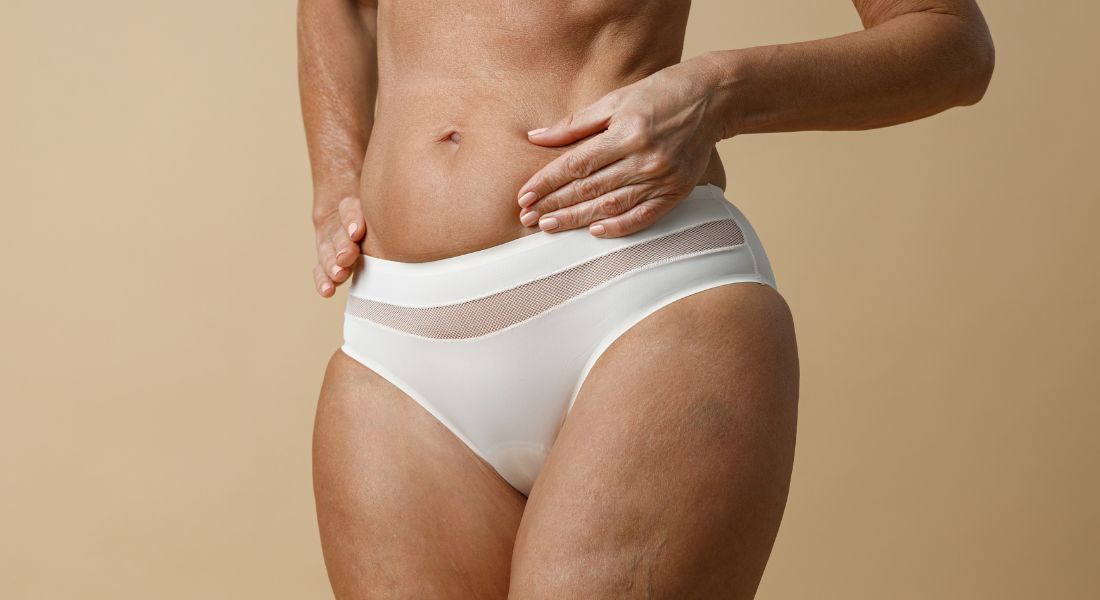
If you have been experiencing persistent itching, soreness, or whitening of the skin in the genital area and something just does not feel right, I want you to know this first: you are not imagining it. Ongoing discomfort in such an intimate area can feel confusing and isolating, especially when symptoms fluctuate. Your concerns are valid, and they deserve proper medical evaluation.
Lichen sclerosus is a chronic inflammatory skin condition that most commonly affects women, particularly the vulval region. In its early stages, it may present as mild itching, fragile skin, small white patches, or subtle changes in texture. Because these symptoms can resemble thrush, eczema or simple irritation, the condition is often overlooked at first.
Without appropriate treatment, the inflammation can lead to thinning of the skin, fissures, pain during intimacy, and progressive structural changes. Early diagnosis is important not only for symptom relief but also to reduce the risk of long-term complications. Prompt intervention makes management significantly more effective.
In this guide, I will explain how to recognise the early warning signs, how dermatologists confirm the diagnosis, and why ongoing monitoring matters. Most importantly, I want you to feel informed rather than frightened, because with the right care, this condition can be managed successfully.
What Is Lichen Sclerosus?
Lichen sclerosus is a long-term inflammatory skin disorder that primarily affects the vulval and perianal area in women. Although it can appear on other parts of the body such as the torso or upper limbs, the genital skin is by far the most commonfly involved site. It is not an infection, and it is not contagious.
The condition causes thinning, whitening and increased fragility of the affected skin. You may notice smooth white patches, delicate skin that tears easily, or persistent itching and soreness. Inflammation can fluctuate, with periods of relative calm followed by flare-ups.
Over time, if untreated, the chronic inflammation can lead to structural or architectural changes in the vulval area. This may include narrowing of the vaginal opening, fusion of surrounding skin, or scarring that affects comfort and intimacy. This is precisely why early recognition and timely treatment are so important.
Who Is Most Affected?
Lichen sclerosus can occur at any age. However, it is most commonly diagnosed in postmenopausal women and in prepubertal girls, suggesting that hormonal factors may play a role in susceptibility.
That said, many women in their thirties and forties are affected as well. It is not limited to one life stage, and being younger does not exclude the possibility of diagnosis.
Because the symptoms often overlap with more common conditions such as thrush, dermatitis or eczema, diagnosis is frequently delayed. If you have been repeatedly treated for infections that keep returning, or if symptoms never fully resolve despite medication, this is something important to consider and discuss with a specialist.
Early Signs You Should Not Ignore
Early symptoms of certain skin and hormonal conditions can be subtle and easy to overlook. You might dismiss them as temporary irritation or minor sensitivity. However, when symptoms persist, fluctuate, or gradually intensify, they deserve proper attention. Recognising these early warning signs allows for earlier diagnosis, simpler treatment, and better long-term outcomes.
1. Persistent Itching: Ongoing itching that feels constant rather than occasional is a key warning sign. If it becomes more noticeable at night, this pattern is particularly important. Chronic irritation should never be ignored.
2. Pale or White Skin Patches: Changes in skin colour, especially pale or white patches, can indicate underlying dermatological changes. These areas may look slightly different in texture or reflect light differently. Any unexplained pigment change warrants assessment.
3. Thinner or More Delicate Texture: If the skin begins to feel fragile, delicate, or thinner than usual, this may signal structural alteration. Increased sensitivity or easy irritation can accompany this change. Texture differences are often easier to feel than see at first.
4. Mild Discomfort with Intercourse or Urination: Subtle discomfort during intercourse or when passing urine should not be dismissed as normal. Even mild pain can indicate inflammation or tissue changes that require evaluation. Early treatment is typically more effective and less invasive.
Because these symptoms can fluctuate, it is easy to rationalise or delay seeking help. Please do not ignore persistent changes in sensation, colour, or comfort. Early consultation can prevent progression and significantly improve quality of life.
The Characteristic Whitening of the Skin
One of the hallmark signs of lichen sclerosus is whitening or depigmentation of the vulval skin. The affected area often loses its normal tone and takes on a pale, almost chalky appearance that stands out clearly from the surrounding tissue.
The skin can look shiny, smooth or porcelain-like, particularly under good lighting. In many women, the whitening forms a classic “figure-of-eight” pattern that extends around both the vulva and the anus. This pattern is highly characteristic and often helps clinicians recognise the condition.
You may also notice that the skin appears unusually fragile, almost tissue-paper thin. It can tear easily, especially during washing, wiping or intimacy, leading to small fissures or soreness. If you observe this type of visible change, even without severe pain, it is important to seek professional assessment rather than waiting for it to settle on its own.
Itching and Irritation
The itching associated with lichen sclerosus can be intense and deeply uncomfortable. It is not the fleeting, mild itch you might notice with simple dryness or irritation. Instead, it can feel persistent, intrusive and difficult to ignore.
For many women, the itch becomes worse at night, disrupting sleep and affecting overall wellbeing. The urge to scratch can be strong, even when you consciously try to avoid it.
Scratching, however, may lead to small tears or fissures in the already fragile skin. These fissures can be painful, sting during urination, and often heal slowly because the tissue is inflamed and delicate. Unfortunately, the resulting discomfort can trigger further scratching, creating an itch–scratch cycle that worsens inflammation and delays recovery.
Pain, Discomfort and Sexual Health
Lichen sclerosus can make intercourse painful, particularly when the skin is inflamed or fragile. This pain during sexual activity is medically known as dyspareunia, and it can range from mild discomfort to significant distress.
The thinning and tightening of the affected skin may cause small splits or fissures during intimacy. These tiny tears can sting, bleed lightly and take time to heal, which understandably creates anxiety around future sexual activity.
Over time, if inflammation remains uncontrolled, scarring can lead to narrowing of the vaginal opening. This structural change may make penetration increasingly difficult and can affect both physical comfort and emotional wellbeing. Addressing the condition early and maintaining appropriate treatment can help prevent these longer-term complications and protect sexual health.
Why Lichen Sclerosus Is Often Misdiagnosed
Because itching is such a common and non-specific symptom, lichen sclerosus is frequently mistaken for thrush. Many women are prescribed repeated courses of antifungal treatment, especially if there is redness or soreness, but these medications do not address the underlying inflammatory process.
While antifungals may temporarily soothe irritation, the core condition remains untreated. Eczema, psoriasis or contact dermatitis are also common alternative diagnoses, particularly in primary care settings where symptoms can overlap and early skin changes may be subtle.
If standard treatments are not resolving your symptoms, or if the problem keeps returning despite medication, further evaluation is essential. A careful clinical examination, and sometimes a biopsy, can clarify the diagnosis. You deserve a clear explanation and a treatment plan that genuinely improves your symptoms rather than masking them.
How Is Lichen Sclerosus Diagnosed?
Diagnosis is usually clinical. A dermatologist examines the skin carefully and looks for the characteristic whitening, thinning and structural changes that are typical of lichen sclerosus.
In many cases, the appearance alone is enough to make a confident diagnosis. If there is any uncertainty, a small skin biopsy may be recommended to confirm the findings and rule out other conditions.
A biopsy is a quick procedure performed under local anaesthetic and is generally well tolerated. It provides clarity, ensures the correct treatment is started, and offers reassurance if you have been struggling with persistent or unexplained symptoms.
Why Early Treatment Is Essential
Lichen sclerosus is not simply an intermittent itchy rash that settles on its own. It is a chronic inflammatory condition that can progressively alter delicate genital tissue if left untreated. Ongoing inflammation gradually damages skin architecture, leading to structural change rather than just surface irritation. Early recognition and consistent treatment are crucial to prevent long-term complications.
1. Risk of Permanent Scarring: Chronic inflammation can trigger fibrosis and scarring within the affected tissue. Over time, this may permanently alter normal anatomy. Once scarring forms, it is difficult to reverse.
2. Labial Shrinkage or Fusion: The labia may gradually shrink, thin, or fuse together. This structural change develops slowly but can significantly affect comfort and function. Preventative treatment helps maintain normal tissue architecture.
3. Burial of the Clitoral Hood: In advanced cases, scarring can cause the clitoral hood to become buried beneath fused tissue. This may lead to discomfort, reduced sensation, or hygiene difficulties. Early medical therapy dramatically reduces this risk.
4. Narrowing of the Vaginal Opening: Progressive tightening and narrowing can occur if inflammation remains uncontrolled. This may result in pain during intercourse and difficulty with examinations. Early intervention preserves elasticity and function.
These anatomical changes are not easily reversible once established. The goal of treatment is not only symptom relief but long-term preservation of structure and quality of life. Early, appropriate therapy significantly reduces progression and protects both comfort and function.
Long-Term Cancer Risk
There is another important reason why ongoing monitoring matters. Chronic lichen sclerosus carries a small but significant increased risk of developing Vulval squamous cell carcinoma compared with the general population.
Although this risk remains relatively low, it is higher than in women without the condition. The likelihood increases when inflammation is persistent and inadequately treated over many years.
Regular follow-up, careful self-monitoring and appropriate use of prescribed treatment significantly reduce this risk. When inflammation is well controlled and any new or unusual changes are assessed promptly, serious complications are far less likely to develop.
First-Line Treatment: Topical Corticosteroids
The cornerstone of treatment is high-potency topical corticosteroids. Although the name may sound intimidating, when these medications are used correctly under medical supervision, they are safe, targeted and highly effective at controlling inflammation.
They work by reducing immune-driven skin inflammation, relieving intense itching and helping to prevent long-term scarring or structural changes. Treatment typically begins with daily application for a prescribed period to bring symptoms under control, after which a structured maintenance schedule is introduced.
Consistency is critical for long-term stability. Stopping treatment too early or using it irregularly can allow inflammation to return, increasing the risk of flare-ups and progressive skin changes.
Are Steroids Safe for Long-Term Use?
This is a very common concern. Many patients worry about thinning of the skin or other side effects, but when topical corticosteroids are prescribed correctly and monitored by a dermatologist, long-term maintenance use is considered safe.
The treatment regimens used for lichen sclerosus are carefully structured, with controlled dosing and clear guidance on frequency. In reality, untreated chronic inflammation poses a far greater risk to the skin than appropriately supervised steroid therapy.
Regular follow-up appointments ensure the treatment remains effective, the skin stays healthy, and any adjustments can be made promptly if needed.
Additional Supportive Treatments
While topical corticosteroids remain the cornerstone of treatment, supportive care plays an equally important role in long-term management. The aim is to protect fragile skin, reduce friction, and maintain hydration. Gentle daily habits can significantly decrease irritation and flare frequency. These measures are simple but highly effective when used consistently.
1. Emollients for Hydration: Regular use of emollients helps maintain moisture and improve skin comfort. Well-hydrated skin is more resilient and less prone to cracking or irritation. They can be applied several times daily as needed.
2. Soap Substitutes: Standard cleansers can strip natural oils and worsen dryness. Soap substitutes are milder and protect the skin barrier while cleansing gently. This reduces unnecessary inflammation.
3. Barrier Creams: Barrier products provide a protective layer against moisture, friction, and external irritants. They are especially helpful in preventing discomfort during daily activities. Consistent use supports healing and comfort.
Avoiding perfumed or fragranced products is equally important, as these can trigger irritation. Gentle care reduces friction and helps maintain tissue integrity over time. When combined with medical therapy, supportive treatments significantly improve symptom control and long-term outcomes.
Managing Flare-Ups
Even with a consistent maintenance plan, flare-ups can still occur. Common triggers include stress, friction from tight clothing, infections, or hormonal fluctuations. Seasonal changes or certain personal care products can also irritate sensitive skin, so awareness of these factors is helpful.
If your symptoms suddenly worsen, it is important to contact your dermatologist promptly. Early adjustment of your treatment schedule, such as temporarily increasing corticosteroid application or adding soothing topical agents, can quickly bring inflammation back under control and prevent further skin changes.
Trying to self-manage without medical guidance is not recommended. Prompt professional review not only reduces discomfort and limits progression but also provides reassurance and ensures that long-term skin health and sexual wellbeing are preserved.
Living With a Chronic Condition
Lichen sclerosus is a chronic condition, meaning it requires ongoing management rather than a one-off treatment. Symptoms may fluctuate over time, so having a clear plan with your dermatologist is essential for long-term control.
Although this may sound overwhelming at first, once you establish a routine including regular use of prescribed topical treatments, gentle skincare, and monitoring for flare-ups it becomes much more manageable. Many women are able to achieve excellent symptom control and continue with their daily lives without significant disruption.
The key to successful management is a partnership with your healthcare provider. Regular follow-ups, open communication about changes or concerns, and adherence to treatment plans help maintain skin health, prevent complications, and preserve comfort, sexual wellbeing, and quality of life.
Emotional and Psychological Impact
Because lichen sclerosus affects intimate areas, it can feel isolating and sometimes overwhelming. Many women hesitate to discuss their symptoms, even with healthcare providers, which can lead to feelings of embarrassment, shame, or frustration.
It’s important to remember that lichen sclerosus is a medical condition, not a reflection of personal hygiene or behaviour. Experiencing discomfort, changes in appearance, or anxiety about intimacy is a normal response to a chronic skin condition affecting sensitive areas.
Seeking medical advice and support is an act of self-care, not weakness. Consulting a knowledgeable dermatologist, particularly one experienced in vulval conditions, can provide reassurance, effective treatment, and guidance on managing both physical symptoms and the emotional impact of the condition.
When Should You Seek Specialist Care?

You should arrange a specialist appointment if you notice persistent symptoms that do not respond to standard treatments. Key warning signs include ongoing itching despite antifungal therapy, the appearance of white or shiny skin patches, pain during intercourse, recurrent fissures or tearing, or any new lumps or persistent sores.
Early consultation with a dermatologist can prevent delays in diagnosis and reduce the risk of long-term complications, including scarring or structural changes. Prompt attention also helps control inflammation and maintain skin health.
For those based in the capital, booking with a trusted female dermatologist in London who specialises in vulval dermatology ensures sensitive, expert care. These specialists are experienced in both the physical and emotional aspects of the condition, providing reassurance and tailored treatment plans.
Can Lichen Sclerosus Be Cured?
Currently, there is no permanent cure for lichen sclerosus. It is a chronic condition that requires ongoing management rather than a one-time treatment.
That said, symptoms can be very effectively controlled. With appropriate therapy, itching often resolves completely, skin appearance improves, and progression or scarring can be halted.
Long-term follow-up with a dermatologist ensures that the condition remains stable, flare-ups are addressed promptly, and overall skin health is maintained. Consistent care allows most women to live comfortably and confidently despite the chronic nature of the disease.
Pregnancy and Lichen Sclerosus

If you are planning pregnancy, it is important to discuss your condition with your dermatologist in advance. Treatment plans can often be adjusted safely to minimise any risk to you or your baby.
Maintaining well-controlled disease during pregnancy is preferable to allowing inflammation to flare, as active symptoms can cause discomfort and complicate skin care.
Open communication with your healthcare team ensures both maternal comfort and safe management throughout pregnancy, allowing you to continue effective symptom control while addressing any pregnancy-specific considerations.
Monitoring and Self-Examination
Regular self-examination is a key part of managing lichen sclerosus, as it helps you identify any changes early. Pay attention to new ulcers, lumps, persistent patches, or areas that do not respond to your usual treatment.
In addition to self-monitoring, an annual review with a specialist dermatologist is often recommended. These check-ups allow for professional assessment of skin health, early detection of flare-ups, and adjustment of treatment if needed.
Monitoring is a protective measure, not something to fear. Being proactive empowers you to maintain long-term skin health, prevent complications, and ensure that any changes are addressed promptly and effectively.
The Importance of Education
Many women have never heard of lichen sclerosus until they are personally affected. This lack of awareness can lead to delays in seeking help, prolonged discomfort, and unnecessary misdiagnoses.
Raising awareness about the early signs such as persistent itching, whitening of the skin, or discomfort during intimacy helps women recognise symptoms sooner and seek timely medical care.
Knowledge empowers you to advocate for your own health. Understanding the condition, its management, and potential complications allows you to engage confidently with your dermatologist and make informed decisions about your long-term care.
FAQs:
1. What is lichen sclerosus?
Lichen sclerosus is a chronic inflammatory skin condition, most commonly affecting the vulval and perianal area in women. It causes thinning, whitening, fragility of the skin, and persistent itching or soreness. It is not contagious or infectious.
2. Who is most at risk of developing lichen sclerosus?
While it can occur at any age, lichen sclerosus is most frequently diagnosed in postmenopausal women and prepubertal girls. Women in their 30s and 40s can also be affected. Hormonal factors and autoimmune predisposition may contribute to susceptibility.
3. What are the early signs to watch for?
Early symptoms include persistent itching, small pale or white patches, delicate or thinning skin, and mild discomfort during intercourse or urination. Because these symptoms can fluctuate, early attention is crucial.
4. How is lichen sclerosus diagnosed?
Diagnosis is usually clinical, based on characteristic skin changes such as whitening, thinning, and textural alterations. If there is uncertainty, a small skin biopsy may be performed to confirm the diagnosis and exclude other conditions.
5. Why is early treatment important?
Early treatment helps prevent permanent scarring, labial shrinkage or fusion, narrowing of the vaginal opening, and other structural changes. Prompt therapy also reduces pain, itching, and sexual discomfort while preserving long-term skin health.
6. What is the main treatment for lichen sclerosus?
High-potency topical corticosteroids are the first-line treatment. When used correctly under medical supervision, they are safe, effectively control inflammation, relieve itching, and prevent progression.
7. Are steroids safe for long-term use?
Yes. When applied as prescribed with regular dermatological follow-up, maintenance use of topical corticosteroids is safe. The risk of complications from untreated chronic inflammation is far greater than potential side effects from supervised steroid therapy.
8. What supportive measures help manage lichen sclerosus?
Supportive care includes regular use of emollients, soap substitutes, and barrier creams to protect fragile skin. Avoiding perfumed products and friction reduces flare-ups and promotes healing.
9. Can lichen sclerosus flare up even with treatment?
Yes. Flare-ups can occur due to stress, friction, infections, hormonal changes, or certain personal care products. Early review and adjustment of treatment can quickly control symptoms and prevent progression.
10. Can lichen sclerosus be cured?
There is currently no permanent cure. However, symptoms can be effectively controlled with long-term therapy and monitoring. Most women achieve significant relief from itching, improved skin appearance, and protection against scarring.
Final Thoughts: Early Action Protects Long-Term Health
If you take one message away from this guide, let it be this: persistent vulval itching, whitening, or discomfort is never something you should ignore or repeatedly self-treat without improvement. Lichen sclerosus is a chronic condition, but with early diagnosis, appropriate treatment, and ongoing monitoring, it can be managed very effectively.
Prompt use of prescribed topical therapy helps control inflammation, prevent scarring, and significantly reduce the risk of long-term complications. Regular follow-up and self-awareness allow you to stay in control of your condition rather than feeling overwhelmed by it. Most importantly, you do not have to navigate this alone specialist support makes a meaningful difference.
If you are experiencing ongoing symptoms or would like expert assessment, consulting an experienced female dermatologist in London specialising in vulval skin conditions can provide reassurance, clarity, and a personalised treatment plan. If you’re considering female dermatologist in London, contact us at London Dermatology Centre to book a consultation with one of our specialists.
References:
- Gulin, S.J., Almlöf, O., Seifert, O., Kravvas, G., Lundin, F., Jungeström, M.B. and Söderman, J. (2025) ‘Genital lichen sclerosus the role of the vulvar microbiome’, Medicina https://www.mdpi.com/1648-9144/61/9/1632
- Beutler, K., Jankowska-Konsur, A. and Nowicka, D. (2025) ‘Regenerative approaches in vulvar lichen sclerosus: A systematic review’, International Journal of Molecular Sciences https://pubmed.ncbi.nlm.nih.gov/41009377/
- Smith, A. (2024) ‘Systematic review of outcome measures evaluating treatment efficacy and patient priorities in vulval lichen sclerosus’, Skin Health and Disease, https://academic.oup.com/skinhd/article/4/5/ski2.422/7896860
- Chi, C.C., Kirtschig, G., Balagula, Y., Dytoc, M., Guitart, J., Habif, T.P. and Korman, N.J. (2007) Lichen sclerosus: review of the literature and current recommendations for management, The Journal of Urology https://www.sciencedirect.com/science/article/abs/pii/S0022534707019957
- Gil-Villalba, A., Ayen-Rodriguez, A., Naranjo-Diaz, M.J. and Ruiz-Villaverde, R. (2023) ‘Laser therapy for vulvar lichen sclerosus: A systematic review’, Life https://pmc.ncbi.nlm.nih.gov/articles/PMC10672171/