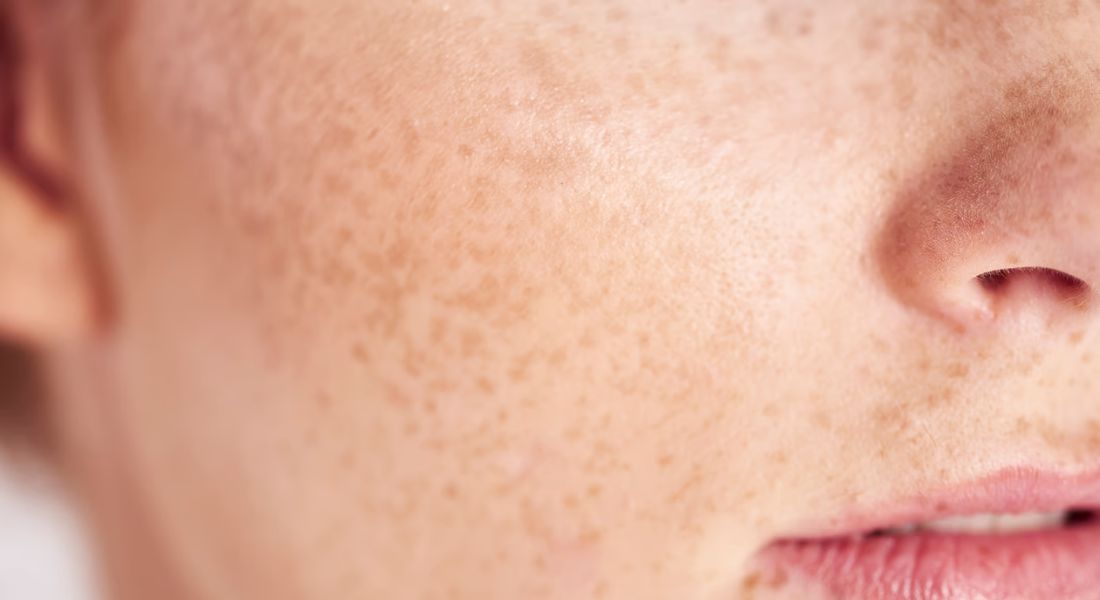
Melasma is a very common skin change during pregnancy, often showing up as dark patches on the cheeks, forehead, or upper lip. While it is easy to assume these patches will disappear soon after childbirth, that is not always the case. Many people find the pigmentation lingers far longer than expected, which can feel frustrating and leave you unsure whether to act or wait.
The reason melasma can persist is closely tied to hormonal changes. During pregnancy, elevated hormone levels stimulate pigment-producing cells, and even after delivery, these cells can remain active for weeks or months. This delayed response is why melasma does not simply vanish overnight, and why post-pregnancy pigmentation can feel stubborn despite your best efforts.
Knowing how long melasma may last and when to intervene is key to managing it effectively. Mild cases may gradually improve on their own, but persistent or worsening pigmentation often benefits from professional care. Understanding the typical timeline, the factors that prolong pigment activity, and the right time to start treatment helps you make informed choices for your skin’s recovery.
What Causes Melasma During Pregnancy
Melasma during pregnancy usually appears as dark patches on the cheeks, forehead, or upper lip. While it’s tempting to expect them to fade quickly after childbirth, many people find the pigmentation lingers for months, which can be frustrating and make it hard to decide whether to wait or act. Understanding why it happens is key to managing expectations and planning the right approach.
Hormonal changes are the main driver. Elevated oestrogen and progesterone stimulate melanocytes, the pigment-producing cells, and even after delivery these cells can stay active for weeks or months. Sun exposure, heat, and other triggers can keep pigmentation going, so persistence isn’t a sign of poor skincare it’s the skin responding to ongoing stimuli.
Timing your response matters. Mild melasma may fade gradually, but persistent patches often benefit from professional assessment. Acting at the right time, while your skin is stable, helps prevent pigment from settling deeper and makes treatments more effective, giving you a smoother, longer-lasting recovery.
How Long Melasma Typically Lasts After Pregnancy
For some new mothers, melasma begins to fade naturally within a few months after childbirth. As hormone levels gradually stabilise, melanocyte activity slows, allowing pigmentation to lighten on its own. In milder cases, this natural fading often occurs over three to six months.
However, not every timeline is this predictable. In many instances, pigmentation can persist for a year or more, especially if triggers like sun exposure or ongoing hormonal influences, such as breastfeeding, remain active. These factors continue to stimulate melanocytes, which slows the skin’s natural recovery.
When melasma lasts beyond twelve months, it is generally classed as long-standing. At this stage, spontaneous fading is less likely, and professional treatment often provides the most reliable path to noticeable improvement. Early assessment and tailored interventions help restore a more even skin tone and prevent pigmentation from becoming deeper or more resistant.
Why Melasma Sometimes Persists
For some people, melasma starts to fade naturally within a few months after childbirth. As hormone levels stabilise, melanocyte activity decreases, allowing pigmentation to gradually lighten. In mild cases, this process typically takes around three to six months.
Not everyone experiences such straightforward improvement, though. Pigmentation can persist for a year or more, particularly if ongoing triggers like sun exposure or hormonal effects from breastfeeding remain active. These factors keep melanocytes stimulated, slowing the skin’s natural recovery and prolonging the appearance of melasma.
When melasma continues beyond twelve months, it is usually considered persistent. At this point, spontaneous fading becomes unlikely, and professional interventions such as targeted topical treatments or gentle procedures are often needed to restore a more even skin tone and reduce stubborn pigmentation.
The Role of Sun Exposure in Prolonging Melasma

Sun exposure is one of the biggest factors that can keep melasma active after pregnancy. Ultraviolet rays directly stimulate melanocytes, causing existing patches to darken even with brief, everyday exposure. Post-pregnancy skin is often more sensitive, making consistent sun protection essential to prevent pigmentation from lingering or worsening.
Even small lapses in daily protection allow melanocytes to reactivate, which can stabilise melasma at a higher intensity and slow down natural fading. Casual or intermittent exposure undermines other preventive measures, meaning your skincare and treatments may struggle to show results if sun defence is inconsistent.
Using a broad-spectrum sunscreen every day, paired with physical protection like hats, creates a strong barrier against further stimulation. By reducing additional triggers, you give your skin the best chance to gradually recover, helping melasma fade more effectively and keeping pigment from becoming entrenched.
Hormonal Influences After Pregnancy
You might expect your skin to settle quickly after pregnancy, but hormonal changes can continue to influence melasma for months. Even as hormone levels begin to decline, your body takes time to fully rebalance, and during this period, pigment-producing cells can remain overactive. This means that melasma may persist even if you’re following a good skincare routine, as internal hormonal signals are still playing a role.
- Hormones take time to stabilise: Your body doesn’t return to its pre-pregnancy state immediately, and these ongoing fluctuations can keep melasma visible for longer.
- Breastfeeding can extend hormonal changes: If you’re breastfeeding, certain hormones remain elevated, which may continue to stimulate pigment production.
- Melanocytes are highly sensitive to hormones: Even small hormonal shifts can trigger these cells to produce more pigment, making melasma slower to fade.
- Hormonal contraceptives may affect pigmentation: Starting some forms of contraception can cause melasma to persist or become more noticeable in certain individuals.
- Results can be gradual and uneven: You might notice slow or inconsistent improvement, as hormonal influence can delay visible changes in your skin.
- Patience is essential during recovery: Allowing time for your hormones to stabilise, while maintaining a consistent routine, gives your skin the best chance to improve.
When you understand how ongoing hormonal changes affect your skin, it becomes easier to manage expectations and stay consistent with your care. Over time, as your body gradually rebalances, you’re more likely to see steady improvement in your melasma.
Skin Type and Genetic Factors
Your skin type plays a major role in how melasma develops and how long it persists. Medium to darker skin tones often have more active melanocytes, which can make pigmentation more stubborn. This doesn’t mean improvement is impossible, but it usually requires patience, consistent protection, and a carefully structured routine.
Genetics further influence how your skin responds to hormonal shifts and environmental triggers. If melasma runs in your family, you may be naturally more prone to prolonged or recurrent pigmentation. Understanding this predisposition helps explain why some cases take longer to fade and why certain triggers affect your skin more than others.
Being aware of both your skin type and genetic tendencies allows you to manage expectations realistically. It also guides your choice of treatments and preventive measures, ensuring they are tailored to your individual needs. A personalised approach significantly improves the likelihood of long-term control and prevents frustration from unrealistic assumptions about speed or results.
When Melasma Becomes Persistent

Melasma is generally considered persistent when it shows little to no improvement after about a year. By this stage, the pigment has stabilised, and natural fading without intervention becomes unlikely. What was once a gradual change now becomes a more fixed condition, demanding a deliberate approach.
Persistent melasma often extends into deeper pigment layers, which makes it resistant to basic skincare alone. Targeted treatments whether topical therapies, chemical peels, or other professional interventions are usually required to achieve noticeable improvement. Early recognition can help prevent the pigmentation from settling even deeper, making future management easier.
Acting promptly when melasma becomes persistent is crucial. Delaying professional guidance can make treatments less effective and slow progress, so timely assessment ensures a more strategic approach. With the right interventions, even long-standing melasma can be controlled, restoring a more even and manageable skin tone.
When Should You Consider Treatment
Melasma is generally considered persistent when it shows little or no improvement after a year. By this stage, the pigment has stabilised, and natural fading without intervention becomes unlikely, shifting the condition from gradual change to a more fixed state.
Persistent melasma often extends into deeper layers of the skin, which makes it less responsive to basic skincare alone. Visible improvement usually requires targeted treatments, and early assessment can help prevent the pigmentation from becoming even more entrenched.
Recognising when melasma has become persistent allows you to act at the right time. Waiting too long can make treatment more challenging and slow progress, so timely professional guidance is crucial for effectively managing long-standing pigmentation.
Treatment Options for Post-Pregnancy Melasma
Once it’s appropriate to start treatment, there are several options to consider. Topical therapies like hydroquinone, retinoids, and azelaic acid are commonly used to reduce pigment production and gradually lighten dark patches over time. These work best when applied consistently and under guidance to avoid irritation.
In some cases, procedures such as chemical peels or laser treatments may be appropriate. These target deeper pigmentation and can improve overall skin tone more effectively, but they must be performed carefully to prevent inflammation or worsening of melasma.
Choosing the right approach depends on your skin type and how deeply the pigment has settled. A personalised plan ensures that treatments are both safe and effective, giving you the best chance of achieving noticeable improvement without compromising skin health.
Why Immediate Treatment Is Not Always Advised
You might feel eager to start treating melasma straight after pregnancy, but beginning too soon isn’t always the best approach for your skin. During this time, your skin can still be sensitive and influenced by ongoing hormonal changes, which may make it more reactive to active ingredients or procedures. Acting too quickly can sometimes lead to irritation or inconsistent results, making it more beneficial to take a gradual and cautious approach.
- Your skin may still be sensitive after pregnancy: Hormonal shifts can leave your skin more reactive than usual, increasing the risk of irritation if strong treatments are introduced too early.
- Ongoing hormonal changes can affect results: Even if you start treatment, fluctuating hormones may continue to trigger pigmentation, limiting how effective those treatments can be.
- Breastfeeding requires extra caution: If you are breastfeeding, certain ingredients or procedures may not be suitable, so delaying treatment helps ensure safety for both you and your baby.
- Early treatment can sometimes worsen irritation: Starting active products too soon may disrupt your skin barrier, which can make melasma appear more pronounced rather than improving it.
- A gradual approach supports better outcomes: Giving your skin time to stabilise allows treatments to work more effectively when they are eventually introduced.
- Professional guidance can help with timing: Consulting a specialist ensures you begin treatment at the right stage, reducing risks and improving long-term results.
By allowing your skin time to recover naturally before starting targeted treatments, you create a more stable foundation for improvement. Once your skin has settled, you’re far more likely to see safer, smoother, and more consistent results from any treatment you choose.
The Importance of Gentle Skincare

Gentle skincare is crucial when managing melasma after pregnancy. Harsh products can inflame the skin and actually worsen pigmentation, so protecting your skin barrier is a top priority. Supporting recovery this way also improves how well treatments perform.
Mild cleansers and hydrating moisturisers help maintain balance, while avoiding aggressive exfoliation prevents unnecessary inflammation that can trigger more pigment production. Often, keeping your routine simple is far more effective than layering multiple strong products.
Consistency is what makes a difference. By supporting your skin every day, you create the environment it needs to improve gradually, making treatments more effective and reducing the risk of flare-ups over time.
Can Melasma Return in Future Pregnancies
Melasma can reappear in future pregnancies because hormonal changes may reactivate pigment cells, causing new or darker patches. This is particularly common if you’ve experienced melasma before, as your skin has already shown sensitivity to these fluctuations.
Preventative steps can help limit the severity of recurrence. Daily sun protection, early skincare adjustments, and careful management of triggers all play a role in keeping pigmentation under control. Being proactive often makes a noticeable difference in how pronounced melasma becomes.
A return of melasma doesn’t mean previous treatments failed it simply reflects your skin’s underlying hormonal responsiveness. Understanding this helps set realistic expectations and guides how you approach prevention and care in future pregnancies.
Emotional Impact of Persistent Melasma
Persistent melasma can take a real emotional toll, even though it poses no medical risk. Seeing changes in your skin can affect your confidence and how you feel about yourself day to day, making it a very valid concern.
Remembering that melasma is common and treatable can bring reassurance. There are numerous effective options to improve its appearance, and you are far from alone in managing this condition.
Getting professional advice can make a big difference. Understanding what to expect, how long it may last, and which treatments are suitable helps reduce uncertainty and gives you a greater sense of control over your skin.
Long-Term Management and Expectations
Melasma is often a long-term condition that needs ongoing management. While you can achieve noticeable improvement, maintenance is usually necessary to prevent recurrence, including daily sun protection and occasional treatments.
The aim is to control pigmentation rather than eliminate it entirely. With the right approach, your skin tone can become more even and manageable, and having realistic expectations helps you feel satisfied with progress.
Consistency is what makes lasting results possible. Small, steady actions over time add up, creating meaningful improvements that keep your melasma under control in the long run.
FAQs:
1. How long does melasma usually last after pregnancy?
Melasma can start fading naturally within three to six months, but in some cases, pigmentation can persist for a year or longer, particularly if triggers like sun exposure or breastfeeding continue to stimulate pigment cells.
2. Why doesn’t melasma disappear immediately after childbirth?
Even after delivery, hormone levels remain elevated for some time, keeping melanocytes active. Sun exposure, heat, and other environmental triggers can also prolong pigmentation.
3. When should I consider professional treatment for post-pregnancy melasma?
If melasma persists beyond twelve months, or if pigmentation worsens, professional treatments like topical therapies or gentle procedures are usually recommended for noticeable improvement.
4. Can sun exposure make melasma worse after pregnancy?
Yes. UV rays stimulate melanocytes directly, darkening existing patches. Daily broad-spectrum sunscreen and physical protection like hats are essential to prevent further pigmentation.
5. Does breastfeeding affect melasma?
Breastfeeding prolongs elevated hormone levels, which can continue to stimulate pigment cells and delay natural fading, making melasma more persistent.
6. Can melasma return in future pregnancies?
Yes. Hormonal fluctuations in subsequent pregnancies can reactivate pigment cells, leading to new or darker patches, especially in people who have had melasma before.
7. How does skin type affect melasma duration?
Medium to darker skin tones often have more active melanocytes, which can make pigmentation more stubborn. Genetics also play a role in how your skin responds to hormones and environmental triggers.
8. Is it safe to start treatment immediately after pregnancy?
Not always. Your skin may still be sensitive due to hormonal shifts, and some active ingredients or procedures could cause irritation. A gradual, professional-guided approach is safer and more effective.
9. What treatments are effective for post-pregnancy melasma?
Topical therapies (hydroquinone, azelaic acid, retinoids) and professional procedures (chemical peels, lasers) are commonly used. Personalised plans based on skin type and pigment depth are essential for safety and results.
10. How can I prevent melasma from worsening or recurring?
Daily sun protection, gentle skincare, avoiding harsh products, and early intervention with triggers can help control pigmentation. Consistency over time is key to maintaining results.
Final Thoughts: Regaining Control Over Post-Pregnancy Melasma
Persistent melasma after pregnancy can feel frustrating, but understanding the timelines, triggers, and hormonal influences helps you approach it strategically rather than reactively. Patience and consistency are your allies rushing treatments too soon or neglecting sun protection often prolongs pigmentation instead of reducing it. By recognising the signs of persistent melasma, you can act at the right time with interventions that truly make a difference.
Long-term management is about control, not perfection. Gentle skincare, regular sun protection, and gradual treatment create the foundation for sustainable improvement. Even if pigmentation recurs in future pregnancies, early planning and proactive measures can keep it manageable and prevent it from becoming entrenched.
Professional guidance ensures treatments are both safe and effective, tailored to your skin type and the depth of pigmentation. If you’re considering melasma treatment in London, contact us at London Dermatology Centre to book a consultation with one of our specialists. Taking deliberate steps now sets the stage for lasting results and renewed confidence in your skin.
References:
- Zhao, L., Fu, X. & Cheng, H., 2024. Prevention of melasma during pregnancy: risk factors and photoprotection‑focused strategies. Clinical, Cosmetic and Investigational Dermatology, 17, pp.2301–2310. Emphasises prevalence during pregnancy, persistence after delivery, hormone triggers and the role of photoprotection. https://pubmed.ncbi.nlm.nih.gov/39430643/
- Parać, E., 2024. Unmasking Melasma: confronting the treatment challenges. Cosmetics (Basel), 11(4), p.143. Comprehensive review covering melasma pathogenesis, hormonal influences, UV/visible light triggers, and long‑term management strategies. https://www.mdpi.com/2079-9284/11/4/143
- Maddaleno, A.S., 2021. Melanogenesis and Melasma Treatment. Cosmetics (Basel), 8(3), p.82. Reviews mechanisms of melanin production, hormonal and environmental triggers including pregnancy‑related factors. https://www.mdpi.com/2079-9284/8/3/82
- Handel, A.C. et al., 2014. Melasma: a clinical and epidemiological review. Anais Brasileiros de Dermatologia, online. Discusses epidemiology, pathophysiology, and persistence of melasma, noting that pregnancy‑associated melasma may spontaneously disappear within about a year in some cases but can persist. https://pmc.ncbi.nlm.nih.gov/articles/PMC4155956/
- Kumar, D., 2025. Melasma management: unveiling recent breakthroughs in understanding pathophysiology and treatment. ScienceDirect Reviews in Dermatological Science (online). Summarises pathogenesis (including hormone and light exposure impacts) and challenges in long‑term management of melasma. https://www.sciencedirect.com/science/article/pii/S2772632025000054