Many people notice that their skin behaves very differently in winter. Conditions that felt stable during warmer months suddenly flare, dryness becomes harder to control, and irritation appears more easily. This change is not your imagination, and it is not simply about cold air touching the skin. Winter affects the skin at a biological level. Changes in temperature, humidity, circulation, and immune activity alter how the skin functions and how resilient it feels.
In this article, we’ll explain what actually happens to the skin during winter, why existing conditions often worsen, and how dermatologists manage seasonal skin instability across different skin types.
Why Winter Has a Stronger Effect Than You Expect
Your skin is a living organ that constantly adapts to its surroundings. We often underestimate how sensitive it is to environmental change, especially when conditions shift quickly. In winter, your skin has to work much harder to maintain balance.
During colder months, several stressors hit the skin at the same time. Cold air, low humidity, indoor heating, and reduced sunlight all combine to disrupt the skin barrier. We see this lead to increased dryness, sensitivity, and irritation.
These overlapping changes create ideal conditions for flare-ups. When the skin barrier is weakened, underlying conditions are more likely to resurface. Understanding this helps you see why winter care needs a more proactive and protective approach.
The Skin Barrier and Its Role in Winter Flares
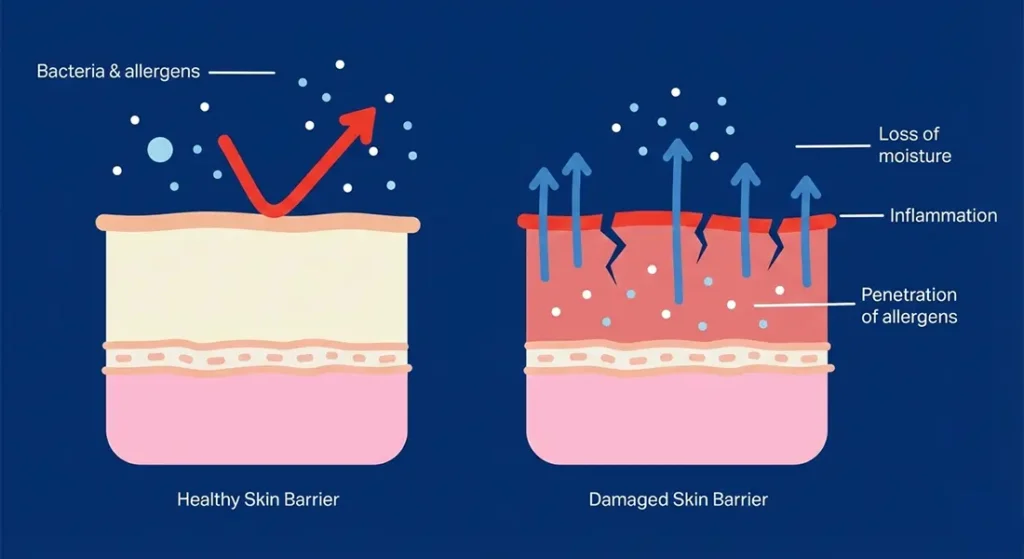
Your skin barrier plays a vital role in keeping your skin healthy, comfortable, and resilient. It acts as the body’s first line of defence, protecting you from environmental stress while helping the skin retain moisture. During winter, this protective system is often put under extra strain.
Here’s why the skin barrier matters so much in colder months:
1. The Skin Barrier Protects and Defends – The barrier is made up of tightly packed skin cells and natural lipids. Together, they keep moisture in and block out irritants, allergens, and bacteria.
2. Winter Weakens the Barrier – Cold air, low humidity, and indoor heating reduce moisture levels in the skin. This makes the barrier less effective and more prone to damage.
3. Moisture Loss Triggers Skin Instability – When the barrier weakens, water escapes more easily from the skin. This leads to dryness, tightness, and increased sensitivity.
4. A Compromised Barrier Worsens Skin Conditions – Once the barrier is damaged, inflammatory skin conditions become harder to control. Flare-ups are more likely, and recovery can take longer.
Protecting the skin barrier is key to reducing winter flares. By supporting hydration and barrier repair, we help your skin stay calmer, stronger, and more resilient throughout the colder months. Understanding this role allows you to take proactive steps rather than simply reacting to flare-ups.
How Cold Air Disrupts Barrier Function
Cold air contains very little moisture, which can quietly stress your skin without you noticing at first. As water evaporates more quickly from the surface, the skin’s protective barrier becomes less effective. Even if your skin condition is usually well controlled, these changes can make it more vulnerable.
Cold air disrupts barrier function because:
- Low humidity increases moisture loss – Water evaporates from the skin more rapidly, leaving it dry and less resilient.
- Barrier lipids become depleted – Reduced natural oils weaken the skin’s protective layer, making it more permeable.
- Sensitivity and reactivity increase – A compromised barrier allows irritants to penetrate more easily, triggering redness or irritation.
- Stable conditions can still flare – Even well-managed skin conditions may worsen when barrier function drops.
By understanding how cold air affects the skin barrier, we can take early steps to protect your skin and reduce seasonal flares.
Top of Form
Bottom of Form
Why Indoor Heating Makes Things Worse
Indoor heating dries the air even further during winter. We often see this constant exposure to warm, dry air pull moisture from your skin throughout the day. Over time, this can be more damaging than the outdoor cold itself.
As moisture loss increases, the skin barrier becomes weaker and less able to protect itself. You may notice more tightness, flaking, or irritation as a result. We recognise this pattern in many patients during colder months.
Heating also creates repeated temperature changes as you move between indoors and outdoors. This constant shift puts additional stress on the skin. When we understand this cycle, it becomes clearer why winter flare-ups are so common and persistent.
Changes in Skin Hydration During Winter
Hydration is not just about how much water you drink. In winter, we see the skin’s ability to retain moisture reduce significantly, even when fluid intake is adequate. This means dryness can develop despite good general hydration.
Cold air and low humidity reduce natural moisturising factors within the skin. At the same time, evaporation from the skin surface increases. We often notice that moisturisers feel less effective because the barrier itself is compromised.
As a result, dryness becomes structural rather than temporary. We focus on repairing and supporting the skin barrier, not just adding moisture. Understanding this shift helps you manage winter skin more effectively and prevent flare-ups.
Why Dry Skin Feels Itchy and Irritated
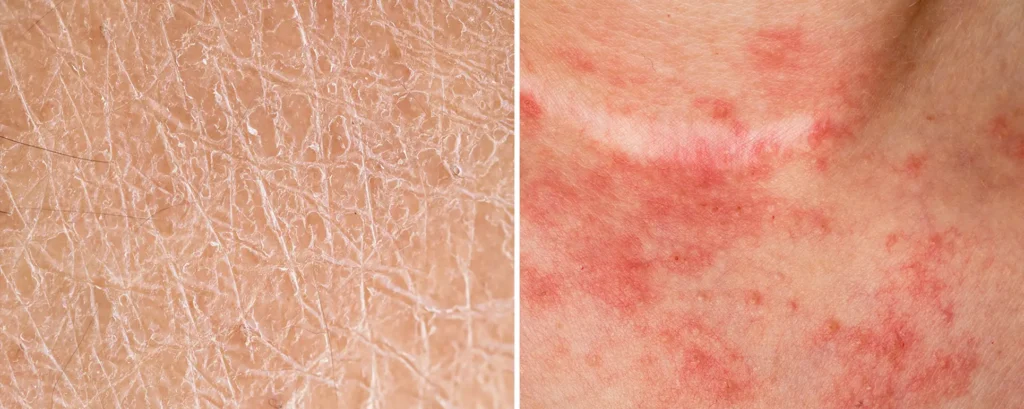
Dry skin is not just uncomfortable it actively triggers irritation. When hydration levels drop, the skin’s protective systems weaken and nerve endings become more exposed. This is why dryness often feels itchy or sore, even when there is no obvious rash.
Here’s what’s happening beneath the surface:
1. Dryness Activates Nerve Endings – As the skin loses moisture, nerve fibres sit closer to the surface and become more reactive. This heightened sensitivity leads to itching, stinging, or burning sensations.
2. Reduced Hydration Increases Sensitivity – Without enough water, the skin cannot cushion nerve endings properly. Even mild friction, clothing, or temperature changes can cause discomfort.
3. Itching Occurs Without Visible Rash – Dry skin can feel intensely itchy even when it looks relatively normal. This often makes the irritation confusing and easy to underestimate.
4. Scratching Worsens Barrier Damage – Scratching breaks down the skin barrier further. This fuels inflammation, increases moisture loss, and creates a cycle of ongoing irritation.
Breaking this itch–scratch cycle is essential for recovery. By restoring hydration and supporting the skin barrier, we calm nerve sensitivity and reduce inflammation. Understanding why dry skin itches helps you respond early, rather than waiting for symptoms to escalate.
How Winter Affects Skin Circulation
Cold temperatures change how blood flows through the body. We know the body prioritises keeping vital organs warm, which means circulation to the skin is reduced. This response is protective, but it has consequences for skin health.
When circulation to the skin decreases, oxygen and nutrient delivery are limited. We often see this make the skin slower to repair itself and more prone to irritation. Healing processes can become less efficient during colder months.
Reduced circulation also increases skin sensitivity. You may notice your skin reacting more easily or taking longer to recover from minor damage. Understanding this helps explain why winter skin often feels more fragile and reactive.
Why Redness and Flushing Behave Differently in Winter
During winter, some people notice increased redness, while others find their skin looks paler. We see this because cold temperatures cause blood vessels to constrict as the body tries to conserve heat. This reduced surface blood flow can temporarily dull skin colour.
When you move indoors, warmth triggers reactive dilation of these vessels. We often observe this rapid constrict-and-dilate cycle stressing the vascular system in the skin. Over time, this instability makes redness and flushing more noticeable.
This pattern is especially relevant for conditions like rosacea. Vascular instability contributes to winter flare-ups and increased sensitivity. Understanding this helps us explain why winter redness can feel harder to control and more unpredictable.
The Impact of Winter on Inflammation

Many people notice that their skin feels more reactive and inflamed during the winter months. This isn’t a coincidence. Colder weather creates several changes in the skin and immune system that make inflammation harder to control.
Here’s why inflammation often worsens in winter:
1. Cold Weather Disrupts the Skin Barrier – Low temperatures and dry air weaken the skin barrier, allowing irritants and allergens to penetrate more easily. This triggers immune responses that increase inflammation.
2. Reduced Sunlight Alters Immune Regulation – Less exposure to natural sunlight affects how the immune system regulates inflammation. For some people, this shift can make inflammatory skin conditions more persistent.
3. Increased Exposure to Irritants – Indoor heating, harsh fabrics, and frequent washing are more common in winter. These factors further irritate the skin and contribute to ongoing inflammation.
4. Low-Grade Inflammation Becomes Persistent – Instead of short flare-ups, inflammation may linger at a low level throughout winter. This can lead to continuous discomfort and repeated flare cycles.
Understanding how winter affects inflammation helps us manage skin conditions more proactively. By supporting the skin barrier and adjusting care during colder months, we can reduce flare frequency and keep inflammation under better control.
Why Eczema Commonly Worsens in Winter
Eczema is strongly linked to weakness in the skin barrier, which makes it particularly sensitive to environmental change. During winter, colder air and lower humidity place extra stress on already vulnerable skin. Even if your eczema is usually mild, these conditions can make it harder to keep symptoms under control.
Eczema often worsens in winter because:
- Barrier weakness becomes more pronounced – Cold, dry air further reduces the skin’s ability to retain moisture.
- Dryness and itch intensify – Increased water loss leads to tighter, itchier skin, which can trigger scratching and flares.
- Tolerance to irritants drops – Skin becomes more reactive to soaps, fabrics, and environmental triggers.
- Mild eczema can escalate quickly – Changes that seem small can push stable eczema into a more active phase.
By recognising winter as a high-risk period, we can adjust care early and help you protect your skin barrier more effectively.
Why Psoriasis Can Become More Active
Psoriasis often behaves differently across the seasons, and winter can be particularly challenging. We see reduced natural sunlight during colder months remove an important anti-inflammatory influence on the skin. This change alone can allow inflammation to become more active.
Winter also brings added triggers such as stress, infections, and increased dryness. These factors combine to weaken the skin barrier and provoke immune activity. You may notice flare-ups becoming more frequent or harder to control during this time.
As a result, plaques often become thicker, drier, and more inflamed. We recognise this seasonal pattern and adjust management accordingly. Understanding why psoriasis worsens in winter helps you take proactive steps to protect your skin.
How Acne Changes During Winter
Acne does not always improve during cold weather, and for many people it can actually feel more unpredictable. We often see winter dryness change how your skin behaves, even if oil production seems lower. This shift can alter the type of breakouts you experience.
Dryness often leads people to over-cleanse or reach for harsher products. We know this can disrupt the skin barrier and trigger more inflammation. Instead of calming acne, these habits can make it more reactive and uncomfortable.
As a result, breakouts may shift from oily congestion to irritated, inflamed acne. We encourage you to adjust your routine for winter rather than treating acne the same way year-round. Supporting the skin barrier helps keep breakouts calmer and more manageable.
Why Rosacea Is Triggered by Cold and Heat Changes
Rosacea-prone skin is especially sensitive to sudden temperature changes. We often see cold wind cause blood vessels to constrict, followed by rapid dilation when you move indoors. This repeated stress makes the skin more reactive.
These constant shifts increase flushing, redness, and sensitivity. Over time, the skin’s vascular response becomes less stable, which can worsen rosacea symptoms during winter months. We recognise this as a common seasonal trigger.
Because of this, winter routines need careful adjustment. We focus on protecting the skin barrier and minimising extreme temperature exposure where possible. Small changes in daily habits can make a noticeable difference in controlling winter flare-ups.
The Effect of Winter on Pigmentation Problems
Pigmentation issues often feel more noticeable during the winter months, and there are clear reasons for this. Seasonal inflammation and slower skin recovery can leave marks behind that take longer to fade. Understanding this process helps you manage pigmentation more effectively.
Here’s how winter affects pigmentation:
1. Pigment Cells React to Inflammation – When the skin becomes inflamed, pigment-producing cells are stimulated. This can lead to dark marks forming after flare-ups, even once the active irritation has settled.
2. Winter Flares Increase Pigmentation Risk – Conditions like eczema, acne, or general irritation often worsen in colder months. These flares increase the likelihood of post-inflammatory pigmentation.
3. Healing Slows Down in Cold Weather – Reduced circulation and slower skin turnover in winter mean the skin repairs itself more slowly. As a result, pigmentation can linger for longer than it would in warmer months.
4. Pigmentation Becomes More Noticeable – With dryness and uneven texture, dark marks may stand out more against winter skin. This can make pigmentation feel more prominent, even if it hasn’t actually worsened.
Pigmentation in winter is often a result of inflammation rather than sun exposure alone. By focusing on calming the skin and supporting healing, we can reduce the chance of marks forming and help existing pigmentation fade more smoothly over time.
Why Wound Healing Slows in Winter
During the colder months, your skin doesn’t repair itself as efficiently as it does in warmer conditions. Lower temperatures affect circulation and skin metabolism, which can slow the healing process. Even small cuts or irritations may take longer to settle than you expect.
Wound healing slows in winter because:
- Reduced blood flow limits repair – Cold temperatures cause blood vessels to constrict, reducing the delivery of oxygen and nutrients needed for healing.
- Inflammation can persist for longer – Ongoing low-grade inflammation interferes with normal tissue repair.
- Skin is drier and more fragile – A weakened barrier makes skin more prone to cracking and delayed closure.
- Minor injuries can linger – Small wounds, scars, or post-procedure sites may take longer to recover.
Understanding these seasonal changes helps us adjust skincare and treatment timing to support healthier, more reliable healing during winter.
Top of Form
Bottom of Form
Why Hands, Lips, and Face Are Affected First
Some areas of your skin are more vulnerable than others, especially during winter. Hands, lips, and the face tend to show problems first because they are exposed constantly and have fewer natural defences. This makes them early indicators of barrier stress.
Here’s why these areas are affected sooner:
1. These Areas Are Constantly Exposed – Your hands, lips, and face are regularly exposed to cold air, wind, and environmental irritants. Unlike covered areas, they rarely get a break from harsh conditions.
2. Frequent Washing Weakens the Barrier – Hands are washed often, especially in winter, which strips away protective oils. Lips and facial skin also lack the same oil gland support as other areas, making barrier breakdown quicker.
3. The Skin Barrier Breaks Down Faster – Repeated exposure and moisture loss weaken the barrier in these zones more rapidly. Once compromised, dryness, cracking, and irritation can develop quickly.
4. Symptoms Appear Earlier and More Intensely – Because damage occurs faster, symptoms such as soreness, redness, and tightness show up sooner. These areas often flare before problems appear elsewhere on the body.
Targeted care is essential for hands, lips, and face during winter. By protecting and restoring the barrier early in these high-risk areas, we can prevent discomfort from escalating and reduce the risk of wider skin flares.
How Winter Affects Different Skin Types
Winter affects every skin type, but not in the same way. Dry skin often becomes drier and more uncomfortable as moisture loss increases. We commonly see flaking, tightness, and increased sensitivity during colder months.
Oily skin can feel tight on the surface yet still break out underneath. We notice many people mistake this tightness for dryness and overcompensate, which can worsen congestion and inflammation. Acne may behave differently rather than disappearing.
Sensitive skin tends to react more easily in winter, and darker skin types may develop more pigmentation after inflammation. We want you to know that winter skin changes are normal. Understanding your skin type helps us adjust care so you stay comfortable and protected.
Why Skincare That Worked in Summer Often Fails
Skincare routines need to change with the seasons. Products that felt perfectly balanced in summer may become too harsh or simply not nourishing enough in winter. We often see flare-ups happen when routines stay the same despite environmental changes.
In colder months, the skin barrier is under more stress from dryness, heating, and reduced humidity. If you continue using lightweight or active-heavy products, irritation can build quietly. You may notice tightness, redness, or breakouts that weren’t an issue before.
Skincare needs to adapt to environmental biology, not habit. We encourage you to adjust textures, hydration, and protection as conditions change. When your routine evolves with the season, your skin is far more likely to stay calm and resilient.
How Dermatologists Approach Seasonal Skin Changes
Seasonal changes, especially winter, are predictable stressors for the skin. Dermatologists don’t wait for flares to happen we anticipate them and adjust care in advance. This proactive approach helps keep your skin stable rather than constantly reacting to problems.
Here’s how we manage seasonal skin changes:
1. Winter Instability Is Anticipated – We know colder months increase dryness, sensitivity, and inflammation. Planning ahead allows us to reduce the likelihood of flares before they start.
2. Treatment Is Adjusted Proactively – Instead of waiting for symptoms to worsen, treatment plans are modified early. This may include stronger barrier support or changes in active treatments.
3. Barrier Support Is Prioritised – Strengthening the skin barrier becomes a key focus in winter. A healthier barrier helps reduce irritation, moisture loss, and flare frequency.
4. Inflammation and Triggers Are Actively Managed – We aim to control low-grade inflammation and reduce exposure to known triggers. This keeps the skin calmer and more resilient throughout the season.
By acting early rather than chasing flares, we help prevent escalation. This proactive strategy supports more comfortable skin, fewer disruptions, and better long-term control during challenging seasonal changes.
Why Moisturising Alone Is Sometimes Not Enough
Moisturising is essential, but it isn’t always enough on its own. We often see that when inflammation is active, simply adding hydration does not restore balance. The skin may stay red, itchy, or reactive despite regular moisturiser use.
If underlying inflammation is driving symptoms, targeted anti-inflammatory treatment may be needed. We focus on calming the skin first rather than endlessly layering products. Treating inflammation allows the barrier to recover more effectively.
Addressing the cause matters more than adding more steps. We help you understand what your skin actually needs at that moment. When treatment is targeted and thoughtful, moisturisers work better as part of a complete approach.
The Role of Preventive Care in Winter
Preventive care is often far more effective than trying to repair damage later. We know that strengthening your skin barrier before winter begins helps reduce the severity of flare-ups. Preparing early allows the skin to cope better with seasonal stress.
By intervening early, we can limit inflammation, dryness, and discomfort before they escalate. This proactive approach helps keep symptoms more manageable throughout the colder months. You’re less likely to experience sudden or severe flares.
Over time, prevention also reduces long-term skin damage. We focus on protecting skin health rather than reacting to crises. When you take a preventive approach, winter becomes far easier for your skin to handle.
Top of Form
Bottom of Form
How Lifestyle Influences Winter Skin Health
During winter, everyday habits can quietly worsen skin problems without you realising it. Cold weather often changes how you bathe, move, and spend time indoors, all of which affect skin balance. Winter skin care is not just about products, but about how you live day to day.
Lifestyle factors influence winter skin health because:
- Hot showers and frequent washing strip the barrier – Heat and over-cleansing remove protective oils, increasing dryness and irritation.
- Indoor heating dries the air – Low indoor humidity accelerates moisture loss from the skin.
- Reduced physical activity affects circulation – Less movement can impact skin repair and immune balance.
- Stress alters inflammatory responses – Winter stress can worsen flares by increasing immune reactivity.
By making small lifestyle adjustments alongside skincare, we can significantly reduce winter flares and support healthier skin throughout the colder months.
When to Seek Professional Help
If your skin condition worsens every winter despite good care, it’s a sign that assessment is important. We see this pattern often, and it usually means something deeper is driving the flare-ups. Repeated seasonal worsening is not something you should ignore.
Persistent flares often suggest underlying inflammation or that current management isn’t quite right. We can help identify what’s causing the instability and adjust treatment accordingly. This is where specialist input makes a real difference.
Early guidance helps break the cycle before it repeats year after year. By understanding what your skin needs, we can reduce flare frequency and protect long-term skin health. Seeking help sooner rather than later leads to better control and reassurance.
Why Personalised Care Matters in Winter
There is no single winter routine that works for everyone. Your skin type, diagnosis, lifestyle, and environment all influence how your skin reacts in colder months. We know generic advice often falls short because it ignores these differences.
Personalised care allows us to address what your skin actually needs, not what usually works for others. By tailoring treatment and skincare, we achieve better control and fewer flare-ups. This individual approach is central to effective dermatology care, especially during winter.
How Expert Care Supports Long-Term Stability
Seasonal flare-ups don’t have to be inevitable. With the right strategy in place, we can help keep your skin stable even through winter. The focus is on understanding how your skin behaves, not following trends.
Expert care looks at the underlying biology driving your symptoms. We use this understanding to guide treatment and prevention in a structured way. This approach helps reduce unpredictability and repeated seasonal cycles.
This is where specialist dermatology care truly adds value. By addressing causes rather than just symptoms, we support long-term stability and healthier skin over time.
FAQs:
1. Why do skin conditions flare every winter even when they are controlled in summer?
Winter places multiple stresses on the skin at the same time, including cold air, low humidity, indoor heating, and reduced circulation. These factors weaken the skin barrier and increase inflammation, making previously stable conditions more vulnerable. Even well-managed skin can flare when its protective systems are under constant strain.
2. Is winter skin worsening caused only by cold weather touching the skin?
No, the worsening of skin problems in winter is not just about cold air contact. The real issue lies in how winter alters skin biology, including moisture retention, lipid production, immune activity, and nerve sensitivity. These internal changes reduce resilience and make the skin more reactive overall.
3. Why does my skin feel itchier in winter even without a visible rash?
In winter, reduced hydration exposes nerve endings closer to the skin surface, making them more sensitive. This heightened nerve activity can cause itching, burning, or stinging without obvious redness or rash. Dryness alone is enough to trigger discomfort when the skin barrier is compromised.
4. How does indoor heating contribute to winter skin problems?
Indoor heating significantly reduces air humidity, which accelerates moisture loss from the skin throughout the day. This ongoing dehydration weakens the skin barrier and increases sensitivity. Repeated movement between cold outdoor air and warm indoor environments adds further stress to the skin.
5. Why do eczema and psoriasis often worsen specifically during winter months?
Eczema worsens because winter further weakens an already fragile skin barrier, increasing dryness and itch. Psoriasis often becomes more active due to reduced sunlight, increased inflammation, and greater environmental stress. Both conditions are highly sensitive to the biological changes that occur in colder seasons.
6. Can winter affect oily or acne-prone skin as well as dry skin?
Yes, winter affects all skin types, including oily and acne-prone skin. Surface dryness can disrupt the skin barrier, leading to increased inflammation and altered oil behaviour. This can result in more irritated or inflamed breakouts rather than classic oily congestion.
7. Why do hands, lips, and face show winter damage before other areas?
These areas are constantly exposed to cold air, wind, and frequent washing, and they have fewer protective oil glands. Because their barriers break down faster, symptoms such as cracking, redness, and soreness appear earlier. They often act as early warning signs of wider barrier stress.
8. Does reduced circulation in winter affect skin healing?
Yes, cold temperatures cause blood vessels to constrict, reducing oxygen and nutrient delivery to the skin. This slows repair processes and makes the skin more fragile. As a result, irritation, wounds, and post-inflammatory marks can take longer to resolve during winter.
9. Why does skincare that worked well in summer stop working in winter?
Summer skincare routines are often too light or too active for winter conditions. When the skin barrier is under greater stress, products that once felt balanced may become irritating or insufficient. Winter skin needs more barrier support and gentler care to stay stable.
10. When should winter skin problems be assessed by a dermatologist?
If your skin flares every winter despite consistent care, professional assessment is important. Repeated seasonal worsening usually indicates underlying inflammation or barrier dysfunction that needs targeted treatment. Early intervention can prevent the same cycle from repeating year after year and improve long-term skin stability.
Final Thoughts: Understanding Winter Biology Helps You Protect Your Skin
Winter skin flare-ups are not simply bad luck or poor skincare. They are driven by real biological changes that weaken the skin barrier, alter circulation, reduce hydration, and increase inflammation. Understanding these processes helps you manage flare-ups more proactively and protect your skin through the colder months rather than reacting once problems escalate. If you’re looking to book a consultation with one of our dermatologists, you can contact us at the London Dermatology Centre.
References:
1. Impact of water exposure and temperature changes on skin barrier function. Journal of Clinical Medicine, 11. https://www.mdpi.com/2077-0383/11/2/298
2. Skin Barrier Function: The Interplay of Physical, Chemical and Biological Factors. Cells, 12(23), p.2745. https://www.mdpi.com/2073-4409/12/23/2745
3. Denda, M., Tsuchiya, T., Elias, P.M. & Feingold, K.R., 1998. Influence of dry environment on epidermal function. Journal of Investigative Dermatology. https://www.sciencedirect.com/science/article/abs/pii/S0923181100001377
4. Thyssen, J.P. & Engebretsen, K.A., 2015. The effect of environmental humidity and temperature on skin barrier function and dermatitis. https://pubmed.ncbi.nlm.nih.gov/26449379/
5. Improvement of mild inflammatory changes of the facial skin induced by winter environment with daily applications of a moisturizing cream. Skin Research and Technology. https://pubmed.ncbi.nlm.nih.gov/14571069/
