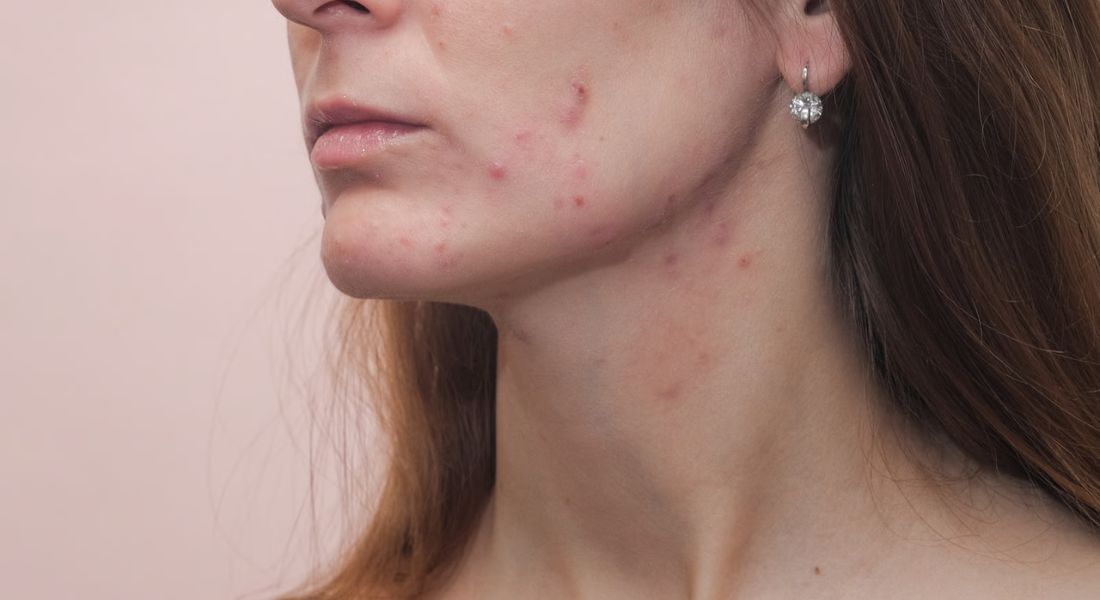
You may not immediately associate psychiatric medications with skin changes, but some can influence acne in noticeable ways. Medications such as lithium are known to affect oil production and trigger inflammatory responses in the skin. These changes can create an environment where breakouts are more likely to develop or worsen.
The impact varies depending on the specific medication and how your body responds to it. Some people may experience only mild or temporary changes, while others notice more persistent or pronounced acne. Factors like dosage, duration of use, and individual skin sensitivity all play a role.
Understanding this connection helps you recognise changes early rather than assuming they are unrelated. If you notice new or worsening acne after starting a medication, it gives you a clearer starting point for discussion with a healthcare professional. This allows for more informed decisions and better management of both your skin and overall treatment plan.
How Lithium Triggers Acne
You should know that lithium can directly influence how your skin behaves. It is thought to increase inflammatory activity and stimulate the oil glands, leading to higher sebum production. This combination creates an environment where pores are more likely to become clogged and inflamed, increasing the risk of breakouts.
Unlike typical acne, lithium-related acne can appear quite suddenly and may progress more rapidly. You might notice clusters of inflamed spots developing over a short period, sometimes in areas that were previously clear. It can also feel more persistent and less responsive to standard over-the-counter treatments.
Recognising lithium as the underlying cause is important for effective management. Once this link is identified, treatment can be adjusted in a more targeted way, often with guidance from a healthcare professional. This helps you manage your skin without compromising your overall treatment plan.
What Lithium-Induced Acne Looks Like
You may notice that acne linked to lithium looks slightly different from typical acne. It often appears as inflamed red bumps or pustules rather than a mix of blackheads and whiteheads. These spots can feel more uniform in appearance and may be more irritated or tender than usual breakouts.
- Inflamed, uniform-looking spots: Lithium-related acne often presents as red, raised bumps or pustules. Unlike typical acne, you may not see many blackheads or whiteheads alongside them.
- More irritation or tenderness: The affected areas can feel more sensitive or sore. You might notice that the spots seem more inflamed and uncomfortable than standard breakouts.
- Wider distribution on the body: It’s not always limited to the face. You may also see breakouts on the chest, back, or shoulders, and sometimes in a more widespread pattern.
- Persistent and recurring flare-ups: New spots may continue to appear even as others start to settle. This can make the acne feel ongoing and harder to fully control.
Understanding these patterns can help you recognise when acne may be medication-related rather than purely hormonal or lifestyle-driven. Spotting this early makes it easier to get the right medical advice and adjust your treatment approach in a more targeted and effective way.
Other Psychiatric Medications and Acne
You may be taking medications other than lithium that can also influence your skin. Certain antipsychotics, antidepressants, and mood stabilisers have been linked to acne in some individuals, although the effect is not universal. The likelihood and severity often depend on the specific medication and your individual sensitivity.
These medications can affect the skin in different ways. Some may alter hormone levels, while others can increase oil production or trigger inflammatory pathways. Over time, this can lead to more frequent or persistent breakouts, even if your skin was previously stable.
Not everyone will experience these effects, but it is a recognised possibility. Being aware of this link helps you identify patterns early and avoid unnecessary confusion. If changes occur, it allows for a more informed discussion with your healthcare provider about how best to manage both your skin and your treatment.
Hormonal Influence of Medications
You should understand that some psychiatric medications can indirectly influence your hormone balance, even if that’s not their primary purpose. Hormones play a central role in regulating oil production and overall skin behaviour, so any shift however small can have visible effects on your skin.
Even subtle hormonal changes can increase oil production or trigger inflammation in sensitive individuals. This is why you might notice new or worsening acne after starting a medication or adjusting the dose. These changes don’t happen to everyone, but when they do, they can feel unexpected.
Monitoring how your skin responds over time is key. By paying attention to patterns and timing, you can better understand whether a medication may be contributing. This information is valuable when discussing treatment options, helping you and your healthcare provider make more informed decisions.
Inflammation and Skin Response
You may notice that medication-related acne often has a stronger inflammatory component. The skin can appear red, swollen, and more reactive than usual, sometimes with tender or deeper spots. This reflects how certain medications can trigger or amplify inflammatory pathways in the skin.
This type of acne can feel more uncomfortable and may take longer to settle compared to typical breakouts. Standard treatments don’t always work as quickly, especially if the underlying trigger such as a medication is still present. You might also notice that flare-ups persist rather than resolving on their own.
Addressing inflammation becomes a key part of management. Treatments that calm the skin, reduce redness, and control irritation are often needed alongside approaches that manage oil production. Taking this more targeted approach helps improve both comfort and overall skin recovery.
When Acne Appears After Starting Medication
You should be aware that acne can sometimes develop soon after starting a new medication. The timing is often one of the most useful clues in identifying whether a medication may be contributing. If your skin was previously stable and changes occur shortly after beginning treatment, it’s worth noting.
Breakouts may appear within a few weeks as your body adjusts to the medication. For some people, this is a temporary phase that settles over time, while for others, acne may persist if the medication continues to influence oil production or inflammation.
Tracking the timing of these changes can be very helpful. Noting when the medication started, when breakouts appeared, and how they evolve provides valuable insight. This makes it easier to have a more informed discussion with your healthcare provider and decide on the best way to manage both your skin and your treatment.
Why Some People Are More Affected
You might wonder why some people develop acne from medications while others notice no change at all. The difference usually comes down to individual factors like skin sensitivity, genetics, and your natural tendency toward oil production and inflammation. Your skin’s baseline behaviour plays a major role in how it responds to any internal or external changes.
- Genetics influence skin response: Your genetic makeup can determine how active your sebaceous glands are and how easily your skin becomes inflamed. This means some people are naturally more prone to breakouts than others.
- Pre-existing acne increases sensitivity: If you already struggle with acne, your skin may react more strongly to medication-related changes. Even small shifts in oil production or inflammation can trigger noticeable breakouts.
- Differences in oil production levels: People who naturally produce more sebum are more likely to experience clogged pores when medication alters their skin balance, even slightly.
- Variation in inflammatory response: Some skin types react more intensely to hormonal or chemical changes, leading to redness, swelling, and more visible acne.
Your baseline skin condition is a key factor in how you respond to medications. That’s why two people taking the same treatment can have completely different experiences. When you understand your own skin tendencies, you’re in a much better position to anticipate changes and manage them proactively.
The Role of Oil Production
You should know that increased oil production is a common factor in medication-related acne. Some psychiatric medications can stimulate the sebaceous glands, leading to higher levels of sebum on the skin. This shift may not always be obvious at first, but it can gradually change how your skin behaves.
When excess oil builds up, it mixes with dead skin cells and blocks pores more easily. This creates the ideal environment for acne-causing bacteria to grow, increasing the likelihood of inflamed breakouts. Over time, this can lead to more persistent or widespread acne.
Controlling oil production becomes a key focus in treatment. By reducing excess sebum and keeping pores clear, it’s possible to limit breakouts and improve overall skin balance. This targeted approach helps manage symptoms more effectively, especially when medication remains part of your routine.
Identifying Medication-Related Acne
You may find it helpful to consider whether your acne began or worsened after starting or changing a medication. A sudden onset, especially if your skin was previously stable, can be a strong indicator that the medication may be contributing.
However, it’s important not to look at this in isolation. Other factors such as stress, hormonal shifts, diet, or changes in your skincare routine can also influence your skin. These can overlap, making it less straightforward to pinpoint a single cause.
A thorough assessment helps bring clarity. Looking at timing, patterns, and any accompanying changes allows for a more accurate understanding of what’s driving your acne. Once the cause is identified, it becomes much easier to choose the right management approach and achieve better, more consistent results.
Should You Stop the Medication?

You should never stop psychiatric medication without medical advice. These treatments are prescribed to manage important mental health conditions, and stopping them suddenly can lead to serious consequences or a return of symptoms.
If you’re concerned about acne, the best approach is to discuss it with your healthcare provider. They can assess whether the medication may be contributing and explore safe options. This might include adjusting the dose, switching to an alternative, or adding targeted acne treatment to manage the side effects.
Your overall health always comes first. Managing your mental health and your skin should go hand in hand, not compete. With the right guidance, it’s usually possible to find a balanced approach that supports both.
Managing Acne Without Stopping Treatment
You may be able to manage acne effectively without changing your medication. In many cases, targeted skincare and appropriate medical treatments can control breakouts while you continue your prescribed therapy. This is often the preferred approach, as it avoids disrupting your mental health treatment.
Topical treatments, oil-control strategies, and anti-inflammatory options can help reduce breakouts and improve skin stability. In some situations, a healthcare provider may also recommend additional medications specifically for acne. These can be tailored to work alongside your existing treatment safely.
This balanced approach allows you to support both your skin and your mental health at the same time. Rather than choosing one over the other, the goal is to create a plan that addresses both effectively. With the right guidance, it’s usually possible to achieve clearer skin without compromising your overall wellbeing.
Topical Treatments for Control
You may benefit from topical treatments that help control both oil production and inflammation. Options like retinoids, benzoyl peroxide, or other prescribed formulations work directly on the skin to keep pores clear and reduce the formation of new breakouts. These treatments are usually tailored to your skin type and how severe your acne is, so the approach can be adjusted to suit your needs.
- They keep pores clear: Retinoids help speed up skin cell turnover, which prevents dead skin cells from building up and blocking your pores. This reduces the chances of new spots forming.
- They reduce bacteria and inflammation: Benzoyl peroxide helps target acne-causing bacteria while also calming inflammation. This can make active breakouts less red and less severe.
- They improve overall skin texture: With consistent use, these treatments can help smooth uneven skin and reduce the frequency of flare-ups over time.
- They require consistency to work: Results don’t appear overnight. You’ll usually need to use them regularly for several weeks before noticing clear improvements, so sticking with the routine is important.
Topical treatments are often the first step in managing medication-related acne and can form the foundation of a wider treatment plan. When used consistently and correctly, they can make a noticeable difference in both the appearance and behaviour of your skin over time.
When Oral Treatments Are Needed
You should consider additional treatment if your acne becomes more severe or does not respond to topical care alone. In these cases, oral medications may be recommended to help control inflammation, reduce bacteria, or regulate oil production more effectively.
These treatments are always tailored to your individual needs, taking into account your skin condition, medical history, and current medications. When prescribed and monitored properly, they can be used safely alongside psychiatric medications. Coordination between healthcare providers ensures that both treatments work well together.
A combined approach often delivers the best results. By addressing acne from both inside and outside the body, you improve the chances of gaining control over breakouts while maintaining your overall health and wellbeing.
The Importance of Gentle Skincare

You should adopt a gentle skincare routine if you are experiencing medication-related acne. It can be tempting to use strong or harsh products to “dry out” breakouts, but this often backfires by increasing irritation and inflammation. When the skin barrier is disrupted, it can actually lead to more oil production and worsening acne.
Using non-comedogenic, fragrance-free, and soothing products helps maintain balance in your skin. Gentle cleansers, light moisturisers, and calming ingredients can support healing without clogging pores or triggering further irritation. This creates a more stable environment for your skin to recover.
Simple routines are often the most effective. Sticking to a few well-chosen products consistently is usually better than constantly changing or overloading your routine. This approach helps reduce flare-ups and supports long-term skin health.
Monitoring Skin Changes Over Time
You may find it helpful to track how your skin changes over time, especially when dealing with medication-related acne. Noting when breakouts occur, how severe they are, and how they respond to different treatments can give you a clearer picture of what’s happening. Patterns often emerge that aren’t obvious day to day.
Keeping a simple record such as photos, notes, or a routine log can make these changes easier to recognise. This becomes particularly valuable when speaking with a specialist, as it provides real, detailed insight into your skin’s behaviour rather than relying on memory alone.
Awareness helps guide better decisions. When you understand how your skin responds, you can adjust your routine or treatment more effectively. Over time, this leads to more consistent control and improved skin health.
Emotional Impact of Acne
You may find it helpful to track how your skin changes over time, particularly when managing medication-related acne. Noting when breakouts occur, how severe they are, and how they respond to different treatments can give you a clearer understanding of what’s happening. Patterns often emerge gradually and may not be obvious in day-to-day observation.
Keeping a simple record such as photos, notes, or a routine log can make these patterns easier to recognise. This information becomes especially valuable when discussing your condition with a specialist, as it provides accurate insight into how your skin behaves over time rather than relying on memory alone.
Awareness helps guide better decisions. When you understand how your skin responds, you can make more informed adjustments to your routine or treatment plan. Over time, this leads to more consistent control and healthier, more stable skin.
Long-Term Outlook for Skin Health
You may be reassured to know that medication-related acne can often be effectively managed and brought under control. With the right combination of treatments and support, symptoms frequently improve over time, even if the triggering medication remains part of your routine.
In many cases, skin becomes more stable as your body adjusts and as targeted treatments begin to take effect. This improvement is usually gradual rather than immediate, and consistency with your skincare and medical plan plays an important role in achieving lasting results.
While individual responses vary, improvement is absolutely achievable with the right approach. With ongoing care and appropriate guidance, many people are able to significantly reduce breakouts and maintain clearer, more balanced skin in the long term.
When to Seek Specialist Advice

You should seek professional advice if your acne becomes persistent, severe, or difficult to manage despite following your current routine. When breakouts continue over time, it can be a sign that underlying factors such as medication, hormones, or inflammation need a more detailed assessment. Getting the right input early can help prevent the issue from becoming more difficult to control later on.
- Persistent breakouts that don’t improve: If your acne continues despite consistent skincare and treatment, it may indicate that a deeper trigger needs to be addressed. This is often the point where self-management alone is no longer enough.
- Possible medication or hormonal involvement: A specialist can help identify whether your medication or hormonal changes are contributing to your symptoms. This ensures the root cause is properly understood rather than just treating the surface.
- Access to targeted treatment options: Based on your assessment, you may be offered prescription treatments, tailored skincare, or adjustments to your current plan. These are designed to better match your specific skin needs.
- Prevention of long-term skin damage: Early support can reduce the risk of scarring, ongoing inflammation, and prolonged discomfort. Acting sooner often leads to better and more stable long-term results.
Seeking specialist advice isn’t just about treating acne once it becomes severe it’s about managing it effectively before it escalates. With the right guidance, you can achieve clearer skin and a more controlled, sustainable treatment plan.
Understanding the Bigger Picture
You should view medication-related acne as just one part of your overall health rather than an isolated issue. While it can be frustrating, it’s important to remember that your mental health treatment and physical wellbeing both play essential roles in your quality of life.
A balanced approach ensures that neither aspect is overlooked. Managing your skin effectively while continuing necessary psychiatric medication allows you to maintain stability in both areas. This often involves combining medical guidance, skincare strategies, and ongoing monitoring to find what works best for you.
Looking at the bigger picture supports more sustainable, long-term success. When both mental and skin health are addressed together, it becomes easier to maintain overall wellbeing and make informed, confident decisions about your care.
FAQs:
1. Can lithium and other psychiatric medications cause acne?
Yes, some psychiatric medications like lithium can trigger or worsen acne in certain people. They may increase oil production or promote inflammation in the skin. However, not everyone will experience these side effects. The severity depends on your individual skin sensitivity and dosage.
2. Why does lithium cause acne?
Lithium is thought to increase inflammatory activity and stimulate the oil glands. This can lead to blocked pores and more frequent breakouts. The acne may appear suddenly and progress quickly in some cases. It often requires targeted treatment to manage effectively.
3. What does medication-related acne look like?
It often appears as red, inflamed spots or pustules rather than blackheads or whiteheads. You may notice more widespread breakouts on the face, chest, or back. The spots can feel tender or irritated. It may also flare repeatedly over time.
4. Can antidepressants or antipsychotics also cause acne?
Yes, some antidepressants, antipsychotics, and mood stabilisers have been linked to acne. The effect varies depending on the medication and your skin type. These drugs may influence hormones, oil production, or inflammation. Not everyone will experience skin changes.
5. Should you stop psychiatric medication if you develop acne?
No, you should never stop psychiatric medication without medical advice. These medications are essential for mental health stability. Stopping them suddenly can cause serious health risks. Instead, you should speak to your doctor about managing the side effect safely.
6. How is medication-related acne treated?
It is usually managed with topical treatments, oral medications, or a combination of both. Treatments focus on reducing oil, inflammation, and bacteria in the skin. In many cases, acne can be controlled without changing your psychiatric medication. A tailored plan gives the best results.
7. Why do some people get acne and others don’t?
It depends on your genetics, hormone balance, and skin sensitivity. If you already have acne-prone skin, you may be more likely to react. Oil production levels and inflammatory response also play a role. This is why reactions vary so much between individuals.
8. How long does medication-related acne last?
It can appear shortly after starting a medication and may continue while you’re taking it. In some people, the skin adjusts over time, while in others it persists. Treatment can help control symptoms during this period. Early management usually leads to better outcomes.
9. What treatments work best for lithium-related acne?
Topical retinoids and benzoyl peroxide are commonly used first-line treatments. These help unclog pores, reduce bacteria, and calm inflammation. In more severe cases, oral treatments may be needed. A dermatologist will tailor treatment to your skin.
10. When should you see a specialist for acne?
You should seek help if your acne is persistent, worsening, or not improving with treatment. A specialist can check whether medication or hormones are contributing. They can also offer prescription-strength options. Early treatment helps prevent scarring and long-term skin damage.
Final Thoughts: Managing Acne While Staying on Treatment
If you’ve noticed acne developing after starting lithium or another psychiatric medication, it can feel frustrating, especially when you’re trying to manage your mental health at the same time. The important thing to remember is that this type of acne is relatively common and doesn’t mean you need to stop your medication. In most cases, it can be managed effectively once the cause is understood.
What really helps is recognising the pattern early and working with a healthcare professional to tailor your skin treatment. With the right combination of topical or oral treatments and a gentle skincare routine, you can usually bring breakouts under control while continuing your prescribed medication safely. It’s all about balancing both aspects of your health rather than choosing one over the other. If you’re considering acne treatment London, you can get in touch with us at London Dermatology Centre.
References:
- Nanavaty, M.A. & Daya, S.M. (2012) ‘Refractive lens exchange versus phakic intraocular lenses’, Current Opinion in Ophthalmology, 23(1), pp. 54-61. https://pmc.ncbi.nlm.nih.gov/articles/PMC3080563/
- Kaweri, L., Wavikar, C., James, E., Pandit, P. & Bhuta, N. (2020) ‘Review of current status of refractive lens exchange and role of dysfunctional lens index as its new indication’, Indian Journal of Ophthalmology, 68(12), pp. 2797-2803. https://pmc.ncbi.nlm.nih.gov/articles/PMC5429107/
- Kim, E.J., Sajjad, A., Montes de Oca, I., Koch, D.D., Wang, L., Weikert, M.P. & Al-Mohtaseb, Z.N. (2017) ‘Refractive outcomes after multifocal intraocular lens exchange’, Journal of Cataract & Refractive Surgery, 43(6), pp. 761-766. https://pubmed.ncbi.nlm.nih.gov/28220628/
- Alió, J.L., Mulet, M.E., Shalaby, A.M. & Attia, W.H. (2016) ‘Phakic intraocular lenses and refractive lens exchange for correction of high myopia’, Canadian Journal of Ophthalmology, 51(6), pp. e201-e207. https://pubmed.ncbi.nlm.nih.gov/27529209/
- Koch, W., Zagórska, J., Michalak-Tomczyk, M., Karav, S. & Wawruszak, A. (2024) ‘Plant phenolics in the prevention and therapy of acne: a comprehensive review’, Molecules, 29(17), p. 4234. https://www.mdpi.com/1420-3049/29/17/4234