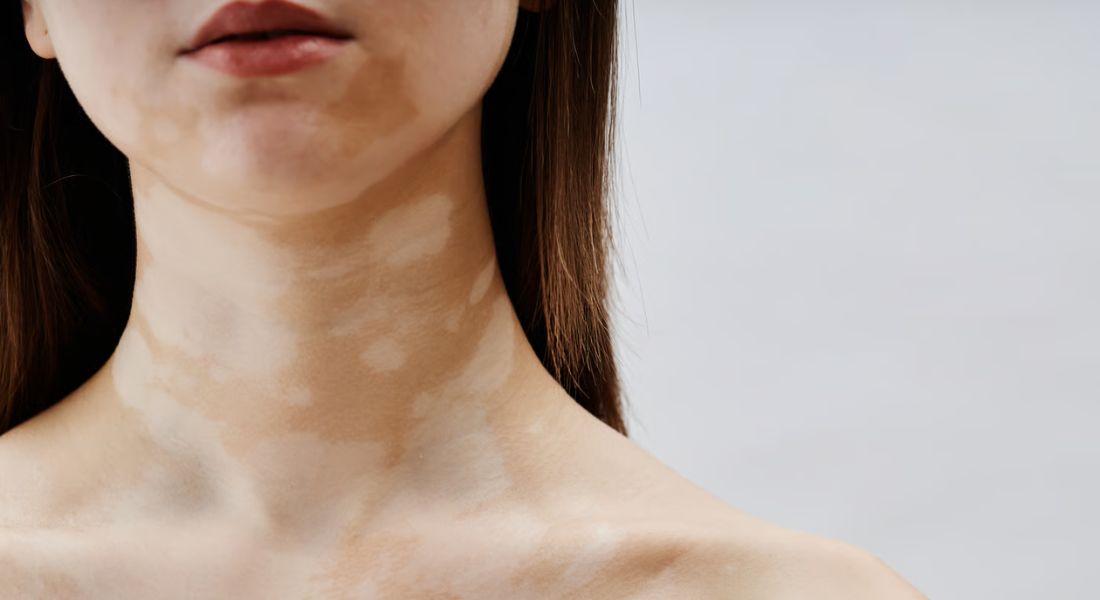
Vitiligo is a condition that many people believe disappears once the skin begins to repigment. However, this is not always the case. Even after successful treatment and visible improvement, patches of depigmentation can sometimes return months or even years later. This pattern can be confusing for patients who believed the condition had fully resolved.
If you have experienced this cycle, it is completely understandable to feel frustrated. Many people wonder why the skin seemed to recover only for pigment loss to appear again. The answer often lies deeper within the immune system. Even when the skin looks normal on the surface, certain immune cells may still remain active in the tissue.
Over the past decade, research has begun to reveal an important explanation. Scientists have identified specialised immune cells known as resident memory T cells that remain in the skin long after visible inflammation has settled. Unlike other immune cells that travel through the bloodstream, these cells stay permanently within the skin.
These cells appear to “remember” the autoimmune attack that originally destroyed pigment-producing cells. Because of this immune memory, they can reactivate the same inflammatory process in the future. In this article, I will explain what resident memory T cells are, how they contribute to vitiligo relapse, and how emerging therapies may help reduce the risk of recurrence.
Understanding Vitiligo and the Immune System
Vitiligo is an autoimmune condition in which the immune system mistakenly attacks melanocytes, the cells responsible for producing melanin. Melanin gives the skin its natural colour, so when these cells are damaged or destroyed, areas of skin lose pigment and appear white. This process creates the distinctive patches that are commonly seen in people with vitiligo.
For many years, the exact reason for this immune reaction remained unclear. Researchers understood that the immune system was involved, but the precise mechanism behind the attack was not fully known. More recent studies have shown that cytotoxic T cells, a type of immune cell responsible for destroying infected or abnormal cells, play a major role in this process.
In vitiligo, these cytotoxic T cells mistakenly identify melanocytes as harmful. The immune system then triggers inflammation in the skin, which eventually leads to the destruction of pigment-producing cells. In recent years, scientists have also identified a particular subgroup of these immune cells that may remain in the skin long after inflammation subsides, helping explain why vitiligo can sometimes return after treatment.
What Are Resident Memory T Cells?
Resident memory T cells are a specialised type of immune cell that live permanently within body tissues. Unlike many immune cells that travel through the bloodstream, these cells remain in a specific location for long periods of time. They are commonly found in areas such as the skin, lungs, and gastrointestinal tract. Their presence allows the immune system to respond quickly to threats in these tissues.
The main role of resident memory T cells is to provide long-term protection. When the body encounters an infection, some immune cells remain behind even after the infection has cleared. These cells act as local sentinels, ready to respond rapidly if the same pathogen appears again. This form of immune memory is an important defence mechanism that helps the body react faster to repeated infections.
In many situations, this system is extremely beneficial for maintaining health. However, in autoimmune conditions such as vitiligo, the same protective mechanism can become problematic. Instead of defending the body from harmful pathogens, these cells may continue to recognise normal pigment-producing cells as targets, which can contribute to the recurrence of depigmented patches.
How Resident Memory T Cells Contribute to Vitiligo
In vitiligo, the immune system mistakenly identifies melanocytes as harmful cells. During the active stage of the condition, cytotoxic T cells attack these pigment-producing cells in the affected areas of the skin. This immune reaction leads to inflammation and eventually causes the loss of pigment that appears as white patches. The process is driven by the body’s own immune defences acting against normal skin cells.
Even after treatment reduces inflammation and repigmentation begins, certain immune cells can remain behind in the skin. These are known as resident memory T cells, and they stay embedded in the same tissue where the earlier immune attack occurred. Unlike other immune cells that leave the area once the reaction subsides, these cells remain in place for long periods. Their presence means the immune system still has a local “memory” of the earlier event.
If these resident memory T cells become reactivated, they can trigger another wave of immune activity in the same area of skin. This renewed response may again target melanocytes and lead to their destruction. As a result, depigmented patches can reappear even after successful treatment. This discovery has helped researchers understand why vitiligo often relapses despite visible improvement in the skin.
Why Vitiligo Often Returns in the Same Locations
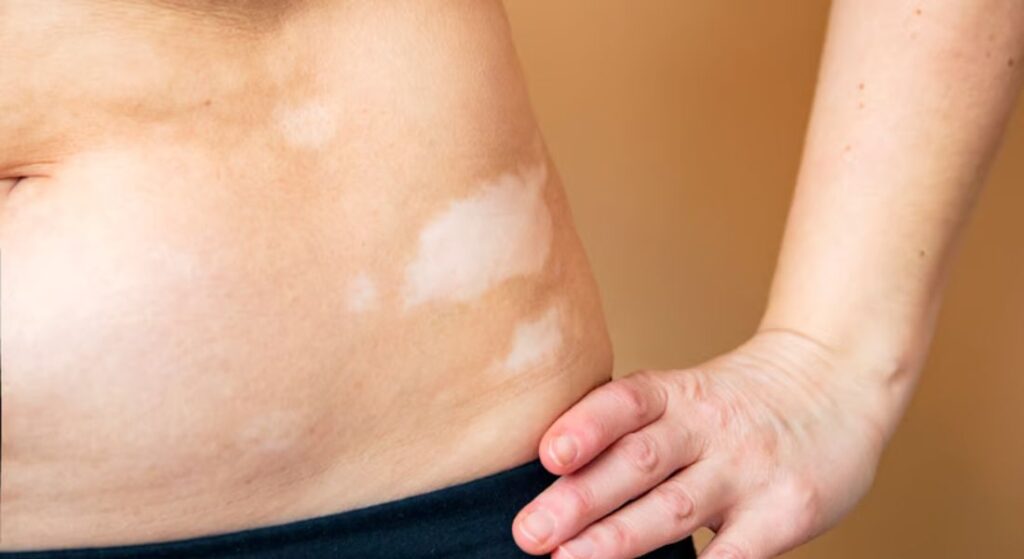
One of the most puzzling aspects of vitiligo relapse is that new depigmented patches often appear in the same areas where they previously existed. Many patients assume that once the skin has repigmented, the underlying problem has been completely resolved. However, vitiligo is closely linked to the immune system, which can retain a form of “memory” even after visible symptoms improve. Understanding this process helps explain why relapse can occur in the same regions of skin.
- Presence of Resident Memory T Cells: Certain immune cells known as resident memory T cells remain in the skin even after vitiligo patches appear to heal. These cells act like long-term sentinels within the tissue, holding information about past immune responses. Because they stay in the same location, they can trigger another immune reaction in that specific area.
- Localised Immune Reactivation: When these memory cells encounter inflammatory signals or stress triggers, they can quickly become active again. Once reactivated, they release chemical signals that alert and attract other immune cells to the same patch of skin. This local response increases the likelihood of depigmentation returning in that exact location.
- Rapid Recruitment of Additional Immune Cells: Resident memory T cells do not work alone. When activated, they recruit additional immune cells that participate in the immune attack against melanocytes. This coordinated response accelerates the destruction of pigment-producing cells in the affected skin area.
- Hidden Immune Activity Beneath the Skin: Even when the skin looks fully repigmented, the immune memory responsible for vitiligo may still remain beneath the surface. This hidden immune activity means that the skin can appear normal externally while still being vulnerable to relapse if certain triggers occur.
In conclusion, the recurrence of vitiligo in the same areas is largely explained by the persistence of immune memory within the skin. Resident memory T cells remain in previously affected locations and can reactivate when triggered by inflammation or other signals. As a result, melanocytes in those areas may once again be targeted and destroyed. Understanding this mechanism helps explain why long-term management and monitoring are important, even after successful repigmentation.
Why Standard Treatments May Not Prevent Relapse
Current vitiligo treatments mainly focus on reducing inflammation and encouraging melanocytes to return to the affected areas of skin. The aim is to calm the immune response while allowing pigment-producing cells to recover and repopulate the skin. Many patients experience visible improvement with these therapies, especially when treatment begins early and is followed consistently. However, these approaches often manage the symptoms rather than removing the underlying immune memory.
Common treatments include topical corticosteroids, calcineurin inhibitors, phototherapy, and targeted immunomodulatory medications. These therapies work by suppressing the immune activity that damages melanocytes and by stimulating repigmentation. In many cases, they can significantly reduce inflammation and restore colour to the skin over time. For this reason, they remain the mainstay of vitiligo management in clinical practice.
Despite their effectiveness, these treatments may not eliminate resident memory T cells that remain hidden within the skin. Because these cells can persist even after visible inflammation has resolved, they may gradually reactivate once treatment stops. When this happens, the immune system can once again target melanocytes, leading to the return of depigmented patches. This is one of the key reasons vitiligo sometimes relapses after therapy has been discontinued.
Phototherapy and Immune Regulation
Phototherapy, particularly narrowband UVB therapy, is considered one of the most effective treatments for vitiligo. This approach uses controlled ultraviolet light to influence the immune activity within the skin. By carefully regulating the treatment schedule, phototherapy can help reduce inflammation and create an environment that supports repigmentation. Many patients experience gradual improvement in skin colour when the therapy is followed consistently.
One of the key benefits of phototherapy is its ability to regulate immune responses while stimulating melanocyte activity. Ultraviolet light can reduce the activity of inflammatory T cells that contribute to pigment loss. At the same time, it encourages melanocytes from surrounding areas or hair follicles to migrate into depigmented patches. This dual effect helps restore colour and improve the appearance of the skin.
However, while phototherapy can effectively suppress active immune responses, it may not completely eliminate resident memory T cells that remain within the skin. These cells can persist even after repigmentation occurs and inflammation appears to have resolved. Because of this, dermatologists sometimes recommend maintenance therapy to help keep the immune system stable. Continued monitoring and occasional treatment sessions may reduce the likelihood of vitiligo returning.
The Emerging Role of JAK Inhibitors
In recent years, a group of medications known as Janus kinase (JAK) inhibitors has attracted significant attention in vitiligo research. These medicines are designed to influence specific signalling pathways that control immune system activity. By targeting these pathways, researchers hope to reduce the abnormal immune responses that damage pigment-producing cells. As a result, JAK inhibitors are being studied as a promising option for improving vitiligo treatment outcomes.
These drugs work by blocking the Janus kinase signalling pathway, which plays an important role in immune activation. In vitiligo, a key inflammatory signal called interferon-gamma stimulates immune cells to attack melanocytes. JAK inhibitors interfere with this signalling process, which can help reduce the inflammatory cascade that leads to pigment loss. By interrupting this pathway, the immune system becomes less aggressive toward melanocytes.
Early clinical studies have shown encouraging results, with some patients experiencing noticeable repigmentation during treatment. However, researchers are still investigating the long-term effects of these medications. One important question is whether JAK inhibitors can also control or suppress resident memory T cells that remain in the skin. Understanding this possibility may be crucial for developing treatments that not only restore pigment but also reduce the risk of vitiligo returning.
Targeting Interleukin-15: A Promising Future Strategy
Recent advances in vitiligo research have highlighted the role of specific immune signals that help sustain the disease. One of the most important of these signals is interleukin-15, a cytokine that supports the survival and activity of certain immune cells in the skin. Scientists are increasingly focusing on therapies that target this pathway to prevent the return of vitiligo patches. By interrupting the signals that maintain immune memory in the skin, future treatments may provide longer-lasting disease control.
- Role of Interleukin-15 in Immune Activity: Interleukin-15 is a cytokine that plays a key role in supporting the survival of resident memory T cells in the skin. These immune cells are involved in the destruction of melanocytes, the pigment-producing cells affected in vitiligo. By sustaining these cells, interleukin-15 contributes to the persistence and recurrence of the condition.
- Weakening Resident Memory T Cells: Because interleukin-15 helps these immune cells survive, blocking its activity could reduce their numbers or limit their function. This approach may weaken the immune memory responsible for vitiligo relapse, potentially preventing the same patches from reappearing.
- Evidence from Early Laboratory Studies: Initial laboratory and experimental studies suggest that interfering with the interleukin-15 pathway can significantly reduce the persistence of resident memory T cells. These findings provide important insight into how targeted therapies might control the disease more effectively in the future.
- Potential for Long-Term Disease Control: If future treatments successfully block the interleukin-15 signal, it may become possible to reduce the likelihood of vitiligo relapse. Such therapies could complement existing treatments by addressing the underlying immune mechanisms rather than just the visible skin changes.
In conclusion, targeting interleukin-15 represents one of the most promising strategies in ongoing vitiligo research. By disrupting the signals that allow resident memory T cells to survive, scientists hope to reduce the recurrence of depigmented patches. Although this research is still evolving, it offers hope for more effective and long-lasting treatment options. Continued studies may eventually lead to therapies that provide better control of vitiligo over the long term.
The Importance of Early Treatment
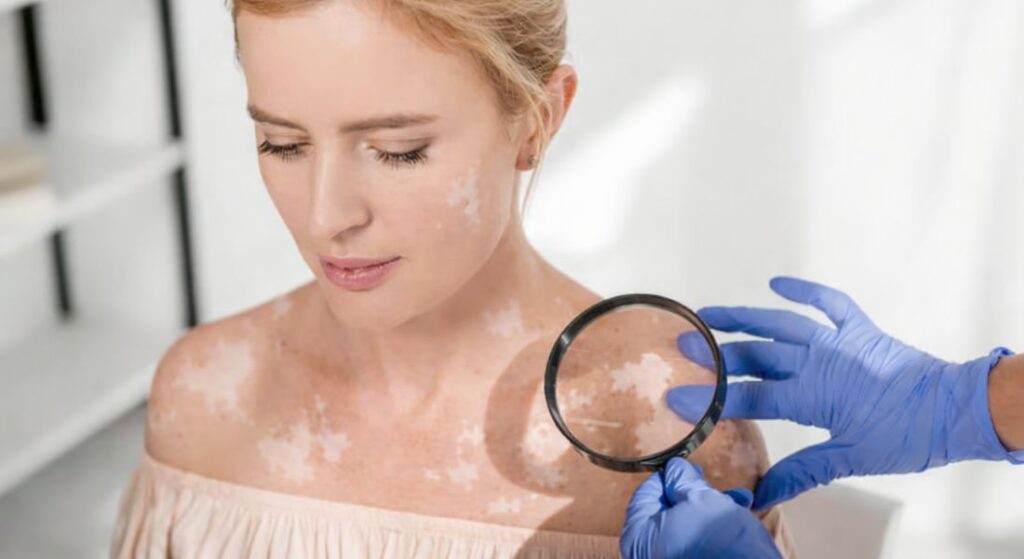
Recent research has highlighted the importance of starting treatment for vitiligo as early as possible. When the condition is addressed during its active inflammatory stage, the immune response may be easier to control. At this point, the autoimmune activity has not yet become deeply established within the skin. Early medical intervention can therefore play a key role in slowing or limiting the progression of pigment loss.
Treating vitiligo early may also reduce the number of immune cells that remain in the skin after the initial inflammation settles. In particular, it may limit the formation of resident memory T cells that can persist in affected areas for long periods. These cells are believed to contribute to future relapses because they retain a memory of the earlier autoimmune attack. By intervening sooner, doctors may be able to reduce the likelihood of these long-lasting immune cells becoming established.
Although further research is still needed to fully confirm this effect, the current evidence strongly supports early management of vitiligo. Prompt treatment may not only improve repigmentation outcomes but could also reduce the risk of long-term recurrence. For patients, this means that seeking medical advice early and following a consistent treatment plan may offer the best chance of maintaining stable skin pigmentation over time.
Environmental and Stress Triggers
Even when resident memory T cells remain inactive in the skin, certain environmental or physical triggers can cause them to reactivate. These triggers may include skin injury or repeated friction, sunburn, severe emotional stress, illness, or other forms of systemic inflammation. Although these events may seem unrelated to vitiligo, they can create changes in the skin’s immune environment. When this happens, the immune system may become more active in the affected areas.
These triggers often produce inflammatory signals that stimulate immune activity within the skin. As the immune system responds to these signals, resident memory T cells that were previously dormant may become active again. Because these cells still “remember” the earlier autoimmune attack against melanocytes, their reactivation can restart the same destructive process. This renewed immune response can once again damage pigment-producing cells.
As a result, depigmented patches may return even after a period of stable or improved skin colour. This helps explain why some people notice new vitiligo patches following periods of physical stress, illness, or emotional strain. Understanding these triggers can help patients take preventive steps, such as protecting the skin from injury and managing stress levels. While these measures may not eliminate the risk entirely, they can support better long-term management of the condition.
Why Maintenance Therapy May Be Recommended
After successful repigmentation, many patients hope that vitiligo will not return. However, because of the presence of resident memory T cells in previously affected skin, there is still a possibility of relapse. For this reason, dermatologists often recommend maintenance therapy to help stabilise the condition. The goal is to keep the immune response under control and reduce the chances of depigmentation returning.
- Occasional Phototherapy Sessions: Some patients may continue with phototherapy at longer intervals after repigmentation has been achieved. These occasional sessions help maintain melanocyte activity and support stable pigmentation, while also reducing the likelihood of immune reactivation in previously affected areas.
- Intermittent Topical Medication: Dermatologists may advise using topical treatments, such as anti-inflammatory creams, periodically even after improvement. This approach helps keep the immune response balanced and prevents resident memory T cells from becoming overly active again.
- Careful Skin Protection: Protecting the skin from excessive sun exposure, irritation, and injury is an important part of maintenance therapy. Triggers such as sunburn or skin trauma can stimulate immune activity, potentially increasing the risk of vitiligo returning in vulnerable areas.
- Long-Term Stability of Pigmentation: Maintenance therapy focuses on preserving the results already achieved through treatment. By continuing gentle management strategies, patients can help maintain pigment stability and reduce the likelihood of future flare-ups.
In conclusion, maintenance therapy is often recommended because the immune mechanisms behind vitiligo can remain active even after visible improvement. While these treatments may not completely eliminate resident memory T cells, they help keep the immune system stable and lower the risk of relapse. With consistent care and monitoring, many patients can maintain their repigmentation for longer periods.
The Psychological Impact of Vitiligo Recurrence
The unpredictable nature of vitiligo can have a significant emotional and psychological impact. Many people feel hopeful and encouraged when treatment begins to work and pigment gradually returns to the skin. Seeing visible improvement can restore confidence and provide reassurance that the condition is under control. However, this sense of progress can be shaken if depigmentation later reappears.
When vitiligo returns after a period of improvement, it can feel deeply discouraging. Patients may question whether the treatment was effective or worry that they did something to trigger the relapse. These feelings are completely understandable because the condition often behaves in ways that are difficult to predict. The cycle of improvement followed by recurrence can create frustration, anxiety, and uncertainty about the future.
Learning about the biological mechanisms behind vitiligo recurrence can sometimes help reduce these emotional burdens. Research shows that relapse is often linked to persistent immune cells that remain in the skin rather than anything a patient has done wrong. Understanding this can remove feelings of blame and help people view the condition more objectively. With the right information and support, patients may find it easier to cope with the ups and downs of managing vitiligo.
Research Into Skin Immune Memory
The discovery of resident memory T cells has significantly changed how researchers understand many skin conditions. In the past, scientists mainly focused on inflammation as the primary driver of disease activity. However, new studies show that long-lasting immune cells within the skin may play a key role in how certain conditions develop and recur. This has opened an entirely new area of research into what is often called skin immune memory.
These specialised immune cells have now been linked to several chronic skin disorders, including psoriasis, eczema, and alopecia areata. In each of these conditions, resident memory T cells can remain in the skin even after symptoms improve. Because they retain a “memory” of previous immune activity, they can sometimes reactivate and trigger a new episode of disease. In vitiligo, researchers believe these cells are an important factor behind the persistence and recurrence of depigmentation.
Understanding how these cells behave inside the skin may eventually lead to more targeted treatment approaches. Instead of only reducing inflammation during active disease, future therapies may aim to control or eliminate the immune memory that drives relapse. By focusing on this deeper immune mechanism, researchers hope to develop treatments that provide longer-lasting stability for people living with vitiligo.
Practical Steps for Patients With Vitiligo

While research continues to explore new treatments, there are several practical steps that people with vitiligo can take to help manage the condition. Protecting the skin from injury, friction, and excessive sun exposure is especially important. Skin trauma can sometimes trigger new depigmented patches, a phenomenon known as the Koebner response. Using sun protection and gentle skincare can therefore support overall skin stability.
Managing stress is another factor that may influence the course of the condition. Severe emotional stress can stimulate immune activity in the body and may contribute to disease flare-ups in some individuals. Although stress alone does not cause vitiligo, learning healthy ways to cope with it may help reduce potential triggers. Techniques such as regular exercise, relaxation practices, and maintaining a balanced lifestyle can support general wellbeing.
Regular follow-up appointments with a dermatologist are also essential for long-term management. Early detection of new depigmented areas allows treatment to begin quickly, which may improve the chances of repigmentation. Some patients choose to seek specialist care through clinics that offer comprehensive vitiligo treatment in London and focus on autoimmune skin conditions. Access to experienced dermatology specialists can provide personalised treatment plans and support for managing recurrent vitiligo.
The Future of Vitiligo Treatment
Research into resident memory T cells is still developing, but the discoveries made so far have significantly changed how scientists view vitiligo. In the past, treatments mainly focused on calming visible inflammation and encouraging repigmentation. While these approaches can be effective, they do not always prevent the condition from returning. Understanding the role of long-lasting immune cells has opened the door to more targeted and potentially durable treatment strategies.
Researchers now believe that successful vitiligo management may involve addressing two separate challenges. The first is suppressing the active immune attack that destroys melanocytes and causes pigment loss. The second is controlling or reducing the resident memory T cells that remain in the skin after the inflammation has settled. These cells can retain a memory of the earlier immune response and may reactivate later, triggering new depigmented patches.
Future therapies may therefore combine several treatment approaches to achieve better long-term results. For example, treatments that reduce inflammation could be paired with therapies designed to disrupt the survival signals of resident memory T cells. If scientists can successfully block the pathways that allow these cells to persist in the skin, it may become possible to reduce the risk of recurrence.
FAQs:
1. What are resident memory T cells in vitiligo?
Resident memory T cells are specialised immune cells that remain permanently in the skin after an immune reaction has occurred. In vitiligo, these cells can stay in previously affected areas even after repigmentation. Because they retain a “memory” of the earlier autoimmune attack against melanocytes, they can reactivate and trigger depigmentation again in the same locations.
2. Why does vitiligo often return after successful treatment?
Vitiligo can return because the immune system may still contain resident memory T cells within the skin. Even when treatment restores pigment and reduces inflammation, these cells can remain dormant in the tissue. If they become reactivated by inflammatory signals or environmental triggers, they may initiate another immune attack on melanocytes, causing depigmented patches to reappear.
3. Do current vitiligo treatments remove resident memory T cells?
Most current vitiligo treatments focus on suppressing inflammation and stimulating repigmentation rather than eliminating resident memory T cells. Treatments such as topical medications and phototherapy can reduce immune activity and help melanocytes recover. However, these immune memory cells may persist in the skin, which explains why relapse can sometimes occur after treatment stops.
4. Why do vitiligo patches often reappear in the same place?
Vitiligo patches frequently return in the same areas because resident memory T cells remain in the skin where the previous immune attack occurred. These cells stay localised in the tissue and can quickly trigger another immune response if activated. As a result, the same patch of skin may become depigmented again even after it previously regained colour.
5. Can phototherapy affect resident memory T cells?
Phototherapy, particularly narrowband UVB therapy, can help regulate immune activity in the skin and reduce inflammation. It may suppress the activity of T cells that contribute to melanocyte destruction. However, while phototherapy can improve pigmentation and control active disease, it may not completely eliminate resident memory T cells that remain in the skin.
6. What role do JAK inhibitors play in vitiligo treatment?
JAK inhibitors are a newer group of medications that target specific immune signalling pathways involved in vitiligo. By blocking these signals, they can reduce the immune response that damages melanocytes. Early research suggests they may help restore pigmentation, and scientists are studying whether they might also influence resident memory T cells and reduce the likelihood of relapse.
7. How does interleukin-15 affect vitiligo relapse?
Interleukin-15 is an immune signalling molecule that supports the survival of resident memory T cells in the skin. Because these cells are involved in recurrent immune attacks against melanocytes, blocking this signal may weaken their ability to persist. Researchers are investigating therapies that target interleukin-15 as a potential strategy for preventing vitiligo from returning.
8. Can stress or skin injury trigger vitiligo recurrence?
Yes, certain triggers such as skin trauma, sunburn, illness, or severe emotional stress may activate inflammatory signals in the body. These signals can stimulate resident memory T cells that remain in previously affected skin. When this happens, the immune system may once again attack melanocytes, leading to the return of depigmented patches.
9. Why is early treatment important for vitiligo?
Early treatment may help control the immune response before it becomes deeply established in the skin. Prompt therapy may also reduce the number of resident memory T cells that develop in affected areas. By managing the condition during its early stages, doctors may improve repigmentation outcomes and potentially reduce the risk of long-term relapse.
10. Can vitiligo relapse be prevented completely?
At present, there is no guaranteed way to completely prevent vitiligo relapse. However, consistent treatment, maintenance therapy, and careful skin protection can reduce the risk. Ongoing research into resident memory T cells and immune signalling pathways may eventually lead to treatments that provide longer-lasting control of the condition.
Final Thoughts: Understanding Vitiligo Relapse
Vitiligo can sometimes return even after successful treatment because the immune system may retain a form of “memory” within the skin. The discovery of resident memory T cells has helped researchers understand why depigmented patches often reappear in the same areas. These long-lasting immune cells can remain in previously affected skin and may reactivate when triggered by inflammation, stress, or skin injury. Understanding this process helps patients realise that relapse is not unusual and is linked to the underlying behaviour of the immune system rather than anything they have done wrong.
Although recurrence can occur, modern vitiligo management focuses on controlling immune activity, restoring pigmentation, and maintaining long-term stability through ongoing care. Early treatment, regular dermatology follow-ups, and appropriate maintenance therapy can all help reduce the risk of new depigmented patches forming. If you’re looking for specialist vitiligo treatment in London, you can reach out to us at the London Dermatology Centre to book a consultation with one of our specialists.
References:
- Pérez‑Bootello, J., Cova‑Martín, R., Naharro‑Rodríguez, J. & Segurado‑Miravalles, G., 2023. Vitiligo: Pathogenesis and New and Emerging Treatments. International Journal of Molecular Sciences https://www.mdpi.com/1422-0067/24/24/17306
- Ryan, G.E., Harris, J.E. & Richmond, J.M. (2021) Resident memory T cells in autoimmune skin diseases. Frontiers in Immunology https://pubmed.ncbi.nlm.nih.gov/34012438/
- Xu, Y., Zhang, B., Lin, M. and Zhang, L. (2022) Discovery of resident memory T cells in inflammatory vitiligo: A case report.Medicine https://pmc.ncbi.nlm.nih.gov/articles/PMC9575797/
- Richmond, J.M., Strassner, J.P., Rashighi, M., Agarwal, P., Garg, M., Essien, K.I. & Harris, J.E. (2019) Resident memory and recirculating memory T cells cooperate to maintain disease in a mouse model of vitiligo.The Journal of Investigative Dermatology, https://www.sciencedirect.com/science/article/pii/S0022202X18328021
- Riding, R.L. & Harris, J.E. (2019) The role of memory CD8⁺ T cells in vitiligo. The Journal of Immunology, https://academic.oup.com/jimmunol/article-abstract/203/1/11/7952382