Basal cell carcinoma (BCC) is often described as a pale, pearly bump, but it doesn’t always present that way. Some BCCs can be darker, pigmented, or even mimic the appearance of a mole, which makes recognising them more challenging.
Pigmented BCC occurs when melanin is present within the tumour cells, giving the lesion a brown, black, or blue-black hue. This can easily be confused with benign spots or other pigmented lesions, increasing the risk of delayed detection.
Knowing that BCC can vary in colour is crucial for early identification. Any dark or changing lesion, especially on sun-exposed areas, should be assessed by a professional to rule out malignancy and ensure timely treatment.
What Is Basal Cell Carcinoma?
Basal cell carcinoma (BCC) is the most common type of skin cancer, arising from basal cells in the lower layer of the epidermis. These cells are responsible for generating new skin cells to replace those that naturally shed, but mutations often triggered by UV damage can cause them to grow uncontrollably.
BCC usually grows slowly and rarely spreads to other parts of the body, but it can invade surrounding tissue and cause significant local damage if left untreated. Early detection makes treatment more straightforward and reduces the risk of scarring or disfigurement, which is why regular skin checks are so important.
Cumulative sun exposure is the main risk factor, explaining why BCC often appears on the face, neck, and hands. Fair-skinned individuals, frequent sunbathers, and those with a history of sunburn are particularly vulnerable. Protecting your skin with sunscreen, clothing, and shade, along with monitoring for any new or changing lesions, remains the most effective strategy for prevention and early management.
The Classic Appearance of BCC
The classic presentation of basal cell carcinoma is typically a pearly or translucent bump, sometimes with small blood vessels visible on the surface. This distinctive look makes it easier to identify in many cases.
Some lesions may develop an ulcer or a small sore that refuses to heal, while others appear as slightly raised, shiny patches. These textbook features are well documented and often guide early detection.
Yet, not all BCCs conform to this standard appearance. Variants can look very different, which is why relying solely on the “classic” description can be misleading. Being aware of these differences is crucial for recognising atypical cases.
Can Basal Cell Carcinoma Be Pigmented?
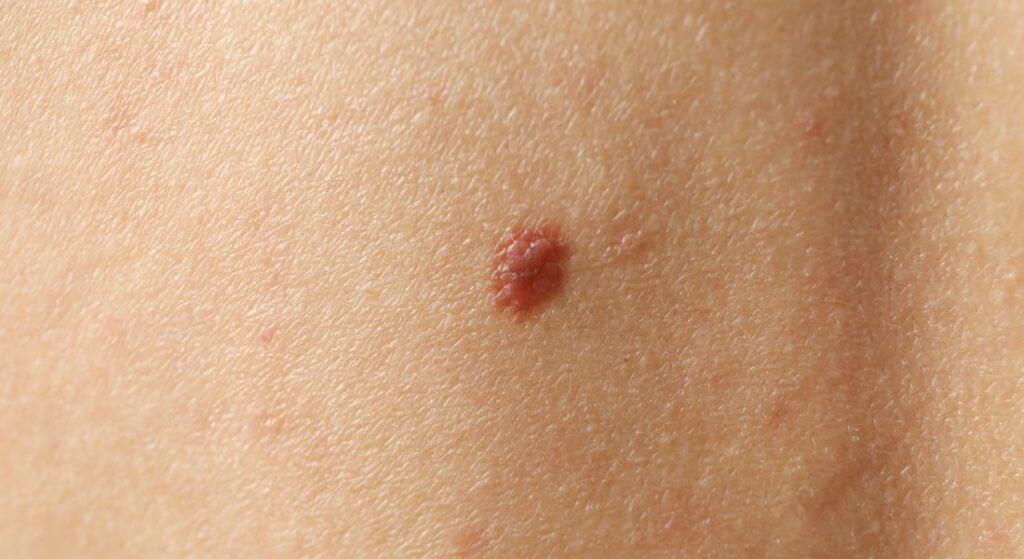
Yes, basal cell carcinoma can indeed be pigmented, a form known as pigmented BCC. These lesions contain increased melanin, which gives them a brown, blue, or even black appearance, making them visually distinct from the classic pearly bump.
While pigmented BCC is more commonly seen in individuals with darker skin types, it can develop in anyone. The presence of pigment does not change the underlying diagnosis or behaviour of the cancer, but it can make recognition more challenging, especially for those unfamiliar with atypical presentations.
The darker colour often leads to confusion with other skin lesions. It can be mistaken for harmless moles, freckles, or even more serious conditions like melanoma. Because of this, professional evaluation is crucial. Dermatologists may use tools like dermoscopy or biopsy to ensure an accurate diagnosis, preventing delays in treatment and reducing the risk of complications. Pigmented BCC reinforces the importance of not assuming every dark spot is harmless and seeking timely expert assessment.
Why Does Some BCC Appear Dark?
When some basal cell carcinomas (BCC) appear darker, it can understandably cause confusion, as they may resemble harmless moles or other pigmented lesions. The colour change is linked to how pigment is produced within the affected area, rather than indicating a completely different condition. Understanding why this happens can help you look beyond colour alone when assessing any changes in your skin.
- Melanin Within the Tumour: In pigmented BCC, the darker appearance comes from melanin, the natural pigment that gives your skin its colour. Tumour cells can stimulate nearby pigment-producing cells, leading to visible darkening within the lesion.
- Variation in Colour Intensity: Not all pigmented BCCs look the same. Some may appear light brown, while others can be much darker, depending on how much melanin is present and how actively it is being produced in that area.
- Uneven Pigment Distribution: The pigment within these lesions is often irregular, meaning you might notice patches of darker and lighter areas. This unevenness can make the lesion look more complex and harder to interpret visually.
- Can Mimic Other Skin Conditions: Because of their colour, pigmented BCCs can sometimes resemble benign moles or even other types of skin lesions. This overlap is one reason why visual appearance alone isn’t always reliable for identification.
- Structure and Behaviour Matter Too: While colour is one clue, it’s important to also consider changes in size, shape, texture, or bleeding. These characteristics often provide more meaningful insight than pigmentation alone when evaluating a suspicious area.
Recognising that darker colour doesn’t always mean a harmless lesion is key. If you notice any new, changing, or unusual marks on your skin, it’s always best to have them assessed professionally, as early evaluation leads to more accurate diagnosis and effective management.Top of Form
How Pigmented BCC Can Be Mistaken for Other Conditions
Pigmented basal cell carcinoma can be tricky because it often looks very similar to benign moles. Its dark colour and well-defined edges may fool the eye, and it can also resemble seborrhoeic keratosis, a harmless, waxy skin growth. These similarities can lead to delays in recognising the true nature of the lesion.
Even more concerning is that pigmented BCC can mimic melanoma, which is a far more aggressive form of skin cancer. Melanoma often requires urgent treatment, so confusing the two could have serious consequences. Early and accurate differentiation is therefore essential for safe and effective care.
Relying on visual assessment alone is not enough. Dermatologists use specialised tools, such as dermoscopy, to examine the structure and pigment patterns in detail. In some cases, a biopsy may be needed to confirm the diagnosis, ensuring that the right treatment is provided promptly and reducing the risk of complications.
Differences Between Pigmented BCC and Melanoma
Although pigmented basal cell carcinoma and melanoma can look alike, there are some key differences. BCC often presents with a smoother surface and sometimes a subtle pearly border, whereas melanoma usually has irregular, jagged edges and multiple colours within the same lesion. These visual cues can help guide suspicion, but they are not definitive.
Melanoma also tends to change more quickly over time. It may become asymmetrical, darken in certain areas, or develop multiple shades, while pigmented BCC generally grows slowly and maintains a more uniform appearance. Monitoring the rate of change can provide important clues for differentiation.
Despite these distinctions, the differences are often subtle and can be missed without professional expertise. Any lesion that looks unusual, changes over time, or raises concern should be assessed by a dermatologist. Early evaluation is critical to ensure accurate diagnosis and timely treatment for either condition.
Other Types of BCC That May Look Different
Basal cell carcinoma isn’t one-size-fits-all; there are multiple subtypes with distinct appearances. Nodular BCC often forms the classic pearly bump, while superficial BCC presents as a flat, red, scaly patch that can easily be mistaken for eczema or dermatitis. Morphoeic BCC, on the other hand, can mimic a scar, appearing pale and with ill-defined edges.
These variations mean that relying on a single textbook description can be misleading. Even experienced clinicians must look closely and consider multiple features before reaching a diagnosis. Misidentifying a subtype can delay treatment, so awareness of the diversity is important.
Recognising that BCC can present in so many ways reinforces the need for professional assessment. Any unusual spot whether raised, flat, pigmented, or scar-like deserves a thorough examination. Early detection remains the most reliable way to ensure effective treatment and minimise local tissue damage.
Common Locations for Pigmented BCC
Pigmented BCC most frequently shows up on sun-exposed areas, with the face being a common site particularly the nose, cheeks, and around the eyes. The scalp, ears, and neck are also vulnerable, especially in individuals with thinning hair or frequent outdoor exposure. Sunlight is the main trigger for these changes.
That said, pigmented BCC can occasionally appear in less obvious places, including the trunk or limbs. While these sites are less typical, they demonstrate that no part of the skin is completely immune. Awareness of your entire skin surface is important for early detection.
Relying on location alone can be misleading. Even lesions in unusual spots may be clinically significant. Regular self-checks combined with professional skin examinations remain the safest approach.
Who Is at Risk of Developing Pigmented BCC?
When it comes to pigmented basal cell carcinoma (BCC), risk isn’t limited to one specific group you might be more susceptible depending on a combination of factors rather than a single cause. While some people are naturally at higher risk, anyone can develop it, which is why staying aware of changes in your skin is so important.
- Fair Skin and Sun Sensitivity: If you have fair skin, light eyes, or burn easily in the sun, your skin has less natural protection against UV radiation. This makes you more vulnerable to damage that can eventually lead to skin cancers, including pigmented BCC.
- History of Sunburn or UV Exposure: Frequent sun exposure, especially episodes of severe sunburn, significantly increases your risk over time. UV damage builds up gradually, meaning even past exposure can contribute to future skin changes.
- Age and Cumulative Damage: As you get older, the effects of long-term sun exposure become more apparent. Pigmented BCC is more commonly diagnosed in adults because the damage that contributes to it develops slowly over many years.
- Darker Skin Tones and Visibility: While BCC is often associated with lighter skin, pigmented forms can be more noticeable in individuals with darker complexions due to increased melanin. However, this doesn’t mean the condition is exclusive to any particular skin tone.
- Multiple Contributing Factors: Your overall risk is shaped by a mix of genetics, environment, and lifestyle. Factors such as outdoor occupations, tanning habits, and even your geographical location can all play a role in how likely you are to develop it.
Understanding your personal level of risk helps you stay proactive rather than reactive. By keeping an eye on your skin and seeking advice if anything changes, you give yourself the best chance of catching issues early, when they are most manageable and treatable.
Signs That Should Prompt Medical Assessment
Changes in size, shape, or colour are the most common red flags for pigmented lesions. Rapid growth, uneven pigmentation, or the development of multiple colours within a single spot warrants prompt attention. Any lesion that bleeds, crusts, or fails to heal within a few weeks should never be ignored.
The “ugly duckling” principle is particularly useful for spotting concerning lesions. If one mole or spot looks different from the rest of your skin, it may indicate an underlying problem. Personal awareness and intuition often catch issues that routine observation might miss.
Early consultation with a dermatologist ensures accurate diagnosis and swift action. Timely assessment not only reduces the risk of serious complications but also allows for simpler, more effective treatment. Acting promptly is always safer than waiting.
How Dermatologists Diagnose Pigmented BCC
Dermoscopy gives dermatologists a detailed view of the lesion’s pigment patterns and vascular structures. This helps distinguish pigmented BCC from benign moles or more serious cancers like melanoma. Visual clues alone are often insufficient, making this tool invaluable.
When uncertainty remains, a biopsy provides definitive confirmation. A small tissue sample is examined under a microscope to identify cancerous cells. This step eliminates guesswork and ensures treatment is targeted correctly.
Accurate diagnosis sets the stage for effective management. It determines the most appropriate treatment method, whether surgical or non-surgical, and reduces the risk of recurrence. Professional evaluation is key to safe, reliable outcomes.
Treatment Options for Pigmented BCC
Surgical excision is the first-line treatment for most pigmented BCCs. The goal is complete removal with clear margins to prevent recurrence. In delicate or cosmetically sensitive areas, Mohs micrographic surgery is often preferred because it allows precise, layer-by-layer removal while preserving healthy tissue.
Topical treatments such as imiquimod or 5-fluorouracil are used for superficial BCCs. Cryotherapy or laser therapy can be considered in carefully selected cases, particularly for small or low-risk lesions. Each approach requires careful assessment to ensure the treatment matches the lesion’s depth and subtype.
Timing and early detection are critical. Lesions identified promptly usually require simpler procedures and heal faster with better cosmetic outcomes. Delayed treatment increases the likelihood of more extensive surgery, longer recovery, and higher risk of complications.
Prognosis and Long-Term Outlook
If you catch basal cell carcinoma early, you’re already putting yourself in a strong position. Most cases don’t spread beyond the skin, so prompt action usually keeps things straightforward. The real risk comes if you let it linger recurrence is far more common than unexpected spread.
You need to stay on top of follow-ups after treatment. Regular check-ups aren’t just formalities; they’re how you spot any returning or new lesions before they become a bigger problem. Skipping these appointments is where people often lose the advantage early treatment gives them.
Long-term, you can expect very good outcomes if you manage it properly. Taking action quickly and staying vigilant makes a huge difference. The key takeaway for you is simple: awareness and consistency in care are your best defence.
Preventing Basal Cell Carcinoma
You can make a real difference in lowering your risk of basal cell carcinoma by being consistent with sun protection. Sunscreen isn’t optional it’s essential every day, even when it’s cloudy. Pair it with hats, long sleeves, and avoiding the midday sun, and you’re stacking the odds in your favour.
Checking your skin regularly should become second nature. You’re the first line of defence, so learn what’s normal for you and notice any new or changing spots. Professional skin reviews complement what you spot yourself, and together they catch problems early, when treatment is simplest.
The best approach is to make prevention part of your routine. Little habits, like reapplying sunscreen or choosing shade, add up over months and years. Protecting your skin now saves you from more complex interventions later it’s an investment in your long-term health.
Why Early Diagnosis Matters

When it comes to skin conditions like basal cell carcinoma, timing can make a significant difference to both your health and the outcome of treatment. Acting early means problems are addressed while they are still small and manageable, helping you avoid more complex procedures later on. By paying attention to changes in your skin and seeking advice promptly, you give yourself the best chance of a straightforward and effective solution.
- Simpler, Less Invasive Treatment: When lesions are identified early, they are usually smaller and more contained. This often means they can be treated with less invasive methods, reducing the need for complex surgical procedures and making the overall experience much more manageable.
- Lower Risk of Scarring and Complications: Early treatment typically involves smaller areas of skin, which helps minimise visible scarring and lowers the risk of complications. This is especially important for areas like the face, where cosmetic outcomes matter just as much as medical ones.
- Prevents Deeper Tissue Involvement: If diagnosis is delayed, the lesion may grow and extend into deeper layers of the skin. This can make treatment more challenging and may require more extensive removal to ensure all affected tissue is addressed.
- Avoids More Complex Procedures: Larger or more advanced lesions often need more involved treatments, which can mean longer recovery times and more noticeable after-effects. Early action helps you avoid unnecessary complexity and disruption.
- Encourages Awareness and Prompt Action: Recognising unusual or changing lesions, including pigmented ones, allows you to act quickly. This awareness plays a key role in ensuring you receive timely care before the condition progresses.
Taking early signs seriously can make all the difference in how easily a condition is managed. By staying vigilant and seeking professional advice when something doesn’t look right, you protect not only your health but also the long-term appearance of your skin.
How Pigmented BCC Appears Under Dermoscopy
When you have a pigmented spot checked, the dermatologist will usually bring out a dermatoscope. This tool lets them see below the surface, revealing structures you simply can’t spot with the naked eye. Those hidden patterns are crucial for telling pigmented basal cell carcinoma apart from other dark marks on your skin.
You’ll notice that pigmented BCC has some pretty distinctive features under dermoscopy. Blue-grey ovoid nests, leaf-like structures these aren’t random; they’re diagnostic markers that guide your doctor. They stand in stark contrast to the messy, irregular pigment networks you see in melanoma, making the difference clear once you know what to look for.
This is why getting a professional evaluation matters so much. What seems like a harmless dark spot could have very telling structures underneath. Dermoscopy gives you a much higher accuracy, reducing the risk of missing a BCC or confusing it with something more serious.
Why Self-Diagnosis Can Be Misleading
It’s tempting to look up images online and try to match your spot, but you have to be careful. Pigmented basal cell carcinoma can vary hugely from one person to the next, so what you see on a screen rarely tells the full story.
Factors like lighting, your natural skin tone, and even the stage of the lesion can completely alter its appearance. A spot that seems harmless at home might actually be more concerning under a dermatologist’s eye. That variability alone makes self-diagnosis risky.
If you rely only on how a lesion looks, you could end up delaying proper treatment. The safest move is to get it checked professionally. Early evaluation not only gives clarity but also peace of mind, letting you act before the situation becomes more complex.
Growth Pattern of Pigmented BCC
Pigmented basal cell carcinoma usually grows at a slow, steady pace. You might notice a spot gradually getting bigger or a little darker over months. It rarely changes overnight, which can make it easy to underestimate.
That slow growth doesn’t mean you can ignore it. Left unchecked, it can start to affect surrounding tissue, and that damage is most concerning in sensitive areas like your face. Even a small lesion can create bigger problems if it’s allowed to progress.
Keeping an eye on changes over time is key. Take note of any evolution in size, colour, or texture, and get it assessed if you see progression. Regular monitoring is what catches subtle shifts before they escalate.
FAQs:
1. Can basal cell carcinoma really appear dark or black?
Yes, some BCCs are pigmented due to melanin in tumour cells. They can range from light brown to deep black, which can make them look like moles or even melanoma.
2. Does pigmentation make BCC more dangerous?
No, the presence of pigment doesn’t increase the cancer’s aggressiveness. However, it can delay diagnosis if mistaken for a benign spot, which is why early professional assessment is crucial.
3. Who is most at risk of pigmented BCC?
Fair-skinned individuals, those with a history of sunburn, chronic UV exposure, or older adults are more susceptible. Pigmented forms are also more noticeable in darker skin tones, but anyone can develop them.
4. How do pigmented BCCs differ from melanoma?
Pigmented BCCs often grow slowly, have smoother surfaces, and sometimes subtle pearly borders. Melanoma usually has jagged edges, multiple colours, and faster changes over weeks or months.
5. Can pigmented BCC be mistaken for a harmless mole?
Absolutely. Dark BCC can mimic moles, freckles, or seborrhoeic keratosis. Relying on colour alone is risky; structural changes like ulceration, bleeding, or slow growth are key warning signs.
6. What should prompt me to see a dermatologist?
Any new, changing, or unusual dark spot, especially one that bleeds, crusts, grows, or doesn’t heal in a few weeks. The “ugly duckling” principle spots that look different from your other marks is a reliable guide.
7. How do dermatologists confirm pigmented BCC?
They use dermoscopy to examine pigment patterns and blood vessel structures. If uncertain, a biopsy provides definitive confirmation by identifying cancerous cells under a microscope.
8. What are the treatment options?
Surgical excision is standard; Mohs surgery is preferred in cosmetically sensitive areas. Superficial BCCs may be treated with topical creams, cryotherapy, or laser in selected cases.
9. Can pigmented BCC recur?
Yes, recurrence is possible, particularly if margins weren’t fully clear or follow-up is inconsistent. Regular post-treatment checks are essential to catch new or returning lesions early.
10. How can I prevent pigmented BCC?
Consistent sun protection daily sunscreen, protective clothing, and avoiding peak UV hours is key. Regular self-exams and professional skin reviews maximise early detection and treatment success.
Final Thought: Staying Ahead of Pigmented Basal Cell Carcinoma
Pigmented basal cell carcinoma can be deceptive, often masquerading as harmless moles or freckles. Early recognition, consistent self-monitoring, and professional evaluation are the pillars of effective management. Paying attention to changes in size, colour, texture, or healing patterns allows you to act before more invasive treatments are required.
Combining daily skin vigilance with expert assessment ensures that you catch lesions early, when treatment is simpler and outcomes are better. While sun protection and routine checks form the first line of defence, timely consultation with a dermatologist provides clarity, precision, and reassurance. If you’re considering basal cell carcinoma treatment in London, you can get in touch with us at London Dermatology Centre to explore tailored strategies and secure professional guidance for long-term skin health.
References:
1. Mazur, E., Kwiatkowska, D. & Reich, A., 2023. Photodynamic Therapy in Pigmented Basal Cell Carcinoma A Review. Biomedicines. https://www.mdpi.com/2227-9059/11/11/3099
2. Halip, I.A., Tomescu, R., Vlădăreanu, A.M. & Ciurea, R.L., 2022. Assessment of Basal Cell Carcinoma Using Dermoscopy. Diagnostics, 12(3), p.735. Summarises how dermoscopy aids classification and early detection of BCC, including pigmented variants. https://www.mdpi.com/2075-4418/12/3/735
3. Deepadarshan, K., Mallikarjun, M. & Abdu, N.N., 2013. Pigmented basal cell carcinoma: a clinical variant, report of two cases. Journal of Clinical and Diagnostic Research. https://pubmed.ncbi.nlm.nih.gov/24551712/
4. Wang, W.-E., Chen, Y.-T., Wang, C.-H., et al., 2024. Dermoscopic features of pigmented basal cell carcinoma according to size. International Journal of Dermatology. https://pubmed.ncbi.nlm.nih.gov/38288856/
5. Rudolph, H. & Rudolph, R.I., 1992. Pigmented basal cell carcinoma: investigation of 70 cases. Journal of the American Academy of Dermatology. https://www.sciencedirect.com/science/article/abs/pii/019096229270160H