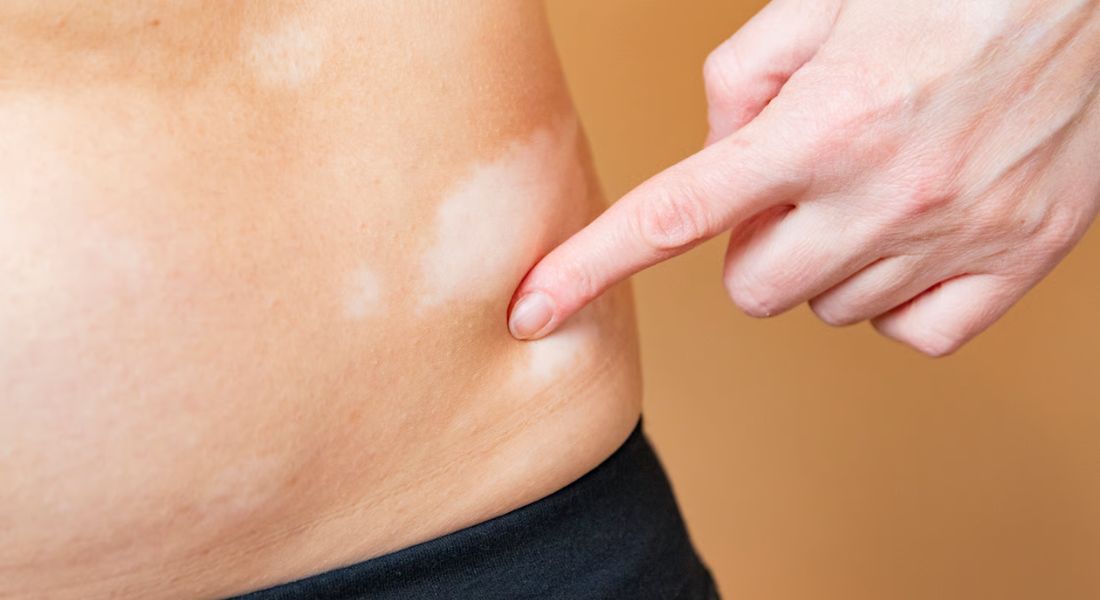
If you’re living with vitiligo, one of the most important questions you may ask is whether it is still spreading or has stabilised. This uncertainty can feel frustrating and difficult to manage in your daily life. You might notice new patches appearing, or you may see no changes for months. Either way, it can leave you unsure about what is really happening with your skin.
Understanding whether your vitiligo is active or stable is not just a medical detail. It plays an important role in deciding which treatments may be suitable for you. It also affects how effective those treatments are likely to be over time. Having this clarity can help you feel more in control of your condition.
Dermatologists use a range of methods to assess whether vitiligo is active or stable. They will look at changes in your skin, review your medical history, and may use specific tools to track progression. These assessments help them understand how your condition is behaving. As a result, they can recommend the most appropriate treatment plan for you.
In this guide, you will learn how dermatologists determine vitiligo stability in a clear and practical way. You will also discover the signs you can look for yourself at home. This can help you better understand what changes in your skin may mean. By the end, you should feel more confident in recognising whether your vitiligo is active or stable.
What Does “Vitiligo Stability” Actually Mean?
To begin with, it is important to understand the basics of vitiligo stability. When dermatologists describe vitiligo as “stable”, they mean that the condition has stopped progressing. This means you are not developing new patches, and the existing areas are not increasing in size. In simple terms, your skin is no longer changing in the way it did before.
Active vitiligo, by contrast, means the condition is still evolving. You may notice new areas of depigmentation appearing over time. In some cases, patches you already have may gradually become larger. This ongoing change is what doctors refer to as active disease.
This distinction is very important when it comes to your treatment. Different therapies are recommended depending on whether your vitiligo is active or stable. Some treatments work best during the active stage, while others are only suitable once the condition has stabilised. Understanding this can help you make more informed decisions about your care.
Why Stability Matters for Treatment
You might wonder why dermatologists place so much importance on whether your vitiligo is stable or active. The reason is quite simple, as effective treatment depends heavily on timing. If your condition is still active, the main goal is usually to slow down or stop its progression. This is often done using medical therapies that help control the immune response.
Once your vitiligo becomes stable, the focus of treatment begins to change. At this stage, the aim is often to restore pigment to the affected areas of your skin. You may be offered treatments that are designed to improve the appearance of existing patches. These approaches are generally more effective when the condition is no longer spreading.
For example, procedures such as skin grafting or melanocyte transplantation are usually only considered when vitiligo is stable. This is because carrying out these treatments during the active stage can lead to poor or short-lived results. If you are considering specialised care, such as vitiligo treatment in London, assessing stability will be one of the first steps in your consultation.
How Dermatologists Define Stability
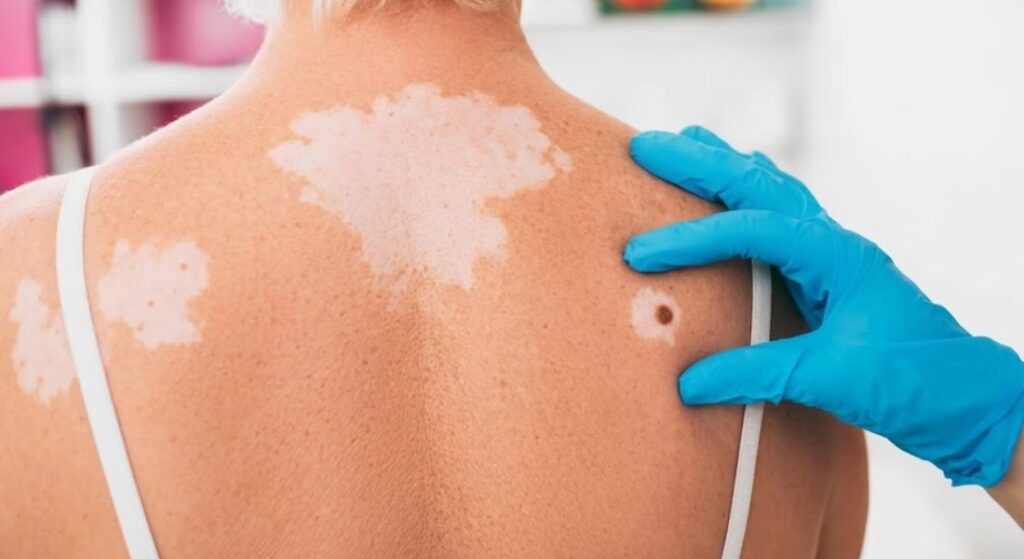
You might assume there’s a simple test to confirm whether vitiligo is stable, but the reality is more complex. Dermatologists rely on a combination of time, clinical observation, and patient history rather than a single diagnostic method. Stability is assessed carefully to ensure the condition is no longer progressing. This detailed evaluation helps guide appropriate treatment decisions and improve outcomes.
- Absence of New Lesions: One of the primary indicators of stability is that no new white patches have appeared over a specific period. This suggests that the condition is not actively spreading. Dermatologists closely monitor this aspect during follow-up visits.
- No Progression of Existing Patches: Stability also means that existing vitiligo patches have not increased in size or changed in shape. Consistency in the appearance of lesions over time indicates that disease activity has slowed or stopped. This is a crucial factor in determining readiness for certain treatments.
- Time-Based Benchmark: A commonly used guideline is a period of 6 to 12 months without any noticeable changes. However, this timeframe can vary depending on the individual’s condition and medical history. Some specialists may recommend a longer observation period before confirming stability.
- Individual Clinical Assessment: Dermatologists often consider additional factors such as disease pattern, past activity, and response to previous treatments. Each case is unique, and stability is not defined by time alone. A thorough clinical assessment ensures a more accurate and personalised evaluation.
Defining stability in vitiligo is not based on a single test but rather a careful combination of observation and time. Dermatologists look for consistent signs such as no new lesions and no progression of existing patches over several months. While general benchmarks exist, individual factors always play a role in the final assessment. This personalised approach ensures that treatment decisions are both safe and effective.
Key Signs That Vitiligo Is Active
To understand whether your vitiligo is still active, it helps to recognise the common signs. One of the clearest indicators is the appearance of new white patches on your skin. If you are noticing fresh areas of depigmentation, it usually means the condition is still progressing. This ongoing change suggests that your vitiligo has not yet stabilised.
Another sign to look out for is the enlargement of existing patches. Even small or gradual increases in size can point to continued activity. You might also notice that the edges of your patches appear less defined or are spreading outwards. These changes can indicate that the condition is still evolving beneath the surface.
In some cases, you may see redness or mild inflammation around the affected areas. This can be a sign of an active immune response in your skin. You might also notice that the hair within these patches starts to lose its colour, a process known as leukotrichia. If you observe any of these changes, it is important to take them seriously as they provide useful clues about your condition.
Signs That Vitiligo May Be Stable
Now it is helpful to look at the signs that suggest your vitiligo may be stable. Stable vitiligo usually shows very little change over time. The patches tend to remain the same size, shape and distribution across your skin. You will also notice that no new areas are appearing.
Another important feature of stability is that existing patches are not spreading. The borders of these patches often become more clearly defined and look more uniform. They may appear less irregular compared to when the condition was active. These visual changes can indicate that the condition has settled.
In some cases, you might notice slight repigmentation within the patches. This can occur naturally or as a result of treatment you are using. You are also unlikely to see redness or inflammation, as stable vitiligo usually appears calm and unchanged. However, it is important to remember that stability does not always mean improvement, only that the condition is not currently progressing.
The Role of Medical History
Dermatologists do not rely on visual examination alone when assessing your vitiligo. Your medical history plays an important role in determining whether the condition is stable or active. You will usually be asked when your vitiligo first appeared and how it has developed over time. This information helps build a clearer picture of your condition.
You may also be asked whether you have noticed any new patches recently. Questions often focus on whether existing areas have grown or remained the same. These details allow dermatologists to understand if there has been any recent progression. Your answers provide valuable insight that cannot be seen through examination alone.
In addition, dermatologists may ask about possible triggers that could influence vitiligo activity. Factors such as stress, illness or skin injury can sometimes play a role. By putting together a timeline of these changes and events, they can better understand the pattern of your condition. This helps them make a more accurate and informed assessment.
Clinical Examination Techniques
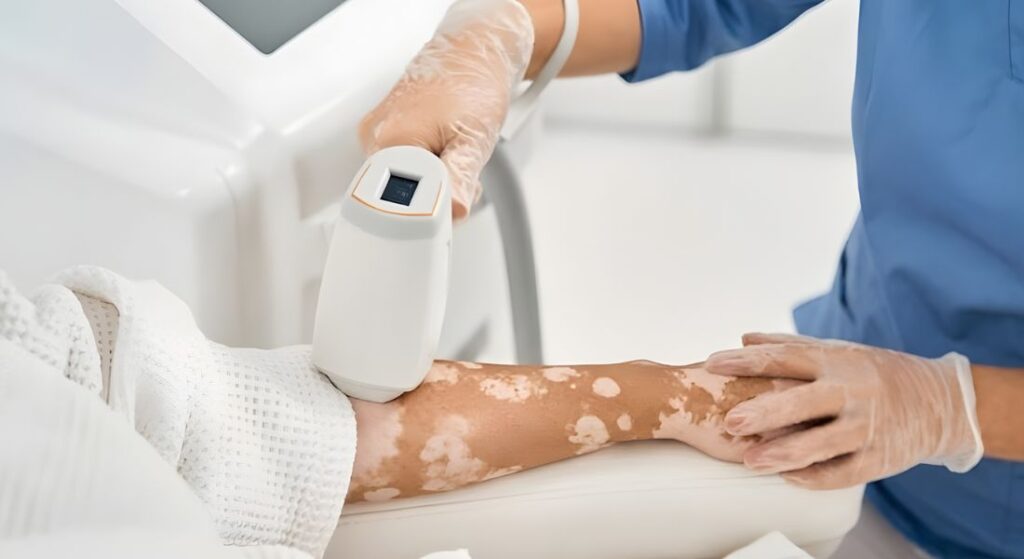
A thorough skin examination is a key step in assessing vitiligo and determining its activity. Dermatologists take a detailed and methodical approach to evaluate visible and subtle changes across the skin. This process goes beyond what may be noticeable to the patient, ensuring nothing important is missed. A comprehensive clinical assessment helps build an accurate understanding of the condition.
- Assessment of Patch Characteristics: Dermatologists carefully examine the size, shape, and distribution of vitiligo patches across the body. This helps identify patterns and determine whether the condition is stable or progressing. Even minor variations can provide important diagnostic clues.
- Evaluation of Lesion Borders: Special attention is given to the edges of the patches, as they can indicate disease activity. Active vitiligo often presents with blurred or expanding borders, suggesting ongoing progression. Well-defined edges, on the other hand, may point toward stability.
- Examination of Less Visible Areas: Certain areas such as the scalp, lips, and genital region are also closely inspected. These regions are commonly affected but can be easily overlooked without a detailed check. Examining these areas ensures a more complete evaluation of the condition.
- Detection of Subtle Changes: Dermatologists look for small or gradual changes that may not be obvious to the patient. These subtle signs can indicate early activity or progression. Identifying them early helps guide timely and appropriate treatment decisions.
Clinical examination techniques play a vital role in understanding the true extent of vitiligo. By carefully evaluating patch characteristics, lesion borders, and less visible areas, dermatologists can detect both obvious and subtle signs of activity. This detailed approach ensures that no aspect of the condition is overlooked. Ultimately, a comprehensive examination leads to more accurate diagnosis and better-informed treatment planning.
Wood’s Lamp Examination
One of the most useful tools your dermatologist may use is the Wood’s lamp. This device emits ultraviolet light, which makes depigmented areas of your skin more visible. Under this light, vitiligo patches appear bright white and stand out clearly. This allows your doctor to see changes that may not be noticeable in normal lighting.
This examination is especially helpful for detecting early or subtle changes in your skin. It can reveal small areas of depigmentation that you might not have noticed yourself. By identifying these areas, your dermatologist can better understand how your condition is developing. This can be important when assessing whether your vitiligo is active.
The Wood’s lamp can also help your dermatologist examine the borders of your patches more closely. Stable patches tend to have clear and well-defined edges, while active ones may look less defined or spreading. Although this tool does not directly measure activity, it provides valuable supporting information. This helps your dermatologist make a more accurate assessment of your condition.
Dermoscopy in Vitiligo Assessment
Dermoscopy is another technique your dermatologist may use when evaluating vitiligo. This involves a specialised magnifying device that allows a close and detailed examination of your skin. It helps reveal patterns and features that are not visible to the naked eye. This added detail can provide important clues about the condition of your skin.
In vitiligo, dermoscopy can highlight specific features linked to activity. These may include changes such as perifollicular depigmentation or irregular patch borders. It can also help identify early signs of repigmentation within affected areas. For example, you might see small dots of pigment forming around hair follicles.
This level of detailed observation helps your dermatologist refine the diagnosis. It provides a clearer understanding of whether your vitiligo is active or stable. By combining this with other assessment methods, a more accurate picture of your condition can be formed. This ultimately supports better treatment decisions.
Monitoring Over Time
One of the most reliable ways to determine whether your vitiligo is stable is through regular follow-up. Dermatologists often monitor your condition over several months to observe any changes. This ongoing assessment helps them track progression in a structured and objective way. It also provides a clearer picture than relying on a single visit.
Photographic documentation is commonly used as part of this process. Images of your skin are taken at regular intervals and compared over time. This makes it easier to identify even small or gradual changes that you might not notice yourself. It also removes much of the guesswork from the assessment.
If no visible changes are observed over a consistent period, your vitiligo may be considered stable. However, this conclusion is only made after careful and repeated monitoring. Stability is not determined quickly, but through clear evidence over time. This approach ensures that any treatment decisions are based on accurate information.
The Importance of Patient Self-Observation
You play an important role in assessing your vitiligo as well. No one sees your skin as regularly as you do in your daily life. This puts you in a unique position to notice even small or early changes. Your awareness can provide valuable information that supports medical evaluation.
Keeping track of new patches or changes in existing ones can be very helpful. Even subtle differences in size, shape or colour may be important. Some people find it useful to take regular photos to monitor their skin over time. This can make it easier for you to compare changes clearly and accurately.
If you notice anything unusual or different, it is always worth mentioning it to your dermatologist. Your observations can help guide their clinical assessment and decision-making. By sharing what you see, you contribute to a more complete understanding of your condition. This combined approach can lead to better and more effective care.
Triggers That May Indicate Activity
Certain triggers can suggest that your vitiligo may be more active. One of the most recognised is skin injury, which can lead to new patches forming. This is known as the Koebner effect, where trauma to the skin triggers depigmentation. Even minor injuries can sometimes have this effect.
Stress is another factor that is often linked to changes in vitiligo activity. While the exact connection is not fully understood, it may influence how the condition behaves. You might notice changes during or after periods of emotional or physical stress. This makes it an important factor to be aware of in your daily life.
Illness or hormonal changes may also play a role in triggering activity. These factors can sometimes coincide with flare-ups or new developments in your skin. If you have experienced any of these recently, it is worth discussing them with your dermatologist. They can provide useful context and help guide your overall assessment and care.
Laboratory Tests and Their Role
Unlike some medical conditions, vitiligo does not have a specific blood test to determine whether it is active or stable. However, laboratory tests can still play an important supporting role in patient evaluation. Dermatologists often use these tests to identify underlying or associated health issues. This broader approach helps ensure that all aspects of a patient’s health are considered during management.
- Screening for Autoimmune Conditions: Vitiligo is often associated with other autoimmune disorders, so tests may be conducted to detect these conditions. Identifying any underlying issues allows for more comprehensive care. This is particularly important for long-term health monitoring.
- Thyroid Function Testing: Thyroid tests are commonly recommended due to the known link between vitiligo and thyroid disorders. Abnormal thyroid function can impact overall health and may influence treatment decisions. Detecting these issues early allows for timely intervention.
- Supporting Overall Assessment: While lab tests do not determine vitiligo stability, they provide valuable background information. This helps dermatologists understand the patient’s overall health status. A well-rounded assessment supports more informed clinical decisions.
- Guiding Long-Term Management: Results from laboratory tests can influence ongoing care and monitoring strategies. Managing associated conditions alongside vitiligo can improve overall outcomes. This integrated approach ensures more effective and personalised treatment.
Although laboratory tests cannot directly confirm whether vitiligo is stable, they still play a crucial role in patient care. By identifying associated autoimmune conditions and assessing overall health, these tests add valuable context to the clinical evaluation. Dermatologists use this information to guide more comprehensive and personalised management plans. Ultimately, a holistic approach leads to better long-term outcomes for patients.
Psychological Impact of Uncertainty
Waiting to see whether your vitiligo stabilises can feel challenging and uncertain. Not knowing what will happen next may affect your confidence in everyday situations. You might feel unsure about starting treatments or making decisions about your care. This uncertainty can be difficult to manage over time.
Skin conditions like vitiligo often have a visible impact, which can add emotional pressure. You may become more aware of changes in your appearance and how others might perceive them. This can sometimes lead to hesitation or self-doubt. These feelings are completely understandable and commonly experienced.
Understanding whether your vitiligo is active or stable can provide a sense of clarity. It allows you to move forward with more confidence when considering treatment options. A proper assessment helps you make informed decisions based on your condition. It is not only about managing your skin, but also about improving your peace of mind.
Treatment Options for Active Vitiligo
When your vitiligo is active, the main focus of treatment is to slow down or stop its progression. At this stage, your dermatologist will usually aim to control the underlying immune response. This helps prevent new patches from forming and existing ones from spreading further. Early intervention can make a meaningful difference in managing the condition.
Topical corticosteroids are commonly prescribed to help reduce inflammation in the skin. These treatments work by calming the immune activity that contributes to depigmentation. Calcineurin inhibitors may also be recommended, especially for more sensitive areas such as your face. These options can be effective while being gentler on delicate skin.
Light therapy, particularly narrowband UVB, is another widely used approach. This treatment can help stabilise your vitiligo while also encouraging some degree of repigmentation. It is often carried out over a period of time under medical supervision. At this stage, the primary goal is control, with stopping the spread being the top priority.
Treatment Options for Stable Vitiligo
Once your vitiligo is stable, a wider range of treatment options may become available to you. At this stage, the focus often shifts towards restoring pigment in the affected areas. Your dermatologist may discuss approaches that aim to improve the appearance of your skin. Stability is important because these treatments tend to work best when the condition is no longer spreading.
Surgical procedures may be considered as part of your treatment plan. Techniques such as skin grafting involve transferring pigment-producing cells to areas of depigmentation. These methods require a stable condition to achieve reliable and lasting results. They are usually recommended only after careful assessment by a specialist.
In addition, laser treatments and other advanced therapies may be used to support repigmentation. These options aim to stimulate melanocyte activity within the skin. If you are exploring specialist care, such as vitiligo treatment in London, this is often the stage where more advanced treatments are discussed. This allows for a more targeted approach based on your condition.
Why Timing Matters So Much
Starting the right treatment at the right time can make a significant difference to your results. If you begin repigmentation treatments too early, the outcomes may not last as expected. This is because active vitiligo can quickly reverse any progress made. Ensuring the timing is correct helps protect the effectiveness of your treatment.
When vitiligo is still active, the priority is to control the condition before focusing on restoring pigment. Beginning advanced treatments too soon may lead to disappointing or short-lived results. This is why dermatologists carefully assess whether your condition has stabilised first. Taking the right approach at the correct stage can improve long-term outcomes.
On the other hand, delaying treatment longer than necessary can also feel frustrating. Waiting without clear guidance may leave you unsure about your next steps. This is why an accurate assessment is so important for your care. It ensures that each decision you make is appropriate and increases your chances of success.
Can Vitiligo Become Stable Permanently?
This is a common question, and the answer is not always straightforward. Some people experience long periods where their vitiligo remains stable. In these cases, the condition may stay unchanged for many years. This can provide a sense of consistency and reassurance in managing your skin.
However, vitiligo does not behave the same way for everyone. You may go through cycles, with periods of stability followed by renewed activity. New patches can sometimes appear after a long time without change. This unpredictability is a natural part of the condition.
Regular monitoring can help you manage this uncertainty more effectively. Keeping track of any changes allows your dermatologist to respond at the right time. Adjustments to your treatment can be made if the condition becomes active again. This approach helps you stay in control of your care over the long term.
Lifestyle Factors That May Support Stability
While vitiligo cannot be completely prevented, certain lifestyle habits may help support stability and reduce the risk of progression. Dermatologists often encourage patients to adopt protective and health-conscious routines as part of overall care. These measures do not cure the condition but can complement medical treatment. Over time, consistent habits may contribute to better skin health and improved disease control.
- Protecting the Skin from Injury: Avoiding cuts, burns, and friction is important, as skin trauma can trigger new vitiligo patches. This phenomenon, known as the Koebner response, highlights how sensitive affected skin can be. Taking simple precautions in daily activities can reduce this risk.
- Practicing Sun Protection: Using sunscreen and protective clothing helps shield the skin from harmful UV exposure. Sun protection also reduces the contrast between depigmented and normal skin, making patches less noticeable. Consistent protection supports overall skin health.
- Managing Stress Levels: Stress is believed to play a role in triggering or worsening vitiligo in some individuals. While it is not a direct cause, managing stress through relaxation techniques or lifestyle changes may help reduce flare-ups. A calmer mind can contribute to overall well-being.
- Maintaining a Balanced Lifestyle: A healthy diet, regular exercise, and adequate sleep all support the body’s immune system. While these factors do not directly treat vitiligo, they create a foundation for better overall health. This can positively influence how the condition behaves over time.
Lifestyle choices can play a supportive role in managing vitiligo and promoting stability. By protecting the skin, practicing sun safety, and maintaining overall well-being, individuals can help reduce potential triggers. Although these steps are not a substitute for medical treatment, they are valuable additions to a comprehensive care plan. Over time, a balanced lifestyle may contribute to more stable and manageable skin changes.
When to Seek Professional Advice

If you are unsure about any changes in your skin, it is important not to wait. Seeking an early assessment can give you much-needed clarity about your condition. It also helps ensure that the right treatment plan is put in place at the appropriate time. Acting early can make managing vitiligo more straightforward and effective.
You should consider seeking professional advice if you notice new patches developing. It is also important to get checked if existing patches appear to be changing in size, shape or colour. These signs may indicate that your vitiligo is active and needs closer attention. A dermatologist can assess these changes accurately and guide your next steps.
Even if your vitiligo appears stable, a professional review can still be very valuable. It can confirm whether what you are seeing is accurate and provide reassurance. Regular check-ups help ensure that your condition is being monitored properly. Taking this step can make a meaningful difference in how confidently you manage your vitiligo.
FAQs:
1. How can I tell if my vitiligo is stable or still active?
You can look for signs such as whether new patches are appearing or existing ones are growing. If there have been no changes for several months, your vitiligo may be stable. However, a dermatologist’s assessment is the most reliable way to confirm this.
2. How long does vitiligo need to remain unchanged to be considered stable?
In most cases, dermatologists consider vitiligo stable if there are no new patches or changes for 6 to 12 months. This timeframe may vary depending on individual circumstances.
3. Can vitiligo become active again after being stable?
Yes, vitiligo can become active again even after a long stable period. Triggers such as stress, illness, or skin injury may lead to new patches forming.
4. Why is it important to know whether vitiligo is stable?
Knowing whether vitiligo is stable helps determine the most suitable treatment. Some treatments are only effective or safe when the condition is no longer progressing.
5. What are the early signs of active vitiligo?
Early signs include new white patches, enlargement of existing patches, blurred edges, and sometimes mild redness or inflammation around affected areas.
6. Can stress cause vitiligo to spread?
Stress is not a direct cause, but it may act as a trigger in some people. It can potentially influence disease activity and contribute to flare-ups.
7. What tests do dermatologists use to assess vitiligo stability?
Dermatologists rely on clinical examination, medical history, and tools like Wood’s lamp or dermoscopy. There is no single test that definitively determines stability.
8. Is there a cure for vitiligo once it becomes stable?
There is currently no complete cure for vitiligo. However, when stable, treatments can help restore pigment and improve the appearance of the skin.
9. Can lifestyle changes help keep vitiligo stable?
Yes, protecting your skin from injury, managing stress, using sun protection, and maintaining overall health may help support stability and reduce triggers.
10. When should I see a dermatologist about my vitiligo?
You should seek medical advice if you notice new patches, changes in existing ones, or if you are unsure whether your condition is stable. Regular check-ups are also recommended for ongoing monitoring.
Final Thoughts: Gaining Clarity and Taking Control
Understanding whether your vitiligo is active or stable can make a significant difference in how you approach your care. While the condition can feel unpredictable at times, recognising the key signs and seeking professional guidance allows you to make informed decisions with greater confidence. Stability is not just a medical label it’s a crucial step in identifying the most effective treatment path for your skin.
By combining your own observations with expert assessment, you can build a clearer picture of how your vitiligo is behaving. This collaborative approach ensures that any treatment you pursue is both timely and appropriate, improving your chances of achieving the best possible outcomes. If you’re considering Vitiligo treatment in London as part of a personalised care plan, you can get in touch with us at London Dermatology Centre.
References:
- Al-Smadi, K., Imran, M., Leite-Silva, V.R. and Mohammed, Y., 2023. Vitiligo: A review of aetiology, pathogenesis, treatment, and psychosocial impact. Cosmetics, 10(3), p.84. Available at: https://www.mdpi.com/2079-9284/10/3/84
- Ibrahim, S., Hegazy, R.A., Gawdat, H.I., Esmat, S., Mahmoud, E., Rashed, L., Hegazy, A.A. and Saadi, D.G., 2022. Differentiating active from stable vitiligo: The role of dermoscopic findings and their relation to CXCL10. Journal of Cosmetic Dermatology, 21(10), pp.4651–4658. Available at: https://pubmed.ncbi.nlm.nih.gov/35298096/
- Kamath, C., Dhurat, R., Shah, B., Sharma, R., Kowe, P.A. and Chamle, S., 2023. Monitoring of vitiligo patches over six months to validate dermoscopic findings of lesional stability. Dermatology Practical & Conceptual, 13(4), p.e2023277. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC10656188
- Jha, A.K., Sonthalia, S. and Lallas, A., 2018. Dermoscopy as an evolving tool to assess vitiligo activity. Journal of the American Academy of Dermatology, 78(5), pp.1017–1019. Available at: https://pubmed.ncbi.nlm.nih.gov/29229577/
- Yang, Y., Morriss, S. and Rodrigues, M., 2024. Dermoscopy in vitiligo, diagnostic clues and markers of disease activity: a review of the literature. Clinical and Experimental Dermatology, 49(9), pp.969–975. Available at: https://academic.oup.com/ced/article-abstract/49/9/969/7513393