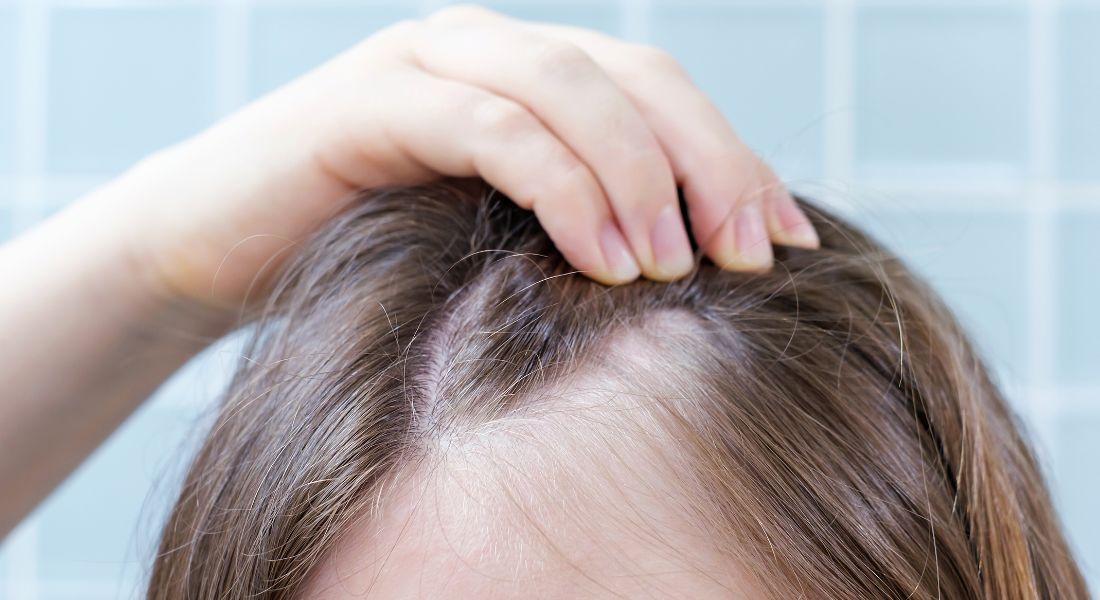
Frontal fibrosing alopecia (FFA) causes permanent hair loss along the frontal hairline and eyebrows. You may notice thinning, small patches breaking, or your forehead appearing higher. Early detection is crucial to protect the hair you still have.
It mostly affects women, especially after menopause, but genetics, immune activity, and environmental factors also play a role. Eyebrow thinning and subtle scalp inflammation are often early signs.
Treatment slows progression rather than restores lost hair. Topical or systemic medications, sometimes combined with steroid injections, reduce inflammation and protect follicles. Consistency and follow-up are key.
Gentle hair care and avoiding harsh chemicals help, while cosmetic options like microblading can boost confidence. Early specialist advice and monitoring give the best chance to maintain hair and manage the emotional impact.
What Is Frontal Fibrosing Alopecia?
Frontal fibrosing alopecia (FFA) is a form of scarring hair loss in which inflammation permanently damages hair follicles. Once a follicle is destroyed, hair cannot regrow. This makes early recognition particularly important. The condition progresses gradually over time.
FFA most commonly affects the frontal hairline, temples, and eyebrows. You may notice a smooth, band-like recession of the hairline that slowly advances. Eyebrow thinning or loss is also frequent. Changes often develop subtly at first.
The skin in affected areas can appear shiny or unusually smooth. FFA is closely linked to lichen planopilaris, an inflammatory scalp disorder. Your immune system mistakenly attacks the hair follicles, and ongoing inflammation leads to permanent hair loss. Understanding this process helps explain why early treatment focuses on control rather than regrowth.
Why Is It More Common in Women?

Frontal fibrosing alopecia (FFA) is a type of scarring hair loss where inflammation permanently destroys hair follicles. Once follicles are damaged, hair cannot regrow, which makes early recognition and treatment essential.
FFA most commonly affects the frontal hairline, temples, and eyebrows. Over time, the hairline may recede in a smooth, uniform pattern, and thinning can gradually become more obvious.
The skin in affected areas can appear shiny or unusually smooth. Early changes are often subtle, so you may not notice them until the recession progresses.
FFA is considered a variant of lichen planopilaris, an inflammatory scalp disorder. In this condition, the immune system attacks the follicles, and ongoing inflammation is the main cause of permanent hair loss.
Why Does It Seem to Be Increasing?
FFA appears to be increasing for several reasons, although no single cause fully explains the trend. Greater awareness among doctors and patients means the condition is recognised and diagnosed more often than in the past. What was once overlooked or mislabelled is now more clearly identified. Earlier diagnosis makes the condition seem more common.
Hormonal and immune factors are also thought to play a role. FFA is most frequently seen in post-menopausal women, suggesting hormonal changes may influence disease onset. At the same time, it behaves like an autoimmune condition, where your immune system mistakenly targets hair follicles. Shifts in immune regulation may be contributing to rising case numbers.
Environmental factors are another area of active research. Some studies have explored links with skincare products, sunscreens, and other leave-on cosmetics, although no definitive cause has been proven. These exposures may act as triggers in genetically susceptible individuals. The increase may reflect a combination of susceptibility and modern lifestyle factors.
Early Hairline Changes to Recognise
Frontal fibrosing alopecia (FFA) is a scarring type of hair loss in which inflammation permanently destroys hair follicles. Once follicles are lost, regrowth is impossible, making early recognition and timely treatment essential to protect the hair that remains. Without intervention, hairline recession progresses steadily, and cosmetic and psychological impact can become significant.
- Typical pattern of hair loss: FFA predominantly affects the frontal hairline, temples, and eyebrows. Hairline recession is often smooth and uniform, developing gradually over months or years, which can make early changes easy to overlook.
- Subtle early signs: The skin over affected areas may look shiny, taut, or unusually smooth. Minor changes are often missed without careful observation or serial photographs, which can help track progression before noticeable thinning occurs.
- Underlying mechanism: FFA is a variant of lichen planopilaris. The immune system mistakenly attacks hair follicles, triggering chronic inflammation that ultimately destroys the follicle. Understanding this autoimmune-driven process highlights why early intervention matters.
- Importance of specialist input: Dermatologists can confirm the diagnosis, monitor disease activity, and start therapies aimed at reducing inflammation, preserving existing hair, and slowing progression. Early intervention often yields the best outcomes, even if regrowth is limited.
- Adjunct considerations: Eyebrow involvement can occur early, and some patients report mild scalp irritation or tingling before visible thinning. Monitoring other hair-bearing areas and scalp health can guide holistic treatment.
Timely recognition, careful monitoring, and consistent specialist management give the best chance of maintaining hair and minimising irreversible loss. Acting early not only preserves hair but also reduces the psychological burden associated with progressive scarring alopecia.
Eyebrow Thinning and Loss
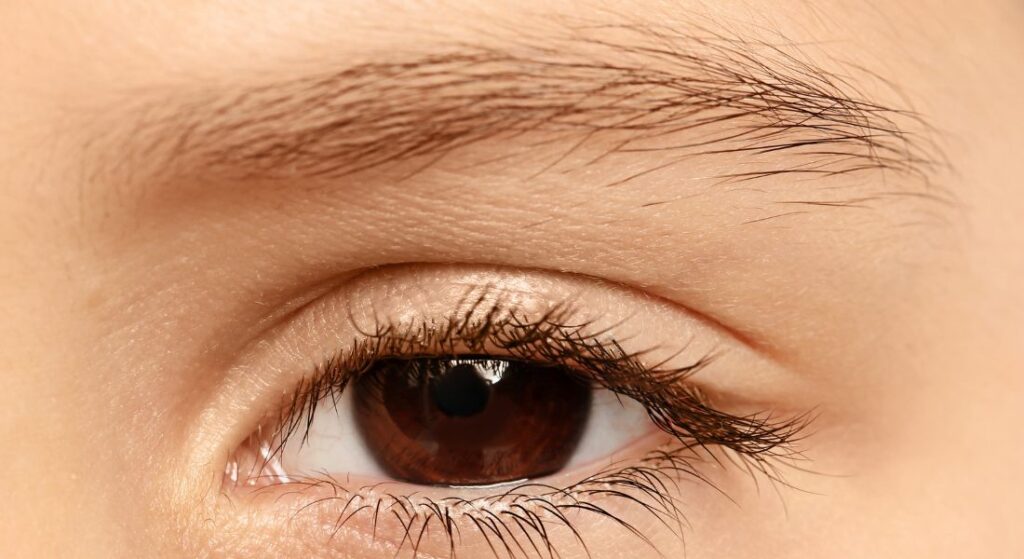
Eyebrow thinning is often one of the first signs of FFA. You may notice hair loss starting at the outer third of the brow, and in some cases, the entire eyebrow can become sparse.
For some women, eyebrow changes appear before any scalp involvement. This can make it easy to dismiss as normal ageing, delaying recognition and treatment.
Early assessment by a specialist can determine if inflammation is active. Treating at this stage often preserves the remaining eyebrow hairs.
Delaying treatment increases the risk of permanent loss. Acting quickly gives the best chance to maintain your eyebrows and overall appearance.
Other Areas That May Be Affected
Although the frontal scalp is most commonly affected, FFA can involve other areas of the body. You may notice thinning of the sideburns, loss of facial hair, or reduced hair growth on the arms and legs. These changes are often subtle and develop gradually. They can easily be overlooked without careful observation.
These wider patterns of hair loss highlight that FFA is a more general inflammatory condition. Your immune system does not always limit its activity to a single area, even though the scalp remains the most visible site. Involvement beyond the hairline can indicate ongoing disease activity. This helps explain why monitoring is important.
Noticing changes in less obvious areas can support earlier diagnosis. Small shifts in hair density elsewhere may provide clues before significant scalp recession occurs. A full scalp and skin examination by a specialist is therefore recommended. This allows all affected areas to be identified and monitored effectively over time.
Symptoms Beyond Hair Loss
Although the frontal scalp is most commonly affected, FFA can cause symptoms beyond hair loss at the hairline. You may notice thinning of the sideburns or facial hair, and some women also experience reduced hair on the arms or legs. These changes reflect the broader inflammatory nature of the condition, where the immune system can affect multiple areas.
Paying attention to subtle changes outside the scalp can help support earlier diagnosis. Hair loss in these regions may indicate ongoing disease activity, even when scalp changes seem mild. A thorough scalp and skin examination by a specialist is therefore recommended. This allows all affected areas to be assessed and monitored to protect as many follicles as possible.
The Role of the Immune System
Although your frontal scalp is usually the first and most noticeable area affected, FFA can involve other parts of your body as well. You may notice thinning of the sideburns or facial hair, and in some cases, reduced hair on the arms or legs. These changes can develop gradually and are easy to overlook at first.
This wider pattern highlights that FFA is a systemic inflammatory condition. Your immune system can target multiple hair-bearing areas, even when scalp involvement remains the main concern.
Paying attention to subtle hair loss beyond your hairline can support earlier recognition. Noticing these patterns may offer valuable clues about how active the condition is and how it may progress.
A thorough scalp and skin examination by a specialist is essential. This allows all affected areas to be identified and monitored, helping treatment protect as many follicles as possible and slow overall progression.
Genetic Susceptibility
Although the frontal scalp is the most obvious site of FFA, the condition can extend to other hair-bearing regions. Sideburns, facial hair, and even hair on the arms or legs may thin over time, often gradually and unnoticed, which can delay recognition of the broader disease pattern.
- FFA is systemic, not just scalp-limited: The immune system can target follicles throughout the body, meaning scalp involvement is only part of the picture. Peripheral hair loss may reflect ongoing systemic inflammation that needs addressing to preserve overall hair health.
- Subtle signs provide diagnostic clues: Early thinning in secondary areas can indicate active disease and alert clinicians to potentially aggressive progression. Recognising these signs may allow therapy to be started sooner.
- Importance of comprehensive assessment: Dermatologists examine both scalp and peripheral sites to identify all affected areas, ensuring monitoring is complete and treatment is targeted effectively.
- Treatment strategy relies on scope of involvement: Understanding which areas are affected helps guide therapy choices, from topical anti-inflammatories to systemic agents, with the goal of protecting as many follicles as possible.
- Monitoring progression over time: Regular follow-ups allow clinicians to track disease activity, adjust medications, and intervene early if new areas become involved, aiming to slow or halt irreversible follicular loss.
- Patient awareness enhances outcomes: Educating patients to notice subtle hair thinning beyond the scalp can prompt earlier evaluation and intervention, improving long-term hair preservation and reducing anxiety about progression.
FFA is more than just frontal hairline recession; it is a systemic inflammatory condition. Comprehensive evaluation, vigilant monitoring, and early recognition of peripheral hair loss are critical to controlling disease activity and maximising the preservation of hair across all affected areas.
How Is It Diagnosed?
Although the frontal scalp is the most obvious site of FFA, the condition can affect other hair-bearing areas. Sideburns, facial hair, and even hair on the arms or legs may thin gradually, often unnoticed, which can delay recognition of the broader disease.
FFA is not limited to the scalp the immune system can target follicles throughout the body. Peripheral hair loss may indicate ongoing inflammation and highlight the need for a more comprehensive treatment approach.
Early thinning in secondary areas provides important clues. Recognising these subtle signs allows your specialist to start therapy sooner, protecting more follicles and slowing progression.
A full scalp and skin assessment is essential. Regular monitoring helps track disease activity, adjust medications if needed, and maximise hair preservation across all affected regions.
Medical Treatments to Slow Progression
Although there is currently no cure for FFA, treatment focuses on slowing or stopping progression. You are often prescribed topical corticosteroids to reduce inflammation in affected areas of the scalp.
These may be combined with calcineurin inhibitors to enhance anti-inflammatory control. Your treatment plan is personalised, taking into account disease activity, the extent of hairline involvement, and your overall health.
If your condition is more active, oral medications such as hydroxychloroquine may be considered. In selected cases, anti-androgen therapies can also play a role, depending on your individual risk factors and clinical profile.
The primary goal of treatment is stabilisation rather than regrowth. Regular follow-up is essential to ensure treatment remains effective, and early intervention gives you the best chance of preserving existing hair over the long term.
Can Hair Grow Back?
Although there is no cure for FFA, treatment focuses on slowing or halting progression. Topical corticosteroids are commonly prescribed to calm inflammation at affected areas and protect remaining follicles.
These are often combined with calcineurin inhibitors to enhance effectiveness. Treatment plans are tailored to each patient, taking into account disease activity, hairline involvement, and overall health.
In more active or widespread cases, oral medications such as hydroxychloroquine may be recommended. Selected patients may also benefit from anti-androgen therapies, depending on hormonal factors and individual risk profiles.
The primary goal is stabilisation rather than hair regrowth. Regular follow-up allows your specialist to monitor progress, adjust therapy if needed, and intervene early to preserve as much hair as possible over the long term.
The Psychological Impact
Although there is no cure for FFA, the main focus of treatment is to slow or stop its progression. Topical corticosteroids are often used to reduce inflammation and help protect the follicles that are still healthy.
These are frequently combined with calcineurin inhibitors for added effect. Each treatment plan is personalised, considering how active the disease is, the areas affected, and the patient’s overall health.
For more active or widespread cases, oral medications such as hydroxychloroquine may be prescribed. In selected patients, anti-androgen therapies can also be helpful, depending on hormonal status and individual risk factors.
The goal is stabilisation rather than regrowth. Regular follow-up appointments allow your specialist to track progress, adjust treatment if necessary, and intervene early to preserve as much hair as possible over time.
Monitoring and Follow-Up
Although there is no cure for FFA, the primary goal of treatment is to slow or stop progression and protect remaining healthy follicles. Early recognition and prompt intervention are crucial, as irreversible hair loss occurs once follicles are destroyed. Treatment is tailored to disease activity, affected areas, and the patient’s overall health.
- Topical corticosteroids: These remain the cornerstone for reducing local inflammation and preserving follicles in early or limited disease. Careful application helps minimise side effects while maximising effectiveness.
- Combination with calcineurin inhibitors: Often used alongside corticosteroids, these agents provide additional anti-inflammatory benefits, especially in sensitive areas like the eyebrows or frontal hairline.
- Oral therapies for more active disease: Hydroxychloroquine or similar systemic agents may be prescribed when scalp involvement is extensive or progression is rapid, controlling inflammation beyond topical reach.
- Hormonal and targeted therapies: Anti-androgen medications can be considered for patients whose hormonal profile contributes to disease activity, providing another layer of personalised intervention.
- Regular specialist monitoring: Consistent follow-ups allow assessment of treatment response, early adjustment of medications, and timely intervention if new areas become affected, which is essential to preserve hair over time.
- Holistic management: Patient education, realistic expectation setting, and psychological support are often incorporated, recognising that FFA can impact appearance and emotional wellbeing.
Management of FFA is a long-term, highly individualised process. The focus is on stabilisation rather than regrowth, combining topical, systemic, and sometimes hormonal strategies with regular monitoring to protect as much hair as possible and maintain quality of life.
Lifestyle and Scalp Care

Although there is no cure for FFA, your main treatment goal is to slow or stop progression and protect the hair that remains. Early recognition and prompt intervention are essential, as hair follicles cannot recover once permanent damage has occurred. Your management plan is tailored to disease activity, affected areas, and your overall health.
Topical corticosteroids play a key role in reducing local inflammation and helping to preserve follicles. These are often combined with calcineurin inhibitors to provide additional anti-inflammatory control, particularly in sensitive areas such as the frontal hairline and eyebrows.
If your disease is more active or widespread, oral medications such as hydroxychloroquine may be considered. Anti-androgen therapies can also be useful in selected cases where hormonal factors appear to contribute to disease activity. These systemic treatments help control inflammation beyond the reach of topical therapies alone.
Distinguishing FFA from Pattern Hair Loss
FFA differs from female pattern hair loss in several important ways. With pattern hair loss, fine baby hairs along the frontal hairline are usually preserved. In FFA, these hairs are often lost completely, leaving a smooth, uniform edge.
Female pattern hair loss is non-scarring, meaning follicles remain intact and regrowth is often possible with treatment. FFA, by contrast, causes permanent follicle destruction due to inflammation, so hair cannot regrow once it is lost. This distinction has major implications for management and prognosis.
Accurate diagnosis is essential. Not all hairline recession is the same, and treating FFA as pattern hair loss can delay appropriate care. Specialist assessment ensures the condition is correctly identified and managed before further irreversible loss occurs.
When to Seek Specialist Advice
If you notice gradual hairline recession, thinning eyebrows, or unusual scalp sensations, it’s important to seek specialist evaluation. Early assessment can determine if inflammation is active and guide treatment.
You don’t need severe hair loss to justify a consultation. Often, subtle changes are the first signs of FFA, and catching them early offers the best chance to stabilise the condition.
Prompt specialist care helps protect your remaining hair. Starting treatment early can slow or halt progression, preserving follicles before irreversible loss occurs.
Delaying assessment reduces the effectiveness of therapy. Acting quickly gives you the greatest opportunity to maintain hair and manage cosmetic concerns over the long term.
Long-Term Outlook
The progression of FFA can vary widely from person to person. You may experience slow, limited recession over many years, or a more active phase that requires systemic treatment to bring inflammation under control.
With appropriate management, many patients achieve stabilisation. This means hair loss slows significantly or stops altogether. At this stage, the goal is no longer regrowth, but protecting the hair you still have.
Long-term care focuses on maintenance. Even when your hairline appears stable, ongoing treatment helps keep inflammation suppressed and reduces the risk of further follicle damage.
Regular monitoring remains essential. If flare-ups are detected early, treatment can be adjusted quickly. Achieving and maintaining stability is considered a positive and successful outcome in the management of FFA.
Research and Future Directions
The progression of FFA can differ greatly from person to person. Some women experience only slow, limited hairline recession, while others may have more active disease that requires systemic therapy to control inflammation.
With the right treatment, many patients reach stabilisation, where hair loss either stops or slows considerably. At this stage, the focus shifts from trying to regrow hair to protecting what remains.
Long-term management revolves around maintenance. Even when hair looks stable, ongoing care is needed to keep inflammation under control and safeguard the follicles that are still healthy.
Regular monitoring is crucial. Detecting flare-ups early allows your specialist to adjust treatment quickly, and achieving stability is considered a successful and reassuring outcome for long-term hair preservation.
FAQs:
1. What is frontal fibrosing alopecia (FFA)?
FFA is a type of scarring hair loss where inflammation permanently destroys hair follicles, primarily affecting the frontal hairline, temples, and eyebrows. Once follicles are damaged, regrowth is impossible.
2. Who is most at risk of developing FFA?
It predominantly affects women, especially post-menopause. Genetics, immune system activity, and environmental factors may also contribute.
3. How can I recognise early signs of FFA?
Look for subtle hairline recession, eyebrow thinning (starting at the outer third), and shiny or smooth scalp skin. Early changes may be easy to miss without photographs or specialist assessment.
4. Can FFA affect areas beyond the frontal scalp?
Yes. FFA can involve sideburns, facial hair, and sometimes hair on arms or legs, reflecting the systemic inflammatory nature of the condition.
5. How is FFA diagnosed?
A specialist performs a full scalp and skin examination. Early thinning in secondary areas, combined with clinical signs, allows for diagnosis and timely intervention.
6. What treatments are available for FFA?
Treatment focuses on slowing progression. Options include topical corticosteroids, calcineurin inhibitors, oral medications like hydroxychloroquine, and anti-androgen therapy in select cases.
7. Can lost hair grow back with treatment?
Regrowth is limited because FFA destroys follicles. Treatment aims to stabilise existing hair and prevent further loss rather than restore what is gone.
8. How important is specialist follow-up?
Extremely. Regular monitoring tracks disease activity, adjusts therapy, and helps intervene early if new areas become affected.
9. Are there lifestyle measures that help?
Gentle hair care, avoiding harsh chemicals, and managing overall scalp health can support treatment. Cosmetic options like microblading can improve confidence.
10. What is the long-term outlook for FFA?
With early recognition and consistent management, many patients achieve stabilisation. Ongoing monitoring ensures inflammation is controlled and hair follicles are protected.
Final Thoughts: Protecting Your Hairline with Early Action
Frontal fibrosing alopecia can feel distressing, especially when changes to your hairline or eyebrows seem subtle at first. Because FFA is a scarring condition, early recognition and prompt treatment are essential to preserve the hair you still have. The goal is not regrowth, but stabilisation protecting healthy follicles before irreversible loss occurs.
Consistent follow-up, personalised medical therapy, and gentle scalp care all play a key role in long-term management. Monitoring even small changes allows early intervention, which significantly improves the chances of maintaining your hairline and overall confidence.
If you’re considering Alopecia treatment in London, you can get in touch with us at the London Dermatology Centre to discuss tailored options for frontal fibrosing alopecia. Early specialist care provides clarity, reassurance, and the best opportunity to slow progression and protect your hair for the future.
References:
1. Kołcz, K., Krawczyk-Wołoszyn, K., Reich, A. and Żychowska, M., 2024. Pruritus in Lichen Planopilaris and Frontal Fibrosing Alopecia Clinical Characteristics and Dermoscopic Correlations. Journal of Clinical Medicine, 13(16), p.4898. https://www.mdpi.com/2077-0383/13/16/4898
2. Frontal Fibrosing Alopecia: An Observational Single-Center Study of 306 Cases. Life, 13(6), p.1344. https://www.mdpi.com/2075-1729/13/6/1344
3. Verma, S., Marak, A. and Paul, D., 2025. Frontal Fibrosing Alopecia: A Comprehensive Review with Recent Updates. Indian Journal of Dermatology, 70(2), pp.115–123. https://pubmed.ncbi.nlm.nih.gov/40162350/
4. Porriño-Bustamante, M.L., Fernández-Pugnaire, M.A. and Arias-Santiago, S., 2021. Frontal Fibrosing Alopecia: A Review. Journal of Clinical Medicine, 10(9), p.1805. https://pubmed.ncbi.nlm.nih.gov/33919069/
5. Frontal fibrosing alopecia. Clinics in Dermatology, 39(2), pp.183–193. Comprehensive review of FFA covering clinical presentation, histology, epidemiology and therapeutic considerations. https://www.sciencedirect.com/science/article/abs/pii/S0738081X20301863