It’s easy to assume that if something doesn’t hurt, it isn’t serious. Many people only seek help when skin changes become painful, itchy, or uncomfortable. Unfortunately, some of the most important skin warning signs cause little to no sensation at all.
Dermatologists are trained to recognise subtle changes that signal underlying disease long before symptoms appear. Understanding these early signs helps protect both your skin health and overall wellbeing.
In this article, we’ll explain which skin changes should never be ignored, why pain is not a reliable indicator of seriousness, and when professional assessment matters most.
Why Pain Is a Poor Indicator of Skin Health
Pain is not a reliable signal of skin health. We often see that the skin does not warn us through discomfort, even when something significant is developing. Many conditions progress silently without causing pain.
Several serious skin problems evolve slowly and quietly. By the time pain or soreness appears, meaningful progression may already have occurred. This delay can create a false sense of reassurance.
That is why we pay closer attention to visual changes, texture, colour, and behaviour of the skin over time. These signs often tell us far more than symptoms alone. Early observation allows us to act before problems become advanced.
Why the Skin Can Look Normal While Disease Develops
Skin disease often begins beneath the surface. Changes in cell behaviour, pigment production, or immune activity can occur at a microscopic level before anything obvious appears. This means the skin may look normal while underlying processes are already shifting.
Early disease can seem subtle or even harmless at first glance. We know that the absence of redness, pain, or visible inflammation does not always mean the skin is healthy. This quiet phase is where conditions are easiest to miss.
Dermatologists focus on pattern and behaviour rather than dramatic signs. We look for small changes over time, not just what stands out on a single day. This approach helps identify problems early, before they become more visible or harder to manage.
Changes in Colour That Deserve Attention
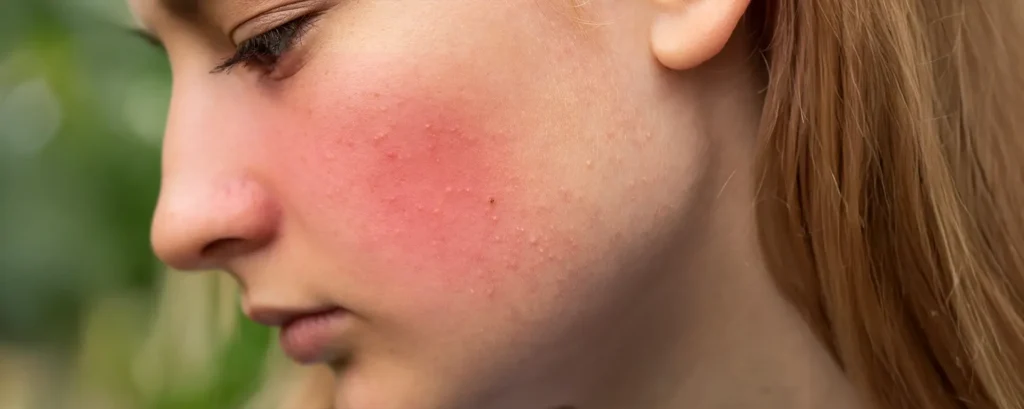
Changes in skin colour are one of the most important clues we look for during assessment. Colour can reveal what’s happening beneath the surface, even when there is no pain or obvious symptom. This is why colour changes should never be ignored.
Here’s what we pay close attention to:
1. Colour Change Is a Key Warning Sign – Darkening, lightening, or uneven pigmentation can signal an underlying problem. These changes often appear before other symptoms develop.
2. Unusual Shades Need Assessment – Red, brown, black, blue, or grey tones that look out of place should always be checked. Even subtle or painless colour changes can be medically significant.
3. Pigmentation Patterns Matter – It’s not just the colour itself, but how it appears. Irregular edges, mixed colours, or patchy distribution can provide important diagnostic clues.
4. Change Over Time Is Just as Important – A colour that evolves, spreads, or deepens over time is more concerning than one that remains stable. Tracking change helps us distinguish harmless variation from early disease.
Colour changes don’t need to hurt to matter. By paying attention to both appearance and progression, we can identify issues earlier and act appropriately. Early assessment helps separate harmless changes from those that require prompt treatment, protecting your skin health in the long term.
Why New Pigmentation Should Never Be Ignored
New pigmentation that appears without clear injury or inflammation should always be taken seriously. We see this as a red flag, especially when dark spots or patches develop suddenly. Skin does not usually change colour without an underlying reason.
Irregular pigmentation, spreading colour, or changes beyond previous boundaries often reflect altered cellular activity beneath the surface. Even when the skin feels normal, these visual changes can signal early disease. We focus on behaviour and pattern, not just symptoms.
Early review makes a real difference to outcomes. We encourage you not to wait and watch when new pigmentation appears. Timely assessment allows us to identify the cause early and guide appropriate care with greater confidence.
When Existing Marks Change Colour
Stable skin marks usually stay the same over time. When a mole, freckle, or patch begins to change colour, it deserves careful attention. We consider this change more important than how the mark looks on any single day.
If an area becomes darker, lighter, patchy, or uneven, it should be assessed. These shifts can indicate altered activity beneath the surface, even if there is no pain or irritation. We focus on evolution rather than reassurance based on familiarity.
Monitoring change over time is critical in skin assessment. We encourage you to note differences rather than dismiss them as normal variation. Early evaluation helps ensure that concerning changes are identified and managed promptly.
Texture Changes That Signal Underlying Problems
Texture changes in the skin are often overlooked, especially when there is no pain or irritation. We see skin become rough, scaly, thickened, shiny, or even subtly indented without obvious symptoms. These quiet changes can still be significant.
Altered texture may reflect chronic inflammation, scarring processes, or early malignant change beneath the surface. Even when colour looks unchanged, the way skin feels can reveal important clues. We do not rely on appearance alone.
Touch can reveal what the eye misses. We assess firmness, thickness, and surface quality as part of proper skin evaluation. Paying attention to texture helps us identify problems earlier, when outcomes are usually better.
Why Persistent Rough Patches Matter
Not all skin changes are dramatic or painful. Rough or gritty patches that linger often seem easy to ignore, but they can be an important signal that something deeper is happening in the skin. This is why persistence matters more than discomfort.
Here’s why these patches deserve attention:
1. Persistence Is a Key Red Flag – If a rough patch doesn’t settle despite moisturising or time, it needs assessment. Skin that fails to return to normal is telling us something isn’t resolving on its own.
2. They Can Represent Precancerous Change – Some persistent rough areas are linked to early precancerous processes. These changes are often subtle and painless, which is why they’re easy to overlook.
3. Chronic Inflammation Is Another Cause – Ongoing inflammation can also create rough, scaly skin that never fully heals. Left untreated, this inflammation can continue to damage the skin barrier and surrounding tissue.
4. Lack of Pain Does Not Mean Low Risk – Many significant skin conditions cause little or no discomfort. The absence of pain should never be used as reassurance when texture changes persist.
Early intervention makes a real difference. By assessing rough patches before they progress, we can treat problems at a simpler stage and reduce the risk of long-term damage. Paying attention early helps protect both your skin health and peace of mind.
Skin Thickening Without Inflammation
Skin thickening is not always caused by friction or repeated rubbing. We often see gradual thickening develop without redness, pain, or obvious inflammation. This makes it easy to overlook.
These changes can reflect chronic low-grade inflammation, fibrosis, or even underlying systemic disease. Because they develop slowly and quietly, they may not draw attention until they are well established. Appearance alone is not always reassuring.
Assessment helps clarify the cause. We examine texture, distribution, and progression over time to understand what is driving the change. Early evaluation allows us to address the underlying issue before it becomes more difficult to manage.
Why Shiny or Tight Skin Is Concerning
Shiny or tight skin can reflect deeper structural change rather than surface dryness alone. We often see this when normal elasticity is reduced or the skin’s support framework is altered. These changes tend to develop gradually and can be easy to dismiss.
Loss of elasticity or abnormal collagen deposition can change how the skin reflects light and moves. We recognise that this appearance is rarely part of normal skin behaviour. Even when there is no redness or discomfort, the visual change can be meaningful.
Subtle tightness should not be ignored. We assess how the skin feels, stretches, and behaves over time. Early recognition helps us identify underlying causes and guide appropriate care before changes become more pronounced.
Lesions That Don’t Heal
When a skin lesion does not heal within a few weeks, it deserves careful attention. Normal skin repair follows a predictable timeline, and delays can signal an underlying issue. Even lesions that seem minor or painless should not be ignored.
Lesions that don’t heal are concerning because:
- Delayed healing is a warning sign – Skin that fails to repair within weeks may indicate abnormal cell behaviour or ongoing damage.
- Bleeding or crusting can persist – Recurrent scabbing, oozing, or surface breakdown suggests the area is not healing normally.
- Lack of pain can be misleading – Many concerning lesions cause little or no discomfort, which can delay seeking review.
- Stability does not equal safety – Lesions that remain unchanged rather than improving still require assessment.
By recognising delayed healing early, we can investigate appropriately and protect long-term skin health.
Why Bleeding Without Injury Is a Red Flag
Healthy skin does not bleed on its own. When bleeding occurs without obvious injury or trauma, we see this as an important warning sign. Skin usually requires force or damage to break the surface.
Bleeding without trauma suggests fragile or abnormal tissue. This can happen even in small lesions that look harmless and cause no pain. The absence of discomfort does not make the finding less significant.
Any unexplained bleeding should always be assessed. We take this sign seriously because it can indicate underlying disease. Early review allows us to identify the cause promptly and guide appropriate management.
New Growths That Feel Different
New skin growths can be easy to dismiss, especially when they don’t hurt. However, sensation alone is not a reliable indicator of risk. What matters most is how a growth behaves and changes over time.
Here’s what we pay attention to:
1. Painless Does Not Mean Harmless – Many significant skin conditions cause little or no pain. The absence of discomfort should never be used as reassurance when a new growth appears.
2. Texture and Consistency Matter – Changes in firmness, softness, or an unusual texture can indicate abnormal behaviour. A growth that feels different from the surrounding skin deserves assessment.
3. Fixation or Rapid Growth Raises Concern – Growths that feel fixed in place or increase in size quickly are more concerning. These features suggest activity beneath the surface rather than a superficial change.
4. Behaviour Is More Important Than Sensation – How a growth develops, changes, or spreads matters far more than whether it hurts. Pattern and progression guide clinical concern, not pain levels.
By focusing on growth behaviour rather than discomfort, we can identify problems earlier. Prompt assessment allows us to intervene at a simpler stage and avoid unnecessary delay. This careful approach helps protect long-term skin health and reassurance.
Why Symptom-Free Lumps Can Be Serious
Many people dismiss lumps simply because they don’t cause pain. We understand why this feels reassuring, but pain is not a reliable indicator of seriousness. The skin does not always signal concern through discomfort.
Some serious skin conditions present as painless nodules that grow slowly and quietly. We often see delays in assessment because nothing feels “wrong.” Waiting for pain can allow progression before attention is sought.
Early evaluation improves safety and outcomes. We encourage assessment based on change, persistence, or unusual features rather than symptoms alone. Identifying concerns early allows us to act before problems become more complex.
Changes in Existing Moles
Moles are expected to remain stable over time. When a mole begins to change in size, shape, border, colour, or elevation, we see this as an important warning sign. Stability matters more than how long a mole has been present.
Pain is rarely present in the early stages of concerning change. We often find that visual or structural changes occur quietly, without discomfort or irritation. The absence of symptoms should not be reassuring.
Evolution is the key feature we assess in dermatology. We focus on how a mole behaves over time rather than how it looks on a single day. Early review of changing moles improves safety and clinical outcomes.
Why Asymmetry Matters More Than Size
When assessing skin lesions, size alone is rarely the most important factor. Many harmless lesions can be large, while more concerning changes may be small and subtle. What matters most is how a lesion looks and behaves as a pattern.
Asymmetry is more important than size because:
- Uneven shape raises concern – Lesions that are not symmetrical are more likely to represent abnormal growth patterns.
- Irregular borders signal instability – Jagged or poorly defined edges are more concerning than smooth, even outlines.
- Uneven colour suggests abnormal change – Variation in colour within a lesion often matters more than how big it is.
- Pattern recognition guides decisions – We assess how features combine, rather than judging risk by size alone.
By focusing on shape, borders, and colour together, we can identify lesions that need attention even when they appear small.
Skin Changes That Appear After Adulthood
Many harmless skin features develop during childhood and remain stable for years. When new skin changes appear later in adulthood, we pay closer attention to them. Timing provides important diagnostic context.
Adult-onset lesions are not automatically serious, but they do deserve assessment. We look carefully at how and when the change appeared, and whether it continues to evolve. New growths behave differently from long-standing marks.
Timing matters in diagnosis because it helps us distinguish normal variation from potential disease. We focus on onset, progression, and behaviour rather than reassurance based on appearance alone. Early review supports safer, more accurate decisions.
Why Itching Is Not Always Present

It’s a common belief that serious skin problems must itch or feel uncomfortable. In reality, many significant skin conditions are silent in their early stages. This is why relying on symptoms alone can be misleading.
Itching is not always present because:
- Many concerning conditions are initially symptom-free – Serious skin changes can develop without itch, pain, or irritation.
- Lack of discomfort delays attention – When a lesion does not bother you, it is easier to overlook or ignore.
- Visual change often comes first – Alterations in colour, shape, or texture frequently appear before any sensation develops.
- Assessment relies on appearance, not symptoms alone – We focus on visible patterns and behaviour rather than waiting for discomfort to appear.
By paying attention to visual changes rather than symptoms alone, we can identify concerning lesions earlier and act more effectively.
Subtle Changes in Nail Appearance
Nails often provide early clues about what’s happening in the skin and the body as a whole. Because nail changes are usually painless and develop slowly, they’re easy to overlook. However, subtle alterations can be clinically important.
Here’s why nail changes deserve attention:
1. Nails Reflect Overall Health – Nails are influenced by circulation, nutrition, inflammation, and systemic disease. Changes in nail appearance can signal issues beyond the nail itself.
2. Discolouration Can Indicate Underlying Problems – White, yellow, brown, or dark streaks are not always cosmetic. These colour changes may point to infection, inflammatory conditions, or systemic disease.
3. Structural Changes Matter – Splitting, ridging, thickening, or separation from the nail bed without injury suggests abnormal nail growth. These patterns often develop due to ongoing skin or internal conditions.
4. Lack of Pain Is Common – Many nail conditions cause little or no discomfort. Absence of pain should not be taken as reassurance when visible changes persist.
Nails should never be ignored when changes are unexplained or progressive. By paying attention early, we can identify underlying causes sooner and manage them more effectively. Careful assessment helps protect both nail health and overall wellbeing.
Changes Around the Lips, Eyes, and Ears
Certain areas of the face require extra caution. We pay close attention to changes around the lips, eyelids, and ears because the skin here behaves differently and is more vulnerable. Even subtle alterations can carry greater significance.
These areas are common sites for serious skin conditions, and changes are often painless. We frequently see lesions that do not cause discomfort but still represent underlying disease. The absence of symptoms should not be reassuring.
Early review helps protect both function and appearance. We assess changes promptly to prevent progression and avoid complex treatment later. Careful attention to these areas supports safer outcomes and long-term skin health.
Skin Changes That Slowly Spread
Gradual spread is an important warning sign in skin assessment. We often see lesions that expand slowly over months rather than days. This pace can make change easy to overlook.
Slowly spreading lesions may indicate underlying inflammatory or malignant processes. Because progression is subtle, it is often underestimated or dismissed as harmless. Lack of pain or irritation does not reduce significance.
The rate of change matters as much as appearance. We assess how a lesion behaves over time, not just how it looks at one point. Recognising gradual spread early helps us guide timely and appropriate care.
Why Long-Standing Skin Changes Still Need Professional Review
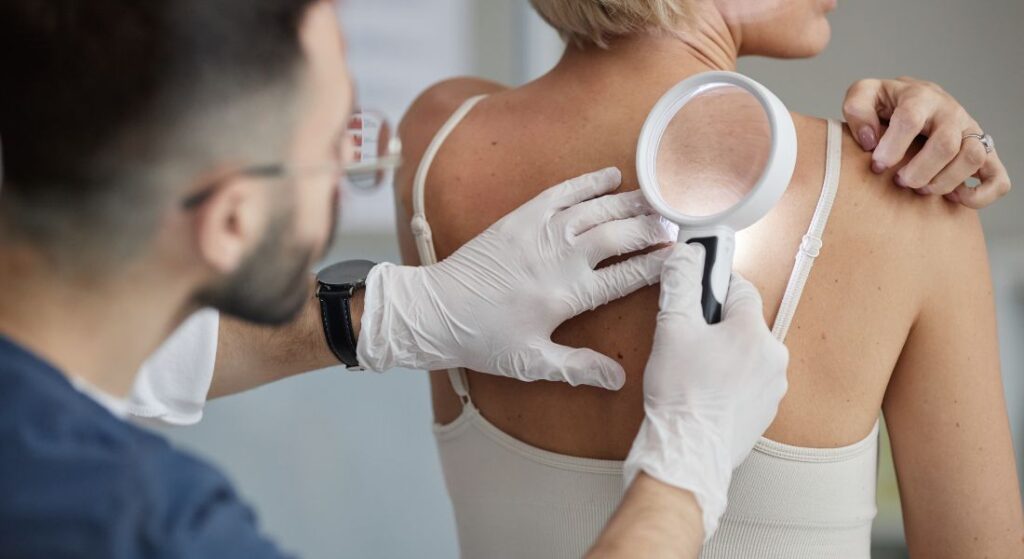
We often feel reassured when a mark or lump has been there for years, but time alone does not confirm safety. Some significant skin conditions develop slowly, and long-standing lesions can still evolve in colour, shape, texture, or behaviour. That is why we treat stability as something to be checked and confirmed, rather than assumed.
We encourage self-checks because they help us stay aware of our skin, but self-monitoring has clear limits. When we see the same area every day, gradual change can be surprisingly easy to miss, and familiarity can make new warning signs feel “normal”. A professional review helps us compare what we are seeing with what should be expected, and it reduces the risk of overlooking slow progression.
When we assess silent skin changes, we look beyond a single spot and focus on patterns and context. We consider symmetry, distribution, evolution over time, surface texture, and how the surrounding skin looks and feels. Tools such as dermoscopy can reveal features not visible to the naked eye, which helps us make a more accurate judgement and decide whether simple monitoring or further investigation is needed.
Why Early Dermatology Review Matters for Unusual Skin Changes
We should seek professional review for any skin change that is new, changing, non-healing, or simply unusual for our skin. If something looks different from what is normal for us, it is worth trusting that instinct rather than waiting for it to “prove” itself. A consultation with a qualified Dermatologist can give clear answers and genuine reassurance, especially when the change is subtle.
Early assessment protects long-term health because earlier diagnosis often leads to simpler, more effective treatment. Many serious skin conditions are highly treatable when caught early, while delays can increase complexity, widen treatment options, and raise overall risk. Skin changes can also be the first signal that something deeper is happening, which is why early review is always the safer choice.
Specialist care makes a difference because it is designed to detect subtle warning signs, not just obvious problems. At the London Dermatology Centre, our evaluation is based on clinical expertise and careful assessment rather than assumptions about what “should” be harmless. This approach supports timely management and prioritises prevention just as strongly as treatment, helping us protect skin health with confidence.
FAQS:
1. Why can serious skin problems develop without any pain or discomfort?
The skin does not always signal concern through pain or irritation. Many serious conditions develop slowly at a cellular level without affecting nerves. By the time discomfort appears, the condition may already be more advanced, which is why visual changes matter more than sensation.
2. Should I worry about a skin change if it doesn’t itch, bleed, or hurt?
Yes, the absence of symptoms does not mean a skin change is harmless. Many important warning signs are completely symptom-free in their early stages. Dermatologists rely on appearance, texture, and behaviour over time rather than discomfort alone.
3. How long should a skin change be present before I seek medical advice?
Any new, changing, or non-healing skin change that persists for more than a few weeks should be assessed. Normal skin repairs itself within a predictable timeframe. Delayed resolution suggests that further evaluation is needed, even if the area feels normal.
4. Are colour changes more important than size when assessing skin lesions?
Colour change is often more significant than size. Small lesions with uneven or changing colour can be more concerning than large, stable marks. Dermatologists focus on variation, pattern, and evolution rather than size alone.
5. Why are changes in texture taken seriously even when colour looks normal?
Texture changes can reflect deeper structural or cellular alterations beneath the surface. Thickening, roughness, or shininess may signal chronic inflammation or abnormal growth. These changes often appear before colour or symptoms develop.
6. Is it normal for skin lesions to bleed occasionally without injury?
No, healthy skin does not bleed without trauma. Unexplained bleeding, even from a small or painless lesion, is a warning sign that should always be assessed. Bleeding often indicates fragile or abnormal tissue rather than harmless change.
7. Can long-standing skin marks still become a problem years later?
Yes, time alone does not guarantee safety. Some skin conditions evolve very slowly and may change subtly after years of stability. Regular review is important because gradual change is often harder to notice without professional assessment.
8. Why are changes on the face, lips, and ears treated more urgently?
Skin in these areas is thinner, more sun-exposed, and behaves differently from other parts of the body. Serious conditions can develop here without pain or obvious symptoms. Early assessment helps protect both function and appearance.
9. Do nail changes really indicate skin or health problems?
Nails can reflect changes in skin biology, circulation, inflammation, or systemic health. Discolouration, thickening, or separation without injury should not be ignored. Nail changes are often painless, which is why they are commonly overlooked.
10. When is the right time to see a dermatologist for a silent skin change?
The right time is when a change is new, evolving, persistent, or simply unusual for your skin. Waiting for pain or irritation can delay diagnosis. Early dermatology review provides reassurance when things are benign and enables prompt care when they are not.
Final Thoughts: Why Silent Skin Changes Deserve Serious Attention
Skin does not always warn us through pain, itching, or discomfort. Many important skin conditions develop quietly, showing their first signs through subtle changes in colour, texture, shape, or behaviour over time. Understanding that symptom-free does not mean harmless allows you to respond earlier, when assessment is simpler and outcomes are usually better. Paying attention to what looks different from your normal skin, rather than waiting for something to hurt, is one of the most effective ways to protect long-term skin health.
If something new, changing, or persistent has caught your attention, an assessment with an experienced Dermatologist can provide clarity and reassurance. If you’re interested in arranging a consultation with one of our dermatologists, you can reach out to us at the London Dermatology Centre.
References
1. Dildar, M., Akram, S., Irfan, M., Khan, H.U., Ramzan, M., Mahmood, A.R., Alsaiari, S.A., Saeed, A.H.M., Alraddadi, M.O. and Mahnashi, M.H. (2021) Skin Cancer Detection: A Review Using Deep Learning Techniques, International Journal of Environmental Research and Public Health, 18(10), 5479. https://www.mdpi.com/1660-4601/18/10/5479
2. Nazari, S. and Garcia, R. (2023) Automatic Skin Cancer Detection Using Clinical Images: A Comprehensive Review, Life, 13(11), 2123. https://www.mdpi.com/2075-1729/13/11/2123
3. Recent Advancements and Perspectives in the Diagnosis of Skin Diseases Using Machine Learning and Deep Learning: A Review (2024) A comprehensive PubMed review summarising diverse diagnostic strategies for skin disease including feature analysis of lesion colour and texture. https://pubmed.ncbi.nlm.nih.gov/38066747/
4. Clinically Inspired Skin Lesion Classification through the Detection of Dermoscopic Criteria for Basal Cell Carcinoma (2022) Demonstrates the importance of colour and texture analysis in differentiating BCC from benign lesions based on dermoscopic criteria. https://pubmed.ncbi.nlm.nih.gov/35877641/
5. Saravanan, S. (2020) Skin cancer detection using dermoscope images, Journal of Dermatological Science Extracts features including asymmetry, border, colour, and diameter for skin cancer detection, highlighting clinical relevance of visual changes even if asymptomatic. https://www.sciencedirect.com/science/article/abs/pii/S221478532036260X
