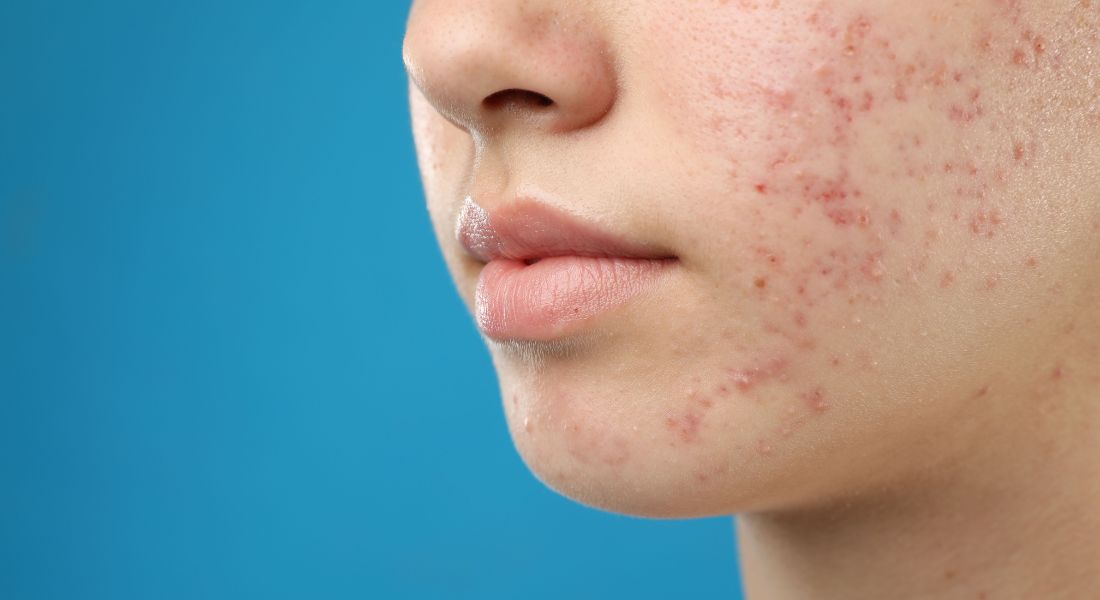
If you’ve ever noticed that your cheeks, nose, or forehead remain persistently flushed, it’s natural to wonder whether it could be rosacea. I want to reassure you from the start: seeing redness on your face doesn’t automatically mean you have a chronic skin condition. Facial redness is actually very common, and its causes are often more varied than most people realise. Understanding the difference between rosacea and other triggers is the first step in managing it effectively.
Persistent redness can be influenced by a range of factors, including environmental triggers, sensitive skin, or lifestyle habits like sun exposure and diet. Not every flush points to a medical issue, but certain patterns may indicate rosacea. Learning to recognise these signs can help you determine whether professional advice is needed. Awareness empowers you to make informed decisions about your skin care.
Dermatologists evaluate persistent redness carefully, looking at the pattern, duration, and accompanying symptoms. They also consider your medical history and potential triggers to distinguish between rosacea and other causes. This thorough assessment ensures that any treatment or management plan is tailored specifically to your needs.
In this article, I’ll walk you through what persistent facial redness is, how specialists assess it, and how to tell whether rosacea is truly the cause. You’ll also learn when it might be appropriate to seek help, such as visiting a rosacea treatment clinic in London. By the end, you should have a clearer understanding of your options and how to manage your skin confidently.
What Is Persistent Facial Redness?
Facial redness can show up as a temporary flush or as a more long-lasting pink or red tone across the cheeks, nose, forehead, or chin. When it persists for weeks, months, or even years, it can affect self-esteem and make social interactions feel uncomfortable. Persistent redness can be more than just a cosmetic concern.
The skin has a complex network of tiny blood vessels, which can dilate and increase blood flow to the surface, causing a red appearance. Sometimes this is completely normal, such as during exercise or when feeling embarrassed. Other times, it may signal an underlying condition.
Persistent redness can be linked to issues like rosacea, eczema, or lupus. Identifying the true cause is important because it determines the right treatment or management plan. Understanding the difference between normal flushing and a medical condition is the first step toward effective care.
Understanding Rosacea
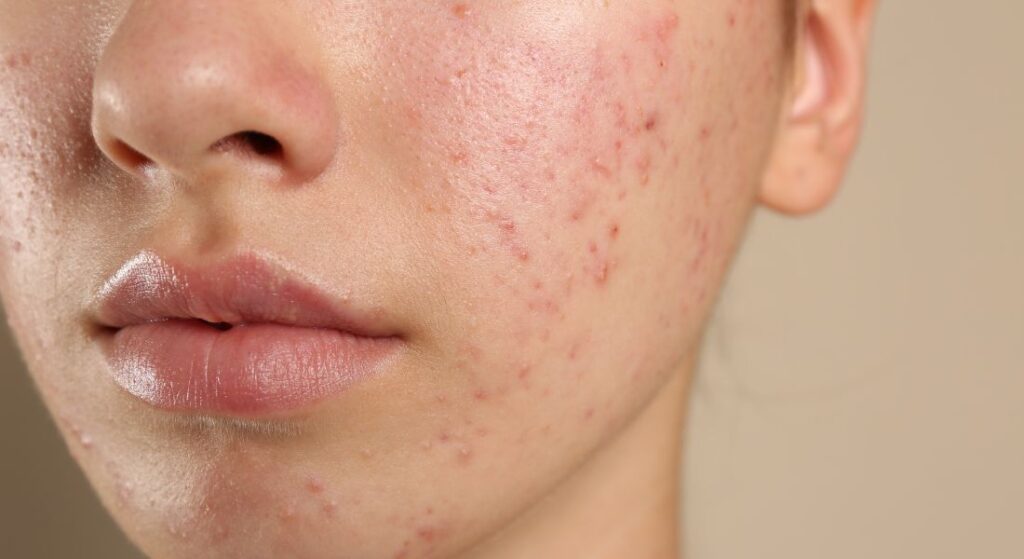
Rosacea is a chronic inflammatory skin condition most commonly affecting adults over 30, especially those with fair skin. It typically begins with intermittent facial redness that can worsen over time if left untreated. Importantly, rosacea is more than just occasional flushing it can present in a variety of ways, affecting both skin and eyes. Recognising the specific manifestations and subtypes is key to effective management and treatment.
- Erythema: Persistent redness often appears across the nose, cheeks, chin, or forehead. This chronic redness is usually more than simple flushing and can be a visible sign of ongoing inflammation. Managing erythema early helps prevent progression and long-term skin changes.
- Telangiectasia: These are small, visible blood vessels commonly referred to as “spider veins.” They develop due to chronic inflammation and can become more pronounced over time. Treatments like laser therapy or intense pulsed light can reduce their appearance effectively.
- Papules and Pustules: Some subtypes of rosacea cause red bumps or acne-like pustules on affected areas. These lesions can be mistaken for acne, but the underlying inflammation is different. Topical or oral treatments targeted to rosacea help control these breakouts and reduce irritation.
- Ocular Involvement: Rosacea can affect the eyes, causing redness, watery eyes, or eyelid irritation in some cases. Ocular rosacea requires careful monitoring, as untreated inflammation may lead to more serious eye problems. Eye drops, eyelid hygiene, and specialist care are often recommended.
In conclusion, rosacea is a multifaceted condition that extends beyond simple facial flushing. Recognising its subtypes erythematotelangiectatic, papulopustular, phymatous, and ocular allows for tailored treatment strategies. Early identification and management can control symptoms, reduce flare-ups, and prevent long-term complications. By understanding the full spectrum of rosacea, patients and dermatologists can work together to achieve clearer, healthier skin.
Why Facial Redness Isn’t Always Rosacea
It’s important to remember that persistent facial redness is not always caused by rosacea. Several other factors, ranging from temporary reactions to underlying medical conditions, can produce a similar appearance. Distinguishing between rosacea and other causes is essential for effective treatment. Understanding these differences helps avoid misdiagnosis and ensures that your skin receives the most appropriate care.
- Sensitive Skin: Many individuals have skin that reacts easily to environmental triggers, such as temperature changes, wind, or certain skincare products. This sensitivity can cause redness that mimics rosacea. Unlike rosacea, sensitive skin usually lacks chronic inflammation, papules, or pustules.
- Acne and Post-Inflammatory Redness: Inflamed acne lesions often leave behind residual redness, called post-inflammatory erythema. This can persist for weeks or even months after the acne clears. People may mistakenly think this redness is rosacea, highlighting the need for careful evaluation.
- Seborrhoeic Dermatitis: This condition produces red, scaly patches on oil-rich areas, such as the forehead, sides of the nose, and behind the ears. Although it can resemble rosacea, seborrhoeic dermatitis usually comes with noticeable flaking or scaling, which is uncommon in classic rosacea.
- Lupus Erythematosus: Both systemic and cutaneous lupus can create a “butterfly rash” across the cheeks and nose. Unlike rosacea, lupus often presents with additional symptoms such as joint pain, fatigue, or sensitivity to sunlight. Diagnosis typically requires blood tests and specialist assessment.
- Medication-Induced Flushing: Certain medications, including corticosteroids, niacin, and some blood pressure drugs, can cause persistent facial redness. If redness appears after starting a new medication, discussing alternatives with a healthcare provider is advisable.
- Alcohol or Food Triggers: Alcohol and spicy foods can temporarily dilate blood vessels, causing facial flushing. While usually short-lived, repeated exposure may create a pattern of persistent redness in some individuals. Awareness of triggers can help manage these episodes effectively.
In conclusion, not all facial redness indicates rosacea. From sensitive skin to medical conditions like lupus or medication-induced flushing, multiple factors can mimic its appearance. Accurate identification is crucial for effective treatment and to avoid unnecessary interventions. Working with a dermatologist ensures that the cause of redness is properly diagnosed and managed for the best skin health outcomes.
How Dermatologists Assess Persistent Facial Redness
When dealing with persistent facial redness, dermatologists follow a structured approach to determine the cause. The first step is taking a detailed history, where they ask about how long the redness has been present, whether it is constant or comes and goes, possible triggers like sun or stress, family history of skin conditions, and any medications or skincare products you use. This helps distinguish between temporary flushing, rosacea, and other underlying conditions.
The next step is a thorough physical examination under proper lighting. Dermatologists look at the distribution of redness, the presence of papules, pustules, or scaling, visible blood vessels (telangiectasia), and any skin thickening or phymatous changes. For example, redness across the central face with visible blood vessels but no scaling is a strong indicator of rosacea.
In some cases, additional diagnostic tests are needed. These may include skin swabs or cultures to rule out infection, blood tests if systemic conditions like lupus are suspected, and patch testing to check for allergic contact dermatitis. By combining the patient history, visual assessment, and any necessary tests, dermatologists can identify the cause and recommend the most effective treatment plan.
Common Triggers That Can Worsen Facial Redness
Even after a formal diagnosis, certain triggers can make facial redness worse. Identifying and managing these factors is an important part of controlling symptoms and maintaining skin comfort. While trigger management does not replace medical treatment, it can significantly improve the appearance of the skin and reduce flare-ups. Awareness of personal triggers allows patients to take proactive steps in everyday life to minimise irritation.
- Sun Exposure: Ultraviolet (UV) radiation can cause blood vessels to dilate and inflame the skin. Regular sun protection, such as sunscreen and protective clothing, helps prevent redness from worsening. Avoiding peak sun hours further reduces exposure and flare-ups.
- Temperature Extremes: Hot drinks, saunas, cold winds, or sudden temperature changes can trigger flushing. Protecting your skin from harsh environmental conditions helps maintain stability and reduces unnecessary irritation. Layering clothing or using gentle skincare routines can mitigate these effects.
- Stress and Emotions: Emotional factors like anxiety, embarrassment, or excitement can lead to temporary facial flushing. Stress management techniques, such as mindfulness, deep breathing, or relaxation exercises, may help minimise these episodes.
- Dietary Factors: Spicy foods, alcohol, and hot beverages can dilate blood vessels and worsen redness. Keeping a food diary can help identify personal dietary triggers and allow for better planning to reduce flare-ups.
- Skincare Products: Alcohol-based toners, harsh exfoliants, and fragranced products can aggravate sensitive skin. Choosing gentle, non-irritating products designed for sensitive or rosacea-prone skin supports long-term skin comfort.
In conclusion, recognising common triggers is an essential part of managing facial redness. Sun exposure, temperature extremes, emotional stress, diet, and certain skincare products can all worsen symptoms. By identifying and minimising these triggers, patients can support medical treatments and maintain healthier, calmer skin. Proactive lifestyle adjustments complement professional care and help improve overall skin appearance and comfort.
Treatment Options for Rosacea
If your persistent redness is diagnosed as rosacea, there are several strategies to manage it. I’ve organised them into categories to help you understand what might suit you best. Treatment often combines medical therapies with lifestyle adjustments to achieve the most effective results.
1. Topical Treatments
Topical therapies are usually the first line of treatment. These include metronidazole cream or gel, which reduces inflammation, azelaic acid to help with redness and papules, and ivermectin cream, which targets inflammatory lesions linked to mites associated with rosacea. Consistency is key, as most treatments take several weeks to show noticeable improvement.
2. Oral Medications
In moderate to severe cases, oral therapy may be recommended. This can include tetracycline antibiotics such as doxycycline or minocycline, which reduce inflammation, and occasionally isotretinoin under specialist supervision for resistant cases. Your dermatologist will discuss potential side effects and suitability for your lifestyle before starting treatment.
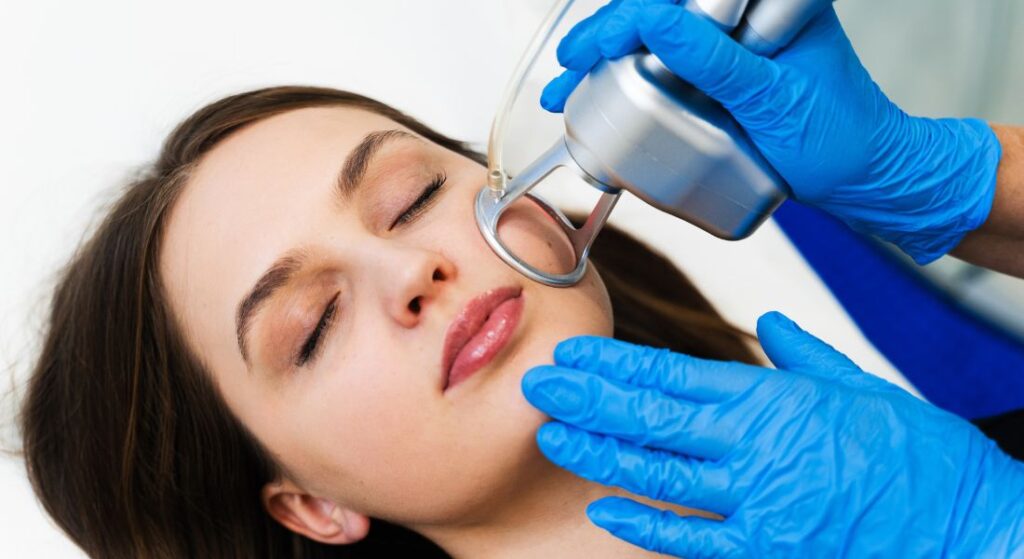
3. Laser and Light-Based Treatments
For persistent redness and visible blood vessels, laser therapies can be highly effective. Pulsed dye laser (PDL) targets dilated vessels, while intense pulsed light (IPL) improves overall redness and skin texture. Multiple sessions may be needed, but results can be long-lasting. Seeking care at a reputable rosacea treatment clinic in London can ensure safety and effectiveness.
4. Lifestyle Adjustments
Small changes in daily routine can also make a significant difference. Using gentle, fragrance-free skincare, applying sunscreen daily, avoiding known dietary or environmental triggers, and practising stress-reducing techniques like mindfulness or meditation can all help. Combining medical therapy with these adjustments often provides the best long-term outcomes.
When Facial Redness Requires Further Investigation
Not all facial redness is straightforward, and sometimes it may signal a condition that needs more than standard topical treatments. It’s important to recognise when further evaluation is necessary. Early assessment can help ensure the correct diagnosis and prevent complications.
I would recommend seeking further investigation if you notice redness accompanied by itching, pain, or scaling. Other warning signs include a sudden onset of facial redness without previous history, symptoms affecting other body systems such as joint pain or fatigue, or redness that worsens despite standard rosacea treatments.
Consulting a dermatologist early in these cases is essential. This helps prevent misdiagnosis and ensures that any underlying conditions, whether skin-related or systemic, are properly identified and managed. Prompt evaluation allows for appropriate treatment and better long-term outcomes.
How Self-Diagnosis Can Be Misleading
It’s natural to assume that persistent facial redness must be rosacea, especially with the wealth of information online. However, self-diagnosis can often be misleading. Redness can have many causes, and treating it incorrectly may do more harm than good.
For example, I once knew someone whose central facial redness was actually mild eczema rather than rosacea. Applying the wrong creams or treatments not only failed to help but also aggravated the skin and prolonged discomfort. This highlights how tricky it can be to identify the cause without professional guidance.
This is why seeking expert assessment is invaluable. A dermatologist can distinguish between different causes of redness and recommend the most effective treatment. Getting the right diagnosis early saves time, reduces frustration, and ensures better results for your skin health.
Support and Psychological Impact
Persistent facial redness can have a real impact on self-confidence, social interactions, and even mental health. Feeling anxious, embarrassed, or withdrawn because of your skin is completely understandable. These emotional effects are just as important to acknowledge as the physical symptoms.
Seeking support can make a big difference. This might include joining support groups, speaking with a counsellor, or discussing your concerns openly with a dermatologist. Sharing your experiences helps you feel understood and less isolated.
In many cases, visible improvement through treatment alone can significantly boost self-esteem. Knowing that effective solutions are available often reduces anxiety and allows you to engage more comfortably in daily life. Combining emotional support with proper care creates the best outcomes for both your skin and wellbeing.
When to Consider a Specialist Clinic
For complex or resistant cases, visiting a specialised clinic can make a significant difference. These clinics provide expert care that goes beyond standard treatments. They are particularly helpful if redness persists despite trying over-the-counter remedies or basic skincare approaches.
A rosacea treatment clinic in London offers access to dermatologists experienced in diagnosing subtle or atypical forms of rosacea. They can provide advanced laser and light-based therapies, which are often more effective for persistent redness and visible blood vessels.
Specialist clinics also create tailored treatment plans that combine medication, lifestyle adjustments, and personalised skincare guidance. This comprehensive approach ensures that persistent facial redness is managed effectively, helping to improve both skin health and overall quality of life.
Practical Daily Skincare Tips

Managing facial redness isn’t just about medical treatments daily skincare plays a vital role in reducing flare-ups and protecting your skin. Gentle, consistent care helps maintain the skin barrier and minimise irritation. Small habits each day can make a big difference over time.
Start by cleansing gently using lukewarm water and a mild, soap-free cleanser. Regular moisturising keeps your skin barrier intact and helps prevent sensitivity. Sun protection is essential: use a broad-spectrum SPF 30+ sunscreen and reapply every two hours when outdoors.
It’s also important to avoid harsh ingredients that can aggravate redness. Products containing retinoids, alpha-hydroxy acids, or high levels of alcohol may worsen flare-ups. By following these steps consistently, you can help reduce the severity and frequency of facial redness and support healthier, calmer skin.
Reducing Flare-Ups With Lifestyle Choices
Managing facial redness isn’t just about skincare lifestyle choices can play a significant role in reducing flare-ups. Small, consistent adjustments in diet, hydration, stress management, and daily habits can support skin health and complement medical treatments. By integrating these practices into everyday life, patients often notice a meaningful improvement in redness and overall skin comfort.
- Balanced Diet: Consuming anti-inflammatory foods, particularly those rich in omega-3 fatty acids, can help calm skin inflammation. Foods such as fatty fish, flaxseeds, and leafy greens provide nutrients that support overall skin health. A well-balanced diet also helps maintain a stable internal environment that may reduce flare-ups.
- Hydration: Drinking adequate water each day keeps the skin hydrated and resilient. Proper hydration supports the skin’s natural barrier, helping to reduce irritation and redness. Even mild dehydration can exacerbate flushing, so consistent fluid intake is important.
- Stress Management: Techniques such as yoga, meditation, and deep breathing can help lower stress levels, which are common triggers for facial flushing. Regular practice not only benefits skin health but also improves overall wellbeing. Reducing stress-induced redness can make a noticeable difference in daily comfort.
- Moderation With Alcohol and Spicy Foods: Alcohol and spicy foods are common triggers for many individuals with facial redness. Consuming these in moderation or avoiding them during flare-ups can help prevent sudden flushing episodes. Awareness of dietary triggers allows for proactive management.
In conclusion, lifestyle adjustments are a powerful complement to medical therapy for managing facial redness. Balanced nutrition, hydration, stress management, and careful attention to dietary triggers can reduce flare-ups and improve skin appearance. By adopting these strategies consistently, patients can take greater control over their condition and enhance both comfort and confidence in daily life.
Common Myths About Facial Redness
There are several misconceptions about facial redness that can cause unnecessary worry. Understanding the facts helps you approach treatment and skincare more effectively. Clearing up these myths also prevents frustration from trying ineffective or unnecessary remedies.
One common myth is that “only fair-skinned people get rosacea.” While it is more frequently diagnosed in fair skin, rosacea can affect all ethnicities. Another misconception is that “rosacea is caused by poor hygiene.” This is completely untrue rosacea is an inflammatory condition and has no connection to cleanliness.
Finally, some believe that “redness always requires medication.” In reality, mild cases can often be managed with lifestyle adjustments and gentle skincare alone. Knowing the truth about these myths helps you make informed decisions and take appropriate steps to care for your skin.
FAQs:
1. Is persistent facial redness always rosacea?
No. Persistent redness can be caused by sensitive skin, acne, seborrhoeic dermatitis, lupus, medication reactions, or lifestyle factors. A dermatologist can help identify the true cause.
2. What are the common signs of rosacea?
Rosacea often causes persistent redness on the cheeks, nose, forehead, or chin. Other signs include visible blood vessels (telangiectasia), red bumps or pustules, and, in some cases, eye irritation.
3. How do dermatologists distinguish rosacea from other causes of redness?
Dermatologists evaluate the pattern, duration, triggers, and accompanying symptoms. They may also use tests like blood work, patch testing, or skin swabs to rule out other conditions.
4. Can lifestyle factors worsen facial redness?
Yes. Sun exposure, temperature extremes, stress, spicy foods, alcohol, and certain skincare products can trigger or worsen redness, even in people with rosacea.
5. What treatment options are available for rosacea?
Treatment can include topical creams (metronidazole, azelaic acid, ivermectin), oral antibiotics (doxycycline), laser or light-based therapies, and lifestyle adjustments to reduce triggers.
6. How can I manage facial redness if it’s not rosacea?
Management depends on the underlying cause. Sensitive skin may benefit from gentle skincare, lupus requires specialist monitoring, and medication-induced flushing may need adjustments by a healthcare provider.
7. When should I see a dermatologist for facial redness?
Seek professional advice if redness persists, worsens, is accompanied by scaling, itching, pain, or affects other parts of the body. Early assessment helps ensure accurate diagnosis and effective treatment.
8. Can facial redness impact mental health?
Yes. Persistent redness can affect self-esteem, confidence, and social interactions. Support, counselling, and effective treatment can help manage these emotional effects.
9. Are there myths about facial redness I should know?
Common myths include “rosacea only affects fair skin” and “redness is caused by poor hygiene.” Understanding the facts helps you manage the condition more effectively.
10. Can daily skincare and lifestyle changes reduce redness?
Yes. Gentle cleansing, moisturising, sun protection, stress management, and avoiding known triggers can significantly reduce flare-ups and improve skin comfort.
Final Thoughts: Understanding and Managing Persistent Facial Redness
Persistent facial redness can be worrying, but it’s important to remember that it isn’t always rosacea. By working with a dermatologist, you can accurately identify the cause whether it’s sensitive skin, a medical condition, lifestyle factors, or true rosacea and receive personalised guidance for effective management. Combining professional treatments, daily skincare routines, and lifestyle adjustments can significantly reduce redness, prevent flare-ups, and improve both your skin health and confidence.
For more complex or resistant cases, visiting a specialised facility can make a real difference. A rosacea treatment clinic in London offers expert care, advanced therapies, and tailored plans to help manage persistent redness effectively. If you’re considering rosacea treatment clinic in London, you can get in touch with us at London Dermatology Centre.
References:
- Rainer, B.M., Kang, S. and Chien, A.L. (2017) Rosacea: epidemiology, pathogenesis, and treatment, Gut Pathogens, 9(1), e1361574. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5821167/
- Johnson, S.M., Berg, A. and Barr, C. (2019) Recognizing rosacea: tips on differential diagnosis, Journal of Drugs in Dermatology, 18(9), pp. 888–894. Available at: https://pubmed.ncbi.nlm.nih.gov/31524344/
- Nowicka, D., Chilicka, K., Dzieńdziora‑Urbińska, I. and Szyguła, R. (2023) Skincare in rosacea from the cosmetologist’s perspective: A narrative review, Journal of Clinical Medicine, 12(1), 115. Available at: https://www.mdpi.com/2077-0383/12/1/115
- Wilkin, J. et al. (2004) Rosacea: I. Etiology, pathogenesis, and subtype classification, Journal of the American Academy of Dermatology, 51(3), pp. 387–395. Available at: https://www.sciencedirect.com/science/article/abs/pii/S0190962204008448
- Tan, J. et al. (2018) Applying the phenotype approach for rosacea to practice and research, British Journal of Dermatology, 179(3), pp. 741–746. Available at: https://academic.oup.com/bjd/article/179/3/741/6732451