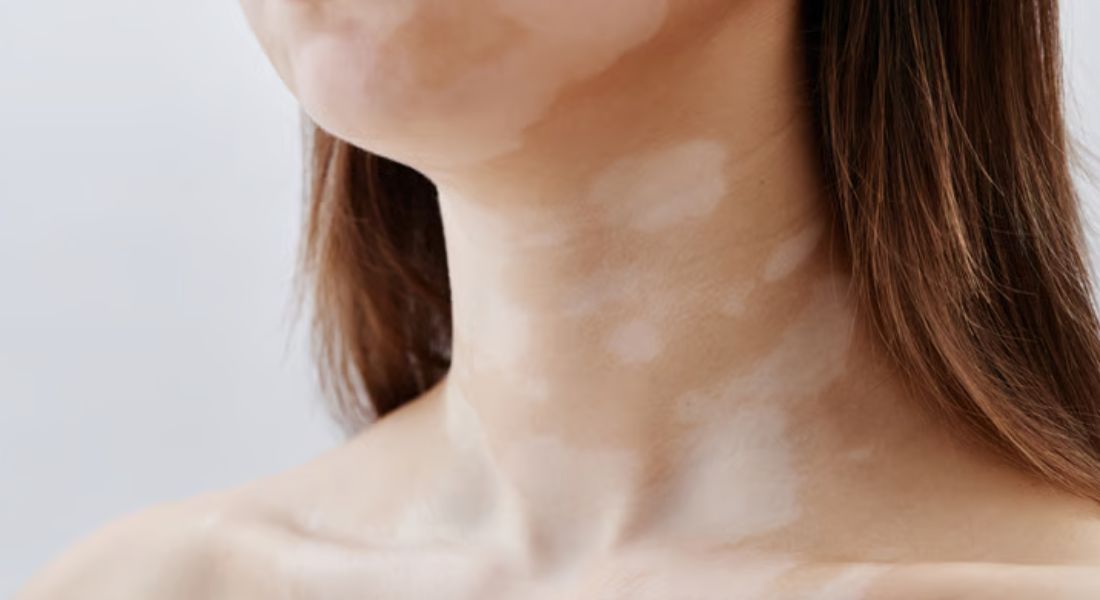
If you or your child has been diagnosed with Vitiligo, you may quickly realise that not all forms of the condition behave in the same way. Some types tend to spread gradually over time, while others remain confined to a specific area. Segmental Vitiligo falls into the latter category and has distinct features that set it apart. It usually affects one side of the body and follows a more localised pattern.
Understanding these differences can help you feel more in control of your diagnosis. It also gives you a clearer idea of what to expect in terms of progression and treatment outcomes. Unlike more common forms, segmental vitiligo often stabilises after an initial period of activity. Knowing this can make the condition feel less uncertain.
In this article, you will learn what makes segmental vitiligo unique. We will explore how it develops, why it behaves differently, and how dermatologists manage it. With the right information, you can approach your treatment with greater confidence and clarity.
What Is Segmental Vitiligo?
Segmental vitiligo is a specific subtype of Vitiligo that affects a clearly defined area, or “segment”, of your body. Unlike more common forms, it usually appears on one side only and follows a localised pattern. This pattern often corresponds to the way nerves are distributed within your skin. You may notice that it behaves differently from other types of vitiligo.
- Localised and one-sided pattern: The depigmented patches typically develop in a specific area, such as part of your face, arm, or torso. They usually do not cross over to the other side of your body.
- Rapid early development: In the initial stage, you may see patches appear or expand relatively quickly over weeks or months. This early phase can feel sudden compared to other types.
- Tendency to stabilise: After the initial progression, the condition often settles and stops spreading. This stability is one of the most distinctive features of segmental vitiligo.
- More predictable course: Because it usually remains confined to one area, it tends to be easier to monitor over time. It does not typically spread unpredictably to new areas of skin.
This more stable and localised behaviour can make long-term management more straightforward. Understanding how segmental vitiligo progresses helps you and your specialist plan treatment and set realistic expectations.
How It Differs from Non-Segmental Vitiligo
The most common form of Vitiligo is known as non-segmental vitiligo. This type usually appears on both sides of your body in a fairly symmetrical pattern. It can continue to spread over time, sometimes in an unpredictable way. You may notice periods of stability followed by new areas of depigmentation.
In contrast, Segmental Vitiligo tends to remain limited to one specific region. It typically affects only one side of your body and rarely crosses the midline. This gives it a very distinct and recognisable pattern. Because of this localised distribution, it often behaves more predictably.
You may also notice differences in how these types develop over time. Segmental vitiligo often appears earlier in life and may progress quite quickly at first. However, it usually stabilises after this initial phase. Non-segmental vitiligo, on the other hand, often follows a longer and more fluctuating course.
Why Segmental Vitiligo Is More Localised
One of the most distinctive features of Segmental Vitiligo is its localised pattern. Researchers believe this may be linked to the nervous system rather than a widespread immune process. In many cases, the patches appear to follow specific nerve-related skin regions known as Dermatomes. This helps explain why the condition often affects only one side of the body.
This connection with nerve pathways may be why the patches remain confined to a single area. Unlike more common forms of Vitiligo, it does not usually spread across different parts of the body. The underlying mechanism appears to be more localised rather than systemic. This difference plays a key role in how the condition behaves.
This predictable pattern can be reassuring for you. Once segmental vitiligo stabilises, further spread is generally unlikely. This allows you and your dermatologist to plan treatment with greater confidence. Understanding this behaviour can make the condition feel more manageable.
The Role of the Immune System
In Vitiligo, the immune system plays a central role. It is generally considered an autoimmune condition, which means your immune system mistakenly targets melanocytes the cells responsible for producing pigment in your skin. When these cells are affected, areas of skin lose their colour. However, Segmental Vitiligo may behave slightly differently from other forms.
- Localised immune activity: In this subtype, immune activity tends to be more confined to a specific area of your skin. This may explain why depigmentation usually affects just one segment rather than spreading widely.
- Targeted impact on melanocytes: The immune response still affects pigment-producing cells, but it may do so in a more focused way. This can lead to clearly defined patches within a limited region.
- Rapid onset followed by stability: The concentrated immune activity may contribute to the faster early development you might notice. After this phase, the condition often stabilises, with little further spread.
- Influence on treatment choices: Because the immune response is more localised, dermatologists may tailor treatments differently. Certain therapies may be more effective when the condition is stable and confined to one area.
Understanding how the immune system behaves in segmental vitiligo helps guide treatment decisions. It also explains why this subtype often follows a more predictable course compared to other forms of vitiligo.
Genetic Factors and Risk
You might wonder whether Segmental Vitiligo runs in families. While genetics can play a role in Vitiligo overall, this subtype is less strongly linked to family history. In many cases, it appears sporadically without a clear inherited pattern. This means you may not see similar cases among your relatives.
Because of this, segmental vitiligo is often considered less influenced by genetic factors compared with non-segmental forms. The condition can develop even if there is no known family history of vitiligo. This is one of the key ways it differs from more common types. It highlights that different mechanisms may be involved.
That said, genetics may still play a subtle role. Researchers continue to study how genes might contribute to this condition. At present, the genetic influence appears less significant in this subtype. Ongoing research will help clarify these connections over time.
When Segmental Vitiligo Typically Appears
Segmental Vitiligo often begins in childhood or adolescence. You may notice patches developing quite suddenly over a short period of time. This rapid onset can feel worrying at first, especially if the changes seem to happen quickly. However, this early phase is a recognised part of how the condition behaves.
In many cases, the condition stabilises within months to a few years. After this initial period, further spread is usually limited or stops completely. This pattern of rapid onset followed by stability is one of its defining features. It makes the condition more predictable compared to other forms of Vitiligo.
An early onset does not necessarily mean a worse outcome. In fact, once the condition stabilises, it can be easier to plan treatment effectively. Your dermatologist can assess the timing and stage of the condition when recommending options. Understanding this timeline helps you make informed decisions about your care.
Common Areas Affected
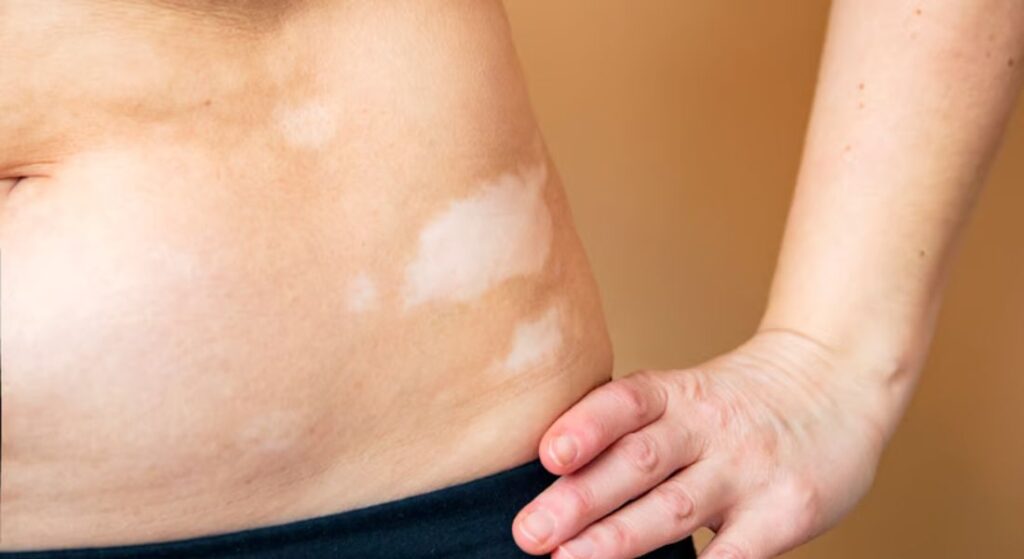
Segmental Vitiligo can affect different parts of your body, although certain areas are more commonly involved. You may notice patches on the face, neck, or upper torso. In some cases, the condition can also affect your arms or legs. The exact location varies, but it usually remains confined to one region.
You might also observe that the patches follow a distinct line or pattern. This is linked to the underlying nerve pathways in your skin. The distribution often reflects specific nerve-related areas, giving the condition its characteristic appearance. This pattern is one of the key features that helps distinguish it from other forms of Vitiligo.
Hair in the affected area may also lose its pigment, a change known as Poliosis. This can occur alongside the skin changes and may be more noticeable in areas such as the scalp or eyebrows. The presence of poliosis can sometimes influence how well certain treatments work. Recognising these changes helps guide management decisions.
The Importance of Early Assessment
If you notice sudden pigment loss, it is important to seek an early evaluation. A dermatologist can determine whether you have Segmental Vitiligo or another form of Vitiligo. This distinction matters because each type behaves differently and requires a tailored treatment approach. Getting a clear diagnosis early helps guide the next steps in your care.
You may also benefit from starting treatment during the active phase of the condition. Some therapies are more effective when the patches are still developing. Acting promptly can improve the chances of achieving better results. Early intervention allows your dermatologist to manage the condition more effectively.
An early assessment can also provide reassurance. Understanding what type of vitiligo you have helps reduce uncertainty and confusion. You will have a clearer idea of what to expect over time. This knowledge can help you feel more confident and in control of your treatment journey.
Treatment Approaches for Segmental Vitiligo
Treatment for Segmental Vitiligo focuses on restoring pigment and stabilising the condition. Because this type often settles on its own after an initial active phase, treatment is usually aimed at improving the appearance of the affected skin. The approach depends on factors such as how long you have had the condition and how extensive the patches are. Your dermatologist will tailor the plan to suit your individual needs.
Topical therapies are often used during the early stages. These may include corticosteroids or calcineurin inhibitors, which help reduce local immune activity in the skin. By calming this response, they can support repigmentation in some cases. Consistent use over time is important to see potential benefits.
Light-based treatments may also be considered as part of your care. However, they are sometimes less effective in segmental vitiligo compared with other forms of Vitiligo. Your dermatologist will assess whether this option is suitable for you. Overall, treatment plans are always individualised to achieve the best possible outcome.
How Dermatologists Diagnose Segmental Vitiligo
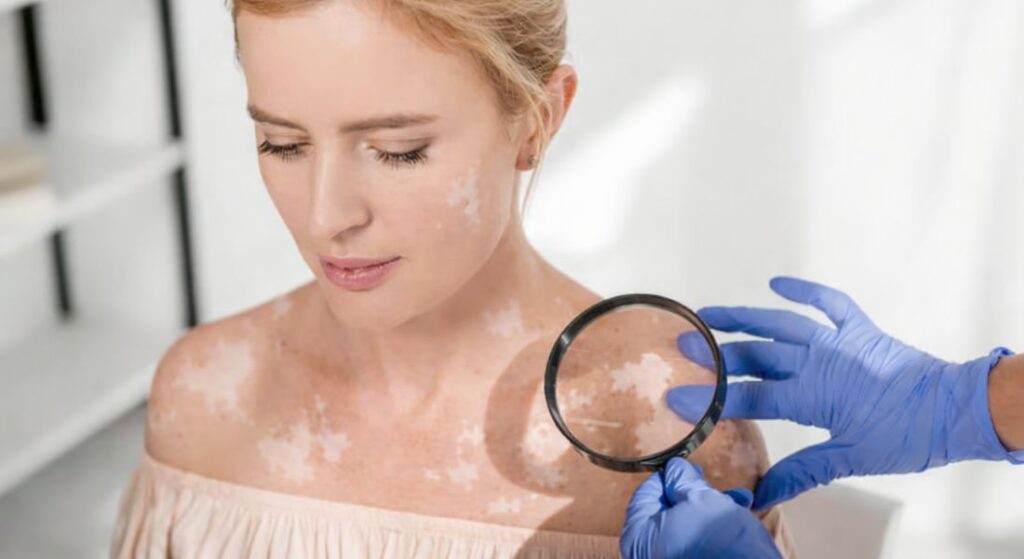
Diagnosing segmental vitiligo is usually straightforward, especially when the pattern is typical. Your dermatologist will begin with a careful clinical examination, looking closely at how the patches appear and how they have developed over time. The one-sided, localised nature of this condition often provides a strong diagnostic clue. To confirm the diagnosis and rule out other conditions, a few simple assessments may be used.
- Clinical examination: Your dermatologist will assess the shape, distribution, and progression of the depigmented patches. A clearly defined area affecting only one side of your body is a key feature they look for.
- Use of a Wood’s lamp: A Wood’s lamp may be used to examine your skin under ultraviolet light. This can make areas of pigment loss appear more distinct, helping to confirm the diagnosis.
- Biopsy in rare cases: In most cases, a biopsy is not needed. However, if the diagnosis is unclear, a small skin sample may be taken and examined to rule out other conditions.
- Assessment of progression: Your dermatologist may also ask about how quickly the patches appeared and whether they have changed. This helps confirm the typical pattern of rapid onset followed by stability.
Early and accurate diagnosis is important. It allows your dermatologist to plan the most appropriate treatment and gives you a clearer understanding of how the condition is likely to behave over time.
Surgical Treatment Options
In stable cases of Segmental Vitiligo, surgical treatments may be considered as part of your management plan. These approaches aim to restore pigment in areas where it has been lost, particularly when other treatments have not produced the desired results. Your dermatologist will usually recommend surgery only after careful assessment.
- Melanocyte transplantation: This technique involves transferring healthy pigment-producing cells (melanocytes) from one area of your skin to the affected patches. Once applied, these cells can begin producing pigment, helping to restore a more natural skin colour.
- Importance of stability: Surgery is typically only suitable if your condition has remained stable for a significant period, often several months to a year. This reduces the risk of new patches developing after treatment and improves the chances of success.
- Careful patient selection: Not everyone is a suitable candidate for surgical treatment. Your dermatologist will consider factors such as the size and location of the patches, your overall skin health, and how your condition has behaved over time.
- Potential for long-lasting results: When successful, surgical procedures can provide durable repigmentation. They are particularly effective for well-defined, localised areas, which makes them especially relevant for segmental vitiligo.
Surgical options can be an effective solution when the condition is stable and clearly defined. A thorough consultation helps determine whether this approach is right for you and ensures realistic expectations about the outcome.
How Response to Treatment Differs
Segmental Vitiligo often responds differently to treatment compared with other forms of Vitiligo. Because it usually stabilises quite early, medical therapies may have a more limited effect once the condition has stopped progressing. This can influence how much improvement you may see with topical or light-based treatments. Understanding this helps set realistic expectations.
You may find that starting treatment early offers the best chance of repigmentation. During the active phase, the skin may respond better to medical therapies. Once the condition becomes stable, surgical options such as skin grafting or melanocyte transfer may be considered. Timing plays an important role in deciding which approach is most suitable.
Managing expectations is an important part of your care. While repigmentation is possible, results can vary from person to person. Your dermatologist will guide you based on your individual case and treatment goals. A personalised approach helps achieve the best possible outcome for your skin.
Psychological Impact and Coping
Living with Segmental Vitiligo can affect how you feel about your appearance and confidence. Even though it is usually localised, it may still have a noticeable emotional impact, especially if it affects visible areas such as your face. Changes in skin colour can draw attention, which can sometimes make you feel more self-aware. These reactions are very common and understandable.
You may find yourself feeling self-conscious or concerned about how others perceive you. It’s important to recognise that these feelings are valid and part of your experience. Looking after your emotional wellbeing is just as important as managing the physical aspects of the condition. Taking time to acknowledge how you feel can help you cope more effectively.
Support can make a meaningful difference. Speaking with a dermatologist, counsellor, or a support group can help you navigate these challenges. Sharing your experience with others who understand can be reassuring. With the right support, you can feel more confident and less alone in managing your condition.
Long-Term Outlook
The long-term outlook for Segmental Vitiligo is generally positive. Once the condition stabilises, it usually remains confined to the same area without spreading further. This predictable pattern can be reassuring and makes it easier to plan your care with confidence. You may still notice some lasting changes, but these are often manageable.
- Stable, non-progressive pattern: After the initial phase, the condition typically stops progressing. This means you are unlikely to see new patches developing in different areas of your body.
- Persistent but controlled patches: Existing depigmented areas may remain, but they usually do not worsen over time. This stability allows you to focus on improving their appearance if you choose.
- Easier long-term management: Because the condition is localised and stable, treatment plans can be more targeted. Your dermatologist can recommend therapies suited specifically to the affected area.
- Improving treatment outcomes: Advances in therapies, including medical and surgical options, continue to improve cosmetic results. Many people achieve noticeable repigmentation or find ways to blend the patches effectively.
With the right approach and guidance, you can manage segmental vitiligo successfully. Ongoing developments in dermatology are making outcomes increasingly positive, helping you maintain both confidence and comfort in the long term.
Differences in Children and Adults
Segmental Vitiligo can affect both children and adults, although it often appears earlier in life. In children, the onset may seem quite rapid, with patches developing over a short period. This can feel worrying, especially for parents noticing sudden changes in their child’s skin. Understanding that this pattern is typical can help provide some reassurance.
The encouraging aspect is that the condition often stabilises relatively quickly. Once it reaches this stable phase, further spread is usually limited. This makes early evaluation particularly important in younger patients. Prompt assessment helps confirm the diagnosis and allows appropriate planning for care.
Treatment approaches may vary slightly depending on age. Dermatologists consider factors such as skin sensitivity, safety, and long-term effects when recommending therapies for children or adults. Your treatment plan will always be tailored to your individual needs. Personalised care helps ensure both safety and effectiveness.
Advances in Research
Ongoing research into Segmental Vitiligo continues to improve understanding of how the condition develops. Scientists are exploring the role of nerve pathways, local immune responses, and genetic influences. These insights are helping explain why this form behaves differently from other types of Vitiligo. As knowledge grows, treatment strategies are becoming more refined.
New therapies are also being investigated. These include targeted treatments designed to act on specific pathways involved in pigment loss. By focusing on the underlying mechanisms, these approaches aim to improve repigmentation and long-term outcomes. Although many of these treatments are still being studied, they offer promising possibilities for the future.
As research progresses, you can expect more personalised approaches to care. Treatments may increasingly be tailored to your specific condition and stage of disease. A deeper understanding benefits both patients and clinicians, leading to more effective management. The future of treatment continues to evolve in a positive direction.
FAQs:
1. What makes segmental vitiligo different from other types?
Segmental vitiligo usually affects only one side of your body and follows a localised pattern. Unlike other types, it does not tend to spread widely over time. It often develops quickly and then stabilises. This makes it more predictable and easier to monitor.
2. Does segmental vitiligo spread over time?
Segmental vitiligo typically spreads rapidly at first but then stops. Once it stabilises, it rarely spreads to new areas. This is different from other forms that may continue to progress. Understanding this can help you feel more reassured.
3. At what age does segmental vitiligo usually start?
You may notice segmental vitiligo beginning in childhood or adolescence. It often appears suddenly over a short period. While this can feel worrying, the condition usually stabilises fairly quickly. Early assessment can help guide treatment decisions.
4. Why does segmental vitiligo stay localised?
Segmental vitiligo is thought to be linked to nerve pathways in your skin. This may explain why it follows a specific pattern and stays in one area. The immune activity involved is more localised rather than widespread. This limits how far it spreads.
5. Can segmental vitiligo affect hair colour?
Yes, you may notice hair in the affected area turning white. This is called poliosis and happens when pigment cells in hair follicles are affected. It can occur alongside skin depigmentation. This may also influence how well treatments work.
6. Is segmental vitiligo hereditary?
Segmental vitiligo is less strongly linked to family history compared to other types. You may not see a clear pattern in relatives. It often appears without a known genetic cause. However, research into genetic factors is still ongoing.
7. What treatments are available for segmental vitiligo?
Treatment may include topical creams to reduce local immune activity. Light therapy can sometimes help, although results may vary. In stable cases, surgical options like melanocyte transplantation may be considered. Your dermatologist will tailor the approach to your needs.
8. Does segmental vitiligo respond well to treatment?
Response to treatment depends on the stage of the condition. Early treatment during the active phase may give better results. Once stabilised, medical treatments may be less effective. Surgical options can sometimes provide more noticeable improvement.
9. When should you see a dermatologist?
You should see a dermatologist if you notice sudden or localised pigment loss. Early diagnosis helps confirm the type of vitiligo. Prompt treatment can improve outcomes, especially in the early stage. Professional advice also helps you manage the condition confidently.
10. What is the long-term outlook for segmental vitiligo?
The long-term outlook is generally positive. Once stabilised, the condition usually does not spread further. You may still have patches, but they are unlikely to worsen. With the right care, you can manage the condition effectively.
Final Thoughts: Understanding and Managing Segmental Vitiligo
Segmental vitiligo can feel worrying when it first appears, particularly because it often develops quickly and affects visible areas. However, its localised pattern and tendency to stabilise make it more predictable than other forms of vitiligo. Once the condition settles, it usually does not spread further, which can provide reassurance and help you feel more in control.
With the right approach, segmental vitiligo can be managed effectively. Early assessment is important, as treatment during the active phase may offer better results. Even after stabilisation, options such as surgical treatments can help improve pigmentation and overall appearance. A personalised plan ensures your treatment is tailored to your specific needs. If you’re considering vitiligo treatment in London, you can get in touch with us at London Dermatology Centre.
References:
- Diotallevi, F. et al. (2023), Vitiligo, from Pathogenesis to Therapeutic Advances: State of the Art, International Journal of Molecular Sciences, 24(5), 4910. https://www.mdpi.com/1422-0067/24/5/4910
- Hann, S.K. and Lee, H.J. (1996) Segmental vitiligo: clinical findings in 208 patients, Journal of the American Academy of Dermatology, 35(5), pp. 671–674. Available at: https://pubmed.ncbi.nlm.nih.gov/8912558/
- Böhm, M. and Tanew, A. (2025), Vitiligo, Journal der Deutschen Dermatologischen Gesellschaft, 23(8), pp. 968–987. https://pubmed.ncbi.nlm.nih.gov/40788636/
- Kim, Y.J. et al. (2014) Clinical course of segmental vitiligo: a retrospective study, Annals of Dermatology, 26(1), pp. 61–66. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3956796/
- Speeckaert, R. et al. (2024), Vitiligo: From Pathogenesis to Treatment, Journal of Clinical Medicine, 13(17), 5225. https://pmc.ncbi.nlm.nih.gov/articles/PMC11396398/