Many people are told they have a fungal infection when they develop a red, itchy, or scaly rash. Antifungal creams are started quickly, often without testing, and weeks later the skin is no better or even worse. This situation is far more common than most people realise.
The problem is that many non-fungal skin conditions closely resemble fungal infections. Treating the wrong condition with antifungals can delay recovery, mask the real diagnosis, and sometimes worsen inflammation.
In this article, we explain the skin conditions most often misdiagnosed as fungal infections, why antifungal treatment can fail, and when seeing a Dermatologist makes all the difference.
Why Fungal Infections Are Over-Diagnosed
Fungal infections are common and familiar, which makes them easy to assume. Many rashes look superficially similar to conditions people already recognise, so treatment is often started based on appearance alone. This approach can be misleading and delay the correct diagnosis.
Fungal infections are over-diagnosed because:
- Classic appearances are over-relied upon – Red, itchy, ring-shaped, or scaly rashes are quickly labelled as “ringworm” or “athlete’s foot” without further assessment.
- Many non-fungal conditions look similar – Eczema, psoriasis, contact dermatitis, and inflammatory rashes can closely mimic fungal patterns.
- Early or treated rashes lose defining features – Previous creams or partial treatment can alter how a condition looks, making visual diagnosis unreliable.
- Appearance alone is rarely diagnostic – Without considering history, distribution, response to treatment, or testing, misdiagnosis becomes more likely.
By looking beyond surface appearance, we can avoid unnecessary antifungal treatment and reach a more accurate diagnosis sooner.
Top of Form
Bottom of Form
Why Treating the Wrong Condition Makes Skin Worse
Treating the wrong condition can often make skin problems worse rather than better. Antifungal creams, for example, are not neutral products. When used incorrectly, they can irritate already inflamed skin and disrupt the skin barrier.
In some cases, antifungals may temporarily suppress visible symptoms without addressing the real cause. We see this delay proper diagnosis while the underlying condition continues to progress quietly. This can make the skin harder to treat later.
Using the wrong treatment creates confusion and prolongs skin problems. We focus on identifying the correct cause before recommending therapy, because accurate treatment matters more than quick fixes. The right diagnosis protects your skin and supports proper recovery.
How Dermatologists Approach Suspected Fungal Rashes
Fungal rashes can look deceptively similar to other inflammatory skin conditions. That’s why we don’t rely on appearance alone when assessing them. A careful, step-by-step approach helps us avoid misdiagnosis and unnecessary treatment.
Here’s how we assess suspected fungal rashes:
1. Appearance Alone Is Not Enough – Many fungal rashes resemble eczema, psoriasis, or dermatitis. Visual similarity can be misleading, especially in early or partially treated cases.
2. We Assess the Full Clinical Pattern – We look at where the rash appears, whether it is symmetrical, how it feels, how long it has been present, and what triggers or relieves it. Your treatment history also provides important clues.
3. Response to Previous Treatment Matters – If a rash has not improved or has worsened with steroid creams, this raises suspicion of a fungal cause. Treatment response often tells us as much as appearance.
4. Investigations Are Used When Needed – Skin scrapings, microscopy, or occasionally a biopsy may be used to confirm the diagnosis. These tests help identify the exact cause rather than relying on guesswork.
This structured approach prevents unnecessary and ineffective treatment. By confirming the diagnosis before escalating care, we protect your skin from prolonged irritation and ensure you receive treatment that actually works.
Eczema Commonly Mistaken for Fungal Infection
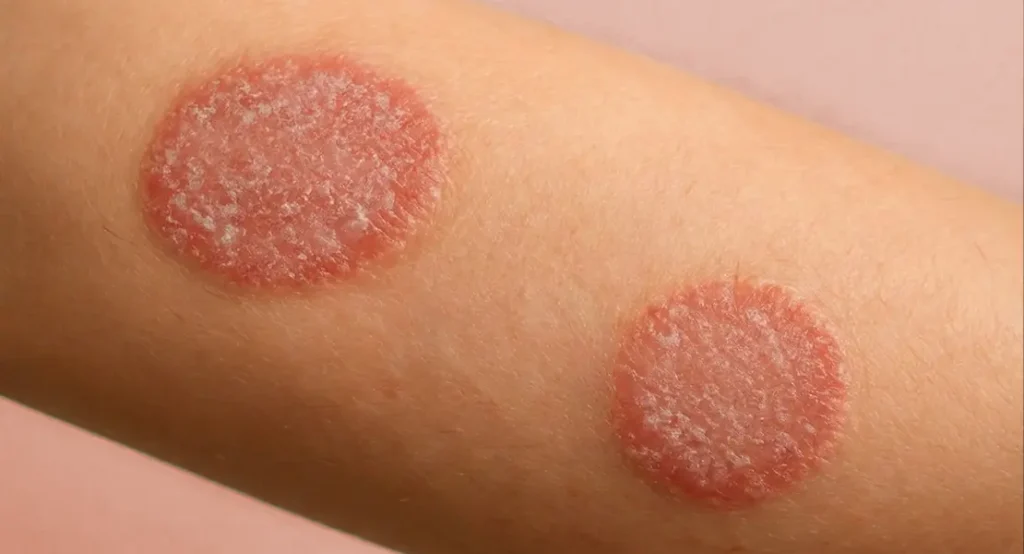
Eczema is one of the most commonly misdiagnosed skin conditions, particularly when it affects body folds or sensitive areas. Its redness, scaling, and itch can closely resemble fungal infection at first glance. When antifungal treatments are used incorrectly, symptoms often worsen rather than improve.
Eczema is often mistaken for fungal infection because:
- The appearance can look deceptively similar – Red, scaly, itchy patches with defined edges can closely mimic fungal rashes, especially in warm or moist areas.
- Body folds increase confusion – Areas such as the groin, underarms, or beneath the breasts are common sites for both eczema and fungal infection.
- Antifungal creams can worsen irritation – When eczema is treated as a fungal condition, the skin barrier may become more inflamed and uncomfortable.
- The treatment approach is completely different – Eczema requires anti-inflammatory care and barrier repair, not antifungal therapy.
By identifying eczema correctly from the outset, we can avoid unnecessary irritation and ensure you receive treatment that actually calms the skin and supports healing.Top of Form
Why Antifungals Aggravate Eczema
Eczema-prone skin already has a weakened protective barrier. We know this makes the skin more sensitive and reactive to topical treatments. When the barrier is compromised, even appropriate products can sometimes cause irritation.
Antifungal agents are designed to disrupt fungal cells, but they can also dry and irritate eczema-affected skin. We often see this increase inflammation, redness, and itch rather than improve symptoms. Instead of calming the skin, these treatments can make flares worse.
When symptoms worsen after antifungal use, it becomes an important diagnostic clue. We pay close attention to this response because it helps distinguish eczema from fungal conditions. Recognising this pattern allows us to adjust treatment correctly and restore skin balance.
Psoriasis That Mimics Fungal Disease
Psoriasis can sometimes look very similar to a fungal rash, especially in certain areas of the body. We often see this confusion in skin folds, where inverse psoriasis appears red, smooth, and shiny rather than scaly. This visual overlap makes misdiagnosis common.
Because inverse psoriasis lacks the classic thick scale, it is frequently mistaken for a fungal infection. You may notice that antifungal treatments fail to improve the rash or even make it more uncomfortable. We see this lack of response as an important clinical signal.
Psoriasis responds to anti-inflammatory treatment rather than antifungals. When we recognise this pattern, we can correct the treatment approach and reduce ongoing inflammation. Accurate identification helps us manage symptoms properly and prevent prolonged skin problems.
Top of Form
Bottom of Form
Seborrhoeic Dermatitis Confused With Fungal Infection
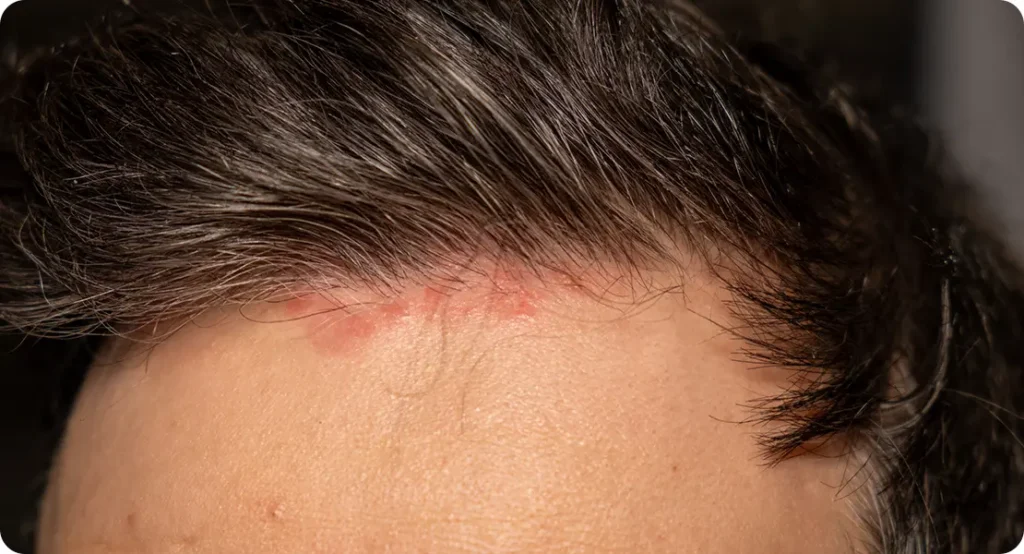
Seborrhoeic dermatitis is a very common condition that is often mistaken for a fungal infection. Because it causes redness and scaling in areas where yeast normally lives, the distinction can be confusing. Understanding the difference helps ensure treatment is effective rather than frustrating.
Here’s why confusion happens:
1. It Commonly Affects the Scalp, Face, and Chest – Seborrhoeic dermatitis typically appears in oily areas such as the scalp, eyebrows, sides of the nose, ears, and upper chest. These are also areas where fungal conditions can occur.
2. Redness and Greasy Scaling Look “Fungal” – The combination of redness and yellowish or greasy scale often resembles a fungal rash. Visually, it can be very difficult to tell the difference without proper assessment.
3. Yeast Plays a Role, but It Is Not an Infection – While yeast contributes to seborrhoeic dermatitis, it is not a simple infection that needs to be eradicated. The core problem is an inflammatory skin response rather than fungal overgrowth alone.
4. Management Focuses on Inflammation Control – Treatment aims to calm inflammation and reduce scaling, sometimes alongside antifungal ingredients. The goal is control, not complete elimination of yeast.
Mistaking seborrhoeic dermatitis for a fungal infection can lead to ineffective treatment and repeated flares. By focusing on inflammation control rather than eradication, we can manage symptoms more reliably and keep the condition stable over time.
Contact Dermatitis That Looks Like Fungus
Allergic and irritant contact dermatitis can closely resemble fungal rashes. We often see red, itchy, and well-defined patches that look convincing at first glance. This similarity makes misdiagnosis common, especially without careful assessment.
These reactions usually appear where the skin comes into contact with products, clothing, metals, or personal care items. You may notice the rash stays localised to one area and does not respond to antifungal treatment. We see this lack of improvement as an important clue.
Identifying and avoiding the trigger is essential for recovery. We focus on understanding what your skin has been exposed to rather than continuing ineffective treatment. Once the trigger is removed and inflammation is addressed, the skin is able to settle and heal properly.
Why Steroid-Modified Fungal Rashes Cause Confusion
Some antifungal creams also contain steroids, which can temporarily calm redness and itching. This short-term improvement can be misleading and make a rash appear to be responding to treatment. When the cream is stopped, symptoms often return or worsen, creating confusion.
Steroid-modified fungal rashes cause diagnostic difficulty because:
- Steroids suppress visible inflammation – Redness and itch may improve briefly, masking the true nature of the rash.
- The underlying infection is not cleared – While symptoms fade, the fungus can continue to grow beneath the surface.
- Rebound worsening occurs after stopping treatment – Once steroids are withdrawn, the rash often returns more aggressively.
- The clinical pattern becomes blurred – Altered appearance makes it harder to distinguish between fungal infection, eczema, or other inflammatory conditions.
This cycle can delay accurate diagnosis and appropriate treatment, which is why careful assessment is essential before combining or continuing therapies.
Granuloma Annulare Mistaken for Ringworm
Granuloma annulare often presents as ring-shaped lesions, which is why it is frequently mistaken for ringworm. We understand how convincing this appearance can be, especially when the rash forms a clear circular pattern. At first glance, it can easily lead to the wrong assumption.
Unlike fungal infections, the surface of granuloma annulare is usually smooth and lacks scaling. You may notice that antifungal treatments do not improve the area at all. We see this lack of response as an important diagnostic clue.
Granuloma annulare is an inflammatory condition, not an infection. This means it requires a very different treatment approach. Recognising this distinction early helps us avoid unnecessary treatments and manage the skin more effectively.
Top of Form
Bottom of Form
Pityriasis Rosea Often Confused With Fungal Rash
Pityriasis rosea is another condition that is commonly mistaken for a fungal infection. Its early appearance can be misleading, especially when the first patch looks very similar to ringworm. Knowing how this condition behaves helps avoid unnecessary and ineffective treatment.
Here’s why confusion occurs:
1. It Causes Scaly, Oval-Shaped Patches – Pityriasis rosea typically presents with oval, slightly scaly patches on the trunk and limbs. This shape and scaling can closely resemble fungal rashes at first glance.
2. The Herald Patch Mimics Ringworm – The condition often begins with a single larger patch known as a “herald patch.” This patch frequently looks like ringworm, which is why antifungal creams are often tried initially.
3. Antifungals Do Not Alter the Condition – Because pityriasis rosea is not a fungal infection, antifungal treatments do not change its course. Lack of response to treatment is often an important diagnostic clue.
4. The Condition Is Self-Limiting – Pityriasis rosea usually resolves on its own over several weeks. Treatment focuses on symptom relief rather than curing the rash itself.
Although it can look alarming, pityriasis rosea is generally harmless and temporary. By recognising its typical pattern and natural course, we can reassure you, avoid unnecessary medications, and focus on keeping the skin comfortable while it settles naturally.
Lichen Planus That Mimics Fungal Infection
Lichen planus can affect the skin, nails, and mucous membranes, and its appearance can be misleading. We often see purple-red, itchy lesions that are mistakenly labelled as fungal infections. This visual similarity can delay the right diagnosis.
Antifungal treatments do not help lichen planus and may leave symptoms unchanged or worse. When a rash fails to respond as expected, we treat this as an important clinical signal rather than persisting with the wrong therapy. Response to treatment matters as much as appearance.
Early diagnosis makes a real difference in symptom control. We focus on identifying inflammation and guiding appropriate care before discomfort becomes prolonged. Recognising lichen planus early helps you manage symptoms more effectively and avoid unnecessary treatments.
Intertrigo That Is Not Fungal
Intertrigo is a condition that affects skin folds, where warmth and moisture are easily trapped. While fungal infection can sometimes be present, it is often not the main cause of the problem. In many cases, inflammation and skin breakdown are the primary drivers.
Intertrigo is not always fungal because:
- Friction and moisture are the main triggers – Skin rubbing together in warm, damp areas leads to irritation and inflammation.
- Redness and soreness can occur without infection – The appearance may look concerning even when no fungus is present.
- Fungal overgrowth may be secondary – Infection can develop later, but it is not always the starting issue.
- Managing inflammation and moisture is essential – Reducing friction, keeping folds dry, and calming the skin are key to recovery.
By addressing the underlying causes rather than assuming infection, we can treat intertrigo more effectively and reduce recurrence.
Why Location Alone Is Misleading
Many people assume that rashes in certain areas must be fungal. We often hear this about the groin, feet, under the breasts, or the armpits. While fungal infections can occur there, they are not the only cause.
A range of non-fungal conditions also prefer warm, moist skin folds. Eczema, psoriasis, and contact dermatitis can all affect these areas and look very similar. We see location used as a shortcut far too often.
Location helps guide suspicion but never confirms a diagnosis. We always look at appearance, symptoms, response to treatment, and history together. This broader assessment prevents misdiagnosis and unnecessary treatment.
Why Long-Standing “Fungal” Rashes Deserve Review
True fungal infections usually show clear improvement within a few weeks of proper treatment. We become concerned when a rash labelled as fungal continues for months without meaningful change. Lack of response is often a sign that the diagnosis may be wrong.
When antifungal treatment does not work, continuing it rarely solves the problem. We see prolonged use sometimes worsen irritation or mask the real condition. This delay can make skin problems harder to manage over time.
Reassessment at this stage is essential. We review the diagnosis, consider alternative causes, and adjust treatment accordingly. Early review helps prevent chronic skin damage and unnecessary frustration.
How Over-The-Counter Treatment Masks Diagnosis
Over-the-counter antifungal treatments are widely available, which makes them an easy first choice when a rash appears. Many people start treating themselves before seeking advice, often with the best intentions. However, early self-treatment can change how the skin looks and make accurate diagnosis more difficult.
Over-the-counter treatment can mask diagnosis because:
- Self-treatment alters appearance – Creams may reduce redness or scaling temporarily, changing the visual clues we rely on.
- Partial improvement creates confusion – Symptoms may improve briefly without resolving the underlying condition.
- Delayed assessment blurs the clinical picture – By the time you’re seen, the rash may no longer show its original features.
- History becomes just as important as examination – We rely on understanding what you used, when you used it, and how the skin responded.
By considering both your treatment history and current appearance, we can work towards a clearer and more accurate diagnosis.
When Antifungal Treatment Actively Makes Things Worse
Antifungal treatments can actually worsen inflammatory skin conditions. We often see these products dry the skin and disrupt the protective barrier. In conditions like eczema or dermatitis, this leads to increased redness, itch, and flare-ups.
When symptoms worsen after starting antifungal treatment, it is a strong signal that the diagnosis may be incorrect. We treat this response as an important clinical clue rather than persisting with the same approach. Worsening is not something to ignore.
Recognising this pattern early allows us to reassess and correct treatment. By identifying the true cause, we can calm inflammation and support proper healing. Accurate diagnosis protects your skin from unnecessary damage and prolonged discomfort.
Why Testing Matters More Than Guesswork
Simple tests like skin scrapings and microscopy can quickly confirm or rule out a fungal infection. We use these tools because they provide objective answers rather than assumptions. Testing removes uncertainty early in the process.
Despite this, testing is often skipped in favour of guesswork. We see how this can lead to months of unnecessary or ineffective treatment. When treatment is based on assumption, skin problems are more likely to persist or worsen.
Objective confirmation makes a real difference. By testing first, we can target the right condition from the start. This saves you time, reduces frustration, and protects your skin from prolonged damage.
How Dermatologists Decide When to Test
Dermatologists don’t test every rash automatically. Decisions about investigation are guided by uncertainty and how the skin responds to initial treatment. This careful approach helps avoid unnecessary testing while still ensuring accuracy.
Testing is considered when:
- The appearance is atypical – If a rash does not fit a clear clinical pattern, further investigation helps clarify the diagnosis.
- Treatment fails to work as expected – Lack of improvement suggests the initial assumption may be incorrect.
- Symptoms evolve unexpectedly – Changes in behaviour or spread can signal the need for closer evaluation.
- Evidence is needed to guide care – Testing supports diagnosis based on facts rather than assumption.
By using targeted testing, we ensure diagnosis remains evidence-based and treatment is both appropriate and effective.
Why Self-Diagnosis Is So Unreliable
Online images often oversimplify skin disease. We know that many different conditions can look almost identical in photos, especially when lighting, angle, and skin tone vary. Visual comparison alone is rarely accurate.
Without proper context, misdiagnosis becomes very likely. Photos cannot show symptoms such as itch, pain, duration, or how the skin feels to touch. We see self-diagnosis delay effective treatment far too often.
Professional assessment considers far more than appearance. We evaluate history, symptoms, distribution, and response to treatment alongside examination. This broader view is what allows accurate diagnosis and safer care.
The Cost of Delayed Correct Diagnosis
When a skin condition is not diagnosed correctly or promptly, the impact goes beyond inconvenience. Delays often allow the condition to evolve, making symptoms more persistent and treatment more complex. This is why early clarity matters so much.
Here’s what can happen when diagnosis is delayed:
1. Symptoms Persist for Longer Than Necessary – Without the right diagnosis, treatments may not address the true cause. This can leave you dealing with ongoing itching, redness, or discomfort for far longer than needed.
2. Inflammation Can Intensify Over Time – Untreated or poorly treated inflammation tends to build rather than settle. As inflammation increases, flare-ups can become more frequent and harder to control.
3. Pigmentation and Barrier Damage May Develop – Prolonged inflammation increases the risk of post-inflammatory pigmentation and skin barrier breakdown. These secondary changes can linger even after the original condition improves.
4. Conditions Can Become Harder to Treat – The longer a condition remains uncontrolled, the more resistant it can become to treatment. What might have been simple to manage early on may later require stronger or longer-term therapy.
Early diagnosis helps us intervene before these complications develop. By identifying the problem clearly from the start, we can reduce symptoms sooner, protect the skin barrier, and improve long-term outcomes for your skin health.
When to Seek Specialist Advice
If a rash does not improve within two to three weeks of antifungal treatment, reassessment is essential. We see this as a clear signal that the original diagnosis may not be correct. Continuing the same treatment rarely leads to improvement.
Persistent itching, a spreading rash, or worsening symptoms should never be ignored. These changes suggest ongoing inflammation or an alternative condition that needs proper evaluation. We encourage you to seek review rather than waiting it out.
Specialist input helps identify the real cause and correct the treatment plan. Early expert guidance prevents unnecessary escalation and prolonged skin damage. The right assessment at the right time makes management far more effective.
Why Correct Diagnosis Protects Long-Term Skin Health
Your skin has a memory, especially when it comes to inflammation and irritation. Repeated flares or incorrect treatment can make the skin more reactive over time. Getting the diagnosis right early helps protect the skin’s long-term resilience.
Correct diagnosis matters because:
- Repeated inflammation leaves lasting impact – Ongoing irritation can weaken the skin barrier and increase sensitivity.
- Incorrect treatment increases relapse risk – Treating the wrong condition often leads to repeated flares rather than resolution.
- Targeted care calms the skin effectively – When treatment matches the diagnosis, inflammation settles more reliably.
- Skin resilience is preserved over time – Accurate management helps the skin recover and remain more stable in the long term.
By focusing on correct diagnosis rather than trial-and-error treatment, we help protect your skin’s health not just now, but for years to come.
How Expert Care Changes the Outcome
Expert care focuses on identifying the true cause rather than relying on assumptions. We look beyond surface appearance and consider history, symptoms, and behaviour of the skin over time. This approach helps avoid repeated trial-and-error treatment.
At The London Dermatology Centre, diagnosis is based on careful clinical evaluation and appropriate testing, not guesswork. We use objective evidence to guide decisions, which leads to faster recovery and fewer relapses. You benefit from clarity rather than uncertainty.
Accurate diagnosis is the foundation of effective dermatology. When the cause is correctly identified, treatment becomes targeted and predictable. This is how expert care changes outcomes and supports long-term skin stability.
FAQs:
1. Why are so many skin rashes incorrectly diagnosed as fungal infections?
Many skin conditions share visual features such as redness, scaling, itching, and defined borders, which makes fungal infection an easy assumption. In busy clinical or self-treatment settings, diagnosis is often made based on appearance alone without considering history, distribution, or testing. This shortcut increases the risk of misdiagnosis and delayed recovery.
2. How can I tell if my rash is not actually a fungal infection?
A key sign is lack of improvement after two to three weeks of appropriate antifungal treatment. If the rash worsens, spreads, becomes more inflamed, or feels more irritated with antifungal use, this often suggests an inflammatory condition rather than an infection. Persistent symptoms should always prompt reassessment.
3. Can antifungal creams make non-fungal skin conditions worse?
Yes, antifungal creams can aggravate conditions such as eczema, contact dermatitis, or psoriasis. These products may dry the skin, disrupt the barrier, and increase inflammation. When used on the wrong condition, they often intensify redness and itching rather than providing relief.
4. Why does eczema so often get mistaken for a fungal infection?
Eczema can appear red, scaly, itchy, and well defined, especially in body folds where fungal infections are common. This overlap in appearance leads to confusion. However, eczema is driven by inflammation and barrier dysfunction, not infection, which is why antifungal treatment usually fails or worsens symptoms.
5. Is it possible for psoriasis to look like a fungal rash?
Yes, certain forms of psoriasis, particularly inverse psoriasis in skin folds, can closely mimic fungal infections. These areas may appear smooth and red rather than scaly, which adds to diagnostic confusion. Failure to respond to antifungal treatment is often an important clue that psoriasis may be the true cause.
6. Why do rashes in the groin or skin folds get labelled as fungal so quickly?
Warm, moist areas are commonly associated with fungal infections, so rashes in these locations are often assumed to be infectious. However, eczema, psoriasis, contact dermatitis, and intertrigo frequently affect the same areas. Location alone is not diagnostic and should never be the sole basis for treatment.
7. What does it mean if a rash improves briefly and then comes back worse?
This pattern is often seen when creams containing steroids are used, sometimes unknowingly. Steroids can temporarily reduce redness and itching while allowing an underlying infection or inflammatory condition to persist. When treatment stops, symptoms may rebound more aggressively, making diagnosis harder.
8. Why don’t long-standing “fungal” rashes clear up properly?
True fungal infections usually show clear improvement within weeks when treated correctly. If a rash persists for months despite antifungal use, it strongly suggests an alternative diagnosis. Continuing ineffective treatment can prolong inflammation and make the skin more difficult to treat later.
9. When should testing be done instead of trying another cream?
Testing becomes important when the rash looks atypical, does not respond to treatment as expected, or keeps recurring. Simple investigations such as skin scrapings can quickly confirm or rule out fungal infection. Objective testing prevents prolonged trial-and-error treatment and unnecessary skin damage.
10. Why is early specialist review so important in suspected fungal rashes?
Early expert assessment helps identify the true cause before prolonged inflammation develops. Misdiagnosis can lead to ongoing discomfort, pigmentation changes, and barrier damage. Accurate diagnosis allows targeted treatment, faster improvement, and better long-term skin health.
Final Thoughts: Correct Diagnosis Is the Key to Lasting Skin Improvement
When a skin rash is mislabelled as fungal, treatment often fails not because the skin is stubborn, but because the diagnosis is wrong. Many inflammatory conditions closely mimic fungal infections, and continuing antifungal treatment in these cases can prolong irritation, worsen inflammation, and delay real improvement. In my experience, recognising when a rash is not behaving like a true fungal infection is often the turning point in effective care.
If a rash keeps returning, fails to respond to treatment, or worsens despite antifungal creams, assessment by a Dermatologist at the London Dermatology Centre can make all the difference. If you would like to book a consultation with one of our dermatologist, you can contact us at the London Dermatology Centre.
Reference:
1. Tinea incognito: Challenges in Diagnosis and Management, Journal of Clinical Medicine, 13(11), 3267. https://www.mdpi.com/2077-0383/13/11/3267
2. Tinea incognito caused by Microsporum spp. Mimicking Subacute Cutaneous Lupus Erythematosus, Journal of Fungi, 11(7), 530. https://www.mdpi.com/2309-608X/11/7/530
3. Misdiagnosed dermatophytosis, Journal of Infection, 4(2), 127–129. https://www.sciencedirect.com/science/article/abs/pii/S0163445382936829
4. Yadgar, R.J., Bhatia, N. & Friedman, A. (2017) Cutaneous fungal infections are commonly misdiagnosed: A survey‑based study, Journal of the American Academy of Dermatology, 76(3) https://pubmed.ncbi.nlm.nih.gov/27866820/
5. Fungal skin disorders: dermatophytes and Malassezia (Year) Fungal Biology Reviews (PMC article). https://pmc.ncbi.nlm.nih.gov/articles/PMC4109575/