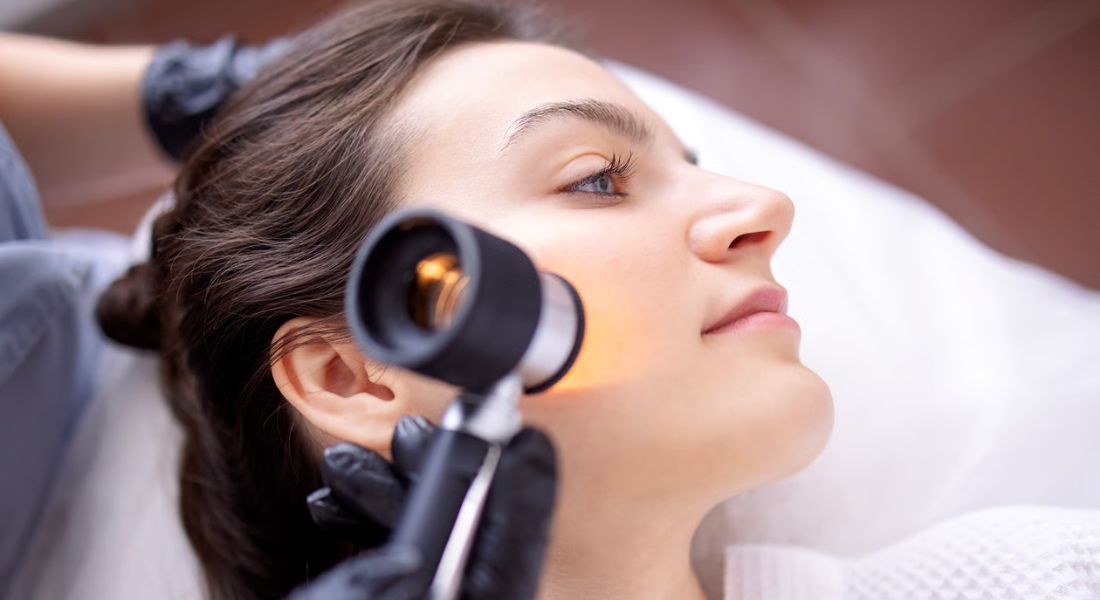
Dermatology is a highly visual medical specialty. When you visit a clinic with a skin concern, one of the first things your clinician does is carefully examine the appearance of your skin. Dermatologists are trained to recognise subtle patterns that can reveal important clues about the underlying condition.
Unlike many other areas of medicine that rely heavily on laboratory tests, dermatology often begins with visual assessment. The shape, colour, texture, and distribution of skin lesions can suggest possible diagnoses almost immediately. Through experience and specialised training, dermatologists learn to interpret these features with remarkable accuracy.
In this article, we look at how pattern recognition works in dermatology. You will learn how clinicians analyse lesion morphology, observe distribution patterns, and consider the broader clinical context. This approach helps narrow down potential diagnoses and guides any further investigations that may be needed.
Why Dermatology Is a Visual Specialty
Dermatology depends heavily on observation because your skin is directly visible. Unlike internal organs, it can be examined immediately without invasive testing. This makes visual pattern recognition one of the most important diagnostic skills in the field.
Dermatologists spend years learning how various conditions appear on the skin. They study the shape, colour, and arrangement of lesions across thousands of clinical examples. Over time, these patterns become familiar, making it easier to recognise different conditions quickly.
Being able to interpret visual clues allows dermatologists to make rapid diagnostic assessments. While additional tests may sometimes be needed, pattern recognition often provides the first and most important insights into your condition.
Understanding Skin Lesion Morphology
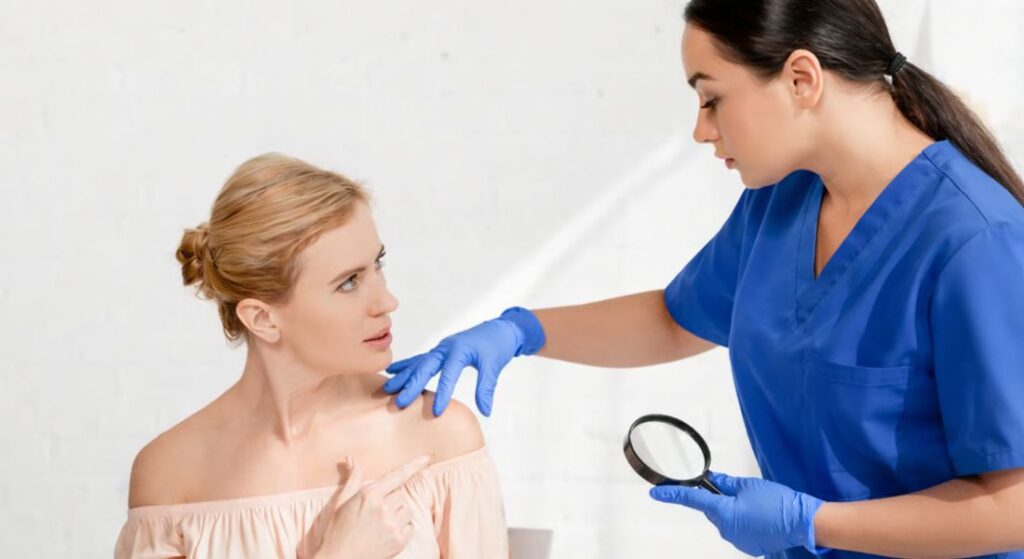
Morphology refers to the physical characteristics of a skin lesion. Dermatologists carefully examine features such as shape, size, colour, surface texture, and the edges of a lesion. Each of these details can provide important clues about the type of condition you may have.
For instance, a raised bump is usually called a papule, while a flat, coloured patch is referred to as a macule. Other patterns include blisters, plaques, nodules, and scales, each representing a distinct morphological type. Learning these terms allows clinicians to describe and classify skin findings accurately.
Classifying lesions by their morphology helps dermatologists group conditions with similar visual features. This approach narrows down the list of possible diagnoses. Morphological assessment is often the first crucial step in clinical reasoning.
The Importance of Lesion Distribution
The location of skin lesions on your body can provide important diagnostic clues. Some conditions tend to appear on sun-exposed areas, while others affect skin folds or areas under pressure. Recognising these patterns helps dermatologists narrow down the possible causes.
For example, psoriasis often develops on the elbows, knees, and scalp. Eczema typically appears in the creases of the arms and behind the knees. Acne usually affects the face, chest, and back.
By observing where lesions occur, dermatologists combine this information with their assessment of morphology. The combination of appearance and location often provides a strong indication of the likely condition.
Pattern Recognition and Differential Diagnosis
When dermatologists evaluate a skin condition, they rarely rely on a single feature. Instead, they look at multiple aspects at once, including the shape, colour, and distribution of lesions. By recognising patterns, they can form an initial understanding of what might be causing your symptoms. This approach helps them assess the situation more accurately and efficiently.
- Combine visual features: Dermatologists consider morphology, distribution, and colour together. This allows them to see how different characteristics interact and form a clearer diagnostic picture.
- Create a differential diagnosis: A differential diagnosis is a list of possible conditions that could explain what you are experiencing. Each option is examined carefully using clinical evidence and experience.
- Prioritise likely conditions: Experienced clinicians can recognise which patterns are typical and which are unusual. This helps them focus on the most probable causes first, saving time and guiding further investigation.
- Confirm with additional testing: Once the most likely conditions are identified, further tests, such as lab work or biopsies, may be used to confirm the final diagnosis.
By using pattern recognition and a structured approach, dermatologists can provide an accurate and timely diagnosis. This method ensures that the most likely causes are considered first, while less common possibilities are not overlooked.
Recognising Primary Skin Lesions
Primary skin lesions are the first visible signs that a skin condition may be developing. They appear directly as a result of the underlying disease process. Being able to identify them accurately is essential for making a correct diagnosis and guiding further investigation.
- Different types of primary lesions: Examples include macules, papules, vesicles, nodules, and plaques. Each type reflects a distinct structural change in the skin, which provides clues about the underlying condition.
- Subtle differences matter: Dermatologists are trained to notice small variations in size, shape, and texture. These subtle differences can significantly narrow down potential diagnoses.
- Diagnostic clues from lesion type: Fluid-filled vesicles may point to viral infections or dermatitis. Thickened plaques could indicate inflammatory conditions like psoriasis, helping clinicians prioritise their assessment.
- Guides further evaluation: Correctly recognising primary lesions informs the next steps, whether that’s additional tests, monitoring, or immediate treatment.
By focusing on primary lesions, dermatologists can often gain early insight into the likely cause of a skin problem. This helps ensure timely and accurate care, improving outcomes for patients.
Understanding Secondary Skin Changes
Secondary skin changes happen when primary lesions evolve or are altered over time. Factors like scratching, infection, or natural healing can change how a lesion looks. These changes may sometimes make it harder to identify the original condition.
Common examples of secondary changes include crusting, scaling, ulceration, and scarring. Dermatologists examine these features closely to understand how the disease has progressed. Recognising these patterns helps them reconstruct what happened to the original lesion.
Distinguishing primary from secondary changes requires careful observation and experience. This skill develops over years of training and is a key part of dermatological expertise. Being able to identify these differences allows clinicians to make more accurate diagnoses.
Colour Patterns in Skin Disease
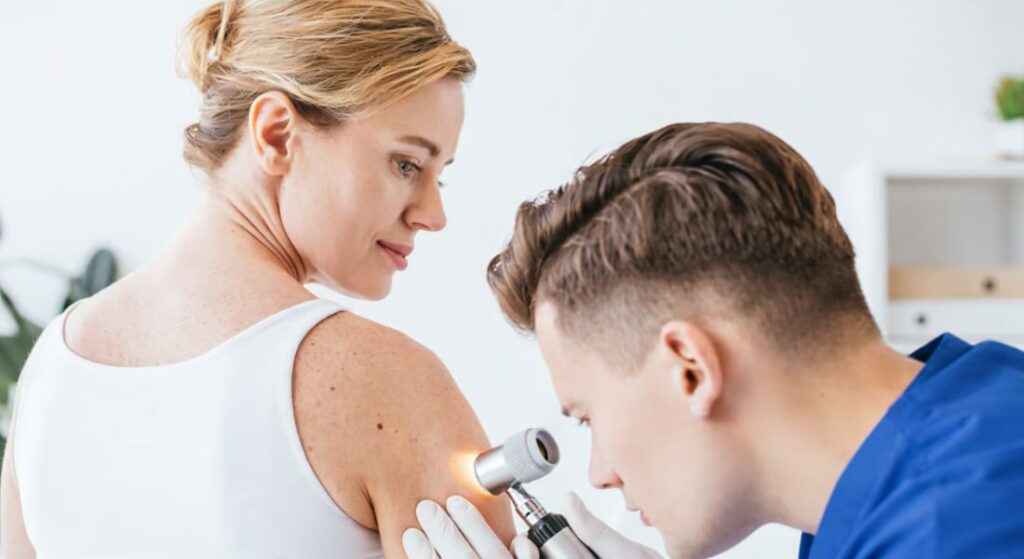
Colour is a key feature that dermatologists use to assess skin conditions. Different colours can indicate different underlying processes, such as inflammation, vascular changes, or pigment alterations. Paying close attention to colour helps clinicians narrow down potential causes and decide on further evaluation.
- Red indicates inflammation: Redness often points to active inflammation or irritation in the skin. This can be seen in conditions like eczema, dermatitis, or infection.
- Purple suggests vascular issues: Purple or bluish lesions may signal problems with blood vessels or circulation. Recognising this can guide further investigation into vascular or bleeding disorders.
- Pigmented lesions indicate melanin changes: Brown, black, or uneven pigmentation may relate to melanin changes or certain vascular structures. Irregular pigmentation can be a warning sign for more serious conditions, such as melanoma.
- Colour variations provide diagnostic clues: Differences in colour within a single lesion are important to note. Subtle shifts can help dermatologists distinguish between benign and potentially harmful conditions.
By carefully analysing colour patterns, dermatologists gain valuable insight into the nature of a skin condition. This understanding, combined with other features like morphology and distribution, supports a more accurate and timely diagnosis.
Surface Texture and Skin Feel
The texture of a lesion can give important clues about a skin condition. Some lesions may feel rough, scaly, smooth, or even waxy. By gently palpating the skin, dermatologists can gather additional information that complements what they see. This tactile assessment helps build a more complete picture of the condition.
- Rough or scaly lesions: Scaling often points to conditions like psoriasis or fungal infections. The texture can help distinguish between different inflammatory or infectious causes.
- Firm nodules: Hard, raised lesions may indicate deeper skin involvement, such as cysts, tumours, or other structural changes beneath the surface.
- Soft or pliable lesions: Soft lesions are often benign, such as cysts or lipomas. Their feel can help differentiate them from more concerning growths.
- Combining touch and sight: Using both visual inspection and tactile assessment improves pattern recognition. This multi-sensory approach increases diagnostic accuracy and helps clinicians prioritise potential conditions.
By paying attention to surface texture and skin feel, dermatologists can gain a deeper understanding of what may be causing a lesion. This combination of observation and touch supports a more confident and precise diagnosis.
Symmetry and Arrangement of Lesions
Symmetry is an important pattern that dermatologists pay close attention to. Many inflammatory conditions appear symmetrically on both sides of the body, which can help distinguish systemic diseases from localised issues. Recognising whether lesions are mirrored or uneven provides valuable diagnostic information.
For example, psoriasis often develops symmetrically on the elbows and knees. In contrast, contact dermatitis usually appears only where the skin has come into contact with an irritant. Observing these patterns helps dermatologists narrow down possible causes.
The arrangement of lesions across the skin is also significant. Some conditions form rings, lines, or grouped clusters. These patterns often offer strong clues and guide clinicians towards the correct diagnosis.
Dermoscopy and Advanced Pattern Recognition
Dermoscopy is a specialised tool that allows dermatologists to examine skin structures in greater detail. This handheld device magnifies the skin and reveals patterns that are not visible to the naked eye. It is especially useful for assessing pigmented lesions and identifying subtle changes.
Using dermoscopy, dermatologists can observe pigment networks, blood vessels, and microscopic patterns within the lesion. These details help distinguish benign moles from potentially dangerous or suspicious growths. The technique is particularly valuable for the early detection of skin cancer.
Dermoscopy builds on the principles of visual pattern recognition. By revealing additional layers of information, it enhances the dermatologist’s ability to make accurate diagnoses. This approach improves both diagnostic confidence and patient safety.
The Role of Clinical Context

When assessing a skin condition, dermatologists don’t rely on what they see alone. Your medical history, current symptoms, and environmental exposures all play a crucial role in understanding the cause. Considering these factors alongside visual examination gives a clearer picture of what may be happening.
- Medication history: A rash that appears after starting a new medication could indicate a drug reaction. Knowing the timing and type of medication helps narrow down possible causes.
- Travel and environmental exposure: Recent travel or exposure to certain environments may point to infectious or environmental causes. This context can guide testing and management decisions.
- Age and lifestyle factors: Age, occupation, hobbies, and lifestyle habits can influence which skin conditions are more likely. These details help dermatologists prioritise potential diagnoses.
- Integrating visual and clinical information: By combining pattern recognition with contextual information, dermatologists can create a more accurate and complete diagnostic picture. This approach supports timely and appropriate treatment.
Taking clinical context into account ensures that the diagnosis reflects both what is seen on the skin and the factors affecting your overall health. This integrated method improves accuracy and helps guide the best care for your condition.
Recognising Inflammatory Skin Patterns
Inflammatory skin diseases often show distinctive patterns that help with diagnosis. Common features include redness, swelling, and scaling, which reflect the immune system’s activity in the skin. Recognising these signs allows dermatologists to understand how the skin is reacting.
Conditions such as eczema, psoriasis, and dermatitis each display unique patterns. Dermatologists develop the ability to identify these variations through training and experience. Even subtle differences in appearance or distribution can provide important diagnostic clues.
Understanding these inflammatory patterns helps clinicians select the most appropriate treatments. Anti-inflammatory medications can be used to calm the immune response and reduce symptoms. Early recognition of these patterns often leads to better outcomes for patients.
Identifying Infectious Skin Conditions
Infectious skin conditions often show characteristic patterns that help dermatologists identify the cause. You may notice specific shapes, colours, or distributions that point to bacterial, viral, or fungal infections. Recognising these patterns early allows for quicker and more effective treatment.
- Bacterial infections: These often cause pustules, spreading redness, or areas of warmth. Observing these signs can indicate the need for antibiotics or further testing.
- Viral infections: Viral rashes frequently present as vesicles or clustered lesions. Examples include chickenpox or shingles, where the arrangement and appearance of lesions are distinctive.
- Fungal infections: Ring-shaped rashes with scaly edges are typical of fungal infections like ringworm. Identifying the shape and texture helps guide antifungal treatment.
- Laboratory confirmation: While visual patterns provide strong clues, lab tests can confirm the specific infectious agent. This ensures accurate treatment and avoids unnecessary medications.
By recognising the characteristic features of infectious skin conditions, dermatologists can act promptly to treat the infection. Early identification helps prevent complications and supports a faster recovery.
Pattern Recognition in Skin Cancer Detection
Recognising suspicious patterns is essential for detecting skin cancer. Dermatologists look for features such as asymmetry, irregular borders, colour variation, and changes in the size of a lesion. These signs can indicate that a mole or spot may be undergoing malignant changes.
Early detection significantly improves treatment outcomes. By identifying concerning patterns quickly, dermatologists can prioritise which lesions need further examination. Suspicious moles are often monitored closely or investigated using additional tests.
A biopsy may sometimes be necessary to confirm the diagnosis. However, visual assessment usually provides the first clue that a lesion requires attention. Skilled observation and pattern recognition are therefore crucial in ensuring timely and accurate identification of skin cancer.
The Importance of Experience in Dermatology
Pattern recognition in dermatology improves greatly with clinical experience. Over the course of their careers, dermatologists see thousands of skin conditions. Each case helps them refine their ability to identify important visual clues.
During training, dermatologists study extensive image libraries of skin diseases. They learn to compare new cases with patterns they have seen before. This process builds diagnostic confidence and sharpens observational skills.
Experience also enables clinicians to recognise rare conditions as well as common ones. Subtle variations in lesions become easier to detect over time. This expertise directly benefits patient care by supporting accurate and timely diagnoses.
Artificial Intelligence and Pattern Recognition
Artificial intelligence is becoming an important tool in dermatology, helping to support pattern recognition and diagnosis. AI systems can analyse images of skin lesions and highlight patterns that may be associated with specific conditions. These tools are particularly useful in complex or ambiguous cases, providing additional insight to clinicians.
- Training on large image databases: AI algorithms learn from thousands of dermatology images. This helps the system recognise subtle features linked to particular diseases, improving detection accuracy.
- Flagging suspicious lesions: AI can highlight lesions that appear unusual or potentially serious. This assists dermatologists in deciding which cases need closer examination or further testing.
- Supports, not replaces, clinicians: Despite these advances, AI cannot replace human judgement. Dermatologists interpret AI results within the context of medical history, symptoms, and overall clinical assessment.
- Improves efficiency and accuracy: By combining AI analysis with expert evaluation, clinicians can make more informed decisions. This approach can enhance diagnostic accuracy while supporting faster patient care.
Using AI in dermatology complements traditional assessment methods. It strengthens pattern recognition and helps clinicians identify conditions more confidently, while human expertise remains central to accurate diagnosis and treatment.
Training the Dermatologist’s Eye
Becoming skilled in dermatology requires extensive visual training. Medical students and dermatology trainees study thousands of images of skin conditions. This repeated exposure helps strengthen their ability to recognise important patterns.
Clinical experience is just as important as image study. Seeing real patients allows trainees to notice subtle variations in skin lesions that may not be obvious in photos. Each patient encounter adds valuable practical experience.
Over time, dermatologists develop an intuitive understanding of skin morphology. They learn to identify patterns quickly and accurately. This expertise forms the foundation of precise and confident dermatological diagnosis.
The Role of Skin Biopsy
When the appearance of a skin condition is unclear, a skin biopsy can provide valuable information. This involves taking a small sample of skin to examine under a microscope. By analysing the tissue, pathologists can see changes that aren’t visible on the surface, helping to clarify the diagnosis.
- Provides detailed cellular information: Biopsies reveal the structure and composition of skin cells. This can highlight abnormalities that visual inspection alone might miss.
- Confirms or rules out conditions: Results help dermatologists verify suspected diagnoses or eliminate other possibilities. This ensures that treatment targets the correct condition.
- Used for atypical presentations: When lesions look unusual or don’t fit common patterns, a biopsy provides additional evidence to guide care.
- Supports, not replaces, pattern recognition: Biopsy complements clinical assessment and pattern recognition. Combining both approaches increases diagnostic accuracy and confidence.
By using a skin biopsy alongside visual and contextual evaluation, dermatologists can make precise diagnoses. This integrated approach helps ensure you receive the most appropriate and effective treatment for your condition.
Combining Observation with Investigation
Dermatologists combine careful visual observation with medical investigations to reach accurate diagnoses. Blood tests, imaging, and biopsy results often support the initial assessment. Each piece of information contributes to understanding the condition fully.
Visual examination usually guides which tests are needed. Recognising patterns in lesions helps narrow down the possible diagnoses, making investigations more focused and efficient. This targeted approach avoids unnecessary testing.
By integrating observation with clinical evidence, dermatologists can provide precise and accurate diagnoses. This method also improves treatment planning and ensures that patients receive the most appropriate care.
Why Pattern Recognition Remains Essential
Despite advances in medical technology, visual pattern recognition remains at the heart of dermatology. Your skin provides visible clues that experienced clinicians can interpret quickly. This skill allows for early detection of many conditions, often before other tests are needed.
Dermatologists combine careful observation, clinical experience, and medical knowledge to diagnose skin problems. Pattern recognition helps guide treatment decisions and determines which further investigations may be necessary. It is one of the most powerful tools in the dermatologist’s toolkit.
Understanding these principles can help you appreciate how skin conditions are diagnosed. Careful visual assessment often reveals crucial information about your condition. Even with modern technology, dermatology continues to rely heavily on this specialised skill.
FAQs:
1. What does pattern recognition mean in dermatology?
Pattern recognition in dermatology is how you and your dermatologist identify and interpret visual clues in your skin, such as the shape, colour, texture, and distribution of lesions, to quickly understand what condition might be causing them.
2. Why is lesion morphology important for diagnosing skin conditions?
Lesion morphology matters because the way a lesion looks, whether it’s raised or flat, scaly or smooth, can help you and your dermatologist pinpoint the type of skin condition you may have and guide the next steps in diagnosis.
3. How does the location of skin lesions support diagnosis?
The area where your lesions appear gives important clues. For example, if your rash appears on your elbows or knees, psoriasis might be more likely, while eczema often shows in skin folds. Your dermatologist uses this information alongside other visual features to make sense of what’s happening.
4. What role does visual pattern recognition play in forming a differential diagnosis?
When your dermatologist assesses your skin, they look at all the features together shape, colour, distribution to form a list of possible conditions. This helps you get a faster and more accurate understanding of what could be causing your symptoms and which conditions need further testing.
5. Can changes in skin colour indicate different types of disease?
Yes. If your skin is red, it could indicate inflammation, purple or bluish patches may signal circulation or vascular issues, and uneven pigmentation can suggest changes in melanin or potential risk factors for conditions like melanoma. Paying attention to colour helps your dermatologist narrow down possibilities.
6. How do primary and secondary skin changes affect diagnosis?
Primary changes are the first visible signs of a condition, while secondary changes occur later, such as scaling, crusting, or scarring. By understanding both, your dermatologist can see how your condition has developed and make a more accurate diagnosis.
7. Why is dermoscopy useful in dermatology?
Dermoscopy allows your dermatologist to see microscopic patterns in your skin that aren’t visible to the naked eye. This is particularly useful if you have pigmented lesions or moles that could be concerning, helping ensure early and accurate detection.
8. How does clinical context influence visual assessment?
Your medical history, recent medication use, lifestyle, and environmental exposures all help your dermatologist interpret what they see on your skin. Combining this context with visual examination ensures that your diagnosis is as precise as possible.
9. Why does experience matter for recognising skin disease patterns?
Experience allows your dermatologist to spot subtle differences in your skin that might be missed by less experienced clinicians. The more conditions they have seen, the better they can recognise both common and rare presentations, which benefits your care directly.
10. Can artificial intelligence replace visual pattern recognition by clinicians?
AI can analyse images of your skin and highlight suspicious features, but it cannot replace the judgement of a trained dermatologist. You still need a professional to interpret the results alongside your history and symptoms to confirm an accurate diagnosis.
Final Thought: Pattern Recognition in Dermatology
Understanding how dermatologists use pattern recognition can give you a clearer picture of how your skin concerns are assessed. By carefully observing lesion morphology, distribution, colour, and texture, your clinician can often identify potential conditions quickly and accurately. When you combine these visual assessments with your medical history, lifestyle factors, and, if needed, further investigations like dermoscopy or biopsies, the result is a comprehensive and reliable diagnosis.
If you would like to book a consultation with one of our dermatologists, you can contact us at the London Dermatology Centre. This ensures you receive personalised advice and care tailored to your skin needs, backed by experienced clinical expertise.
References:
- Rimoin, L., Altieri, L., Craft, N., Krasne, S. and Kellman, P.J. (2015) ‘Training pattern recognition of skin lesion morphology, configuration, and distribution’, Journal of the American Academy of Dermatology, 72(3), pp. 489–495. Available at: https://pubmed.ncbi.nlm.nih.gov/25592621/
- Errichetti, E. and Stinco, G. (2016) ‘Dermoscopy in general dermatology: a practical overview’, Dermatology and Therapy, 6(4), pp. 471–507. Available at: https://pubmed.ncbi.nlm.nih.gov/27613297/
- Dermatoscopic Patterns of Genodermatoses: A Comprehensive Analysis (2021) Available at: https://pubmed.ncbi.nlm.nih.gov/37893091/
- Debelee, T.G. (2023) ‘Skin lesion classification and detection using machine learning techniques: A systematic review’, Diagnostics, 13(19), 3147. Available at: https://www.mdpi.com/2075-4418/13/19/3147
- Sun, J., Yao, K., Huang, G., Zhang, C., Leach, M. and Huang, K. (2023) ‘Machine learning methods in skin disease recognition: A systematic review’, Processes, 11(4), 1003. Available at: https://www.mdpi.com/2227-9717/11/4/1003