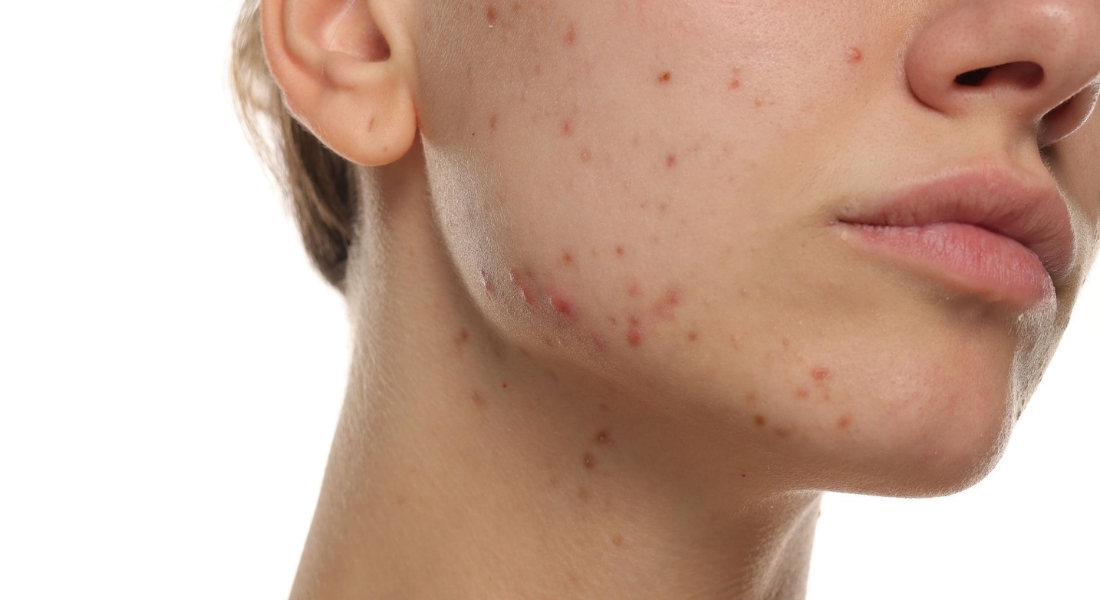
Excess facial hair, medically known as hirsutism, is one of the most common and emotionally challenging skin-related symptoms of PCOS. If you have noticed thicker, darker hair developing on your chin, upper lip, jawline, chest or abdomen, it is usually linked to elevated androgen levels. These hormones stimulate certain hair follicles, causing fine vellus hairs to transform into coarser, more visible terminal hairs.
In PCOS, the body becomes more sensitive to androgens, or produces them in higher amounts than normal. This hormonal shift directly affects hair growth cycles, making hair grow thicker and sometimes faster in androgen-sensitive areas. At the same time, you may notice thinning of scalp hair, as hormonal imbalance can impact different follicles in different ways.
Unlike typical body hair growth, PCOS-related hirsutism tends to persist without medical intervention. Temporary methods such as shaving, waxing or threading can manage appearance, but they do not influence the hormonal driver behind the growth. This is why the hair often returns consistently and may feel progressively more noticeable.
The key thing I want you to understand is that this is a physiological response, not something you have caused. With appropriate treatment, including hormonal regulation, anti-androgen medications, and professional laser or light-based hair reduction, excessive hair growth can be significantly reduced and controlled safely over time.
What Is PCOS and Why Does It Affect Your Skin?
Polycystic Ovary Syndrome (PCOS) is a hormonal condition that affects how your ovaries function and regulate ovulation. It is characterised by an imbalance in reproductive hormones, particularly androgens. Although androgens are often described as “male hormones,” they are naturally present in women in small amounts, but in PCOS their levels may be elevated or the body may be more sensitive to them.
When androgen levels rise beyond what your body needs, they stimulate oil glands, hair follicles and pigment-producing cells in the skin. This increased hormonal activity can lead to excess oil production, persistent acne, thicker facial or body hair, and areas of darkened pigmentation. These changes are not random; they are direct responses to internal hormonal signals.
Because the root cause is hormonal, treating the skin alone often brings only temporary improvement. If you have been relying solely on topical products, it can feel like an ongoing battle. Addressing the underlying hormonal imbalance alongside targeted skin treatment is usually the key to achieving more consistent, long-term results.
How Hormones Influence Your Skin
Let me explain what is happening beneath the surface. Your sebaceous glands naturally produce oil, known as sebum, to protect and lubricate the skin. When androgen levels rise, they stimulate these glands to produce more sebum than necessary. Excess oil mixes with dead skin cells, leading to blocked pores and creating the perfect environment for inflammation and acne to develop.
At the same time, androgens act on hair follicles in hormonally sensitive areas such as the chin, upper lip, chest and abdomen. This stimulation can cause fine hairs to become thicker and darker. In some individuals, these hormones also influence melanocytes, the pigment-producing cells, contributing to areas of darkened or uneven skin tone.
When acne, excess hair growth and pigmentation appear together, it is often not a coincidence. Rather than being three separate skin conditions, they frequently represent one underlying hormonal pattern expressing itself in different ways on the skin.
PCOS Acne: How It Differs from Typical Adult Acne
This is one of the most important distinctions you need to understand if you are struggling with persistent breakouts. Acne linked to Polycystic Ovary Syndrome (PCOS) behaves differently from standard adult acne. It follows a hormonal pattern, often feels deeper and more painful, and tends to resist conventional topical treatments. Recognising these differences can help you seek the right evaluation and avoid years of frustration.
1. Lower Face Distribution: PCOS-related acne commonly appears along the jawline, chin, and neck. This hormonal pattern is distinct from teenage acne, which often affects the forehead and cheeks. If your breakouts consistently cluster around the lower face, hormones may be playing a central role.
2. Deep, Painful Cysts: The lesions are often inflamed, deep, and tender rather than small surface whiteheads. These cystic breakouts can linger for weeks and carry a higher risk of scarring. Their depth reflects stronger androgen influence on sebaceous glands.
3. Hormonal Flare Pattern: Breakouts frequently worsen in line with menstrual cycle fluctuations. Unlike acne triggered mainly by skincare or diet, PCOS acne tends to follow internal hormonal rhythms. This cyclical pattern is an important diagnostic clue.
4. Resistance to Standard Topicals: Many patients report trying multiple creams with only temporary or minimal improvement. While topical treatments may reduce surface inflammation, they do not address the underlying hormonal imbalance driving the condition.
5. Persistence Into Adulthood: Unlike teenage acne, which is typically linked to puberty-related hormonal surges, PCOS acne often continues into your twenties, thirties, or even forties. Persistent severe cystic acne in adulthood warrants consideration of a hormonal cause.
If you are experiencing ongoing, deep breakouts that follow a hormonal pattern, it may not be “just adult acne.” Understanding the distinction allows for more targeted treatment approaches that address the root cause rather than repeatedly managing symptoms. Recognising this difference is often the first step toward long-term control and clearer skin.
Excess Hair Growth (Hirsutism)
One of the most distressing symptoms of PCOS for many women is unwanted facial or body hair. You may begin to notice coarse, dark hairs appearing on your chin, upper lip, sideburn area or neck. Some women also experience increased hair growth on the chest, abdomen or inner thighs. This male-pattern distribution of hair growth is medically known as hirsutism.
Hirsutism is directly linked to elevated androgen levels or increased sensitivity of hair follicles to these hormones. Androgens stimulate certain follicles to transform fine, soft hairs into thicker, darker terminal hairs. Unlike normal body hair, this growth pattern tends to persist and may gradually become more noticeable without appropriate hormonal management.
The emotional impact of hirsutism can be profound. Many women feel embarrassed, self-conscious or exhausted by the need for frequent hair removal. It is important to remember that this is a physiological hormonal response, not a reflection of femininity, personal hygiene or self-care.
Pigmentation Changes and PCOS
Another common but often overlooked sign of PCOS is pigmentation change. You may notice darkened, slightly thickened or velvety patches of skin developing on the neck, underarms or groin. This condition is known as acanthosis nigricans, and it is frequently associated with underlying metabolic changes rather than being purely cosmetic.
Acanthosis nigricans is strongly linked to insulin resistance, which commonly accompanies PCOS. Insulin resistance means your body does not respond efficiently to insulin, so higher levels circulate in the bloodstream. Elevated insulin can stimulate skin cell proliferation and increase pigment production, leading to visible darkening in certain areas.
In addition, you may experience post-inflammatory hyperpigmentation after acne lesions heal. Because PCOS-related acne tends to be deeper and more inflammatory, it is more likely to leave behind lingering dark marks. As a result, pigmentation changes in PCOS can arise both from hormonal-metabolic imbalance and from the after-effects of persistent acne.
Hair Thinning on the Scalp
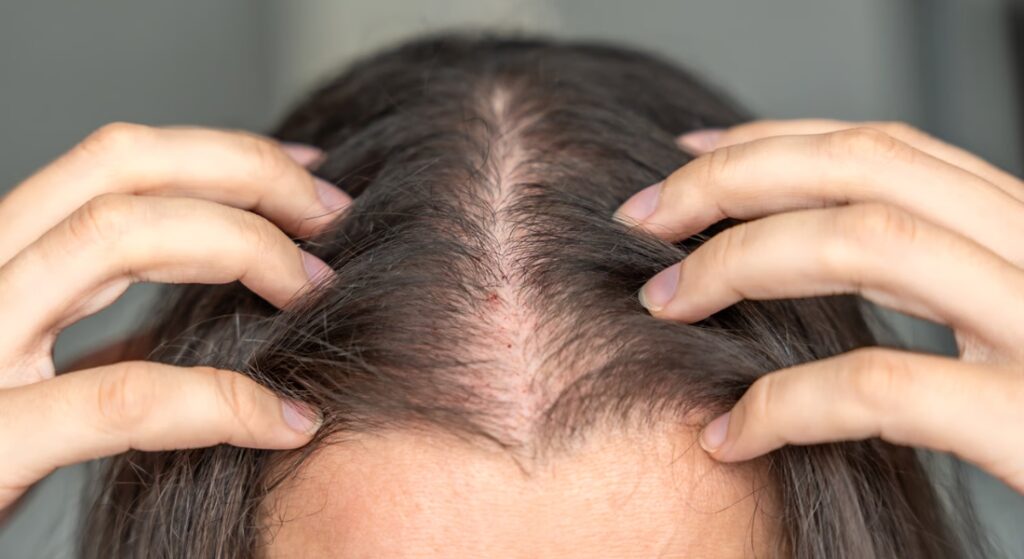
While excess hair may grow in unwanted areas, you might simultaneously notice thinning on your scalp. This pattern is known as androgenic alopecia and is influenced by the same hormonal imbalance seen in PCOS. Rather than general shedding, it usually presents as gradual thinning over time.
You may observe widening of your central parting or reduced density at the crown. In some cases, the overall hair volume feels noticeably lighter, especially when styling or tying your hair back. Androgens can cause susceptible hair follicles on the scalp to shrink, producing finer, shorter hairs before eventually reducing growth altogether.
The contradiction can feel particularly upsetting. More hair where you do not want it, and less hair where you do. Understanding that both changes stem from the same hormonal mechanism can help you see that this is a medical pattern, not random hair behaviour.
Why Topical Treatments Alone Often Fail
If your acne keeps returning despite using over-the-counter products or prescription creams, there is usually a reason. Topical treatments are designed to reduce surface inflammation, control bacteria and unclog pores. While they can improve symptoms, they do not address the hormonal imbalance driving excess oil production in PCOS.
Because the underlying androgen influence remains active, improvement may only be partial or temporary. You might notice that your skin clears for a while, only for deep, painful breakouts to return, particularly around the jawline or lower face. Repeatedly switching products can become frustrating when the root cause has not been corrected.
If this pattern sounds familiar, a hormonal evaluation is worth considering. Managing PCOS-related skin concerns often requires a combined dermatological and medical approach, targeting both the skin itself and the internal hormonal drivers responsible for the flare-ups.
How Dermatologists Diagnose PCOS-Related Skin Conditions
When you see a specialist, they do not simply assess the visible acne or pigmentation. A thorough consultation usually includes questions about your menstrual cycle, recent weight changes, hair growth patterns and family history. This broader discussion helps identify whether your skin symptoms may be part of an underlying hormonal condition rather than isolated dermatological concerns.
Blood tests are often arranged to measure androgen levels and assess markers of insulin resistance. In some cases, a pelvic ultrasound may be recommended to evaluate the ovaries for features consistent with PCOS. Diagnosis is typically based on a combination of clinical history, examination findings and investigation results, rather than a single test alone.
If you are considering specialist support, consulting a female dermatologist in London with experience in hormonal skin disorders can be particularly helpful. Practitioners who regularly manage PCOS-related concerns are often highly attuned to both the physical changes and the psychological impact on women. Early diagnosis allows for a more strategic, coordinated and effective treatment plan tailored to your individual needs.
Treatment Pathways for PCOS Skin Symptoms
Let us talk about what can actually help. When it comes to PCOS-related skin symptoms, there is no single universal solution that works for everyone. Your treatment plan depends on your individual hormone levels, the severity of your acne, hair changes or pigmentation, and your overall metabolic health.
Dermatologists usually take a combined approach rather than relying on one intervention alone. This may involve targeted topical treatments for acne, prescription oral medications to regulate androgens, and therapies that address insulin resistance where appropriate. Lifestyle support, including weight management and dietary guidance, may also form part of the strategy if insulin imbalance is contributing to symptoms.
The key is personalisation. Effective management focuses on controlling hormonal drivers while simultaneously improving visible skin concerns. When treatment is tailored to your specific pattern of symptoms, outcomes are typically more stable and sustainable over the long term.
1. Hormonal Regulation
Combined oral contraceptive pills are often prescribed to help regulate menstrual cycles and reduce androgen production. By lowering circulating and free androgen levels, they can decrease sebaceous gland activity, which in turn reduces excess oil production. Over time, this can lead to gradual improvement in acne severity and may also slow unwanted hair growth.
In certain cases, anti-androgen medications such as spironolactone may be recommended. These medications work by blocking androgen receptors in the skin and hair follicles, limiting the hormonal stimulation that drives breakouts and hirsutism. They are typically used under careful medical supervision, particularly in women of reproductive age.
It is important to understand that results are not immediate. Because hair growth cycles and sebaceous gland activity change gradually, it often takes several months before noticeable improvement becomes visible. Patience and consistent follow-up are essential parts of successful hormonal management.
2. Acne-Specific Dermatological Treatments
When managing PCOS-related acne, treatment often requires a layered approach. While hormonal therapy addresses the underlying trigger, dermatological treatments help control inflammation, reduce lesions, and protect against scarring. These medications are selected based on acne severity, skin sensitivity, and long-term goals. Combining systemic and topical strategies typically produces the most stable results.
1. Topical Retinoids: Retinoids help normalise skin cell turnover and prevent clogged pores. They also improve post-acne pigmentation and refine overall texture. Consistent use is key, as results build gradually over several weeks.
2. Benzoyl Peroxide Combinations: Benzoyl peroxide reduces acne-causing bacteria and inflammation. It is often combined with topical antibiotics to minimise bacterial resistance. This approach helps control active breakouts while other treatments address the root cause.
3. Oral Antibiotics (Short-Term Use): For moderate to severe inflammatory acne, short courses of oral antibiotics may be prescribed. These reduce inflammation and bacterial load quickly. However, they are not a long-term solution and should be used strategically.
4. Oral Isotretinoin (In Selected Cases): Isotretinoin may be considered for severe, scarring, or treatment-resistant acne. It significantly reduces sebaceous gland activity and can lead to long-term remission. Careful monitoring is essential due to potential side effects.
It is important to understand that while these treatments can dramatically improve acne, they do not correct the hormonal imbalance driving PCOS. If androgens remain elevated, breakouts may recur after treatment stops. For lasting control, dermatological therapy and hormonal management must work together rather than in isolation.
3. Managing Excess Hair
There are both medical and procedural options available for managing excess hair associated with PCOS. Hormonal therapies, such as combined oral contraceptives or anti-androgen medications, may help slow the development of new terminal hairs over time. These treatments target the underlying hormonal drive rather than removing hair that is already present.
For existing unwanted hair, laser hair removal can significantly reduce density and thickness by targeting pigment within the hair follicle. Multiple sessions are usually required because hair grows in cycles, and maintenance treatments may be needed to sustain results. Electrolysis is another option and works by permanently destroying individual hair follicles, making it suitable for smaller or more stubborn areas.
Results vary from person to person depending on hormone levels, hair colour, skin type and consistency of treatment. Improvement is often gradual rather than immediate. Patience, realistic expectations and ongoing hormonal management are key to achieving the best long-term outcome.
4. Treating Pigmentation
For acanthosis nigricans, improving insulin sensitivity is often the most important step. Lifestyle changes such as weight management, balanced nutrition and regular physical activity can significantly improve skin texture and pigmentation over time. In some cases, medication prescribed to address insulin resistance may further support visible improvement.
Topical lightening agents such as azelaic acid or hydroquinone may be used under medical supervision to gradually reduce darkened areas. These treatments work by slowing excess melanin production and encouraging a more even skin tone. Consistent use and careful monitoring are important to avoid irritation or uneven results.
Procedures such as chemical peels and selected laser treatments can also assist with post-inflammatory hyperpigmentation, particularly after acne. However, while these options improve surface pigmentation, treating the underlying hormonal and metabolic imbalance remains crucial for long-term stability and prevention of recurrence.
The Role of Lifestyle in PCOS Skin Management

You might be wondering how much lifestyle truly influences PCOS-related skin changes. The honest answer is: quite a lot. While medication and dermatological treatments play a crucial role, daily habits can significantly affect insulin levels, androgen activity, and overall hormonal balance. Small, consistent changes often create meaningful improvements over time.
1. Weight Management (If Relevant to You): In individuals with insulin resistance, weight reduction can improve metabolic function and lower circulating androgens. Even modest weight loss has been shown to improve acne and other PCOS symptoms in some women. However, this is highly individual and not universally required.
2. Balanced Nutrition: Diets that support stable blood sugar levels may help reduce insulin spikes that stimulate androgen production. Emphasising whole foods, fibre, and protein while limiting refined sugars can support hormonal stability. Consistency matters more than extreme restriction.
3. Regular Exercise: Physical activity improves insulin sensitivity and supports endocrine health. It also reduces stress, which can indirectly influence hormonal fluctuations. Sustainable routines are more beneficial than short bursts of intensity.
4. Adequate Sleep and Stress Control: Poor sleep and chronic stress can worsen hormonal imbalance. Prioritising restorative sleep and stress management supports overall endocrine regulation. This can indirectly reduce flare frequency and severity.
It is important to remember that PCOS affects women of all body types. Weight alone is not the sole cause, and thin women can experience significant hormonal imbalance as well. Lifestyle is a supportive pillar, not a cure, and it works best alongside medical management tailored to your specific hormonal profile.
Emotional Impact and Self-Confidence
I want to address something that often goes unspoken. Skin changes linked to PCOS can have a profound emotional impact, even if others cannot fully see what you are going through. Acne, pigmentation and excess hair are not simply cosmetic concerns; they can influence how you feel about your appearance every single day.
You may find yourself avoiding social events, cancelling plans or feeling uncomfortable leaving the house without make-up. The constant need for hair removal or covering pigmentation can become exhausting and frustrating. Over time, this can chip away at your self-confidence in ways that are difficult to explain to others.
These feelings are completely valid. PCOS is not just a hormonal condition; it affects how you see yourself and how you move through the world. Seeking professional support, whether dermatological to manage physical symptoms or psychological to address emotional wellbeing, is a sign of strength and self-care, not weakness.
Why Early Intervention Matters
The longer hormonal acne persists, the greater the risk of permanent scarring. Deep, inflamed cystic lesions can damage the underlying skin structure and leave lasting marks that are far more difficult to treat than active breakouts. Addressing inflammation early significantly reduces the likelihood of long-term textural changes.
Similarly, untreated insulin resistance does not just affect the skin. Over time, it can contribute to broader metabolic complications, including weight gain and an increased risk of type 2 diabetes. When PCOS-related hormonal imbalance is left unmanaged, both dermatological and systemic consequences may gradually develop.
Early diagnosis allows you to protect not only your skin but also your overall health. If you suspect your acne, pigmentation or excess hair may be hormonally driven, seeking medical advice sooner rather than later can make a meaningful difference in long-term outcomes.
Can PCOS Skin Symptoms Be Fully Cured?
This is one of the most common questions. PCOS itself is a chronic condition, which means there is currently no definitive cure for the underlying hormonal imbalance. It requires long-term management rather than a one-time treatment.
However, symptoms can be managed extremely effectively. With the right combination of hormonal therapy, dermatological treatments and sustainable lifestyle adjustments, many women achieve clear skin and a significant reduction in unwanted hair and pigmentation.
The key is consistency and proper medical guidance. Treatments take time to show results, and regular follow-up ensures adjustments can be made when needed. While PCOS may not be cured, its skin symptoms can often be controlled to a level that no longer disrupts daily life or confidence.
When Should You See a Specialist?
Knowing when to escalate from over-the-counter treatments to specialist care is crucial in PCOS-related skin concerns. Persistent, hormonally patterned symptoms rarely resolve with surface-level solutions alone. Early evaluation can shorten the diagnostic journey and prevent long-term scarring or frustration. If multiple signs are present together, a more comprehensive hormonal assessment is often warranted.
1. Severe, Cystic or Persistent Acne: Deep, painful cysts that linger for weeks or leave marks behind should not be ignored. If your acne continues despite appropriate skincare, it may signal an internal hormonal driver. Early intervention reduces the risk of permanent scarring.
2. Irregular Periods with Skin Symptoms: When acne is accompanied by irregular or absent periods, this combination strongly suggests hormonal imbalance. Skin and menstrual changes together are important diagnostic clues. A specialist can coordinate dermatological and endocrine evaluation.
3. Excess Facial Hair Growth: Increased hair along the chin, jawline, chest, or abdomen may indicate elevated androgens. When combined with acne, this pattern strengthens suspicion of PCOS. Hormonal testing may be appropriate.
4. Darkened Skin Patches in Body Folds: Areas of darker, velvety skin often around the neck, underarms, or groin can signal insulin resistance. This finding, alongside acne and cycle irregularity, warrants medical assessment.
5. Repeated Failure of Over-the-Counter Treatments: If multiple topical products provide only temporary or minimal improvement, the root cause may not be superficial. Continuing to switch creams without investigation can delay effective care.
If you live in or near the capital, consulting a female dermatologist in London who understands hormonal acne patterns can help streamline both diagnosis and treatment. Integrated care addressing hormones, skin, and metabolic factors together often produces more stable and lasting results. Early specialist input can prevent years of reactive management and move you toward a structured, effective plan.
Realistic Expectations

I always encourage realistic timelines when managing PCOS-related skin concerns. Hormonal treatments typically take three to six months before visible improvement becomes noticeable, as your body needs time to respond to changes in androgen levels. Expecting instant results can lead to unnecessary frustration.
Laser hair removal also requires multiple sessions spaced several weeks apart to effectively target hair in different growth cycles. Similarly, pigmentation fading is usually gradual, particularly when linked to hormonal or metabolic imbalance. Consistency matters far more than speed.
Quick fixes rarely produce sustainable results. Patience, adherence to your prescribed plan and regular follow-up appointments are vital to achieving long-term improvement and preventing recurrence.
FAQs:
1. How does PCOS affect the skin?
PCOS increases androgen levels or makes your body more sensitive to them. These hormones stimulate oil glands, hair follicles and pigment cells, leading to acne, excess facial hair, scalp thinning and pigmentation changes.
2. Why does PCOS cause acne on the jawline and chin?
Hormonal acne linked to PCOS typically appears along the lower face, especially the jawline, chin and neck. These areas are more sensitive to androgen stimulation, which increases oil production and inflammation.
3. How is PCOS acne different from regular adult acne?
PCOS acne tends to be deeper, more cystic and more persistent. It often follows a menstrual pattern and does not respond fully to topical treatments alone because the root cause is hormonal.
4. Can skincare alone clear PCOS acne?
Skincare can improve inflammation and reduce clogged pores, but it does not correct hormonal imbalance. Without addressing androgen levels, acne may continue to recur.
5. What is hirsutism?
Hirsutism is excessive hair growth in areas such as the chin, upper lip, chest or abdomen. In PCOS, it occurs because elevated androgens stimulate hair follicles to produce thicker, darker hairs.
6. Will shaving or waxing make PCOS hair worse?
No. Hair removal methods do not change the thickness or growth rate at a hormonal level. However, they do not treat the underlying cause, so hair will continue to regrow.
7. Can laser hair removal help with PCOS-related hair growth?
Yes. Laser hair removal can significantly reduce hair thickness and density. However, maintenance sessions may be required because ongoing hormonal influence can stimulate new growth over time.
8. Why do I have dark patches on my neck or underarms?
Darkened, velvety patches may be acanthosis nigricans, which is linked to insulin resistance. Elevated insulin levels stimulate skin cell growth and pigmentation.
9. Does PCOS cause hair thinning on the scalp?
Yes. Elevated androgens can shrink scalp hair follicles over time, leading to gradual thinning, particularly along the central parting or crown.
10. Can PCOS skin symptoms be cured permanently?
PCOS is a chronic condition, so there is no permanent cure. However, skin symptoms can often be controlled very effectively with long-term management.
Final Thoughts: Managing PCOS Skin Symptoms Effectively
Navigating skin changes caused by PCOS can feel overwhelming, but understanding the hormonal roots of acne, excess hair, and pigmentation is the first step toward meaningful improvement. While topical products alone may offer temporary relief, lasting results come from a combination of targeted dermatological treatments, hormonal regulation, and lifestyle adjustments. Patience and consistency are essential, as improvement often takes several months and requires ongoing care.
Equally important is addressing the emotional impact of PCOS-related skin changes. Persistent acne, hirsutism, or pigmentation can affect self-confidence and daily life, so seeking professional support is not just about appearance it’s about overall wellbeing. Early intervention can prevent scarring, reduce long-term complications, and provide a structured approach to managing symptoms.
If you’re considering a female dermatologist in London, contact us at London Dermatology Centre to book a consultation with one of our specialists. With personalised care that addresses both the hormonal drivers and visible skin changes, you can achieve clearer skin and greater confidence over time.
References:
- Archer, J.S. and Chang, R.J. (2004) ‘Hirsutism and acne in polycystic ovary syndrome’, Best Practice & Research Clinical Obstetrics & Gynaecology, https://pubmed.ncbi.nlm.nih.gov/15380144/
- Polycystic ovary syndrome: A review for dermatologists: Part I. Diagnosis and manifestations (2015) Journal of the American Academy of Dermatology, https://www.sciencedirect.com/science/article/abs/pii/S0190962214014340
- Farhan, M., Seyfi, A., Alnuaimi, A., et al. (2025) A narrative review on cutaneous manifestations in polycystic ovary syndrome: pathophysiology, diagnosis, management, and psychosocial impact, Annals of Medicine and Surgery https://pmc.ncbi.nlm.nih.gov/articles/PMC12055046/
- Daniele, S., Chelucci, E., Scarfò, G. and Artini, P.G. (2023) ‘Molecular research on polycystic ovary syndrome (PCOS) https://www.mdpi.com/2227-9059/11/5/1358
- Purwar, A. and Nagpure, S. (2022) ‘Insulin resistance in polycystic ovarian syndrome’, Cureus, https://pubmed.ncbi.nlm.nih.gov/36407241/