and protect against external irritants. Without it, the barrier that separates your body from the environment becomes compromised.
You produce filaggrin in the upper layers of the epidermis, where it helps skin cells mature, flatten, and pack tightly together. This process forms the outer protective layer of your skin, limiting water loss and preventing allergens, microbes, and irritants from penetrating too easily. Filaggrin also breaks down into natural moisturising factors that help your skin retain water and maintain the correct pH.
When filaggrin levels are reduced or the protein does not function properly, your skin barrier becomes weaker. This leads to increased dryness, heightened sensitivity, and a greater tendency toward inflammation. Over time, this fragile barrier makes your skin more reactive, helping to explain why eczema-prone skin flares so easily and struggles to recover fully between episodes.
How the Filaggrin Gene Works
The filaggrin gene (FLG) is essential for maintaining a strong, functional skin barrier. It controls key processes that keep the skin hydrated, flexible, and protected from irritants and microbes. When this system works properly, the skin remains resilient and balanced.
- Role of the Filaggrin Gene (FLG): FLG provides the instructions to produce profilaggrin, a precursor protein in the skin. During normal skin maturation, profilaggrin is broken down into filaggrin in the upper layers of the epidermis. This process is crucial for building a structured and resilient skin barrier.
- Filaggrin and Natural Moisturising Factors (NMFs): Filaggrin is further degraded into natural moisturising factors (NMFs). These small molecules help the skin retain water, maintain elasticity, and support a slightly acidic surface pH. This acidic environment supports healthy enzyme activity and helps control harmful bacteria.
- Impact of FLG Mutations: Mutations in the FLG gene disrupt the normal conversion of profilaggrin into filaggrin. As a result, fewer NMFs are produced and the skin barrier weakens. This leads to increased water loss, dryness, and greater susceptibility to irritation and inflammation.
The filaggrin gene plays a foundational role in skin barrier integrity. When its function is impaired, the skin becomes dry, fragile, and more prone to inflammatory conditions such as eczema.
What Happens When Filaggrin Is Deficient?
When filaggrin is deficient, the skin barrier begins to fail in multiple ways at the same time. One of the earliest changes is increased transepidermal water loss. Your skin is no longer able to retain moisture efficiently, leading to chronic dryness that often develops before any redness or itching becomes visible.
As hydration levels drop, the tightly packed structure of the outer skin layer loosens. Microscopic gaps form between skin cells, weakening the barrier that normally keeps the external environment out. This makes the skin far more permeable to allergens, irritants, and microbes that would otherwise be blocked.
Once these substances penetrate the skin, they trigger immune activation and inflammation. Bacteria such as Staphylococcus aureus can colonise more easily, further aggravating symptoms. Over time, this cycle of dryness, barrier disruption, and inflammation significantly increases the risk of developing eczema and sustaining repeated flares.
Filaggrin Mutations and Skin Barrier Breakdown
Your skin barrier functions much like a brick wall. The skin cells form the bricks, while lipids and structural proteins such as filaggrin act as the mortar that holds everything together. This arrangement creates a strong, flexible barrier that protects against water loss and external irritants.
When filaggrin levels are reduced due to genetic mutations, the mortar begins to weaken. Even though the skin may appear intact on the surface, microscopic cracks develop within the barrier. These defects compromise the skin’s ability to retain moisture and maintain its protective role.
As a result, irritants, allergens, and microbes can penetrate more easily into deeper skin layers. This intrusion activates immune responses, leading to inflammation and itching. Over time, this barrier breakdown becomes a key driver of eczema development and ongoing disease activity.
Why Filaggrin Mutations Increase Eczema Risk
Research consistently shows that filaggrin mutations are among the strongest genetic risk factors for eczema. However, carrying a mutation does not automatically mean you will develop the condition. Genetics increase susceptibility, but they do not act in isolation.
When a filaggrin mutation is present, the skin barrier begins life at a structural disadvantage. Reduced barrier integrity makes the skin less able to retain moisture and more vulnerable to external triggers such as allergens, irritants, microbes, and climate changes. As a result, everyday environmental exposures have a much greater impact on the skin.
This gene–environment interaction helps explain why eczema varies so widely between individuals. Some people with filaggrin mutations develop severe, early-onset disease, while others experience mild or intermittent symptoms. It also explains why barrier-focused prevention and early intervention can significantly influence long-term outcomes.
Why Not Everyone with a Filaggrin Mutation Gets Eczema
Having a filaggrin (FLG) mutation does not automatically lead to eczema. While reduced filaggrin weakens the skin barrier, eczema develops only when multiple factors interact. This explains why some people with the mutation never experience symptoms.
- Filaggrin Deficiency Increases Vulnerability, Not Certainty: An FLG mutation weakens the skin barrier, making it more prone to irritation and water loss. However, filaggrin deficiency alone is not enough to cause eczema. Additional genetic, immune, or environmental triggers are required.
- Role of the Immune System: Individuals with less reactive immune responses may tolerate barrier weakness without excessive inflammation. Th2-dominant immune tendencies increase the likelihood of eczema developing. Immune balance plays a critical role in determining outcomes.
- Environmental and Lifestyle Influences: Climate, stress, skincare habits, and exposure to allergens or irritants can influence whether symptoms appear. Protective environments may prevent inflammation, while harsh conditions can trigger it. Daily habits often shape disease expression.
- Adaptive Compensatory Mechanisms in the Skin: The skin can increase production of other barrier proteins, lipids, and repair pathways. These adaptations partially compensate for reduced filaggrin function. Such mechanisms help explain why eczema does not develop in everyone with an FLG mutation.
Eczema arises from a complex interaction between genetics, immune response, and environmental exposure. While filaggrin mutations increase susceptibility, compensatory mechanisms and external factors determine whether the condition actually develops.
Environmental Triggers That Interact with Filaggrin Deficiency
When your skin barrier is compromised due to filaggrin deficiency, ordinary environmental exposures can have an outsized effect. Even mild irritants, such as soaps or detergents, may penetrate more easily and provoke inflammation.
Low humidity and frequent washing can strip moisture from already fragile skin, worsening dryness and making it more prone to eczema flares. Airborne allergens like dust, pollen, or pet dander also interact with the weakened barrier, increasing the likelihood of irritation.
Early-life exposures are particularly influential, as they can shape the skin’s long-term response to environmental stress. Understanding these triggers helps explain why some individuals with filaggrin deficiency develop eczema early, while others may remain symptom-free despite carrying the same mutation.
Filaggrin Mutations and Childhood Eczema
Filaggrin mutations play a major role in childhood eczema, with many children showing symptoms within their first year. At this age, the skin barrier is still developing, making it particularly vulnerable to environmental stressors and allergens.
A weakened barrier due to filaggrin deficiency allows irritants and microbes to penetrate more easily, triggering inflammation and the characteristic dryness and redness of eczema. Early signs may include persistent dryness, redness, or itchiness, often before more obvious rashes appear.
Recognising filaggrin-related risk early is important. Prompt intervention with gentle skincare, moisturisation, and, when needed, medical treatment can help support the barrier and may reduce the severity or frequency of eczema as the child grows.
Adult Eczema and Filaggrin Deficiency
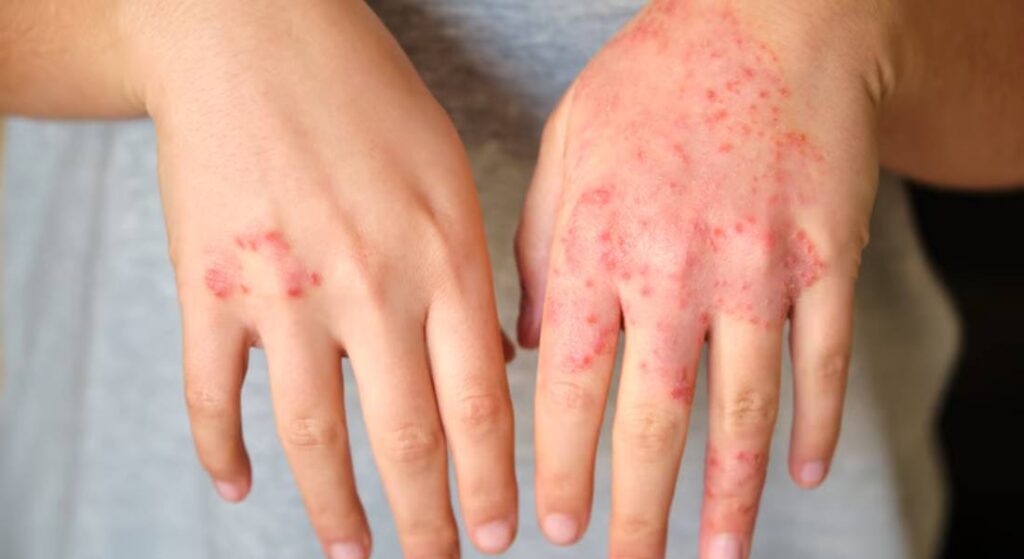
Filaggrin mutations don’t only affect children; they can also contribute to adult eczema. In adults, symptoms often differ, presenting as chronic hand eczema, persistent dry patches, or flare-ups in previously unaffected areas.
Over time, the skin accumulates environmental stress from factors like repeated washing, irritants, and allergens. When filaggrin is deficient, the barrier is less able to cope, making these stresses more likely to trigger or worsen eczema.
This delayed vulnerability helps explain why some people develop eczema later in life or why pre-existing conditions can flare despite previous periods of clear skin. Understanding filaggrin’s role can guide targeted skincare and preventative strategies for adults.
The Link Between Filaggrin and Other Atopic Conditions
Filaggrin mutations affect more than just the skin they are also linked to other atopic conditions, such as asthma and allergic rhinitis. These mutations weaken the skin barrier, making it easier for allergens and irritants to penetrate and interact with the immune system.
This process is part of the “atopic march,” where early skin barrier defects increase immune sensitisation. When allergens enter through compromised skin, the immune system may overreact, setting the stage for allergic responses in other organs, particularly the lungs and nasal passages.
Over time, this heightened immune activity can lead to a broader spectrum of atopic diseases. Understanding this connection highlights the importance of early skin barrier support in individuals with filaggrin deficiency, as it may reduce the risk of developing subsequent allergic conditions.
How Filaggrin Deficiency Affects Skin Microbiome Balance
Filaggrin deficiency doesn’t just weaken the skin barrier—it also alters the balance of microbes living on the skin. A healthy barrier helps regulate which bacteria thrive, but when filaggrin is lacking, harmful microbes can take hold more easily.
One of the most common offenders is Staphylococcus aureus, which can trigger inflammation, increase itching, and worsen eczema flare-ups. This imbalance can create a cycle where barrier disruption and microbial overgrowth feed into each other, making symptoms harder to control.
For this reason, modern eczema care focuses not only on repairing the skin barrier with moisturisers and barrier-supporting treatments but also on managing the skin’s microbiome. Strategies may include gentle cleansing, topical therapies, and sometimes targeted antimicrobial interventions, all aimed at restoring a balanced environment that supports long-term skin health.
Can Filaggrin Levels Be Tested Clinically?
Currently, routine testing for filaggrin levels or mutations is not part of standard clinical practice. Most eczema diagnoses are made based on visible skin features, patient history, and patterns of flare-ups rather than genetic testing.
That said, knowing that a patient may have filaggrin deficiency can influence treatment choices. For example, clinicians may prioritise intensive barrier repair, early intervention, and strategies to prevent skin dryness and microbial imbalance. This awareness allows for a more proactive approach, even without formal genetic confirmation.
Research is ongoing to develop easier, more accessible ways to measure filaggrin function. In the future, such tests could help personalise eczema care further, identifying individuals at higher risk and enabling targeted preventative strategies.
How Filaggrin Research Changed Eczema Treatment Approaches
Research on filaggrin has fundamentally changed how we approach eczema treatment. Previously, care focused primarily on controlling inflammation, but we now recognise that a weakened skin barrier is often the root problem. Supporting and repairing this barrier is central to long-term disease management.
Clinicians increasingly emphasise the regular use of emollients and moisturisers. This isn’t just about keeping the skin soft it actively compensates for filaggrin deficiency, helping to maintain hydration, reduce cracks between skin cells, and protect against irritants and allergens.
By prioritising barrier repair alongside anti-inflammatory therapies, patients often experience fewer flares and milder symptoms. Understanding filaggrin has shifted eczema care from reactive treatment to a more proactive, preventative strategy, improving both short-term comfort and long-term skin health.
Modern Barrier-Focused Treatments
Modern eczema care places a strong emphasis on barrier-focused treatments. These therapies are designed to compensate for the effects of filaggrin deficiency, restoring hydration, lipids, and overall skin integrity. By addressing the underlying barrier weakness, they help reduce vulnerability to irritants, allergens, and microbial imbalance.
Ceramide-rich moisturisers are a cornerstone of this approach. Ceramides reinforce the “mortar” between skin cells, strengthening the barrier, while humectants attract and retain water in the outer layers of skin. Together, they help maintain elasticity, smoothness, and protective function.
Consistency is key for long-term success. Regular, ongoing application ensures the skin remains resilient, reduces the frequency of flares, and supports overall skin health. Barrier-focused care, when combined with targeted anti-inflammatory treatments, forms a modern, evidence-based approach to managing eczema.
Anti-Inflammatory Treatments Still Matter
Barrier repair is crucial in managing eczema, but controlling inflammation remains equally important. Even with a strong skin barrier, immune responses triggered by irritants, allergens, or filaggrin deficiency can cause redness, itching, and flare-ups.
Topical anti-inflammatory treatments, including corticosteroids and non-steroidal alternatives, help calm these immune responses. They reduce swelling, redness, and discomfort while allowing the skin to heal.
When used appropriately and in combination with barrier-focused care, these treatments prevent long-term skin damage, reduce flare frequency, and support overall skin health. This dual approach repairing the barrier and controlling inflammation is central to modern eczema management.
Personalised Treatment and Genetic Risk
Filaggrin research has highlighted the importance of personalised approaches to eczema care. Genetic differences mean that not every patient experiences the same triggers, symptoms, or treatment responses.
For patients whose eczema is closely linked to barrier dysfunction, strategies that focus on intensive moisturisation and barrier repair are particularly valuable. These interventions help restore hydration, strengthen the skin’s protective function, and reduce flare frequency.
By considering genetic risk alongside clinical presentation, dermatologists can design long-term management plans that are tailored to each individual. This approach improves outcomes, supports skin health, and empowers patients to participate actively in their care.
Daily Skincare Habits for Filaggrin-Deficient Skin
For filaggrin-deficient skin, daily care plays a crucial role in supporting a weakened skin barrier. Gentle, consistent routines help retain moisture, reduce irritation, and lower the risk of eczema flare-ups. Small habits, done regularly, make a meaningful difference over time.
- Gentle Cleansing: Use mild, non-fragranced cleansers to minimise irritation and barrier disruption. Avoid harsh soaps or strong surfactants that strip natural oils. Gentle cleansing helps preserve the skin’s protective function.
- Moisturising Immediately After Washing: Apply moisturiser while the skin is still slightly damp to lock in hydration. Regular moisturising reduces water loss and supports barrier repair. Consistent use improves skin comfort and flexibility.
- Consistency Matters: Daily skincare habits build resilience gradually rather than delivering instant results. Regular care helps reduce flare-ups and maintain overall skin health. Long-term consistency is especially important for managing filaggrin deficiency.
Consistent gentle cleansing and timely moisturising are central to caring for filaggrin-deficient skin. Protecting the skin barrier daily improves hydration, reduces irritation, and supports healthier skin over time.
Can Filaggrin Deficiency Be Reversed?
Filaggrin deficiency cannot be reversed because it is genetic, but you can support your skin through targeted care. Focusing on barrier repair helps compensate for the protein your skin lacks.
Early and consistent interventions, such as regular moisturisation with ceramide-rich products and gentle cleansing, can make a meaningful difference in reducing dryness and preventing flare-ups.
Research is ongoing into therapies that may enhance filaggrin expression or mimic its function. While we cannot change your genes, these advances offer hope for more effective, personalised management in the future.
The Role of Diet and Lifestyle
Filaggrin deficiency cannot be reversed because it is genetic, but you can support your skin through targeted care. Focusing on barrier repair helps compensate for the protein your skin lacks.
Early and consistent interventions, such as regular moisturisation with ceramide-rich products and gentle cleansing, can make a meaningful difference in reducing dryness and preventing flare-ups.
Research is ongoing into therapies that may enhance filaggrin expression or mimic its function. While we cannot change your genes, these advances offer hope for more effective, personalised management in the future.
When to Seek Specialist Care
If your eczema continues to flare despite standard care, it’s important to seek specialist input. Ongoing or severe symptoms may point to more complex barrier dysfunction or underlying factors that require expert evaluation.
A dermatologist can carefully assess your triggers, review how your skin responds to treatments, and recommend therapies tailored to your needs. This ensures both effective symptom control and long-term skin health.
Accessing specialist eczema care in London provides the benefit of a personalised, evidence-based plan. Working with an expert helps you manage flares more effectively and supports strategies to maintain healthy, resilient skin over time.
What Current Research Is Exploring
Researchers are investigating how filaggrin influences interactions between the immune system, skin microbes, and environmental factors. Understanding these pathways may reveal why some people are more prone to eczema than others.
New therapies are being developed to target these mechanisms directly. Topical barrier enhancers and biologic treatments are evolving quickly, offering options that go beyond simply managing symptoms.
These advances bring hope for improved long-term control of eczema. By addressing the underlying biology, future treatments may provide more personalised and effective care for those affected by filaggrin-related skin barrier issues.
What This Means for You

Filaggrin mutations help explain why eczema varies so much between individuals. Your symptoms, triggers, and response to treatment are influenced by your skin’s genetic makeup.
This knowledge emphasises the importance of prevention and consistent maintenance. Daily skincare routines that support the barrier can make a significant difference in reducing flare-ups and protecting your skin.
Understanding how your skin works empowers you to make informed decisions about treatment and lifestyle. Being aware of filaggrin’s role is a key step toward more effective, personalised eczema management.
FAQs:
1. What is the filaggrin gene and why is it important in eczema?
The filaggrin gene helps your skin form a strong protective barrier. When it does not work properly, the skin loses moisture more easily and becomes more sensitive to irritants, increasing the risk of eczema.
2. Does having a filaggrin mutation mean I will definitely get eczema?
No. A filaggrin mutation increases your risk, but it does not guarantee eczema. Environmental factors, immune responses, and skincare habits all influence whether symptoms develop.
3. How does filaggrin deficiency affect the skin barrier?
Low or faulty filaggrin weakens the outer skin layer, allowing water to escape and irritants, allergens, and microbes to enter more easily. This makes the skin drier, more reactive, and prone to inflammation.
4. Why does eczema vary so much between people with filaggrin mutations?
Everyone’s immune system, lifestyle, and environment are different. Some skin can partially compensate for reduced filaggrin, while others react strongly, leading to frequent or severe flare-ups.
5. Is filaggrin deficiency more important in childhood eczema?
Yes. Many children with eczema have filaggrin-related barrier weakness. Because infant skin is still developing, this makes it more vulnerable to dryness, irritation, and early eczema symptoms.
6. Can filaggrin mutations cause eczema in adults too?
They can. In adults, filaggrin deficiency may contribute to chronic hand eczema, persistent dry patches, or flare-ups later in life, especially with repeated exposure to irritants or frequent washing.
7. How do environmental triggers interact with filaggrin deficiency?
When the skin barrier is weak, everyday triggers like soaps, detergents, cold weather, low humidity, or allergens can penetrate more easily and trigger inflammation or itching.
8. Can filaggrin levels or mutations be tested clinically?
Routine genetic testing is not usually done for eczema. Dermatologists diagnose eczema based on symptoms and skin behaviour, but knowledge of filaggrin deficiency can still guide treatment choices.
9. How has filaggrin research changed eczema treatment?
Treatment now focuses strongly on repairing and protecting the skin barrier, not just reducing inflammation. Regular moisturising and barrier support are seen as essential parts of long-term management.
10. Can filaggrin deficiency be cured or reversed?
No, because it is genetic. However, consistent barrier-focused skincare, gentle cleansing, and appropriate medical treatments can effectively manage symptoms and reduce flare-ups.
Final Thoughts: What Filaggrin Research Means for Your Eczema Care
Filaggrin gene research has transformed how we understand eczema, shifting the focus from seeing it as purely an inflammatory condition to recognising it as a disease rooted in skin barrier weakness. Knowing how filaggrin affects moisture retention, barrier integrity, and immune activation helps explain why eczema behaves differently from one person to another and why long-term management must go beyond treating flares alone.
This science reinforces the importance of consistent, barrier-focused skincare combined with targeted anti-inflammatory treatment when needed. By supporting the skin’s structure every day, you can reduce flare frequency, improve resilience, and gain better long-term control of symptoms, even when genetic risk is present.
If you’re thinking about eczema treatment in London, you can contact us at London Dermatology Centre to book a consultation with one of our specialists. A personalised assessment allows your care to be tailored to your skin’s unique barrier needs, helping you manage eczema more effectively and confidently over time.
References:
- Brown, S.J. and Irvine, A.D., 2008. Atopic eczema and the filaggrin story. Seminars in Cutaneous Medicine and Surgery https://pubmed.ncbi.nlm.nih.gov/18620134/
- Smith, F.J.D., et al., 2010. Filaggrin loss‑of‑function mutations are associated with early‑onset eczema, eczema severity and transepidermal water loss at 3 months of age. https://academic.oup.com/bjd/article-abstract/163/6/1333/6643928
- Hoyer, C., et al., 2022. Filaggrin gene mutations and eczema in infants. British Journal of Dermatology, https://academic.oup.com/bjd/article-abstract/186/3/e114/6705821
- McGrath, J.A., 2008. Filaggrin and eczema: a unifying hypothesis. Dermatology Clinics https://pubmed.ncbi.nlm.nih.gov/19720209/
- Thyssen, J.P. and Kezic, S., 2014. The role of filaggrin in the skin barrier and disease development. Journal of Dermatological Science, https://www.sciencedirect.com/science/article/pii/S1578219014003333