If you have ever developed a rash that does not behave like a typical skin condition, it can feel unsettling and frustrating. You may apply topical treatments, change skincare products, and follow advice carefully, yet nothing seems to improve the situation. When a rash repeatedly fails to respond to standard approaches, it often suggests that the issue may not be confined to the skin itself.
Your skin is closely connected to what is happening inside your body and often acts as an early warning system. It can reflect internal inflammation, immune activity, or systemic imbalance before other symptoms become obvious. When a rash does not follow expected patterns, spreads unpredictably, or behaves unusually, it signals the need to look beyond surface-level explanations.
In these situations, dermatologists assess more than just the visible rash. Internal causes such as immune-related conditions, infections, medication reactions, hormonal changes, or systemic inflammation may be considered during evaluation. This broader approach helps identify triggers that topical treatments alone cannot address.
Sometimes, these rashes fluctuate in line with your overall health rather than external factors. You may notice worsening during periods of illness, fatigue, hormonal shifts, or internal stress, even when your skincare routine remains unchanged. This pattern often provides a key clue that the root cause lies beneath the surface.
Why the Skin Reflects Internal Health
Your skin is the largest organ in your body and is in constant communication with your immune, nervous, and endocrine systems. Because of this close interaction, internal imbalances often become visible on the skin before they are felt elsewhere. Changes beneath the surface can quickly influence how your skin looks and behaves.
Blood flow, hormonal signals, immune activity, and inflammatory mediators all play a role in regulating skin function. When one of these systems becomes disrupted, the skin may respond with redness, scaling, hives, or changes in pigmentation. This reaction follows a biological pattern and is not random.
Many internal conditions first present through changes in the skin. In some cases, these signs appear well before other symptoms develop, offering an early opportunity for detection. This is why dermatological assessment can play a crucial role in identifying underlying health issues and guiding further investigation.
When a Rash Raises Red Flags
Most rashes are harmless and tend to resolve on their own. However, some rashes may signal a more serious underlying condition and require professional assessment. Recognising the warning signs early can help you seek timely care.
- Persistent or widespread rashes are concerning
Rashes that cover large areas of the body or do not improve over time should not be ignored. Recurrent flare-ups or rashes that fail to respond to standard treatments may indicate a more serious issue. Early recognition helps ensure proper evaluation and management. - Systemic symptoms may indicate underlying illness
The presence of fever, unexplained weight loss, fatigue, joint pain, or night sweats alongside a rash is a significant warning sign. Gastrointestinal symptoms or neurological changes can also point to systemic involvement. These clues guide doctors in identifying the root cause. - Pattern and behaviour of the rash are important
How a rash spreads, its colour, and the timing of flare-ups provide valuable diagnostic information. Dermatologists use pattern recognition to differentiate between minor irritations and conditions requiring further investigation. Careful observation can prevent misdiagnosis. - Professional assessment ensures correct diagnosis and treatment
Even rashes that seem minor may sometimes mask serious conditions. Consulting a dermatologist allows for accurate testing and targeted treatment. Early intervention can reduce complications and improve outcomes.
Rashes are usually harmless, but certain signs should never be ignored. Recognising patterns, persistent symptoms, and systemic clues helps you take action promptly. Seeking professional care ensures that any underlying issues are addressed before they become more serious.
Autoimmune Conditions and Skin Manifestations

Autoimmune diseases frequently affect the skin, as your immune system mistakenly attacks healthy tissue. In many cases, the skin becomes one of the most visible targets, providing early clues that something internal may be wrong.
Lupus is a classic example of an autoimmune condition with prominent skin signs. You may notice facial rashes, increased sensitivity to sunlight, or mouth ulcers, which often lead dermatologists to order further blood tests to confirm the diagnosis.
Dermatomyositis is another autoimmune disease where the skin can show changes before other symptoms develop. Distinctive rashes may appear alongside or even before muscle weakness, making early recognition crucial for effective management.
Vasculitis, which causes inflammation of blood vessels, can also present through the skin. This may produce purpura, ulcers, or painful nodules, and these skin findings often reflect a systemic problem rather than a purely cutaneous issue.
Allergic and Hypersensitivity Reactions
Not all allergic reactions begin in the skin, yet many are first noticed through visible changes on your body. Widespread rashes, redness, or raised bumps often signal that your immune system is responding to an internal trigger. Paying attention to these signs can help you identify when a reaction is more than a minor irritation.
These reactions can be triggered by food, medications, or environmental allergens. Drug eruptions are particularly common, where a new prescription or over-the-counter medication may cause a rash days or even weeks after you begin taking it. The appearance of these rashes can vary widely, from subtle redness to dramatic, widespread eruptions, which can make recognising the cause more challenging.
Some allergic reactions can be severe and require urgent medical attention. Certain rashes may indicate potentially life-threatening hypersensitivity, such as those linked with anaphylaxis or serious drug reactions. Early recognition and prompt management are essential not only to relieve symptoms but also to protect your overall health and prevent more serious complications.
Being aware of how your skin reacts to internal triggers empowers you to act quickly. Documenting new rashes, noting recent exposures, and seeking professional advice can help dermatologists pinpoint the cause. This proactive approach ensures your skin is not only treated effectively but also that any underlying systemic issue is addressed safely.
Infectious Diseases That Present as Rashes
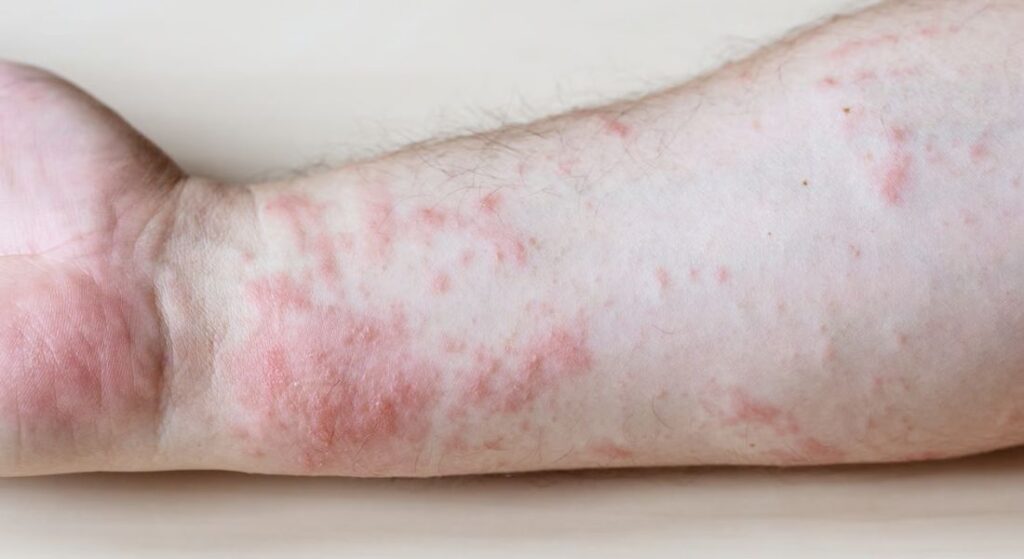
Many infections can cause changes in your skin, often reflecting your body’s immune response rather than a direct infection of the skin itself. Recognising the timing, pattern, and distribution of these rashes can provide important clues to the underlying illness.
Viral infections frequently produce rashes as part of their clinical presentation. Conditions such as measles, rubella, and parvovirus are classic examples, although adults may sometimes present with atypical symptoms that make diagnosis more challenging. Paying attention to accompanying signs, such as fever or fatigue, can help you and your healthcare provider identify the cause.
Bacterial infections can also affect the skin, sometimes in subtle ways. For example, endocarditis or other systemic bacterial illnesses may produce small lesions on the hands, feet, or elsewhere, which are often diagnostically significant even if they appear minor.
Systemic fungal infections may involve the skin as well, particularly in individuals with compromised immune systems. These cases can present with unusual rashes, scaling, or discolouration, and prompt investigation is vital to prevent more serious complications. Being aware of these potential infectious causes emphasises the importance of not ignoring unexplained skin changes.
Gastrointestinal Disease and Skin Clues
Your gut and skin are closely connected through shared immune pathways, meaning that disruption in one system often affects the other. This gut skin connection is well recognised, and changes in your skin can sometimes provide early clues to underlying gastrointestinal issues.
Coeliac disease frequently presents with a distinctive rash called dermatitis herpetiformis. This intensely itchy, blistering rash reflects gluten sensitivity and cannot be managed with topical treatments alone it requires strict dietary and systemic management. Noticing these signs early allows for timely intervention and improved long-term outcomes.
Inflammatory bowel disease (IBD) can also produce skin manifestations. Conditions such as erythema nodosum and pyoderma gangrenosum are examples, and these rashes often correlate with periods of active disease. Observing changes in your skin can therefore provide valuable information about your underlying gastrointestinal health.
Liver disease may also affect your skin, causing symptoms such as persistent itching, pigmentation changes, or yellowing (jaundice). These signs warrant immediate evaluation, as they can indicate significant systemic involvement that requires prompt medical attention. Being aware of these skin clues helps you respond quickly and seek appropriate care.
Hormonal and Endocrine Disorders
Hormones play a crucial role in maintaining healthy skin. Imbalances in these systems often lead to visible changes that can provide important clues about your overall health. Recognising these signs early can help prevent complications.
- Hormonal imbalances often produce noticeable skin changes
Changes in hormone levels can affect skin texture, colour, and sensitivity. Rashes may appear as one of several visible indicators. Paying attention to these changes can help identify underlying endocrine issues. - Thyroid disorders affect skin, hair, and nails
Conditions like hypothyroidism or hyperthyroidism can cause dryness, flushing, swelling, and changes in skin texture. Hair thinning and nail abnormalities often occur alongside skin changes. These symptoms together provide important diagnostic clues. - Diabetes can influence skin health
Poor glucose control impacts circulation and immune response, increasing the likelihood of infections or delayed healing. Certain rashes may signal uncontrolled blood sugar levels. Early detection allows timely intervention to prevent further complications. - Adrenal disorders may cause gradual pigmentation changes
Disorders affecting adrenal function can result in subtle, progressive changes in skin colour. These changes often develop slowly, making them easy to overlook without careful observation. Dermatological expertise can aid in identifying and managing these conditions.
Hormonal and endocrine disorders can have a wide-ranging impact on skin health. Observing changes in rashes, texture, and colour can provide early clues to underlying problems. Seeking professional assessment ensures accurate diagnosis and timely management, helping to protect both skin and overall wellbeing.
Nutritional Deficiencies and Skin Signs
Your skin relies on adequate nutrition to function and maintain its protective barrier. When essential nutrients are lacking, deficiencies may present as rashes, dryness, changes in texture, or increased sensitivity, yet these signs are often overlooked or misattributed.
Certain nutrients are particularly important for skin health. For example, zinc deficiency can cause periorificial rashes around the mouth, eyes, or nose, while iron deficiency may lead to pallor, itching, or subtle changes in hair and nails. Vitamin deficiencies, such as those of vitamin A, C, or D, can impair barrier function and delay healing, making your skin more vulnerable to irritation and inflammation.
These nutritional conditions are more common than many people realise and often coexist with underlying absorption disorders or chronic illnesses. Because of this, investigation usually extends beyond the skin itself, involving dietary assessment, blood tests, and sometimes referral to a specialist. Recognising these signs early allows you to address deficiencies proactively and support both skin and overall health.
Haematological Conditions and the Skin
Blood disorders frequently present with changes in your skin, often providing early clues to underlying health issues that may not yet be obvious. Alterations in clotting, platelet function, or blood cell counts can produce visible signs, which may occur without discomfort or itching, making them easy to overlook. Being aware of these subtle cues can help you seek assessment before more serious complications arise.
Petechiae tiny red or purple spots and larger purpura are classic indicators of bleeding under the skin. These signs require urgent evaluation, as they can point to conditions such as thrombocytopenia, clotting disorders, or other systemic blood diseases. Early recognition is vital, as timely intervention can prevent progression and support safer management of these disorders.
Anaemia can also show in your skin, causing noticeable pallor, dryness, and a general dullness to your complexion. You may also bruise more easily or notice changes in nail and hair health, reflecting underlying deficiencies or red blood cell abnormalities. Paying attention to these subtle changes can guide further testing and help identify the root cause.
In some cases, skin changes can provide diagnostic clues even before more severe systemic symptoms develop. Documenting new spots, bruising patterns, or persistent pallor and sharing these observations with a healthcare professional can assist in accurate diagnosis. Early detection ensures that any underlying haematological condition is addressed promptly, supporting both your skin’s health and your overall wellbeing.
When Dermatologists Investigate Beyond the Skin

A dermatologist is trained to recognise patterns and subtle clues that indicate whether a rash is purely a skin issue or a sign of something deeper. When a rash does not fit a primary skin diagnosis, further investigation is often necessary to protect your overall health and ensure nothing significant is missed.
This process may involve a variety of diagnostic steps. Blood tests can identify systemic conditions, hormonal imbalances, or nutrient deficiencies, while imaging or skin biopsy may be required to provide more detailed information. Each investigation is tailored to your individual presentation to guide accurate diagnosis and treatment.
In some cases, referral to other specialists, such as immunologists, gastroenterologists, or haematologists, may be appropriate to address underlying causes effectively. A consultation with a specialist dermatologist at the London Dermatology Centre can help ensure that systemic causes are identified and managed, giving you peace of mind and a clear plan for your skin and overall health.
Why Topical Treatment Alone Sometimes Fails
Topical treatments are designed to target inflammation and irritation at the surface of your skin, providing relief for redness, itching, or swelling. While these treatments can be effective for managing symptoms, they do not address the internal drivers that may be causing the rash in the first place.
This is why some rashes persist despite careful application of creams or ointments. Repeated flare-ups, or temporary improvement followed by relapse, are often a sign that the underlying cause whether it’s immune-related, nutritional, hormonal, or systemic remains active.
Understanding this concept can prevent frustration when standard treatments appear ineffective. By recognising that skin symptoms often reflect deeper issues, you can shift focus toward a more comprehensive approach, combining topical care with investigation and management of internal factors.
Taking this holistic view leads to better long-term outcomes. Your skin becomes healthier and more resilient, and flare-ups are reduced, because both the visible symptoms and their underlying causes are being addressed together.
The Emotional Impact of Unexplained Rashes
Unexplained rashes can be worrying and affect more than just your skin. They often cause anxiety and raise concerns about underlying health issues. Understanding the emotional side of skin conditions is an important part of care.
- Rashes can create anxiety and uncertainty
Sudden or unexplained skin changes may lead to worry about serious illness. The unpredictability of flare-ups can make daily life stressful. Recognising this emotional impact is important for overall wellbeing. - Validation of symptoms is crucial
Your concerns and experiences are real and deserve professional attention. Being heard and understood helps reduce stress and fosters trust in your care. This validation can make navigating treatment much easier. - Early assessment reduces worry
Prompt dermatological evaluation can clarify the cause of your symptoms. Knowing what is happening lessens uncertainty and allows timely treatment. Early intervention supports both physical and emotional health. - Holistic care ensures nothing is overlooked
Dermatology often overlaps with general medicine, addressing broader health concerns. A holistic approach helps identify underlying issues that may contribute to skin changes. This ensures comprehensive care for both body and mind.
Recognising the emotional impact of unexplained rashes is as important as addressing the physical symptoms. Early evaluation and empathetic care can ease anxiety and provide clarity. By taking both aspects seriously, you can protect your skin and support your overall wellbeing.
What You Can Do as a Patient
Pay close attention to the timing of your skin changes and any potential triggers. Note when rashes appear, worsen, or improve, and consider whether they coincide with diet, stress, environmental factors, or new medications. Keeping a detailed record can provide valuable insight for both you and your dermatologist, making it easier to pinpoint underlying causes.
Observe and document any associated symptoms beyond the skin, such as digestive disturbances, fatigue, joint pain, or fever. Sharing this information clearly during consultations allows your healthcare provider to build a more complete picture of your overall health, helping to identify systemic factors that may be contributing to your skin condition.
Avoid self-diagnosing online, as misinformation is common and can increase anxiety or prompt unnecessary interventions. While it may be tempting to look for answers yourself, professional assessment is the safest and most effective way to understand what is happening with your skin and to ensure appropriate care is provided.
If your symptoms persist, worsen, or flare repeatedly, seek review promptly rather than waiting. Early input can make a significant difference in diagnosing and managing the issue, helping to prevent complications or chronic problems. Remember, your skin may be signalling something important about your internal health, and listening carefully to these signals enables you to take control of both your skin and overall wellbeing.
FAQs
1. When should I suspect that a rash is linked to an internal health problem?
A rash may indicate an internal issue if it is persistent, widespread, unpredictable, or does not respond to standard topical treatments. Additional warning signs include systemic symptoms like fever, fatigue, joint pain, or digestive changes.
2. How can skin reflect internal health conditions?
Your skin communicates closely with the immune, endocrine, and nervous systems. Hormonal imbalances, inflammation, or immune activity can manifest as rashes, redness, scaling, or pigmentation changes before other symptoms appear.
3. Which autoimmune conditions often present with skin changes?
Autoimmune diseases such as lupus, dermatomyositis, and vasculitis frequently cause rashes or other skin changes. Dermatologists often detect these early signs and may order blood tests for confirmation.
4. Can allergies or medication reactions cause systemic rashes?
Yes. Food, medications, or environmental allergens can trigger rashes that appear suddenly or gradually. Some reactions, like drug eruptions or anaphylaxis, may require urgent medical attention.
5. What infections can show early signs on the skin?
Viral infections (measles, rubella, parvovirus), bacterial illnesses (like endocarditis), and systemic fungal infections may all present with rashes that reflect the body’s immune response rather than direct skin infection.
6. How do gastrointestinal diseases impact the skin?
Conditions such as coeliac disease, inflammatory bowel disease, and liver disorders can produce characteristic rashes. Recognising these early skin signs can help diagnose underlying gastrointestinal problems.
7. Which hormonal and endocrine issues cause skin changes?
Thyroid disorders, diabetes, and adrenal conditions can all alter skin texture, colour, or sensitivity. Observing rashes alongside other symptoms can guide diagnosis and treatment.
8. Can nutritional deficiencies show up as rashes?
Yes. Deficiencies in zinc, iron, vitamins A, C, or D may cause rashes, dryness, or delayed healing. Early recognition allows for dietary correction and improved skin health.
9. Why might topical treatments fail to improve certain rashes?
Topical creams address surface inflammation but cannot treat underlying systemic causes. Persistent rashes often indicate immune, hormonal, nutritional, or internal health issues that require investigation.
10. What should I do if I notice an unexplained rash?
Document the rash, note timing, triggers, and any systemic symptoms, and consult a dermatologist promptly. Avoid self-diagnosis online and seek professional assessment to identify potential internal causes and receive appropriate care.
Final thought: When a Rash Signals More Than Skin Deep
Rashes that do not respond to standard treatments may signal underlying internal health issues rather than a simple skin problem. Understanding that your skin can reflect systemic conditions ranging from autoimmune diseases to hormonal imbalances, nutritional deficiencies, or infections helps you take a proactive approach to your health. Paying attention to patterns, triggers, and associated symptoms can provide valuable insights that guide more effective care.
For personalised assessment and guidance, consulting a qualified dermatologist is essential. They can investigate both surface and internal causes, ensuring that any underlying conditions are identified and managed appropriately. You can book a consultation with one of our dermatologists by contacting us at the London Dermatology Centre.
References
- Méndez‑Flores, S., et al. (2021) Skin manifestations associated with systemic diseases: Part I, Journal of the European Academy of Dermatology and Venereology, 35(7), pp. e394–e404 https://pubmed.ncbi.nlm.nih.gov/34544638/
- Reunala, T., Salmi, T.T., Hervonen, K., Kaukinen, K. and Collin, P.(2018) Dermatitis herpetiformis: a common extraintestinal manifestation of coeliac disease, Nutrients, 10(5), 602. https://www.mdpi.com/2072-6643/10/5/602
- Lazear, J.W. and Hammer, K.A.(2021) Skin manifestations associated with systemic diseases – Part II, Anais Brasileiros de Dermatologia, 96(6), pp. 672–687. https://www.sciencedirect.com/science/article/pii/S0365059621002051
- Association between atopic dermatitis and autoimmune diseases (2024) British Journal of Dermatology, 185(2), pp. 335–345. https://academic.oup.com/bjd/article/185/2/335/6600304
- Bargai, D. and Goldberg, E. (2015)Dermatologicmanifestations of systemic diseases, Primary Care: Clinics in Office Practice, 42(3), pp. 333–352. https://pubmed.ncbi.nlm.nih.gov/26612375/
