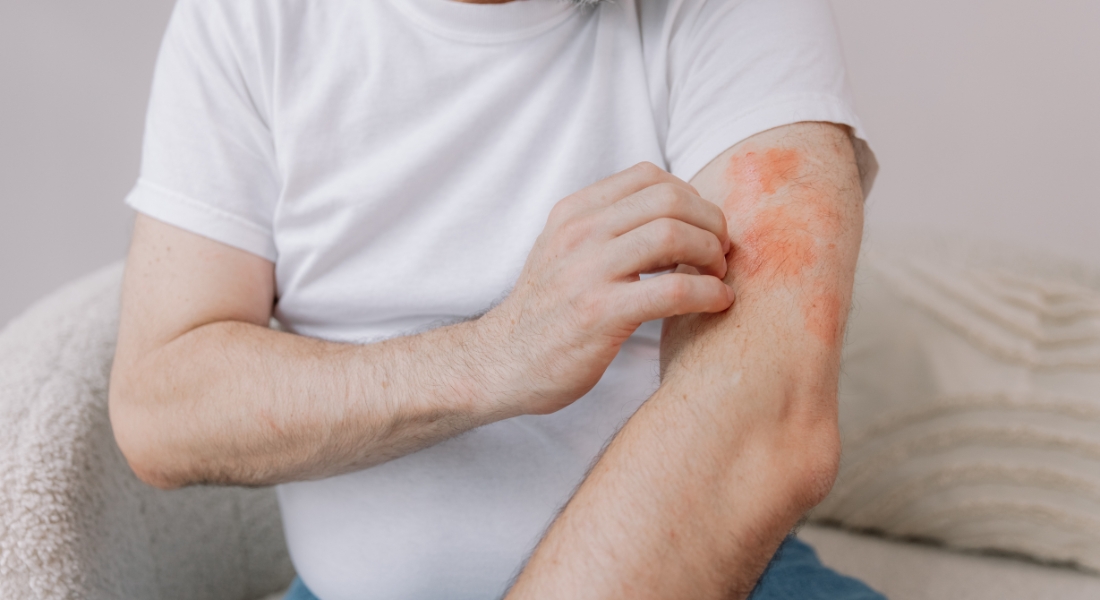
Skin irritation and skin inflammation are often used interchangeably, but they are not the same thing. If you have ever tried treating a skin problem that did not improve or worsened, misclassification may be the reason. Understanding the difference is essential for effective treatment.
Although both conditions can cause redness, discomfort, and sensitivity, they arise from different processes. Each requires a different management approach. Treating one as the other often leads to treatment failure.
In this article, we explain how irritation and inflammation differ, how dermatologists identify each, and why correct classification matters. Clear understanding helps you make better skincare and treatment decisions. Precision leads to better outcomes.
What Is Skin Irritation?
Skin irritation happens when your skin barrier is disrupted by an external trigger. This could be due to chemicals, friction, temperature changes, or even over-cleansing. Unlike allergic reactions, irritation is local and doesn’t involve the immune system.
When your skin barrier is compromised, it can’t protect itself as effectively. This leads to increased water loss and exposed nerve endings, which is why you may notice stinging, dryness, or a burning sensation. These symptoms are often uncomfortable but usually temporary.
In most cases, skin irritation is reversible once the trigger is removed. As your skin barrier repairs itself, the skin can recover naturally. Inflammation isn’t always present, which is why irritation often settles with gentle care and time.
What Is Skin Inflammation?
Skin inflammation is driven by your immune system rather than by simple surface damage. It happens when immune activity is triggered within the skin, often by infection, allergy, or an underlying skin condition. This makes it different from irritation, which doesn’t involve an immune response.
During inflammation, immune cells release chemical messengers that increase blood flow and draw more immune cells to the area. This is why you may notice redness, swelling, warmth, and itchiness. These signs are your body’s way of responding to a perceived threat.
Unlike irritation, inflammation can continue even after the original trigger has gone. It often needs targeted medical treatment to settle, as repairing the skin barrier alone is usually not enough.
Why These Two Conditions Are Commonly Confused

Skin irritation and inflammation can both cause redness and discomfort, which is why they’re often mistaken for the same problem. In mild cases, they can even look very similar, making it hard for you to tell the difference just by appearance.
To add to the confusion, many over-the-counter products use vague terms like “soothing” or “calming”. These labels don’t explain whether a product is addressing surface irritation or immune-driven inflammation, which can leave you guessing.
When you don’t understand what’s actually happening in your skin, treatment becomes a bit of trial and error. Guesswork can make symptoms worse rather than better, which is why correct identification is so important for your skin’s recovery.
How Dermatologists Distinguish Between Them
When you visit a dermatologist, they don’t just look at your skin they consider how it behaves over time. They’ll ask about when symptoms started, what triggers you’ve noticed, and how your skin reacts to different products. Recognising patterns in your skin’s response is a key part of figuring out what’s really happening.
Irritation often appears quickly after you come into contact with a trigger, such as a harsh cleanser or friction. In contrast, inflammation may develop more slowly or continue even when you’ve avoided the initial trigger. The duration and persistence of symptoms give your dermatologist important clues.
Your clinical history is just as important as what your skin looks like. How your skin reacts over days or weeks can reveal the underlying mechanism. This approach allows your dermatologist to make an accurate diagnosis and recommend the right treatment for you.
Quick Comparison: Irritation vs Inflammation:
| Feature | Skin Irritation | Skin Inflammation |
| Cause | External triggers (chemicals, friction, over-cleansing) | Immune response (infection, allergy, chronic skin disease) |
| Onset | Rapid, often immediately after exposure | Gradual or persistent, may continue after trigger is gone |
| Symptoms | Stinging, burning, dryness | Redness, swelling, heat, itch |
| Duration | Usually short-term; resolves when trigger removed | Can persist; may require medical treatment |
| Treatment | Gentle care, barrier repair | Targeted medical therapy, may need prescription products |
The Role of the Skin Barrier in Irritation
Your skin barrier acts like a protective shield, keeping irritants and environmental stressors out. When it’s intact, your skin can tolerate everyday exposures with little problem. But when the barrier is damaged, your skin becomes more sensitive and reacts more easily to triggers.
Irritation happens because your barrier has failed, not because your immune system is activated. Your skin reacts simply because it’s exposed and vulnerable. By repairing the barrier, you can restore your skin’s balance and reduce sensitivity.
This is why moisturisers and barrier creams are so effective if your skin is irritated. They work on the root cause rather than just masking symptoms. In most cases, anti-inflammatory medications aren’t necessary, as supporting the barrier is enough to help your skin recover.
The Immune System’s Role in Inflammation
Inflammation happens when your immune system is activated within the skin. Cells like T lymphocytes and mast cells start responding, which creates a sustained reaction. Unlike irritation, this is driven by your body’s defence mechanisms rather than surface damage.
Chemical messengers called inflammatory mediators amplify the response. They cause blood vessels to dilate and fluid to accumulate, which is why you may notice redness, swelling, or warmth. Over time, repeated inflammation can even lead to skin thickening in some conditions.
Because inflammation is immune-driven, simply repairing your skin barrier isn’t enough. In many cases, medical treatment is needed to calm the immune response. Targeted therapies help control symptoms and prevent long-term damage to your skin.
Symptoms That Suggest Irritation Rather Than Inflammation
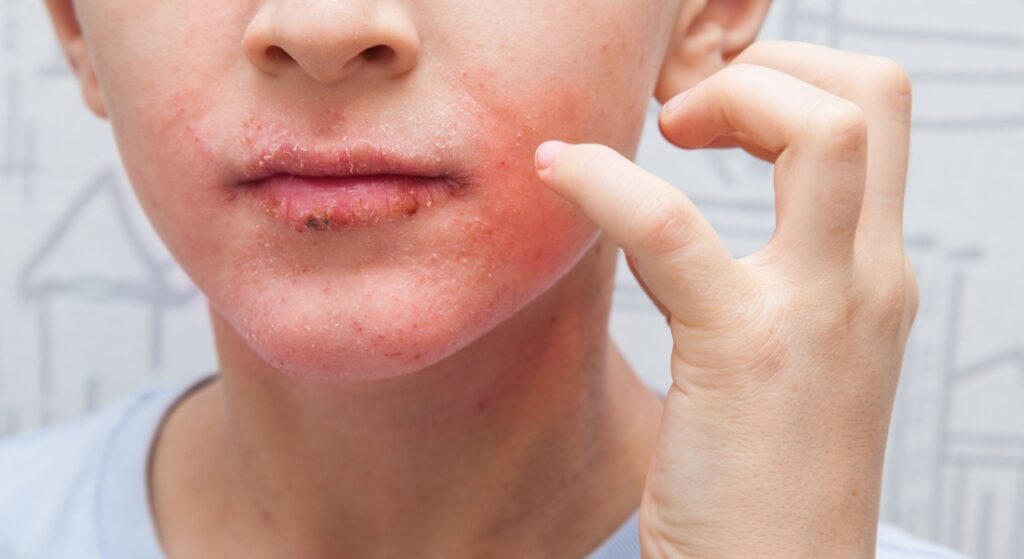
Not all reactions on the skin indicate true inflammation; some are simply a response to irritation. Irritation can occur from new products, environmental factors, or minor friction, and recognising it early helps prevent unnecessary worry or overtreatment.
Unlike inflammation, which may require medical intervention, irritation is usually temporary and resolves quickly once the trigger is removed. Being able to identify typical signs of irritation empowers you to care for your skin effectively and avoid further discomfort.
- Common signs of irritation: Stinging, burning, tightness, and dryness are typical symptoms. These often appear immediately after using a skincare product or exposure to a trigger.
- Visual cues without inflammation: The skin may look red, but there is usually no swelling, heat, or tenderness. Symptoms often improve quickly with gentle care and by removing the offending product or trigger.
- Short-lived flare-ups: Irritation tends to resolve as the skin barrier recovers. Episodes are generally brief, and normal skin function returns once the irritant is avoided.
Understanding these patterns helps distinguish minor irritation from more serious inflammatory conditions. Promptly addressing triggers and supporting the skin barrier ensures relief and prevents worsening.
Symptoms That Point to Inflammation
If your skin is inflamed, you’re more likely to notice itch rather than a stinging or burning sensation. Swelling and warmth may also appear, and redness tends to persist rather than fade quickly. These signs indicate that your immune system is active in your skin.
Symptoms can gradually worsen over time and usually don’t resolve just by stopping the products you’re using. Night-time itch is particularly common in inflammatory conditions, which can affect your sleep and comfort.
One of the biggest clues that inflammation is at play is chronicity. If your symptoms keep returning or lingering, it suggests immune involvement. In these cases, a medical assessment is recommended so you can get the right treatment.
Why Misclassification Leads to Treatment Failure
If your skin is irritated but you use strong anti-inflammatory products, you could actually make the barrier damage worse. Steroid creams, for example, may thin already fragile skin and make stinging, dryness, or sensitivity worse. This is why using the wrong treatment can escalate your symptoms instead of helping them.
On the other hand, if your skin inflammation is immune-driven and you only use moisturisers or barrier creams, it won’t be enough. The immune activity continues unchecked, which can cause redness, swelling, or thickening to persist or even worsen.
Getting the diagnosis right from the start is key to success. Using the correct approach prevents delays in improvement and helps you avoid frustration. Knowing whether your skin problem is irritation or inflammation guides the right treatment and speeds up recovery.
Common Conditions That Are Primarily Irritative
Many everyday skin issues are caused mainly by irritation rather than inflammation. These conditions often result from external triggers such as harsh products, over-exfoliation, or environmental exposure. Understanding that the cause is irritative helps guide simple, effective care rather than unnecessary medical treatments.
- Contact irritation from soaps and detergents: Frequent contact with harsh cleansers, household products, or fragranced soaps can strip the skin’s natural barrier. Redness, tightness, or mild stinging may occur, but these reactions usually resolve once the irritant is avoided.
- Over-exfoliation or aggressive skincare: Excessive use of physical scrubs or strong chemical exfoliants can damage the outer layer of the skin. This leads to temporary sensitivity, dryness, and stinging, which improves when exfoliation is paused and barrier support is provided.
- Environmental exposure: Wind, cold, or sun can irritate the skin, especially when the protective barrier is compromised. Simple protective measures, such as moisturisers or barrier creams, help the skin recover naturally.
- Barrier-focused care is usually sufficient: Avoidance of triggers and regular moisturisation are central to recovery. Medical treatments are rarely required, and minimal intervention often supports the best healing outcomes.
Recognising these common irritative conditions allows for effective self-care and faster recovery. Simple, consistent measures are often enough to restore healthy, comfortable skin.
Common Conditions That Are Inflammatory
Conditions like eczema, psoriasis, and allergic contact dermatitis are driven by inflammation in your skin. They involve immune system dysregulation, which is why symptoms often come back or persist over time. Unlike simple irritation, these conditions usually need more than just barrier repair to improve.
Managing these inflammatory conditions typically requires targeted therapy. Anti-inflammatory medications, such as topical corticosteroids or other prescription treatments, are commonly used to calm the immune response and reduce symptoms.
Repairing your skin barrier is still important, as it supports overall skin health and can make treatments more effective. However, barrier repair alone won’t control immune-driven inflammation. A combined strategy treating the immune response while supporting the barrier tends to give the best results for long-term skin health.
How Treatment Approaches Differ
If your skin is irritated, treatment focuses on protecting and repairing the barrier. Gentle cleansing, moisturising, and avoiding harsh ingredients are the main strategies. The goal is to reduce sensitivity and help your skin recover naturally.
When your skin is inflamed, the focus shifts to calming your immune system. Prescription treatments, such as topical anti-inflammatories or other targeted therapies, are often needed. Regular monitoring ensures the treatment is working and helps prevent flare-ups.
Using the wrong approach can slow down healing and even make symptoms worse. Aligning your treatment with the underlying condition whether irritation or inflammation is essential. Understanding this distinction really matters if you want your skin to recover effectively and stay healthy long-term.
The Risks of Over-Treating Irritated Skin

If your skin is already irritated, using strong active products can make sensitivity worse rather than better. These ingredients can further disrupt your skin barrier, leaving your skin more reactive and uncomfortable.
When this cycle repeats, recovery becomes slower and your skin may stay sensitive for longer. Over time, repeated damage can create a pattern of chronic irritation that is harder to manage.
Keeping your routine simple is often the most protective approach. Allowing your skin time to heal and focusing on gentle care helps restore balance. Exercising restraint with products can improve outcomes and prevent further frustration.
The Risks of Under-Treating Inflammation
Inflammation is the body’s natural response to injury or irritation, but when it is not treated appropriately, it can become harmful. Persistent inflammation keeps the immune system active in the affected area, potentially leading to long-term changes in skin structure and appearance. Understanding the risks emphasises why timely professional care is important.
- Chronic inflammation can damage the skin: Ongoing immune activity may cause thickening, scarring, or changes in pigmentation. Over time, the skin’s texture and tone can be permanently altered if inflammation persists untreated.
- Delayed treatment complicates recovery: When inflammation is left unmanaged, more aggressive therapies may be required later. Early intervention is usually simpler, less intensive, and more effective.
- Professional assessment ensures proper management: Consulting a dermatologist or skin professional helps identify the cause and determine the appropriate treatment. Correct timing and strategy reduce the risk of complications and support better long-term outcomes.
Ignoring inflammation or under-treating it can have lasting consequences. Prompt recognition and treatment protect both the skin’s health and appearance.
When Professional Assessment Is Important
If your symptoms persist or get worse despite home care, it’s time to seek professional evaluation. Reassessment helps your dermatologist recognise patterns and decide on the next steps for your skin.
A professional assessment clarifies the underlying cause and prevents unnecessary trial-and-error with products. Getting the right diagnosis ensures that your treatment is effective and targeted, whether your skin is irritated or inflamed.
Early input from a specialist can make a big difference in how quickly your skin improves. Delaying assessment may allow symptoms to become more complex or harder to manage. Expert guidance supports your recovery and helps you maintain healthier, more resilient skin.
How Understanding the Difference Empowers You
When you know whether your skin is irritated or inflamed, it changes how you respond and the choices you make. You can avoid treatments that might do more harm than good, and you’ll feel more confident in your decisions.
Understanding the difference also helps prevent the overuse of products and supports more realistic expectations about healing. This knowledge can reduce anxiety and help you feel more in control of your skin’s recovery.
Patients who are empowered in this way tend to experience better outcomes. Having clarity about your condition gives you a sense of control and allows you to take precise, effective steps toward healthier skin.
FAQs:
1. How can you tell if your skin problem is irritation or inflammation?
We usually look at how your skin behaves over time. Irritation tends to appear quickly after exposure to a trigger such as a product, friction, or weather changes, and often improves once that trigger is removed. Inflammation, on the other hand, often persists or worsens gradually and does not settle simply by stopping products, which suggests immune involvement.
2. Can skin irritation turn into inflammation if it is ignored?
Yes, it can. We see that repeated or ongoing irritation can weaken the skin barrier for long periods, making the skin more vulnerable to immune activation. When this happens, what began as irritation may progress into true inflammation, which is why early and appropriate management is important.
3. Does redness always mean your skin is inflamed?
No, redness alone does not always indicate inflammation. We often see redness in irritated skin due to barrier disruption and increased sensitivity. The difference lies in how long the redness lasts and whether it is accompanied by swelling, warmth, or itch, which are more typical of inflammation.
4. Why do anti-inflammatory creams sometimes make your skin feel worse?
When the underlying issue is irritation rather than inflammation, anti-inflammatory treatments may further disrupt an already fragile skin barrier. We find this can increase sensitivity and delay recovery, which is why correct classification is essential before starting treatment.
5. Can moisturisers alone treat skin inflammation?
Moisturisers are helpful, but they are usually not enough on their own to treat inflammation. We use them to support the skin barrier, but inflammation involves immune activity that often requires targeted medical treatment. Both approaches are important, but they serve different purposes.
6. Will irritated skin always settle by itself?
In many cases, irritated skin improves once the trigger is removed and the barrier is allowed to repair. However, we see delayed recovery when irritation is ongoing or when the skin is over-treated. Gentle care and avoidance are key to helping the skin heal properly.
7. Why does inflamed skin often itch more than irritated skin?
Itch is closely linked to immune signalling within the skin. In inflammation, immune cells release substances that stimulate itch pathways. Irritation more commonly causes burning, stinging, or tightness rather than persistent itch.
8. Can over-cleansing cause irritation without inflammation?
Yes, it can. We frequently see irritation caused by excessive or harsh cleansing that strips the skin barrier without triggering the immune system. This leads to dryness, sensitivity, and discomfort, which usually improve once cleansing is simplified and barrier repair is prioritised.
9. When should you seek professional assessment for skin symptoms?
If your symptoms persist, worsen, or keep returning despite gentle care, we recommend professional assessment. A dermatologist can determine whether irritation or inflammation is present and guide appropriate treatment, helping you avoid unnecessary trial and error.
10. Why does correctly identifying irritation versus inflammation matter so much?
Correct identification allows us to match treatment to the underlying problem. Irritation requires protection and repair, while inflammation requires immune control. When the wrong approach is used, improvement is delayed and symptoms may worsen, which is why accurate diagnosis is central to successful skin care.
Final Thought: Why Getting the Right Diagnosis Matters for Your Skin
Understanding whether your skin is irritated or inflamed makes a real difference to how well treatment works. When the underlying cause is identified correctly, we can focus on the right approach, whether that means restoring the skin barrier or addressing immune-driven inflammation. This clarity helps prevent unnecessary treatments, reduces frustration, and supports healthier long-term outcomes for your skin.
If your symptoms are persistent, worsening, or difficult to interpret, speaking with an experienced Dermatologist at the London Dermatology Centre can provide clarity and reassurance. We take the time to assess your skin properly and guide you towards treatment that is appropriate for your specific condition. You can book a consultation with one of our dermatologists by contacting us at the London Dermatology Centre.
References:
1. Baker, P., et al. (2023) Skin Barrier Function: The Interplay of Physical, Chemical, and Immunologic Properties, Cells, 12(23), 2745. https://www.mdpi.com/2073-4409/12/23/2745
2. Lin, T.-K., Zhong, L. and Santiago, J.L. (2018) Anti-Inflammatory and Skin Barrier Repair Effects of Topical Application of Some Plant Oils, International Journal of Molecular Sciences, 19(1), 70. https://www.mdpi.com/1422-0067/19/1/70
3. Yang, G., et al. (2020) Skin Barrier Abnormalities and Immune Dysfunction in Atopic Dermatitis, International Journal of Molecular Sciences, 21(8), 2867. https://pubmed.ncbi.nlm.nih.gov/32326002/
4. Extended Panel (Example): Exploring the Complexities of Atopic Dermatitis: Pathophysiological Mechanisms and Therapeutic Approaches, https://pubmed.ncbi.nlm.nih.gov/39119011/
5. Schmuth, M., et al. (2024) Skin Barrier in Atopic Dermatitis, Journal of Investigative Dermatology, Elsevier. https://www.sciencedirect.com/science/article/pii/S0022202X24001878