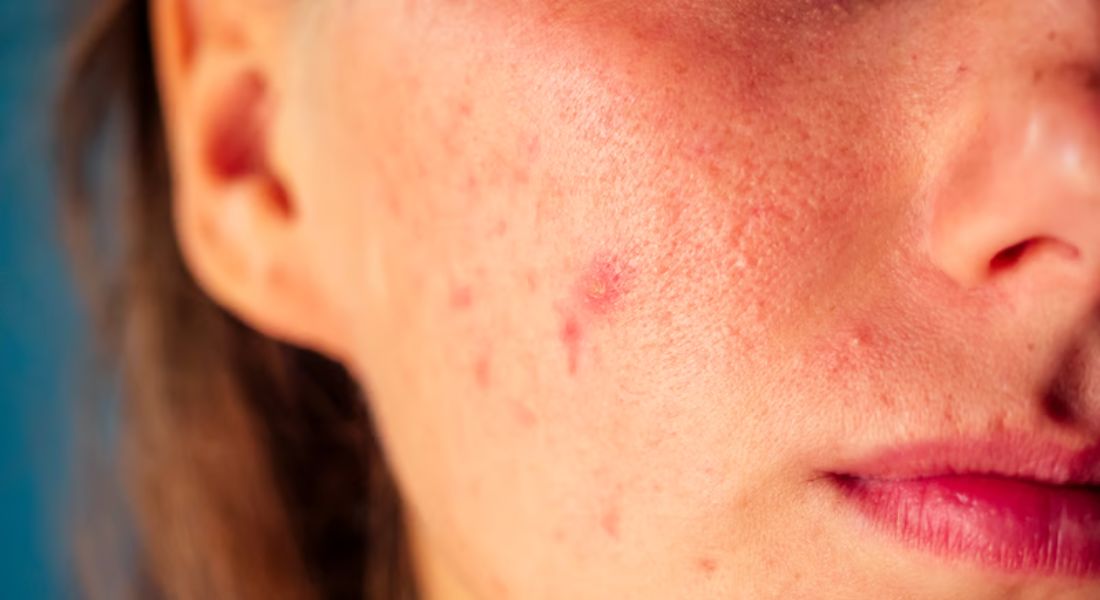
If you have ever been told that you have rosacea but something about the diagnosis does not feel quite right, you are not alone. Many people spend months or even years treating a condition that is not actually causing their symptoms. This can be frustrating, especially when treatments do not deliver the results you expect. It may also leave you feeling uncertain about what is really happening with your skin.
Skin conditions can appear very similar on the surface, which is why misdiagnosis happens so often. Symptoms such as redness, bumps, irritation, and sensitivity are not exclusive to rosacea. You may notice overlapping signs that make it difficult to clearly identify the condition. This can make it challenging to rely on assumptions or self-diagnosis alone.
In some cases, subtle differences between conditions are easy to overlook without professional guidance. You might be treating what seems like rosacea when, in fact, another skin concern is responsible. This can delay effective treatment and allow symptoms to persist for longer than necessary. Understanding these differences is an important step towards clearer answers.
In this guide, you will learn about the conditions most commonly mistaken for rosacea and how they are distinguished. You will also gain insight into why an accurate diagnosis is so important for your skin. Identifying the correct condition allows for more targeted and effective treatment. This can make a meaningful difference to your skin’s long-term health and comfort.
What Is Rosacea?
Rosacea is a long-term inflammatory skin condition that mainly affects your face. It often causes persistent redness, flushing, and sometimes spots that can look similar to acne. You may notice these symptoms appearing across areas such as your cheeks, nose, chin, or forehead. The way it presents can vary depending on your skin and its sensitivity.
One of the features that makes rosacea distinct is how it tends to fluctuate over time. You may experience periods where your skin feels relatively calm, followed by sudden flare-ups. These changes can sometimes happen without a clear warning, which can make the condition feel unpredictable. Recognising these patterns can help you better understand your skin.
Rosacea is not simply a cosmetic concern, even though it affects your appearance. It is a condition that requires proper understanding and careful management. You may need to make adjustments to your routine and be aware of potential triggers. With the right approach, it can be effectively controlled over time.
Why Rosacea Is Commonly Misdiagnosed

Rosacea is often described as a condition that is diagnosed based on patterns rather than a single definitive test. This means that identifying it relies on recognising visible signs along with understanding your medical history. A professional will assess how your symptoms appear and how they have developed over time. This approach requires careful observation rather than a quick judgement.
One of the main challenges is that many other skin conditions share similar features. Symptoms such as redness, irritation, and sensitivity are not unique to rosacea and can appear in several conditions. You may notice overlapping signs that make it difficult to clearly identify the cause. This can make self-diagnosis unreliable and sometimes misleading.
If a diagnosis is made too quickly or based on limited information, it is easy to mistake one condition for another. You may end up treating the wrong issue, which can delay improvement and cause frustration. A thorough and considered approach helps ensure a more accurate diagnosis. This is why taking the time to properly assess your skin is so important.
What Rosacea Typically Looks Like
Before exploring misdiagnosis, it is helpful for you to understand what rosacea usually looks like. Having a clear idea of its common features can make it easier to recognise. You may find that knowing these signs helps you better assess your own skin. This provides a useful starting point for understanding the condition.
Rosacea most commonly affects the central areas of your face, including the cheeks, nose, chin, and forehead. You will often notice persistent redness in these areas, which may gradually become more noticeable over time. Flushing episodes are also common and may come and go in the early stages. As the condition progresses, this redness can become more constant.
Some people also develop visible blood vessels or spots that resemble acne. However, rosacea does not usually include blackheads, which helps distinguish it from typical acne. You might also notice that your skin feels more sensitive or reactive than usual. Recognising these features can help you better understand what your skin may be experiencing.
Why an Accurate Diagnosis Matters
It can be tempting to assume that all skin redness can be treated in the same way, especially when symptoms appear similar on the surface. However, different skin conditions require very different approaches, and using the wrong treatment can sometimes do more harm than good. When products or routines fail to deliver results, it often leads to confusion and frustration. This is why understanding the exact cause of your symptoms is essential for effective care.
- Risk of Using the Wrong Treatment: Not all redness responds to the same products, and misidentifying the condition can lead to ineffective or harmful treatment. For example, using harsh or unsuitable products may worsen sensitivity rather than improve it. This can prolong symptoms and make the condition harder to manage.
- Certain Treatments Can Aggravate Symptoms: Treatments designed for other conditions, such as acne, often focus on drying out the skin. While this may help acne, it can irritate and worsen rosacea-prone skin. Similarly, topical steroids may provide temporary relief but can lead to more persistent issues over time if used incorrectly.
- Short-Term Improvement vs Long-Term Effects: Some treatments may appear to work initially by reducing redness or inflammation. However, this improvement is often temporary and may be followed by flare-ups or worsening symptoms. Without an accurate diagnosis, it becomes difficult to achieve lasting results.
- Targeted and Effective Management: A correct diagnosis allows for a treatment plan that is specifically tailored to your skin’s needs. This helps ensure that the products and methods used are appropriate and less likely to cause irritation. Over time, this targeted approach leads to more consistent and manageable results.
In conclusion, an accurate diagnosis is a crucial step in effectively managing skin conditions like rosacea. It helps prevent the use of inappropriate treatments that may worsen symptoms or delay improvement. By understanding the true cause of your skin concerns, you can follow a more suitable and effective care routine. This ultimately leads to better long-term outcomes and healthier, more balanced skin.
How I Differentiate Between These Conditions
When assessing your skin, I do not rely on a single sign or symptom. Instead, I look at the overall pattern and how different features come together. This includes understanding how your skin behaves over time and in response to certain triggers. Taking a broader view helps create a more accurate picture of what may be causing your symptoms.
A detailed history is always an important starting point. You will be asked about your symptoms, possible triggers, and how long the condition has been present. Understanding what makes your skin better or worse can provide valuable clues. I also consider where the symptoms appear, as rosacea typically affects the central areas of the face, while other conditions may show up in different patterns.
Close attention is also given to the type of marks or changes on your skin. For example, blackheads may suggest acne, while dryness or scaling can point towards dermatitis. Your response to previous treatments is another key factor, as worsening with certain products can help narrow down the diagnosis. In addition, I consider any symptoms beyond the skin, as issues such as fatigue or joint pain may indicate an underlying condition that needs further investigation.
Ageing and Skin Barrier Changes
As you age, your skin naturally undergoes structural changes that can weaken its protective barrier. This barrier is essential for keeping irritants out while maintaining hydration and balance within the skin. Over time, reduced resilience makes the skin more vulnerable to external stressors. As a result, your skin may become increasingly reactive and sensitive.
- Weakened Skin Barrier Function: The skin barrier becomes less effective at protecting against environmental irritants as it ages. This allows substances that were previously harmless to penetrate more easily. As a result, the skin is more prone to irritation and imbalance.
- Increased Reactivity: With a compromised barrier, the skin can react more strongly to everyday products and environmental factors. Even gentle skincare items may start to cause discomfort such as stinging or redness. This heightened sensitivity can make routine care more challenging.
- Greater Susceptibility to Irritation: External triggers like pollution, temperature changes, and skincare ingredients can have a stronger impact on ageing skin. Because the barrier is weakened, these triggers can lead to more frequent irritation. Over time, repeated exposure can worsen skin sensitivity.
- Contribution to Rosacea Development: Persistent sensitivity and irritation can play a role in the development of rosacea symptoms. As the skin struggles to defend itself, inflammation becomes more common. This ongoing cycle can contribute to redness and long-term skin concerns.
In conclusion, ageing has a direct impact on the strength and function of the skin barrier. As this barrier weakens, the skin becomes more reactive and prone to irritation. These changes can increase the likelihood of developing conditions such as rosacea. Supporting the skin barrier is key to maintaining healthier, more resilient skin over time.
Immune System Sensitivity
Rosacea is linked to an overactive immune response within your skin. This means your skin may react more strongly than it normally should to certain triggers. You might notice increased redness, irritation, or sensitivity in situations that would not affect others. This heightened response can make your skin feel more unpredictable.
Triggers that seem harmless to other people can lead to noticeable flare-ups for you. These may include factors such as temperature changes, certain foods, or stress. Over time, your skin may become more reactive to these influences. This gradual change can make it harder to ignore the symptoms.
As this sensitivity develops, it often becomes more consistent and easier to recognise. What may have started as occasional reactions can turn into more persistent symptoms. You might find that redness or discomfort lasts longer than before. This is when the effects of rosacea become more clearly established.
The Role of Professional Diagnosis

Self-diagnosis can only take you so far when it comes to understanding your skin. While it can be helpful to explore possible causes, it does not always provide clear or accurate answers. You may find that symptoms overlap, making it difficult to be certain about what you are experiencing. This is why a professional assessment is an important step.
Dermatologists are trained to recognise subtle differences between skin conditions. They look beyond surface-level symptoms and consider patterns, history, and specific features. This allows for a more accurate and confident diagnosis. With the right expertise, you are more likely to receive guidance that truly suits your skin.
If you are unsure about your condition, seeking professional advice can provide clarity and reassurance. A proper evaluation helps you understand what is happening and how to manage it effectively. You do not need to rely on guesswork when support is available. Taking this step can make a meaningful difference to your skin’s long-term health.
What Happens After Diagnosis?
Once you receive an accurate diagnosis, managing your skin becomes far more structured and effective. Instead of relying on guesswork or constantly switching products, you gain a clear understanding of what your skin truly needs. This clarity can bring both relief and confidence, as you begin to follow a more informed approach. With the right direction, your skincare journey becomes more consistent and less frustrating.
- A Clear and Targeted Treatment Plan: After diagnosis, you can move away from trial-and-error methods and follow a plan tailored specifically to your condition. This approach focuses on addressing the root cause rather than just the visible symptoms. As a result, treatments are more effective and aligned with your skin’s unique needs.
- More Consistent Skin Response: When your routine is personalised, your skin is more likely to respond in a stable and predictable way. You may notice fewer unexpected reactions and more gradual improvement over time. This consistency makes it easier to track progress and adjust your routine when necessary.
- Comprehensive Approach to Care: Your treatment plan may include a combination of skincare adjustments, prescription treatments, and lifestyle changes. Each element works together to reduce triggers and support overall skin health. This holistic strategy helps manage symptoms while also preventing future flare-ups.
- Long-Term Skin Strength and Resilience: The goal of treatment is not just short-term relief but also long-term improvement in skin health. By strengthening the skin barrier and reducing sensitivity, your skin becomes more resilient over time. This can lead to fewer flare-ups and better overall control of the condition.
In conclusion, receiving the correct diagnosis marks an important turning point in managing your skin effectively. It replaces uncertainty with a clear, targeted approach that supports both immediate and long-term results. With the right plan in place, your skin can become more stable, balanced, and resilient. Over time, this leads to greater confidence and better overall skin health.
The Risks of Misdiagnosis
Misdiagnosis does not only delay improvement in your skin; it can also make the condition worse over time. You may find that symptoms persist or even become more noticeable despite your efforts to treat them. This can be discouraging, especially when you feel like you are doing the right things. Without the correct diagnosis, it becomes difficult to move forward with confidence.
Using the wrong treatments can further irritate your skin and disrupt its natural balance. Products that are not suited to your condition may increase sensitivity, redness, or inflammation. You might notice that your skin reacts more easily or takes longer to recover. Over time, this can make your skin more difficult to manage.
There is also an emotional impact that comes with ongoing uncertainty about your skin. You may feel frustrated when treatments do not work as expected or when symptoms continue. This can affect your confidence and how you feel in everyday situations. Recognising the importance of an accurate diagnosis can help you avoid these challenges and move towards more effective care.
When You Should Seek a Second Opinion
If your current treatment is not giving the results you expected, it is reasonable for you to question the diagnosis. You do not need to accept ongoing uncertainty when it comes to your skin. It is important that you feel confident in the care you are receiving. Seeking further clarity can help you move in the right direction.
You may want to consider a second opinion if your symptoms continue or worsen despite following treatment. This can be a sign that the condition has not been correctly identified. You might also notice that your skin is not responding in the way it should. In these situations, another professional perspective can be very helpful.
It is also worth seeking further advice if your condition changes unexpectedly over time. Skin conditions can evolve, and new symptoms may point to a different issue. You may find that what once seemed accurate no longer fully explains your skin. Revisiting your diagnosis can help ensure you are receiving the most appropriate care.
How to Support Your Skin While Waiting for Diagnosis
If you are still in the process of understanding your skin, there are a few simple steps you can take to protect it. During this time, it is best to avoid overcomplicating your routine or trying too many treatments at once. You may feel tempted to experiment, but this can sometimes make things worse. Keeping things calm and consistent can help reduce unnecessary irritation.
Try to keep your skincare routine as simple as possible. Avoid introducing multiple new products at the same time, as this can make it harder to identify what is helping or causing a reaction. Using gentle, fragrance-free products can help minimise sensitivity. This approach allows your skin to settle while you work towards a clearer diagnosis.
It is also important to protect your skin from sun exposure on a daily basis. Ultraviolet light can trigger or worsen many skin conditions, including rosacea. Using a broad-spectrum SPF can help prevent flare-ups and support your skin’s recovery. These small, consistent steps can make a positive difference while you seek further guidance.
Living with Uncertainty: A Common Experience
It is completely understandable for you to feel frustrated when you do not have clear answers about your skin. Skin conditions can be unpredictable, and this uncertainty can sometimes feel stressful or overwhelming. You may find yourself questioning what is happening and why things are not improving. These feelings are a very common part of the process.
It is important for you to remember that you are not alone in this experience. Many people go through a period of trial and error before reaching the correct diagnosis. You might need time to fully understand how your skin behaves and what affects it. This stage, although challenging, is often part of finding the right solution.
With the right support and guidance, clarity is absolutely achievable. Seeking professional advice and staying consistent with gentle care can help move things in the right direction. You may gradually begin to see patterns and improvements over time. This can give you more confidence in managing your skin moving forward.
FAQs:
1. Why is rosacea often misdiagnosed?
Rosacea is commonly misdiagnosed because its symptoms such as redness, bumps, and sensitivity overlap with many other skin conditions, making it difficult to identify without a detailed assessment.
2. What conditions are most commonly mistaken for rosacea?
Conditions often confused with rosacea include acne, eczema, seborrhoeic dermatitis, allergic contact dermatitis, and lupus.
3. How can I tell if I have rosacea or acne?
Rosacea usually does not involve blackheads or whiteheads, while acne typically does. Rosacea also tends to cause persistent redness and flushing, which are less common in acne.
4. Can eczema look like rosacea?
Yes, eczema can cause redness and irritation similar to rosacea, but it is often accompanied by dryness, flaking, and itching.
5. What is the difference between rosacea and seborrhoeic dermatitis?
Seborrhoeic dermatitis often presents with greasy scales and dandruff-like flakes, especially around the nose and eyebrows, while rosacea mainly causes flushing and visible blood vessels.
6. Why is an accurate diagnosis so important?
An accurate diagnosis ensures you receive the correct treatment. Using the wrong products can worsen symptoms, delay improvement, and increase skin sensitivity.
7. Can treating the wrong condition make my skin worse?
Yes, inappropriate treatments such as harsh acne products or steroid creams can aggravate rosacea or other skin conditions and lead to further irritation.
8. When should I seek a second opinion?
You should consider a second opinion if your symptoms are not improving, are getting worse, or if your diagnosis does not seem to match how your skin behaves.
9. How do dermatologists diagnose rosacea accurately?
Dermatologists assess patterns such as redness distribution, triggers, skin texture, and your medical history to distinguish rosacea from similar conditions.
10. What should I do while waiting for a diagnosis?
Keep your skincare routine simple, use gentle and fragrance-free products, avoid known irritants, and apply daily sun protection to minimise further irritation.
Final Thoughts: The Importance of Getting the Right Diagnosis
When it comes to skin conditions like rosacea, clarity is everything. Many conditions can look similar on the surface, but the underlying causes and treatments can be very different. Taking the time to understand what your skin is truly experiencing allows you to move away from guesswork and towards a more effective, targeted approach.
An accurate diagnosis not only helps prevent unnecessary frustration but also protects your skin from treatments that may do more harm than good. With the right guidance, you can begin to manage your condition with confidence, knowing that your routine is tailored specifically to your needs. Over time, this leads to more consistent results, improved skin comfort, and greater peace of mind. If you’re considering a rosacea treatment clinic in London, you can reach out to us at the London Dermatology Centre to book a consultation with one of our specialists.
References:
- Two, A.M., Wu, W., Gallo, R.L. and Hata, T.R., 2015. Rosacea: Part I. Introduction, categorization, histology, pathogenesis, and risk factors. Journal of the American Academy of Dermatology, 72(5), pp.749–758. Available at: https://pubmed.ncbi.nlm.nih.gov/25890455/
- Woo, Y.R., Lim, J.H., Cho, D.H. and Park, H.J., 2016. Rosacea: molecular mechanisms and management of a chronic cutaneous inflammatory condition. International Journal of Molecular Sciences, 17(9), p.1562. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5037831/
- Wilkin, J., 2004. Rosacea: I. Etiology, pathogenesis, and subtype classification. Journal of the American Academy of Dermatology, 51(3), pp.327–341. Available at: https://www.sciencedirect.com/science/article/abs/pii/S0190962204008448
- Andrusiewicz, A., Khimuk, S., Mijas, D., Shmorhun, B. and Nowicka, D., 2025. Molecular mechanisms in the etiopathology of rosacea systematic review. International Journal of Molecular Sciences, 26(23), p.11292. Available at: https://www.mdpi.com/1422-0067/26/23/11292
- Tan, J., Almeida, L.M.C., Bewley, A., Cribier, B., Dlova, N.C., Gallo, R., et al., 2017. Updating the diagnosis, classification and assessment of rosacea: recommendations from the global ROSacea COnsensus (ROSCO) panel. British Journal of Dermatology, 176(2), pp.431–438. Available at: https://academic.oup.com/bjd/article/176/2/431/6601814