After pregnancy, your body goes through a major transition as your hormone levels shift and your immune system readjusts. These internal changes can have a noticeable effect on your skin, sometimes leading to new concerns or making existing conditions more visible. You may find these changes unexpected, especially during an already demanding time.
Your skin can respond in different ways depending on your hormones, genetics, and overall health. You might notice increased oiliness and breakouts, or instead experience dryness, sensitivity, or changes in pigmentation. These variations are a normal part of your body adjusting after childbirth.
In this article, you will explore the most common postpartum skin changes, why they happen, and how dermatologists diagnose and manage them. Understanding what’s happening to your skin can help you feel more in control and manage these changes more effectively.
Hormonal Shifts After Pregnancy
After childbirth, your levels of oestrogen and progesterone drop significantly. These hormonal changes affect many systems in your body, including your skin. The sudden shift can influence oil production, hydration, and inflammation, which may lead to noticeable changes.
During pregnancy, higher oestrogen levels often help keep your skin smoother and more hydrated. After delivery, this hormonal support decreases, which can leave your skin feeling drier or less balanced. You may notice that your skin behaves quite differently compared to how it did during pregnancy.
These hormonal adjustments are a natural part of your body returning to its pre-pregnancy state. This transition can take several weeks or even months. Understanding this process helps you make sense of the changes you are experiencing in your skin.
Postpartum Acne
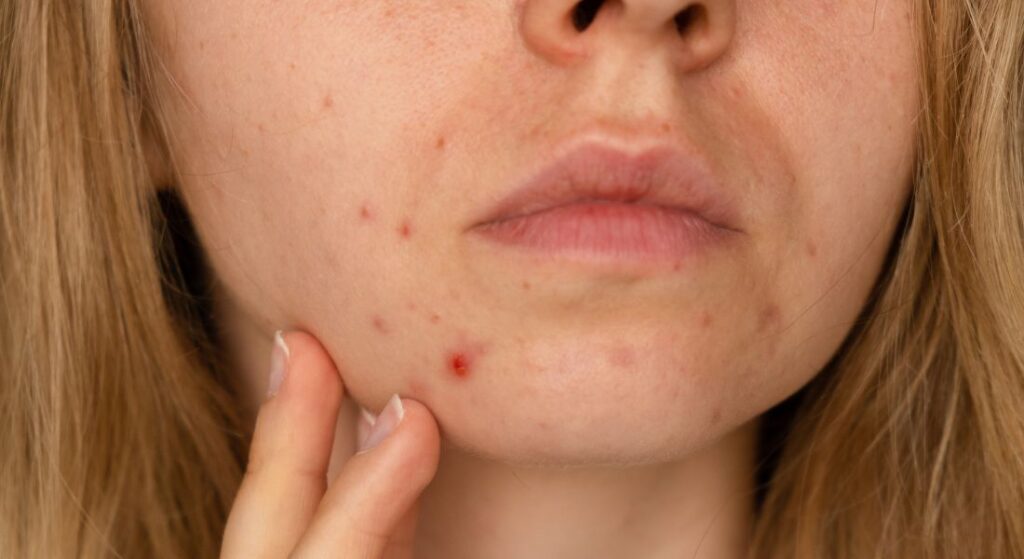
Many women experience acne after pregnancy, even if they have never had it before. Hormonal fluctuations can increase your skin’s oil production, which may lead to clogged pores and breakouts. You may notice this acne appearing more commonly along your lower face and jawline.
Inflammation also plays a role in postpartum acne. After childbirth, changes in your immune system can affect how your skin responds to bacteria. As a result, your breakouts may feel more persistent or harder to manage during this period.
Your dermatologist may recommend gentle treatments that are safe if you are breastfeeding. Focusing on controlling oil production and reducing inflammation can help improve your symptoms. Starting treatment early can also help prevent long-term scarring.
Skin Dryness and Sensitivity
You may notice that your skin becomes drier after pregnancy. Lower oestrogen levels can reduce your skin’s ability to retain moisture, which may lead to tightness, flaking, or increased sensitivity. These changes are common as your body adjusts after childbirth.
Your skin barrier can also become more reactive during this time. Products that previously suited you may suddenly cause irritation or discomfort. External factors such as weather or pollution can make this sensitivity more noticeable.
Using gentle, hydrating skincare products can help restore balance to your skin. You should try to avoid harsh ingredients that may worsen irritation. Supporting your skin barrier is an important part of recovery during the postpartum period.
Postpartum Pigmentation Changes
You may notice that pigmentation changes developed during pregnancy continue after childbirth. Conditions such as Melasma can remain visible for some time, often appearing as darker patches on your face. These changes are closely linked to hormonal fluctuations.
Sun exposure can make this pigmentation more noticeable. Even after your hormone levels begin to stabilise, it may take time for these patches to fade. Using consistent sun protection is essential to prevent further darkening.
Your dermatologist may recommend topical treatments to help reduce pigmentation gradually. Improvement usually takes time rather than happening immediately. Being patient and consistent with your skincare routine can help you achieve better results.
Stretch Marks and Skin Texture Changes
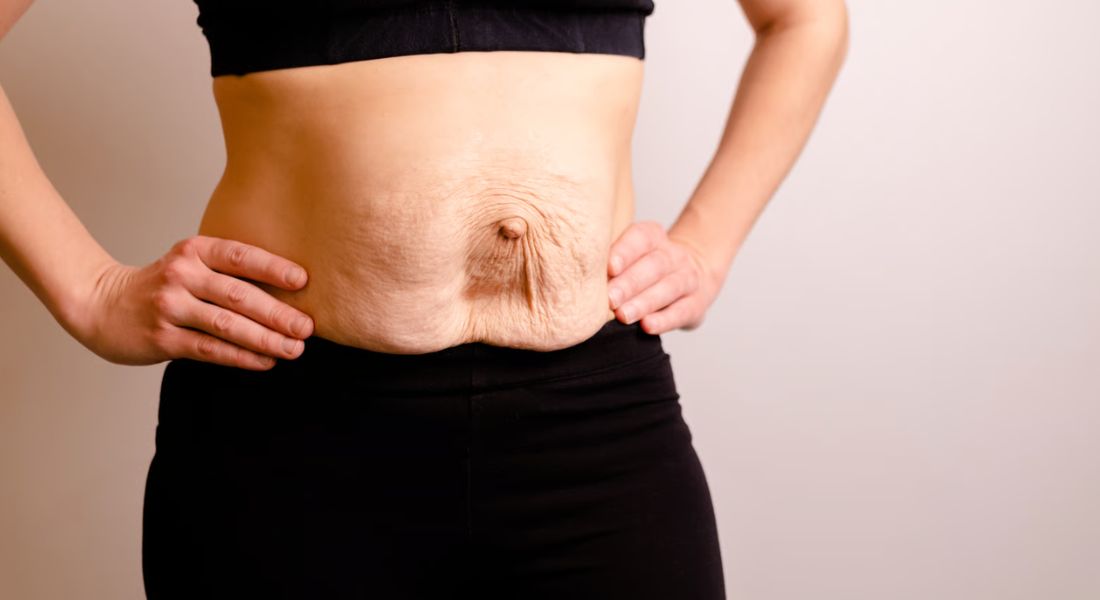
Stretch marks are a common skin change during and after pregnancy. They develop as your skin stretches to accommodate physical changes, particularly around the abdomen, hips, and thighs. After childbirth, you may notice that these marks begin to change in both colour and texture. Although they may appear prominent at first, they often become less noticeable over time as your skin gradually recovers. You may also observe changes in how firm or smooth your skin feels in certain areas.
- How stretch marks develop: Stretch marks form when the deeper layers of your skin are stretched beyond their usual limits. This affects collagen and elastin fibres, which are responsible for keeping your skin firm and elastic. As a result, lines or streaks appear on the surface of the skin.
- Changes in colour and texture over time: Initially, stretch marks may look red, purple, or darker than your surrounding skin. Over time, they usually fade to a lighter, silvery tone. The texture may also soften, making them less noticeable, although they may not disappear completely.
- Looser or less firm skin: After pregnancy, you may notice that your skin feels looser in areas that were stretched. This is due to changes in collagen and elastin during pregnancy. The degree of recovery varies from person to person, depending on factors such as skin type and overall health.
- Treatment options for improvement: Dermatological treatments can help improve the appearance of stretch marks. These may include topical therapies, as well as procedures designed to support collagen production. Results usually develop gradually over time, rather than immediately.
Although stretch marks and texture changes are very common, they often improve naturally as your body recovers. With the right care and, if needed, professional guidance, you can support your skin’s gradual return to a more even and comfortable state.
Hair Loss and Its Impact on the Skin

Postpartum hair loss is a common and often temporary change that occurs after childbirth. It is mainly caused by hormonal shifts as your body adjusts after pregnancy. While the hair shedding itself affects the scalp, you may also notice subtle changes in the skin around your hairline. This area can sometimes feel more sensitive, dry, or slightly different in texture during this period. Understanding why this happens can help you manage it with more confidence and less concern.
- Changes in the hair growth cycle: During pregnancy, higher hormone levels keep more of your hair in the growth phase for longer. This is why your hair may have felt thicker or fuller. After childbirth, hormone levels drop, and many hairs move into the shedding phase at the same time, leading to noticeable hair loss.
- Impact on the scalp and hairline skin: As shedding increases, the scalp and skin around your hairline may feel more exposed or sensitive. You might notice mild dryness, tenderness, or a change in how your skin reacts to products. These changes are usually temporary and improve as your hair cycle stabilises.
- Temporary nature of postpartum hair loss: Although hair shedding can feel alarming, it is typically short-lived. Most people see improvement within a few months as the hair growth cycle returns to normal. The skin around the scalp also tends to recover as hormone levels settle.
- Supporting scalp and skin health: Gentle care is important during this phase. Using mild shampoos, avoiding harsh treatments, and keeping the scalp well-hydrated can help maintain comfort. Dermatologists can offer reassurance and recommend suitable products if you have concerns.
Postpartum hair loss can feel unsettling, but it is a normal part of recovery after pregnancy. With time and proper care, both your hair and the surrounding skin usually return to their usual state.
Changes in Oil Production
After pregnancy, hormonal fluctuations can affect how much oil your skin produces. You may notice that your skin becomes oilier than usual, or in some cases, much drier. These changes can shift over time as your body continues to adjust during the postpartum period.
If your skin produces more oil, you may experience clogged pores and breakouts. On the other hand, reduced oil production can leave your skin feeling dry, tight, or more sensitive. It can take some time for your skin to find its natural balance again.
Adjusting your skincare routine can help you manage these changes more effectively. Using products suited to your current skin type is important during this stage. Your dermatologist can guide you in choosing the right approach for your skin.
Eczema and Dermatitis Flare-Ups
After pregnancy, you may notice that existing skin conditions such as eczema or dermatitis become more active. Hormonal shifts and changes in your immune system can trigger flare-ups during this time. In addition, factors like stress, fatigue, and disrupted sleep can make symptoms feel more intense or harder to control. These flare-ups can vary in severity, but recognising the signs early helps you manage them more effectively.
- Common symptoms to watch for: You may experience increased itching, redness, dryness, or patches of irritated skin. In some cases, the skin can feel tight, rough, or inflamed. These symptoms may appear in areas where eczema has occurred before or in new areas.
- Role of hormonal and lifestyle factors: After childbirth, hormonal changes can affect your skin’s barrier function and immune response. At the same time, stress and lack of sleep can further weaken the skin’s ability to protect itself. Together, these factors can trigger or worsen flare-ups.
- Importance of managing triggers: Identifying and avoiding triggers is an important part of controlling symptoms. Triggers may include harsh skincare products, temperature changes, or certain fabrics. Keeping your routine simple and consistent can help reduce irritation.
- Treatment and skincare support: Dermatologists may recommend treatments that are safe and suitable for your situation, especially if you are breastfeeding. Gentle skincare, regular moisturisation, and prescribed treatments when needed can help calm inflammation and restore the skin barrier.
Although eczema flare-ups can be uncomfortable, they can usually be managed with the right approach. Early care, combined with consistent skincare, can improve comfort and help keep your skin more stable during the postpartum period.
Psoriasis Changes After Pregnancy
Psoriasis symptoms can change noticeably after childbirth. You may find that your skin improved during pregnancy, only to experience flare-ups in the postpartum period. These shifts are linked to hormonal changes that influence your immune system activity.
Psoriasis typically appears as red, scaly patches on the skin, and flare-ups can vary in severity. Some people notice mild changes, while others experience more persistent symptoms. Keeping track of these changes can help you understand your triggers and patterns.
Dermatologists adjust treatment plans based on your individual needs, especially during the postpartum phase. Managing inflammation is a key focus of care. With the right support and ongoing monitoring, you can maintain better control and improve skin stability over time.
Increased Skin Sensitivity
After pregnancy, your skin can become more sensitive as hormone levels shift. This can temporarily weaken your skin barrier, making it more reactive than usual. As a result, your skin may respond more strongly to products or environmental factors that never bothered you before.
You might notice increased redness, stinging, or irritation. Ingredients such as fragrance, alcohol, or strong actives can feel uncomfortable during this time. These changes are usually temporary and tend to improve as your body gradually rebalances.
Switching to a gentle, minimal skincare routine can help reduce irritation. Focus on soothing and hydrating products that support your skin barrier. Dermatologists often recommend keeping things simple while your skin recovers, allowing it to regain its natural resilience.
The Role of the Immune System
During and after pregnancy, your immune system goes through important changes. These adjustments help support the developing baby, but they can also influence how your skin behaves. After childbirth, your immune system gradually returns to its usual state, and this transition can affect existing or new skin conditions. As your body readjusts, you may notice changes in inflammation and skin sensitivity.
- Immune system adaptation during pregnancy: During pregnancy, your immune system shifts to protect both you and your baby. This altered response can sometimes improve certain inflammatory skin conditions. However, it may also mask symptoms that return later.
- Postpartum immune reset: After childbirth, your immune system begins to return to its normal balance. This transition can trigger changes in how your skin reacts. Some conditions may reappear or become more noticeable during this phase.
- Impact on inflammatory skin conditions: Conditions such as eczema, acne, or other inflammatory disorders may either improve or worsen. The response varies from person to person, depending on how their immune system readjusts. This unpredictability is a normal part of postpartum recovery.
- Importance of personalised care: Dermatologists take these immune changes into account when assessing your skin. Understanding the role of the immune system helps guide diagnosis and treatment choices. Personalised care ensures that your treatment plan matches your specific needs.
Although these changes can feel unpredictable, they are part of your body’s natural recovery process. With the right guidance and support, you can manage your skin more effectively as your immune system stabilises.
Impact of Stress and Sleep Deprivation
The postpartum period often brings major lifestyle changes, including less sleep and higher stress levels. These factors can have a direct effect on your skin. When your body is under stress, it releases hormones that can increase inflammation and trigger breakouts or sensitivity. At the same time, disrupted sleep can make it harder for your skin to repair itself properly. Although these changes are common, understanding their impact can help you manage your skin more effectively.
- Stress and its effect on the skin: Increased stress can raise levels of cortisol, a hormone that influences oil production and inflammation. This may lead to more frequent breakouts, redness, or flare-ups of existing skin conditions. Your skin may also feel more reactive during stressful periods.
- Reduced sleep and slower skin repair: Sleep plays an important role in skin regeneration. When you are not getting enough rest, your skin may take longer to heal and recover. You might notice a dull or tired appearance, along with reduced brightness and uneven texture.
- Visible changes in skin appearance: A combination of stress and sleep deprivation can make your skin look less refreshed. Dark circles, dryness, or a lack of radiance may become more noticeable. These changes are usually temporary but can affect how your skin feels day to day.
- Supporting skin through lifestyle adjustments: Managing stress and improving sleep, even in small ways, can support better skin health. Simple steps such as short rest periods, staying hydrated, and maintaining a gentle skincare routine can help. These lifestyle adjustments work alongside any medical treatments you may be using.
While it may not always be possible to avoid stress or sleep disruption during this time, small changes can still make a difference. By supporting your overall wellbeing, you also support your skin’s ability to recover and stay balanced.
Safe Treatments While Breastfeeding
It’s completely understandable to be cautious about skincare treatments while breastfeeding. Certain medications and active ingredients are not recommended during this time, as they may pass into breast milk. This makes safety an important part of any treatment decision.
Dermatologists can guide you towards treatments that are considered safe during breastfeeding. These often include specific topical therapies that have minimal absorption into the bloodstream. The goal is to manage your skin concerns effectively while ensuring no risk to your baby.
Discussing your options with a specialist is essential before starting any new treatment. This helps you avoid unnecessary risks and ensures that your care is both safe and appropriate. With the right guidance, you can manage your skin confidently while supporting both your health and your baby’s wellbeing.
Skincare During the Postpartum Period

Adapting your skincare routine after pregnancy can make a noticeable difference in how your skin feels and behaves. During this time, focusing on gentle cleansing and proper hydration is essential. Avoiding harsh treatments or strong active ingredients helps reduce the risk of irritation.
Choosing products designed for sensitive skin can improve comfort and support your skin barrier. Consistency is key, as regular care helps maintain balance while your skin adjusts. Dermatologists may recommend tailored routines based on your specific concerns, whether that’s dryness, acne, or sensitivity.
Keeping your routine simple is often the most effective approach during the postpartum period. Using too many products can overwhelm your skin and lead to further irritation. A balanced, minimal routine supports recovery and helps your skin gradually return to a more stable state.
Long-Term Skin Recovery
Postpartum skin changes often improve gradually as your hormone levels begin to stabilise. Over time, your body works towards returning to its pre-pregnancy state, and your skin follows this process. The pace of recovery can vary from person to person.
Some changes may resolve within a few months, while others can take longer or may need targeted treatment to improve. It’s important to be patient, as your skin needs time to rebalance and repair itself naturally.
Long-term care focuses on maintaining overall skin health. Sticking to a consistent routine and seeking professional guidance when needed can support recovery. By monitoring your skin over time, you can make informed adjustments and achieve more stable, lasting results.
Psychological Impact of Skin Changes
Visible changes in your skin during the postpartum period can affect how you feel about yourself. As your body recovers after childbirth, adjusting to these changes may feel challenging at times. It is completely normal for your confidence to fluctuate, especially when changes appear suddenly or persist longer than expected. Recognising the emotional side of skin concerns is an important part of overall recovery. Understanding what is happening can help you feel more in control and reassured.
- Impact on confidence and self-image: Changes such as acne, pigmentation, or dryness may make you feel less confident in your appearance. You might feel self-conscious in social situations or daily interactions. These feelings are common and often improve as your skin recovers.
- Emotional response to physical changes: Adjusting to visible skin changes can sometimes feel overwhelming, especially alongside other postpartum adjustments. You may feel frustrated or concerned if improvements take time. Acknowledging these emotions is an important step in managing them.
- Reassurance through understanding and support: Knowing that many postpartum skin changes are temporary can provide comfort. Speaking with a healthcare professional can help you understand what to expect and how to manage symptoms. Early guidance can reduce uncertainty and improve confidence.
- Holistic approach to care: Looking after both your skin and your emotional wellbeing is essential. Dermatological care, combined with emotional support, helps you feel more balanced. As your skin improves with time and treatment, your confidence often begins to return.
Postpartum recovery is not just physical it also includes emotional adjustment. By seeking support and taking a balanced approach to care, you can manage skin changes more effectively and feel more confident as your body continues to heal.
When to Seek Dermatological Advice
If your skin changes persist, worsen, or start to affect your daily comfort, it’s important to seek professional advice. A dermatologist can assess your symptoms and recommend appropriate treatment based on your individual needs. Early intervention often leads to better and faster outcomes.
Some postpartum skin conditions may require medical management rather than over-the-counter solutions. Ignoring ongoing symptoms can sometimes lead to complications or prolonged recovery. Getting an accurate diagnosis ensures you receive the right care from the start.
A consultation also allows for a personalised treatment plan that takes into account hormonal and immune changes after pregnancy. With expert guidance, you can manage your skin more effectively and support a smoother recovery.
Advances in Postpartum Dermatology
Research into postpartum skin changes is continuing to expand, improving how these conditions are understood and managed. Scientists are exploring how hormonal shifts and immune responses interact with the skin during the postpartum period. These insights are helping shape more effective and targeted treatment approaches.
New therapies are being developed to focus on specific biological pathways involved in skin conditions. This more precise approach can improve treatment effectiveness while reducing unnecessary side effects. As a result, care is becoming increasingly personalised.
Ongoing research is providing better options for patients dealing with postpartum skin concerns. Future treatments are likely to offer even greater precision and improved outcomes. As dermatology continues to evolve, you can expect more advanced and supportive care during the postpartum period.
Individual Variation in Skin Changes
Every person experiences postpartum skin changes differently. Your genetics, lifestyle, and overall health all influence how your skin responds after pregnancy. You may notice only minor changes, while others experience more noticeable or persistent concerns.
Understanding that this variation is completely normal can help reduce unnecessary worry. Comparing your skin to someone else’s experience is not always helpful, as no two postpartum journeys are the same. Your skin will follow its own pattern of recovery.
Dermatologists focus on tailoring treatment to your specific needs rather than taking a one-size-fits-all approach. This ensures that your concerns are managed effectively. Individualised care plays a key role in achieving better and more consistent outcomes.
Why Understanding Postpartum Skin Changes Matters
Understanding postpartum skin changes allows you to manage your skin more effectively during this transitional period. When you recognise patterns and triggers, you can respond proactively rather than reacting after symptoms appear. This often leads to more consistent and improved results.
Dermatologists use this understanding to guide treatment decisions and address the underlying causes of your skin concerns. By focusing on what is driving the changes, care becomes more targeted and effective. This approach helps improve overall outcomes.
When you understand what your skin is going through, you can make more informed decisions about your skincare and treatment options. This knowledge builds confidence and reduces uncertainty. With the right approach, effective management can significantly improve your comfort and quality of life.
FAQs:
1. Why does your skin change after pregnancy?
Your skin changes after pregnancy because your hormone levels, particularly oestrogen and progesterone, drop significantly following childbirth. These hormonal shifts affect oil production, hydration, and inflammation, which can lead to noticeable differences in how your skin looks and feels.
2. Is postpartum acne normal even if you never had acne before?
Yes, it is completely normal to develop acne after pregnancy, even if you have never experienced it before. Hormonal fluctuations can increase oil production and trigger inflammation, which may lead to breakouts, particularly around the jawline and lower face.
3. How long do postpartum skin changes usually last?
Postpartum skin changes can last anywhere from a few weeks to several months, depending on how quickly your hormone levels stabilise. In some cases, certain conditions may take longer to resolve or may require treatment to improve.
4. Why does your skin feel drier after giving birth?
Your skin may feel drier after childbirth because oestrogen levels decrease, which reduces your skin’s ability to retain moisture. This can lead to dryness, tightness, and increased sensitivity, especially in the early postpartum period.
5. Can pregnancy pigmentation go away on its own?
Yes, pigmentation such as melasma may gradually fade on its own after pregnancy as hormone levels return to normal. However, this process can take time, and sun exposure may slow improvement, which is why consistent sun protection is important.
6. Is postpartum hair loss related to skin health?
Postpartum hair loss is primarily related to hormonal changes affecting the hair growth cycle, but it can also influence the scalp and surrounding skin. You may notice increased sensitivity or changes in the skin around the hairline during this time.
7. Can existing skin conditions get worse after pregnancy?
Yes, conditions such as eczema or psoriasis can worsen after pregnancy due to hormonal and immune system changes. You may notice flare-ups during the postpartum period, especially if combined with stress or lack of sleep.
8. What skincare routine should you follow after pregnancy?
After pregnancy, it is best to follow a simple and gentle skincare routine that focuses on hydration and barrier repair. Using mild cleansers and avoiding harsh ingredients can help your skin recover while reducing the risk of irritation.
9. Are skincare treatments safe while breastfeeding?
Some skincare treatments are safe while breastfeeding, but others may not be recommended. It is important to consult a dermatologist before starting any new treatments so that you can ensure they are appropriate and safe for both you and your baby.
10. When should you see a dermatologist for postpartum skin issues?
You should consider seeing a dermatologist if your skin concerns are persistent, worsening, or affecting your confidence. Professional advice can help you understand what is happening and provide effective, personalised treatment options.
Final Thoughts: Supporting Your Skin Through Postpartum Changes
Your skin goes through a period of adjustment after pregnancy, and these changes can sometimes feel unexpected or difficult to manage. From breakouts and dryness to pigmentation and sensitivity, each response is linked to the natural shifts in your hormones and immune system as your body recovers.
Understanding what is happening beneath the surface allows you to approach your skincare with more confidence and clarity. By keeping your routine simple, focusing on hydration, and responding to your skin’s changing needs, you can support its recovery more effectively. Over time, many of these changes will gradually improve as your body returns to balance.
If your symptoms persist or begin to affect your confidence, seeking expert guidance can make a meaningful difference. If you’re thinking about female dermatologist in London, you can contact us at London Dermatology Centre to book a consultation with one of our specialists.
References:
- Stichert, V.R., Korman, A.M. and Mostaghimi, A. (2026) ‘Managing skin diseases that flare during pregnancy and in the postpartum period: Classification, epidemiology and pathogenesis’, Journal of the American Academy of Dermatology. Available at: https://www.sciencedirect.com/science/article/abs/pii/S0190962226002422
- Alhomieed, M.F. et al. (2025) ‘The effect of pregnancy on dermatological disorders: A systematic review’, Clinics and Practice, 15(4), p. 68. Available at: https://www.mdpi.com/2039-7283/15/4/68
- Faissal Alhomieed, M. et al. (2025) ‘Hormonal and immunological influences on dermatological conditions during and after pregnancy’, Clinics and Practice, 15(4), pp. 68–75. Available at: https://www.mdpi.com/3234712
- Anzelc, M.J. and Bechtel, M.A. (2023) ‘Considerations for cutaneous physiologic changes of pregnancy that fail to resolve postpartum’, International Journal of Dermatology, 62(2), pp. 190–196. Available at: https://pubmed.ncbi.nlm.nih.gov/35132624/
- Lyons, C.E., Smith, A.D., Schwartzman, G., Buscemi, L., Hickman, A. and Grant-Kels, J.M. (2026) ‘Managing skin diseases that flare during pregnancy and in the postpartum period: Part 2 – Management and safety considerations’, Journal of the American Academy of Dermatology. Available at: https://pubmed.ncbi.nlm.nih.gov/41692217/