Autoimmune skin diseases develop when your immune system mistakenly attacks healthy skin cells. Instead of protecting your body from infections, your immune response becomes misdirected and leads to inflammation, irritation, and visible skin changes. These conditions can vary widely in how they appear and how severe they become.
You may notice that many autoimmune conditions are more common in women than in men. Researchers have consistently observed this pattern across several skin diseases and continue to study the reasons behind it. Hormonal influences, genetic factors, and differences in how your immune system functions all seem to play a role.
If you are dealing with a long-term skin condition, understanding why these diseases affect women more often can give you useful insight. It can also help you make more informed decisions about your care. In this article, you will explore the most common autoimmune skin conditions, why they occur more frequently in women, and how they are diagnosed and managed.
What Are Autoimmune Skin Diseases?
Autoimmune skin diseases develop when your immune system mistakenly attacks your own skin tissues. This abnormal response leads to inflammation, redness, and structural changes in your skin. Each condition has its own distinct pattern, so the symptoms you experience can vary.
Your immune system is meant to protect you from bacteria and viruses. However, in autoimmune conditions, it cannot properly distinguish between harmful invaders and healthy cells. This confusion causes your body to trigger ongoing inflammation in the skin.
These conditions are often chronic and may follow a cycle of flare-ups and remission. Treatment focuses on helping you control symptoms and prevent the condition from worsening. Getting an early diagnosis can significantly improve your long-term outcomes.
Why Women Are More Affected
You are more likely to develop autoimmune conditions if you are a woman, and this pattern is seen across many parts of the body, including the skin. Researchers believe this is partly due to differences in how your immune system functions. The female immune system tends to be more reactive, which can increase the likelihood of it mistakenly attacking healthy tissue.
Hormones such as oestrogen also play an important role in regulating your immune response. These hormones can enhance immune activity, which may raise the risk of autoimmune reactions. Although this link is well recognised, researchers are still studying exactly how these hormonal effects influence different conditions.
Genetic factors also contribute to this increased risk. Certain immune-related genes may be more active in women, affecting how the body responds to triggers. When combined, these hormonal, genetic, and immune system differences help explain why autoimmune diseases are more common in women.
The Role of Hormones
Your hormones play an important role in how your immune system behaves. Oestrogen, in particular, can stimulate immune responses and make them more active. While this can help your body fight infections, it may also increase the risk of autoimmune reactions.
You may notice that hormonal changes during puberty, pregnancy, or menopause affect your symptoms. Some women experience flare-ups during these stages, while others may notice temporary improvement. These shifts can vary from person to person.
Understanding how your hormones influence your condition helps explain why your symptoms may change over time. It also helps guide your treatment plan. Your doctor will often consider these patterns when managing your autoimmune skin condition.
Genetic and Immune System Differences
Your genetics and immune system both play an important role in the development of autoimmune conditions. In women, these factors can make the immune response more active, which may increase the likelihood of the body mistakenly attacking its own tissues. Understanding these differences helps explain why autoimmune diseases are often more common in women.
- The role of X chromosomes: Women have two X chromosomes, and these contain many genes related to immune function. Having two copies can sometimes lead to a stronger or more reactive immune response, which may increase the risk of autoimmune activity.
- Genetic variations and susceptibility: Certain genetic variations can affect how your immune system recognises your body’s own cells. If this recognition process becomes less accurate, your immune system may mistakenly target healthy tissue.
- Differences in immune response: Your immune system is unique to you. Some people naturally have a more active or inflammatory response, which can increase susceptibility to autoimmune conditions.
- Impact on disease development: These genetic and immune differences do not guarantee that you will develop an autoimmune condition, but they can increase your overall risk. Environmental and hormonal factors also play a role.
By understanding how your genetics and immune system interact, you can better appreciate why autoimmune conditions develop and why individual risk can vary from person to person.
Psoriasis in Women
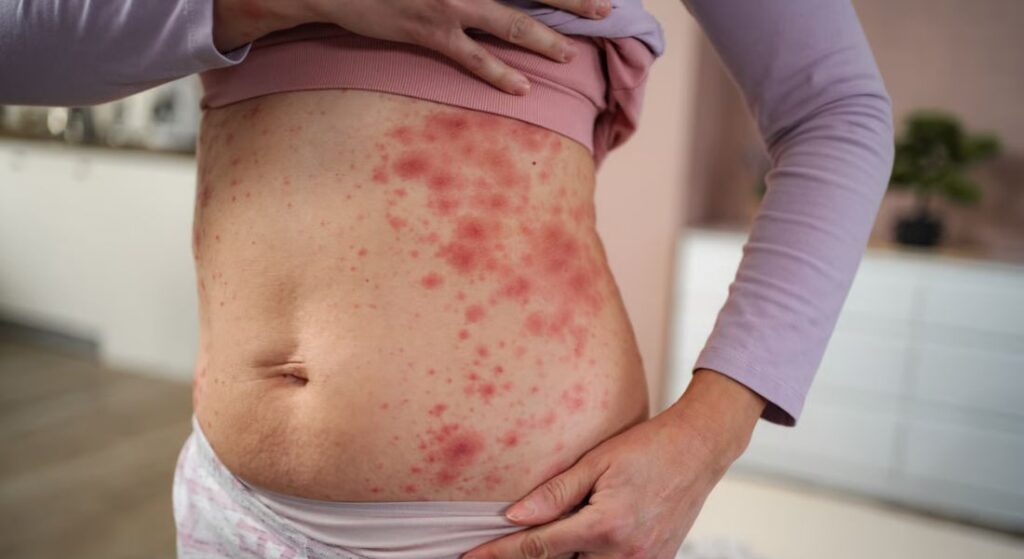
Psoriasis is an autoimmune skin condition that speeds up the life cycle of your skin cells. Instead of renewing gradually, cells build up quickly on the surface, forming thick, scaly patches. These areas can feel dry, itchy, and sometimes uncomfortable. Although psoriasis affects both men and women, hormonal changes can influence how your symptoms appear and fluctuate over time.
- How it affects your skin: You may notice red, raised patches covered with silvery scales. These commonly appear on the elbows, knees, scalp, or lower back, but they can occur anywhere on your body.
- Hormonal influence: Changes during pregnancy, menstrual cycles, or menopause can affect your symptoms. You might notice flare-ups at certain times, while in other periods, your skin may improve.
- Triggers and flare-ups: Stress is a well-known trigger. Illness, skin injury, and certain medications can also cause symptoms to worsen. Learning your personal triggers can help you manage flare-ups more effectively.
- Personalised management: Psoriasis varies from person to person, so your treatment plan will be tailored to your needs. Managing inflammation and maintaining skin health are key to improving long-term outcomes.
With the right care and a clear understanding of your triggers, you can keep psoriasis under control and maintain healthier, more comfortable skin.
Lupus and Skin Involvement
Systemic lupus erythematosus is a well-known autoimmune condition that often affects your skin as well as other parts of your body. It is significantly more common in women than in men. You may notice symptoms such as rashes, sensitivity to sunlight, and different types of skin lesions. These skin changes can vary in appearance and severity.
One of the most recognised signs is the butterfly-shaped rash that appears across your cheeks and nose. This rash may become more noticeable after sun exposure. You might also experience other skin-related symptoms, depending on how the condition affects you. Being aware of these signs can help you seek medical advice early.
Managing lupus involves controlling your immune system activity to reduce inflammation. Your treatment may include medications that help calm the immune response and protect your skin. Early diagnosis and ongoing care are important for preventing complications. With proper management, you can keep symptoms under control and protect your long-term health.
Lichen Planus
Lichen planus is an inflammatory condition that can affect your skin as well as the mucous membranes, such as the inside of your mouth. You may notice purple, itchy, flat-topped bumps that can appear on areas like your wrists, ankles, or lower back. Women are commonly affected by this condition.
The exact cause is not fully understood, but your immune system plays a key role in its development. It may be triggered by factors such as infections, certain medications, or stress. The symptoms you experience can vary, with some people having mild irritation while others develop more widespread lesions.
Treatment focuses on reducing inflammation and relieving your symptoms. Your doctor may recommend topical corticosteroids to calm the affected areas. In more severe cases, additional treatments may be needed to manage the condition effectively.
Dermatomyositis
Dermatomyositis is an autoimmune condition that affects both your skin and your muscles. It is more commonly diagnosed in women than in men. You may notice a distinctive rash on your face, eyelids, or upper body, which is often one of the earliest signs.
Alongside skin changes, you may also experience muscle weakness. This can make everyday activities, such as climbing stairs or lifting objects, more difficult. Because the condition affects both skin and muscle, early diagnosis is important for effective management.
Treatment usually involves medications that help suppress your immune system and reduce inflammation. You will also need regular monitoring to track your progress and adjust treatment if needed. With comprehensive care, you can manage symptoms more effectively and improve your overall quality of life.
Vitiligo and Autoimmune Mechanisms

Vitiligo develops when your immune system attacks the cells responsible for producing pigment in your skin. As a result, you may notice patches of lighter or completely depigmented skin. This condition can affect anyone, but autoimmune mechanisms play a central role in how it develops and progresses.
You may find that your vitiligo changes during periods of stress or hormonal shifts. In some cases, the condition can progress more noticeably at these times. Because the changes are visible, vitiligo can also affect your confidence and emotional wellbeing. Supportive care and reassurance are often an important part of managing the condition.
Treatment options may include topical medications, light therapy, or other medical approaches recommended by your doctor. Early intervention can help stabilise the condition and limit further spread. With ongoing care, you can manage vitiligo effectively and maintain your quality of life.
Autoimmune Blistering Diseases
Autoimmune blistering diseases are a group of conditions in which your immune system mistakenly attacks the structures that hold your skin layers together. This leads to the formation of blisters on the skin and sometimes on mucous membranes, such as the mouth. Conditions such as pemphigus and bullous pemphigoid fall into this category, and some types are seen more frequently in women. These conditions can vary in severity, but early recognition and proper treatment make a significant difference in outcomes.
- Why blisters form: In these conditions, your immune system targets specific proteins that act like “glue” between skin cells. When these proteins are damaged, the layers of your skin separate, leading to fluid-filled blisters. These blisters may appear on the skin or inside the mouth and can sometimes be painful or fragile.
- Symptoms and discomfort: You may notice blisters that break easily, leaving raw or sore areas behind. The skin can feel tender, and everyday activities like eating or dressing may become uncomfortable if sensitive areas are affected. The severity of symptoms can vary from mild to more widespread involvement.
- How diagnosis is confirmed: To diagnose these conditions accurately, your doctor will usually perform a skin biopsy. This involves taking a small sample of skin to examine under a microscope. Additional laboratory tests help identify the specific antibodies involved, ensuring the correct diagnosis is made.
- Treatment and long-term management: Treatment focuses on calming the immune system. This often involves medications such as corticosteroids or other immunosuppressive therapies. You may need regular follow-up appointments to monitor your condition and adjust treatment as needed.
Managing autoimmune blistering diseases requires ongoing care, but early diagnosis and treatment can significantly improve your comfort and long-term outlook. With the right support, many people are able to control symptoms effectively and maintain a good quality of life.
Alopecia Areata
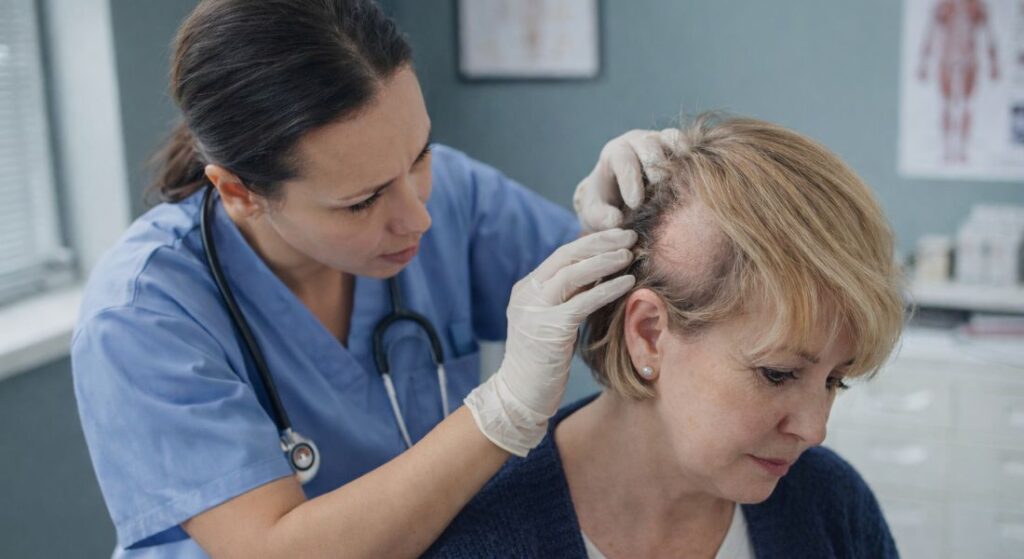
Alopecia areata is an autoimmune condition that causes hair loss when your immune system targets your hair follicles. You may notice small, round patches of hair loss on your scalp or other areas of your body. In some cases, hair loss can become more widespread. Women are commonly affected by this condition.
You may find that hair loss happens suddenly and without warning. This unpredictability can have a strong emotional impact, especially if the changes are noticeable. Support from your doctor, along with counselling if needed, can help you cope with these changes.
Treatment options may include topical therapies and medications that help regulate your immune response. Some people experience natural hair regrowth over time, although this can vary. Management focuses on supporting hair recovery and helping you feel more confident during the process.
The Impact of Stress on Autoimmune Skin Diseases
Stress can have a noticeable effect on your immune system. You may find that your symptoms worsen during periods of emotional or physical stress. In many cases, stress can trigger flare-ups in autoimmune skin conditions.
The link between stress and your immune response is complex. When you are stressed, your body releases hormones that can influence inflammation levels. These changes may make your symptoms more noticeable or harder to control.
Managing your stress can play an important role in supporting your skin health. Simple steps such as relaxation techniques, regular exercise, and getting enough sleep can help. Taking a more holistic approach to your care can improve your overall outcomes.
Diagnosing Autoimmune Skin Conditions
Diagnosing autoimmune skin conditions involves a careful clinical evaluation of your skin. Your dermatologist will examine the appearance, pattern, and distribution of any changes you have noticed. These visual clues often provide important insights into the underlying condition.
To confirm the diagnosis, your doctor may recommend additional tests. These can include blood tests and a skin biopsy to assess immune system activity. The results help identify the exact condition and guide your treatment plan.
Getting an early diagnosis is essential for effective management. Starting treatment promptly can help prevent the condition from progressing. With specialist care, you can achieve better long-term outcomes and maintain healthier skin.
Treatment Approaches
Treatment for autoimmune skin diseases focuses on helping you control your immune response. If your condition is mild, you may be prescribed topical treatments such as creams or ointments. For more severe cases, your doctor may recommend systemic medications that work throughout your body.
In some conditions, biologic therapies are now being used more frequently. These treatments target specific parts of your immune system rather than suppressing it entirely. This more targeted approach can improve effectiveness while reducing unwanted side effects.
Your treatment plan will always be tailored to your individual needs. Your doctor will consider factors such as the severity of your condition and your overall health. Personalised care helps you achieve better and more consistent results over time.
The Role of Lifestyle in Management
Your lifestyle can play an important role in managing autoimmune skin conditions. Maintaining a balanced diet and staying physically active can support your overall wellbeing. These habits may also help reduce inflammation and improve how your body responds to treatment.
You may also benefit from identifying and avoiding your personal triggers. For example, if you have conditions like lupus, protecting your skin from sun exposure is especially important. Using gentle, supportive skincare products can also help reduce irritation and protect your skin barrier.
Taking a holistic approach to your care can make a real difference. Combining medical treatment with healthy daily habits often leads to better outcomes. Consistency is key when it comes to managing your condition over the long term.
Hormonal Life Stages and Disease Patterns
Hormonal changes at different stages of your life can influence how autoimmune diseases behave. Periods such as puberty, pregnancy, and menopause are times when your hormone levels shift significantly. These changes can affect your immune system, which may lead to variations in symptoms. Understanding these patterns helps you and your doctor manage your condition more effectively. At different stages, you may notice changes in how your symptoms appear or progress.
- Puberty and early hormonal changes: During puberty, rising hormone levels can influence how your immune system functions. Some autoimmune conditions may first appear during this stage, while others may become more noticeable. These early changes can help doctors identify patterns in disease onset.
- Pregnancy and symptom changes: During pregnancy, some women notice that their symptoms improve. This is thought to be linked to changes in the immune system that help support the pregnancy. However, this is not the same for everyone, and some conditions may remain unchanged.
- Postpartum flare-ups: After childbirth, hormone levels shift again quite rapidly. This can sometimes trigger flare-ups or worsening of symptoms. It is important to monitor your condition closely during this time and seek medical advice if you notice any changes.
- Menopause and long-term effects: During menopause, declining hormone levels can also affect autoimmune disease activity. Some women may notice changes in symptom severity or new patterns emerging. Your doctor may adjust treatment to help manage these changes effectively.
Recognising how hormonal life stages affect your condition allows for more personalised care. Your doctor can take these factors into account when planning treatment and monitoring your health. With the right approach, you can manage symptoms more effectively through each stage of life.
Psychological Impact of Chronic Skin Conditions
Living with a chronic skin condition can affect your emotional wellbeing as well as your physical health. Visible skin changes may make you feel self-conscious or anxious, especially in social situations. You may also feel additional pressure due to appearance-related expectations.
Support from healthcare professionals can make a meaningful difference. You may benefit from counselling or joining a support group where you can share your experiences. Addressing your mental health is an important part of managing a long-term condition.
As your skin improves with treatment, you may notice a boost in your confidence. Managing symptoms effectively can enhance your overall quality of life. With the right emotional and medical support, you can achieve better long-term outcomes.
Advances in Dermatological Research
Research into autoimmune skin diseases is continuing to evolve, giving you access to better and more effective treatment options. Scientists are studying how your immune system behaves at a molecular level. This helps them develop therapies that target the exact pathways involved in inflammation.
Biologic medications are one of the most important advances in recent years. These treatments are designed to target specific immune molecules rather than suppressing your entire immune system. This approach can offer better control for certain conditions and improve treatment outcomes.
Ongoing research is focused on making treatments more personalised for you. Future therapies may be tailored even more closely to your specific condition and immune profile. As innovation continues, dermatology is moving towards more precise and effective care.
Importance of Early Intervention
When it comes to autoimmune skin diseases, acting early can make a significant difference to your long-term skin health. These conditions often develop gradually, but without timely treatment, inflammation can worsen and lead to more persistent symptoms. Starting treatment early helps control the condition before it becomes more difficult to manage. Recognising the early signs allows you to seek medical advice before complications develop.
- Reducing inflammation early: Early treatment helps calm the immune response before it causes extensive skin damage. By controlling inflammation at the start, you can reduce discomfort such as redness, itching, or pain. This also lowers the risk of long-term skin changes.
- Preventing complications: If treatment is delayed, symptoms may become more severe or widespread. In some cases, untreated inflammation can lead to scarring, infection, or ongoing skin sensitivity. Early intervention helps minimise these risks and supports better skin recovery.
- Getting an accurate diagnosis: Seeing a dermatologist early means you are more likely to receive a correct diagnosis. Autoimmune skin conditions can sometimes look similar to other skin issues, so proper assessment is important. An accurate diagnosis ensures you receive the most effective treatment for your condition.
- Improving long-term outcomes: Starting treatment at the right time can improve how well your condition is controlled over the long term. It may reduce flare-ups, improve comfort, and help you maintain healthier skin. Consistent care also makes it easier to adjust treatment if your condition changes.
You should not ignore persistent or unusual skin changes. If symptoms continue or worsen, it is important to seek professional advice. With early intervention and the right care, you can manage autoimmune skin conditions more effectively and achieve better overall results.
Why Specialist Care Matters
Autoimmune skin diseases can be complex, so it’s important that you receive expert care. Dermatologists are specially trained to diagnose and manage these conditions accurately. Their experience helps ensure that your symptoms are properly assessed and not mistaken for other skin issues.
Seeing a specialist means your treatment plan is tailored specifically to you. Your dermatologist will consider factors such as your age, overall health, and how severe your condition is. This personalised approach helps you achieve better and more consistent results.
Regular follow-up appointments with your specialist are also essential. These visits allow your treatment to be adjusted as your condition changes over time. With ongoing expert care, you can manage your condition more effectively and maintain healthier skin in the long term.
FAQs:
1. Why are autoimmune skin diseases more common in women?
Autoimmune skin diseases are more common in you as a woman because your immune system tends to be more active and responsive. Hormones such as oestrogen can enhance immune reactions, which is helpful for fighting infections but can also increase the risk of the body mistakenly attacking healthy skin cells.
2. Can hormones trigger flare-ups in autoimmune skin conditions?
Yes, hormonal changes can influence your symptoms. You may notice flare-ups during puberty, pregnancy, or menopause because shifts in hormone levels can affect how your immune system behaves and how your skin responds.
3. What are the most common autoimmune skin diseases in women?
Some of the most common conditions you may encounter include lupus, psoriasis, vitiligo, lichen planus, and alopecia areata. Each of these conditions affects the skin differently but shares the underlying issue of an overactive immune response.
4. Are autoimmune skin diseases curable?
Most autoimmune skin diseases are not completely curable, but you can manage them effectively. With the right treatment and lifestyle adjustments, you can control symptoms, reduce flare-ups, and maintain healthy skin over time.
5. How are autoimmune skin conditions diagnosed?
To diagnose your condition, a dermatologist will examine your skin closely and may recommend tests such as blood work or a skin biopsy. These tests help confirm whether your immune system is causing the symptoms.
6. Can stress make autoimmune skin diseases worse?
Yes, stress can play a significant role in worsening your symptoms. When you are under stress, your body releases hormones that can increase inflammation, which may trigger or intensify flare-ups in your skin condition.
7. What treatment options are available for autoimmune skin diseases?
Your treatment will depend on the specific condition and its severity. It may include topical creams, oral medications, light therapy, or advanced treatments like biologics that target specific parts of your immune system.
8. Can lifestyle changes help manage autoimmune skin conditions?
Yes, making healthy lifestyle choices can support your treatment. Eating a balanced diet, staying active, managing stress, and protecting your skin from triggers such as sunlight can all help improve your overall skin health.
9. Is it important to see a specialist for these conditions?
Seeing a dermatologist is important because these conditions can be complex. A specialist can give you an accurate diagnosis and create a personalised treatment plan that suits your specific needs and helps you manage the condition effectively.
10. When should you seek medical advice for skin symptoms?
You should seek medical advice if you notice persistent rashes, unusual skin changes, or symptoms that do not improve with basic care. Early evaluation allows you to start treatment sooner and helps prevent the condition from becoming more severe.
Final Thought: Taking Control of Your Skin Health
If you are living with an autoimmune skin condition, it is important to understand that you are not alone and more importantly, that effective support and treatment are available. These conditions can feel unpredictable, especially when symptoms fluctuate due to hormonal changes, stress, or other triggers. However, with the right guidance, you can take control of your skin health and improve your quality of life.
Early diagnosis and a personalised treatment plan can make a significant difference in how your condition progresses. By recognising symptoms early and seeking professional advice, you give yourself the best chance of managing flare-ups and preventing complications. Consistency in treatment, along with healthy lifestyle choices, can help you maintain more stable and comfortable skin. If you’re looking for female dermatologist in London, you can reach out to us at the London Dermatology Centre to book a consultation with one of our specialists.
References:
- Carlucci, P., Spataro, F., Cristallo, M., Di Gioacchino, M., Nettis, E. and Gangemi, S. (2024) ‘Immune-molecular link between thyroid and skin autoimmune diseases: A narrative review’, Journal of Clinical Medicine, 13(18), p. 5594. https://www.mdpi.com/2077-0383/13/18/5594
- Paganelli, A., Cristofoletti, C., Moro, F., Corrente, A., Colonna, L., Scala, E. and Picardo, M. (2025) ‘Comprehensive overview of cytokine interplay in vitiligo: A decade of meta-analyses systematically reviewed’, Life, 15(5), p. 684. https://www.mdpi.com/2075-1729/15/5/684
- Patel, S., Rauf, A., Khan, H., Meher, B.R. and Hassan, S.S.U. (2017) ‘A holistic review on the autoimmune disease vitiligo with emphasis on the causal factors’, Biomedicine & Pharmacotherapy, 92, pp. 501–508. https://pubmed.ncbi.nlm.nih.gov/28575807/
- Das, D., Akhtar, S., Kurra, S., Gupta, S. and Sharma, A. (2019) ‘Emerging role of immune cell network in autoimmune skin disorders: An update on pemphigus, vitiligo and psoriasis’, Cytokine & Growth Factor Reviews, 45, pp. 35–44. https://pubmed.ncbi.nlm.nih.gov/30773437/
- Dopytalska, K., Czaplicka, A., Szymańska, E. and Walecka, I. (2023) ‘The essential role of microRNAs in inflammatory and autoimmune skin diseases: A review’, International Journal of Molecular Sciences, 24(11), p. 9130. https://pubmed.ncbi.nlm.nih.gov/37298095/